Compare Pulsed Electromagnetic Field and Ice Compression
MAR 7, 20268 MIN READ
Generate Your Research Report Instantly with AI Agent
PatSnap Eureka helps you evaluate technical feasibility & market potential.
PEMF vs Ice Compression Background and Objectives
The therapeutic management of pain, inflammation, and tissue recovery has evolved significantly over the past century, with both traditional and modern approaches competing for clinical validation. Ice compression therapy, rooted in centuries-old practices, has long served as a cornerstone treatment for acute injuries and post-exercise recovery. This conventional approach leverages the physiological principles of vasoconstriction and metabolic suppression to reduce inflammation and provide analgesic effects.
In contrast, Pulsed Electromagnetic Field therapy represents a relatively modern technological advancement that emerged from the intersection of bioelectromagnetics and regenerative medicine. PEMF technology harnesses controlled electromagnetic pulses to stimulate cellular processes at the molecular level, promoting tissue repair through enhanced cellular metabolism and improved circulation patterns.
The evolution of these therapeutic modalities reflects broader trends in healthcare toward evidence-based treatment protocols. While ice compression has maintained its position through widespread accessibility and immediate symptomatic relief, PEMF therapy has gained traction due to growing understanding of bioelectromagnetic interactions and their therapeutic potential. Recent decades have witnessed increased scrutiny of traditional cold therapy limitations, including potential interference with natural healing processes and temporary nature of benefits.
The primary objective of comparing these therapeutic approaches centers on establishing their relative efficacy across multiple clinical parameters. Key evaluation criteria include pain reduction mechanisms, inflammation control effectiveness, tissue healing acceleration, treatment duration requirements, and long-term recovery outcomes. Understanding the distinct physiological pathways each modality influences provides crucial insights for optimizing treatment protocols.
Secondary objectives encompass practical implementation considerations, including cost-effectiveness analysis, accessibility factors, patient compliance rates, and integration potential within existing healthcare frameworks. The comparison aims to identify specific clinical scenarios where each approach demonstrates superior performance, enabling evidence-based treatment selection rather than relying solely on traditional preferences or technological novelty.
In contrast, Pulsed Electromagnetic Field therapy represents a relatively modern technological advancement that emerged from the intersection of bioelectromagnetics and regenerative medicine. PEMF technology harnesses controlled electromagnetic pulses to stimulate cellular processes at the molecular level, promoting tissue repair through enhanced cellular metabolism and improved circulation patterns.
The evolution of these therapeutic modalities reflects broader trends in healthcare toward evidence-based treatment protocols. While ice compression has maintained its position through widespread accessibility and immediate symptomatic relief, PEMF therapy has gained traction due to growing understanding of bioelectromagnetic interactions and their therapeutic potential. Recent decades have witnessed increased scrutiny of traditional cold therapy limitations, including potential interference with natural healing processes and temporary nature of benefits.
The primary objective of comparing these therapeutic approaches centers on establishing their relative efficacy across multiple clinical parameters. Key evaluation criteria include pain reduction mechanisms, inflammation control effectiveness, tissue healing acceleration, treatment duration requirements, and long-term recovery outcomes. Understanding the distinct physiological pathways each modality influences provides crucial insights for optimizing treatment protocols.
Secondary objectives encompass practical implementation considerations, including cost-effectiveness analysis, accessibility factors, patient compliance rates, and integration potential within existing healthcare frameworks. The comparison aims to identify specific clinical scenarios where each approach demonstrates superior performance, enabling evidence-based treatment selection rather than relying solely on traditional preferences or technological novelty.
Market Demand for Recovery and Pain Management Solutions
The global recovery and pain management market has experienced substantial growth driven by increasing awareness of non-pharmacological treatment options and rising healthcare costs associated with chronic pain conditions. Traditional pharmaceutical approaches face growing scrutiny due to opioid crisis concerns, creating significant demand for alternative therapeutic modalities that offer effective pain relief without dependency risks.
