Quantifying Posterior Enhancement by Evaluating Echogenicity
JAN 20, 20269 MIN READ
Generate Your Research Report Instantly with AI Agent
PatSnap Eureka helps you evaluate technical feasibility & market potential.
Posterior Enhancement Quantification Background and Objectives
Posterior acoustic enhancement represents a fundamental ultrasound imaging phenomenon characterized by increased echogenicity in tissues located behind structures with low acoustic attenuation. This artifact occurs when ultrasound waves traverse through fluid-filled or homogeneous structures, resulting in relatively stronger signal intensity in the posterior region compared to adjacent tissues at the same depth. While traditionally recognized as a qualitative diagnostic feature in clinical ultrasound interpretation, the systematic quantification of posterior enhancement has emerged as a critical research frontier with significant implications for tissue characterization and lesion differentiation.
The historical evolution of posterior enhancement assessment has been predominantly subjective, relying on visual interpretation by experienced sonographers and radiologists. This qualitative approach, though clinically valuable, introduces inherent variability and limits reproducibility across different operators and imaging systems. The absence of standardized quantitative metrics has constrained the integration of posterior enhancement characteristics into computer-aided diagnosis systems and artificial intelligence algorithms, which increasingly demand objective, numerical parameters for optimal performance.
The primary objective of quantifying posterior enhancement through echogenicity evaluation is to establish reproducible, operator-independent metrics that can objectively measure the degree of acoustic transmission through tissues. This quantification aims to transform a subjective visual impression into measurable parameters that can be standardized across different ultrasound platforms, imaging protocols, and clinical settings. By developing robust quantitative frameworks, researchers seek to enhance diagnostic accuracy in distinguishing benign from malignant lesions, particularly in breast, thyroid, and liver imaging applications.
Furthermore, quantitative posterior enhancement assessment holds promise for advancing tissue characterization beyond conventional B-mode imaging. The degree of posterior enhancement correlates with tissue composition, fluid content, and structural organization, providing complementary information to other quantitative ultrasound techniques such as elastography and attenuation imaging. Establishing validated quantification methodologies will enable integration of posterior enhancement metrics into multiparametric diagnostic algorithms, potentially improving sensitivity and specificity in detecting pathological conditions while reducing unnecessary biopsies and invasive procedures.
The historical evolution of posterior enhancement assessment has been predominantly subjective, relying on visual interpretation by experienced sonographers and radiologists. This qualitative approach, though clinically valuable, introduces inherent variability and limits reproducibility across different operators and imaging systems. The absence of standardized quantitative metrics has constrained the integration of posterior enhancement characteristics into computer-aided diagnosis systems and artificial intelligence algorithms, which increasingly demand objective, numerical parameters for optimal performance.
The primary objective of quantifying posterior enhancement through echogenicity evaluation is to establish reproducible, operator-independent metrics that can objectively measure the degree of acoustic transmission through tissues. This quantification aims to transform a subjective visual impression into measurable parameters that can be standardized across different ultrasound platforms, imaging protocols, and clinical settings. By developing robust quantitative frameworks, researchers seek to enhance diagnostic accuracy in distinguishing benign from malignant lesions, particularly in breast, thyroid, and liver imaging applications.
Furthermore, quantitative posterior enhancement assessment holds promise for advancing tissue characterization beyond conventional B-mode imaging. The degree of posterior enhancement correlates with tissue composition, fluid content, and structural organization, providing complementary information to other quantitative ultrasound techniques such as elastography and attenuation imaging. Establishing validated quantification methodologies will enable integration of posterior enhancement metrics into multiparametric diagnostic algorithms, potentially improving sensitivity and specificity in detecting pathological conditions while reducing unnecessary biopsies and invasive procedures.
Clinical Demand for Echogenicity Assessment
Echogenicity assessment plays a critical role in modern ultrasound imaging, particularly in the evaluation of posterior acoustic enhancement, which serves as a key diagnostic indicator for characterizing tissue composition and pathology. The clinical demand for accurate and quantitative echogenicity evaluation has grown substantially as healthcare providers seek to improve diagnostic precision, reduce inter-observer variability, and enhance patient outcomes across multiple medical specialties.