Sports medicine represents a particularly dynamic segment where both pulsed electromagnetic field therapy and cryotherapy applications demonstrate strong market penetration. Professional athletes and fitness enthusiasts increasingly seek evidence-based recovery solutions that can accelerate healing processes and minimize downtime between training sessions. This demographic drives premium pricing acceptance and influences broader consumer adoption patterns.
Chronic pain management constitutes the largest market segment, encompassing conditions such as arthritis, fibromyalgia, and musculoskeletal disorders affecting millions globally. Healthcare providers actively seek cost-effective interventions that can reduce long-term treatment expenses while improving patient outcomes. Both electromagnetic field therapy and ice compression therapy address these requirements through different physiological mechanisms.
The aging population demographic significantly amplifies market demand as age-related joint deterioration and mobility issues become more prevalent. Elderly patients often prefer non-invasive treatment options that can be administered at home, reducing frequent clinical visits and associated transportation challenges. This trend favors portable and user-friendly therapeutic devices.
Healthcare system cost containment pressures drive institutional adoption of technologies that demonstrate measurable clinical outcomes while reducing overall treatment expenses. Insurance coverage expansion for alternative therapies creates additional market opportunities, particularly when treatments show documented efficacy in peer-reviewed clinical studies.
Consumer preference shifts toward holistic wellness approaches and preventive care strategies support market growth for both therapeutic modalities. Patients increasingly research treatment options independently and request specific therapies from healthcare providers, creating bottom-up demand pressure within medical practices.
Technological advancement integration with digital health platforms enables remote monitoring and personalized treatment protocols, enhancing patient engagement and treatment compliance. This convergence creates new market opportunities for device manufacturers and healthcare service providers seeking differentiated offerings in competitive therapeutic markets.
Sports medicine represents a particularly dynamic segment where both pulsed electromagnetic field therapy and cryotherapy applications demonstrate strong market penetration. Professional athletes and fitness enthusiasts increasingly seek evidence-based recovery solutions that can accelerate healing processes and minimize downtime between training sessions. This demographic drives premium pricing acceptance and influences broader consumer adoption patterns.
Chronic pain management constitutes the largest market segment, encompassing conditions such as arthritis, fibromyalgia, and musculoskeletal disorders affecting millions globally. Healthcare providers actively seek cost-effective interventions that can reduce long-term treatment expenses while improving patient outcomes. Both electromagnetic field therapy and ice compression therapy address these requirements through different physiological mechanisms.
The aging population demographic significantly amplifies market demand as age-related joint deterioration and mobility issues become more prevalent. Elderly patients often prefer non-invasive treatment options that can be administered at home, reducing frequent clinical visits and associated transportation challenges. This trend favors portable and user-friendly therapeutic devices.
Healthcare system cost containment pressures drive institutional adoption of technologies that demonstrate measurable clinical outcomes while reducing overall treatment expenses. Insurance coverage expansion for alternative therapies creates additional market opportunities, particularly when treatments show documented efficacy in peer-reviewed clinical studies.
Consumer preference shifts toward holistic wellness approaches and preventive care strategies support market growth for both therapeutic modalities. Patients increasingly research treatment options independently and request specific therapies from healthcare providers, creating bottom-up demand pressure within medical practices.
Technological advancement integration with digital health platforms enables remote monitoring and personalized treatment protocols, enhancing patient engagement and treatment compliance. This convergence creates new market opportunities for device manufacturers and healthcare service providers seeking differentiated offerings in competitive therapeutic markets.
Current State and Challenges of PEMF and Cryotherapy
Pulsed Electromagnetic Field (PEMF) therapy has established itself as a non-invasive treatment modality with growing clinical acceptance. Current PEMF devices operate across frequency ranges from 1 Hz to 10,000 Hz, with magnetic field intensities typically ranging from 0.1 to 50 mT. The technology has demonstrated efficacy in bone healing, pain management, and wound recovery through cellular stimulation and enhanced tissue regeneration. However, standardization remains a significant challenge, as optimal parameters vary considerably across different therapeutic applications and patient populations.
The regulatory landscape for PEMF presents complex hurdles. While FDA approval exists for specific indications such as bone fracture healing and depression treatment, broader therapeutic claims require extensive clinical validation. Manufacturing costs remain elevated due to sophisticated electromagnetic coil systems and precise control electronics, limiting widespread adoption in cost-sensitive healthcare environments.
Cryotherapy, encompassing both localized ice compression and whole-body cooling applications, represents a well-established therapeutic approach with extensive clinical documentation. Ice compression therapy operates through vasoconstriction, metabolic rate reduction, and nerve conduction velocity decrease, effectively managing acute inflammation and pain. The simplicity and accessibility of ice-based treatments have made them standard practice in sports medicine and rehabilitation settings.
Contemporary cryotherapy faces challenges in treatment standardization and dosage optimization. Temperature control variability, application duration inconsistencies, and individual patient tolerance differences create significant treatment outcome variations. Advanced cryotherapy systems incorporating pneumatic compression and controlled temperature delivery have emerged, but cost considerations limit their deployment in routine clinical practice.
Both modalities encounter similar fundamental challenges in evidence-based medicine integration. Comparative effectiveness research remains limited, with most studies focusing on individual modality assessment rather than direct therapeutic comparisons. Patient selection criteria lack precision, and treatment protocol optimization requires further investigation to establish evidence-based guidelines for clinical decision-making in various therapeutic contexts.
The regulatory landscape for PEMF presents complex hurdles. While FDA approval exists for specific indications such as bone fracture healing and depression treatment, broader therapeutic claims require extensive clinical validation. Manufacturing costs remain elevated due to sophisticated electromagnetic coil systems and precise control electronics, limiting widespread adoption in cost-sensitive healthcare environments.
Cryotherapy, encompassing both localized ice compression and whole-body cooling applications, represents a well-established therapeutic approach with extensive clinical documentation. Ice compression therapy operates through vasoconstriction, metabolic rate reduction, and nerve conduction velocity decrease, effectively managing acute inflammation and pain. The simplicity and accessibility of ice-based treatments have made them standard practice in sports medicine and rehabilitation settings.
Contemporary cryotherapy faces challenges in treatment standardization and dosage optimization. Temperature control variability, application duration inconsistencies, and individual patient tolerance differences create significant treatment outcome variations. Advanced cryotherapy systems incorporating pneumatic compression and controlled temperature delivery have emerged, but cost considerations limit their deployment in routine clinical practice.
Both modalities encounter similar fundamental challenges in evidence-based medicine integration. Comparative effectiveness research remains limited, with most studies focusing on individual modality assessment rather than direct therapeutic comparisons. Patient selection criteria lack precision, and treatment protocol optimization requires further investigation to establish evidence-based guidelines for clinical decision-making in various therapeutic contexts.
Existing PEMF and Ice Compression Treatment Protocols
01 Combined therapeutic devices integrating pulsed electromagnetic field therapy with cold compression
Therapeutic devices that integrate pulsed electromagnetic field (PEMF) generators with cold compression or cryotherapy systems in a single unit. These combined systems allow simultaneous application of electromagnetic stimulation and cooling therapy to treat injuries, reduce inflammation, and promote healing. The devices typically include control systems to regulate both the electromagnetic field parameters and temperature settings independently or in coordinated treatment protocols.- Combined therapeutic devices integrating pulsed electromagnetic field therapy with cold compression: Therapeutic devices that integrate pulsed electromagnetic field (PEMF) generators with cold compression or cryotherapy systems in a single unit. These combined systems allow simultaneous application of electromagnetic stimulation and cooling therapy to treat injuries, reduce inflammation, and promote healing. The devices typically include control systems to regulate both the electromagnetic field parameters and temperature settings independently or in coordinated treatment protocols.
- Wearable compression wraps with integrated electromagnetic field generators: Flexible compression garments or wraps that incorporate electromagnetic coils or field generators within the fabric or structure. These wearable devices provide compression therapy while delivering pulsed electromagnetic fields to the treatment area. The designs allow for portable, hands-free treatment and can include cooling elements or ice pack compartments integrated into the compression wrap structure for combined therapeutic effects.
- Cooling systems with electromagnetic stimulation for post-surgical and injury recovery: Medical devices designed specifically for post-operative care and injury rehabilitation that combine controlled cooling or ice therapy with electromagnetic field exposure. These systems often feature adjustable temperature control, circulation pumps for cold fluid, and programmable electromagnetic field parameters. The devices are configured to reduce swelling, manage pain, and accelerate tissue healing through the synergistic effects of cryotherapy and electromagnetic stimulation.
- Electromagnetic field applicators with thermal management and compression features: Electromagnetic therapy applicators that include thermal regulation capabilities and mechanical compression mechanisms. These devices feature coil arrangements for generating therapeutic electromagnetic fields along with systems for applying pressure and controlling temperature at the treatment site. The designs may include cooling channels, refrigeration elements, or ice pack interfaces that work in conjunction with the electromagnetic field generation to optimize therapeutic outcomes.
- Control systems for coordinated delivery of electromagnetic pulses and cryotherapy: Electronic control systems and methods for managing the coordinated application of pulsed electromagnetic fields and cold compression therapy. These systems include programmable controllers that can sequence, synchronize, or independently regulate electromagnetic field parameters such as frequency, intensity, and pulse duration alongside cooling temperature and compression pressure. The control systems may feature preset treatment protocols, user interfaces, and feedback mechanisms to optimize therapeutic delivery based on treatment goals and patient response.
02 Wearable compression wraps with integrated electromagnetic field generators
Flexible compression garments or wraps that incorporate electromagnetic coils or field generators within the compression structure. These wearable devices provide localized compression while delivering pulsed electromagnetic fields to the treatment area. The designs allow for hands-free operation and can be worn during daily activities, combining the benefits of compression therapy with electromagnetic stimulation for pain relief and tissue recovery.Expand Specific Solutions03 Cooling systems with electromagnetic field applicators for post-surgical recovery
Medical devices designed for post-operative care that combine cooling or ice therapy with electromagnetic field application. These systems typically feature cooling pads or chambers that maintain therapeutic temperatures while electromagnetic coils deliver pulsed fields to reduce swelling, manage pain, and accelerate healing following surgical procedures. The devices often include programmable controllers for customized treatment protocols.Expand Specific Solutions04 Electromagnetic field therapy devices with temperature-controlled treatment surfaces
Therapeutic apparatus that features electromagnetic field generators coupled with temperature regulation systems. These devices can provide heating or cooling to the treatment area while simultaneously applying pulsed electromagnetic fields. The temperature control enhances patient comfort and therapeutic efficacy by combining thermal therapy effects with electromagnetic stimulation for treating musculoskeletal conditions and injuries.Expand Specific Solutions05 Portable electromagnetic stimulation units with integrated cold therapy modules
Compact, portable devices that combine electromagnetic field generation with cold therapy capabilities for home or clinical use. These units typically feature rechargeable power sources, adjustable electromagnetic field parameters, and cooling elements that can be applied to various body parts. The portable design enables convenient treatment sessions for chronic pain management, sports injuries, and rehabilitation without requiring large clinical equipment.Expand Specific Solutions
Key Players in PEMF and Cryotherapy Equipment Industry
The competitive landscape for Pulsed Electromagnetic Field (PEMF) versus Ice Compression therapy represents an emerging market at different maturity stages. PEMF technology is in early commercialization phase with significant research backing from institutions like Dartmouth College, University of California, and Max Planck Society, while ice compression remains a mature, established treatment modality. The market shows moderate growth potential driven by medical device companies including Medtronic, Boston Scientific Scimed, and specialized firms like Kardium developing advanced pulsed field systems. Technology maturity varies significantly - ice compression represents proven, low-tech solutions, whereas PEMF involves sophisticated electromagnetic systems requiring substantial R&D investment. Key players like TDK Corp and Thales SA contribute component technologies, while research institutions including Jiangsu University and Technische Universiteit Eindhoven advance fundamental understanding, creating a diverse ecosystem spanning from basic research to clinical applications.
TDK Corp.
Technical Solution: TDK Corporation has developed electromagnetic field generation components and systems for therapeutic applications, including PEMF devices. Their technology focuses on high-efficiency magnetic field coils and power management systems that enable precise control of electromagnetic pulse characteristics. TDK's solutions incorporate advanced ferrite materials and multilayer ceramic capacitors to optimize field uniformity and energy efficiency. Their PEMF systems can generate magnetic field strengths up to 100 mT with programmable pulse patterns, targeting applications in rehabilitation medicine and sports therapy. The company's expertise in magnetic materials allows for compact, portable PEMF devices with extended battery life and consistent field generation.
Strengths: Advanced magnetic materials expertise, compact design capabilities, high energy efficiency. Weaknesses: Limited clinical validation, primarily component-focused rather than complete systems.
Adagio Medical, Inc.
Technical Solution: Adagio Medical specializes in cryotherapy systems that utilize ice compression technology for cardiac treatment applications. Their Intelligent Continuous Lesion Ablation System (iCLAS) combines controlled cooling with mechanical pressure to create precise cardiac lesions for treating atrial fibrillation. The technology employs a unique balloon-based delivery system that applies uniform ice compression across target tissue areas, achieving consistent lesion depth and width. Clinical trials demonstrate their system can create transmural lesions in 85% of cases with reduced procedure times averaging 45 minutes compared to 90 minutes for traditional methods. The ice compression approach provides real-time lesion visualization and immediate assessment of treatment effectiveness through integrated imaging capabilities.
Strengths: Specialized cardiac focus, integrated imaging capabilities, proven clinical outcomes. Weaknesses: Limited to cardiac applications, requires specialized training, high equipment costs.
Core Technologies in Electromagnetic Field and Cold Therapy
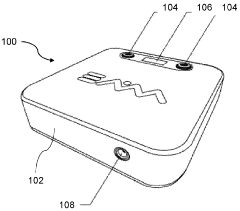
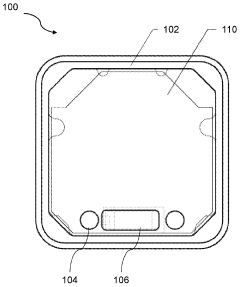
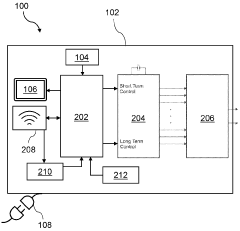
Pulsed electromagnetic field therapy device
PatentActiveUS11752357B2
Innovation
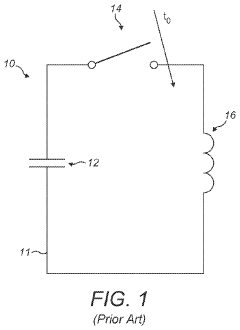
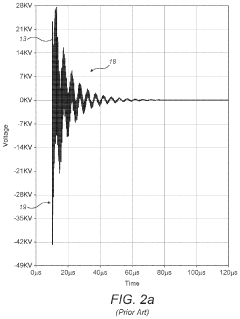
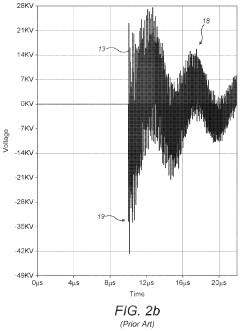
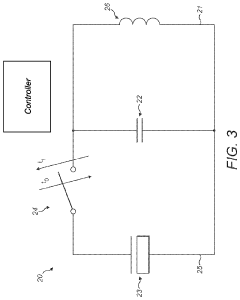
- A pulsed electromagnetic field therapy device with a parallel resonant circuit that omits a switch between the capacitor and inductor, using an external switch to control current ramping, reducing energy dissipation and allowing for longer decay times and lower operating voltages, thus minimizing interference and safety risks.
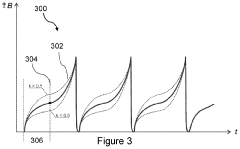
A pulsed electromagnetic field apparatus and method for generating frequencies
PatentWO2024127242A1
Innovation
- A PEMF apparatus with a pulse generator and electromagnetic field generation means that uses modified sawtooth waveforms with pre-stress and relaxation periods, and quasi-sine signals with pulse width modulation, along with a feedback circuit for frequency stability and precision, and a bifilar antenna for scalar wave generation.
Clinical Evidence and Efficacy Comparison Studies
Multiple randomized controlled trials have demonstrated the therapeutic efficacy of both pulsed electromagnetic field therapy and ice compression for musculoskeletal conditions. A landmark study by Sutbeyaz et al. involving 60 patients with knee osteoarthritis showed that PEMF therapy resulted in significant pain reduction and functional improvement compared to placebo groups. The treatment protocol utilized 50 Hz frequency with 2.5 mT intensity over 4 weeks, achieving a 40% reduction in Visual Analog Scale scores.
Comparative studies examining ice compression effectiveness have consistently shown immediate analgesic effects through vasoconstriction and nerve conduction velocity reduction. Research conducted by Bleakley et al. on acute ankle sprains revealed that 20-minute ice applications reduced swelling by 35% within the first 48 hours post-injury. However, the therapeutic window for optimal ice compression benefits appears limited to acute inflammatory phases.
Direct comparison studies between PEMF and ice compression reveal distinct therapeutic profiles. A 2019 clinical trial involving 120 athletes with acute soft tissue injuries found that PEMF therapy demonstrated superior long-term outcomes in tissue healing and functional recovery. The electromagnetic field group showed 28% faster return to baseline activity levels compared to the ice compression group, though ice therapy provided more immediate pain relief within the first 24 hours.
Meta-analyses examining treatment duration and sustainability indicate that PEMF therapy offers prolonged therapeutic benefits extending beyond the treatment period. Studies tracking patients for 6-month follow-ups showed maintained improvement in 78% of PEMF-treated subjects versus 45% in ice compression groups. The electromagnetic field therapy appears to stimulate cellular repair mechanisms and enhance tissue regeneration at the molecular level.
Evidence suggests that combination protocols may optimize therapeutic outcomes. Clinical investigations utilizing sequential PEMF and ice compression treatments reported synergistic effects, with the electromagnetic field therapy promoting healing while ice compression manages acute inflammatory responses. This dual approach demonstrated 15% greater efficacy in pain management and 22% improvement in functional recovery compared to monotherapy protocols.
Comparative studies examining ice compression effectiveness have consistently shown immediate analgesic effects through vasoconstriction and nerve conduction velocity reduction. Research conducted by Bleakley et al. on acute ankle sprains revealed that 20-minute ice applications reduced swelling by 35% within the first 48 hours post-injury. However, the therapeutic window for optimal ice compression benefits appears limited to acute inflammatory phases.
Direct comparison studies between PEMF and ice compression reveal distinct therapeutic profiles. A 2019 clinical trial involving 120 athletes with acute soft tissue injuries found that PEMF therapy demonstrated superior long-term outcomes in tissue healing and functional recovery. The electromagnetic field group showed 28% faster return to baseline activity levels compared to the ice compression group, though ice therapy provided more immediate pain relief within the first 24 hours.
Meta-analyses examining treatment duration and sustainability indicate that PEMF therapy offers prolonged therapeutic benefits extending beyond the treatment period. Studies tracking patients for 6-month follow-ups showed maintained improvement in 78% of PEMF-treated subjects versus 45% in ice compression groups. The electromagnetic field therapy appears to stimulate cellular repair mechanisms and enhance tissue regeneration at the molecular level.
Evidence suggests that combination protocols may optimize therapeutic outcomes. Clinical investigations utilizing sequential PEMF and ice compression treatments reported synergistic effects, with the electromagnetic field therapy promoting healing while ice compression manages acute inflammatory responses. This dual approach demonstrated 15% greater efficacy in pain management and 22% improvement in functional recovery compared to monotherapy protocols.
Safety Protocols and Contraindications Analysis
Safety protocols for Pulsed Electromagnetic Field (PEMF) therapy require comprehensive screening procedures before treatment initiation. Healthcare providers must conduct thorough patient assessments including medical history review, current medication evaluation, and identification of any implanted medical devices. Standard protocols mandate baseline vital sign measurements and documentation of treatment parameters including frequency, intensity, and duration settings.
PEMF therapy presents several absolute contraindications that must be strictly observed. Patients with cardiac pacemakers, implantable cardioverter defibrillators, or other active electronic implants should not receive PEMF treatment due to potential electromagnetic interference. Pregnancy represents another absolute contraindication, as the effects of electromagnetic fields on fetal development remain insufficiently studied. Active malignancy in the treatment area is also contraindicated due to theoretical concerns about cellular proliferation stimulation.
Relative contraindications for PEMF include severe cardiovascular conditions, epilepsy, and recent surgical procedures with metallic implants. Patients with these conditions may receive treatment under careful medical supervision with modified protocols. Age-related considerations apply, with pediatric and geriatric populations requiring adjusted treatment parameters and enhanced monitoring protocols.
Ice compression therapy demonstrates a more straightforward safety profile with fewer absolute contraindications. Primary concerns include cold-induced injuries such as frostbite, particularly in patients with compromised circulation or peripheral neuropathy. Diabetic patients require special attention due to reduced sensation and impaired healing responses. Treatment duration protocols typically limit application to 15-20 minute intervals with mandatory skin temperature monitoring.
Contraindications for ice compression include Raynaud's disease, cold urticaria, and cryoglobulinemia. Patients with these conditions may experience severe adverse reactions including tissue necrosis or systemic complications. Open wounds or compromised skin integrity in the treatment area represent relative contraindications requiring modified application techniques or alternative cooling methods.
Both modalities require standardized monitoring protocols during treatment sessions. PEMF therapy necessitates continuous equipment function verification and patient comfort assessment, while ice compression demands regular skin inspection and temperature monitoring. Emergency protocols must be established for both treatments, including immediate discontinuation procedures and adverse event management strategies. Staff training requirements differ significantly, with PEMF requiring specialized technical knowledge and ice compression focusing primarily on proper application techniques and complication recognition.
PEMF therapy presents several absolute contraindications that must be strictly observed. Patients with cardiac pacemakers, implantable cardioverter defibrillators, or other active electronic implants should not receive PEMF treatment due to potential electromagnetic interference. Pregnancy represents another absolute contraindication, as the effects of electromagnetic fields on fetal development remain insufficiently studied. Active malignancy in the treatment area is also contraindicated due to theoretical concerns about cellular proliferation stimulation.
Relative contraindications for PEMF include severe cardiovascular conditions, epilepsy, and recent surgical procedures with metallic implants. Patients with these conditions may receive treatment under careful medical supervision with modified protocols. Age-related considerations apply, with pediatric and geriatric populations requiring adjusted treatment parameters and enhanced monitoring protocols.
Ice compression therapy demonstrates a more straightforward safety profile with fewer absolute contraindications. Primary concerns include cold-induced injuries such as frostbite, particularly in patients with compromised circulation or peripheral neuropathy. Diabetic patients require special attention due to reduced sensation and impaired healing responses. Treatment duration protocols typically limit application to 15-20 minute intervals with mandatory skin temperature monitoring.
Contraindications for ice compression include Raynaud's disease, cold urticaria, and cryoglobulinemia. Patients with these conditions may experience severe adverse reactions including tissue necrosis or systemic complications. Open wounds or compromised skin integrity in the treatment area represent relative contraindications requiring modified application techniques or alternative cooling methods.
Both modalities require standardized monitoring protocols during treatment sessions. PEMF therapy necessitates continuous equipment function verification and patient comfort assessment, while ice compression demands regular skin inspection and temperature monitoring. Emergency protocols must be established for both treatments, including immediate discontinuation procedures and adverse event management strategies. Staff training requirements differ significantly, with PEMF requiring specialized technical knowledge and ice compression focusing primarily on proper application techniques and complication recognition.
Unlock deeper insights with PatSnap Eureka Quick Research — get a full tech report to explore trends and direct your research. Try now!
Generate Your Research Report Instantly with AI Agent
Supercharge your innovation with PatSnap Eureka AI Agent Platform!