In oncology and breast imaging, posterior enhancement patterns are essential for differentiating benign from malignant lesions. Cystic structures typically exhibit strong posterior enhancement due to minimal sound attenuation, while solid masses demonstrate variable patterns that correlate with tissue cellularity and vascularity. Radiologists rely heavily on these acoustic signatures to guide biopsy decisions and treatment planning, yet subjective visual assessment remains prone to inconsistency and interpretation errors.
Abdominal and pelvic imaging similarly depends on echogenicity evaluation for characterizing liver lesions, renal masses, and gynecological abnormalities. Hepatic hemangiomas, focal nodular hyperplasia, and hepatocellular carcinomas each present distinct posterior acoustic behaviors that inform differential diagnosis. The ability to quantify these differences objectively would significantly enhance diagnostic confidence and facilitate earlier detection of pathological changes.
Musculoskeletal ultrasound applications also demonstrate substantial clinical need for standardized echogenicity assessment. Evaluation of tendon integrity, muscle pathology, and joint effusions requires precise characterization of tissue acoustic properties. Quantitative metrics would enable more reliable monitoring of treatment response and disease progression in conditions such as tendinopathy and inflammatory arthritis.
The increasing adoption of point-of-care ultrasound across emergency medicine, critical care, and primary care settings has further amplified the demand for objective echogenicity assessment tools. Non-specialist operators require standardized, reproducible methods to interpret acoustic phenomena accurately without extensive training in subjective pattern recognition. Automated or semi-automated quantification systems could democratize access to high-quality ultrasound interpretation while maintaining diagnostic accuracy.
Current limitations in subjective assessment methods, including operator dependency, equipment variability, and lack of standardized reporting frameworks, underscore the urgent clinical need for robust quantitative approaches to posterior enhancement evaluation. Such advancements would support evidence-based decision-making, facilitate multi-center research collaboration, and ultimately improve patient care quality across diverse clinical contexts.
In oncology and breast imaging, posterior enhancement patterns are essential for differentiating benign from malignant lesions. Cystic structures typically exhibit strong posterior enhancement due to minimal sound attenuation, while solid masses demonstrate variable patterns that correlate with tissue cellularity and vascularity. Radiologists rely heavily on these acoustic signatures to guide biopsy decisions and treatment planning, yet subjective visual assessment remains prone to inconsistency and interpretation errors.
Abdominal and pelvic imaging similarly depends on echogenicity evaluation for characterizing liver lesions, renal masses, and gynecological abnormalities. Hepatic hemangiomas, focal nodular hyperplasia, and hepatocellular carcinomas each present distinct posterior acoustic behaviors that inform differential diagnosis. The ability to quantify these differences objectively would significantly enhance diagnostic confidence and facilitate earlier detection of pathological changes.
Musculoskeletal ultrasound applications also demonstrate substantial clinical need for standardized echogenicity assessment. Evaluation of tendon integrity, muscle pathology, and joint effusions requires precise characterization of tissue acoustic properties. Quantitative metrics would enable more reliable monitoring of treatment response and disease progression in conditions such as tendinopathy and inflammatory arthritis.
The increasing adoption of point-of-care ultrasound across emergency medicine, critical care, and primary care settings has further amplified the demand for objective echogenicity assessment tools. Non-specialist operators require standardized, reproducible methods to interpret acoustic phenomena accurately without extensive training in subjective pattern recognition. Automated or semi-automated quantification systems could democratize access to high-quality ultrasound interpretation while maintaining diagnostic accuracy.
Current limitations in subjective assessment methods, including operator dependency, equipment variability, and lack of standardized reporting frameworks, underscore the urgent clinical need for robust quantitative approaches to posterior enhancement evaluation. Such advancements would support evidence-based decision-making, facilitate multi-center research collaboration, and ultimately improve patient care quality across diverse clinical contexts.
Current Challenges in Posterior Enhancement Measurement
Posterior acoustic enhancement remains one of the most challenging phenomena to quantify objectively in ultrasound imaging, despite its widespread recognition as a diagnostic feature. The primary difficulty stems from the inherent variability in ultrasound systems, imaging parameters, and tissue characteristics that influence echogenicity measurements. Current methodologies lack standardized protocols for defining the region of interest behind suspected lesions, leading to inconsistent measurements across different operators and institutions. The selection of appropriate reference regions for comparison introduces significant subjectivity, as there is no consensus on whether adjacent tissues, contralateral structures, or predefined depth-matched areas should serve as baseline controls.
Technical limitations of existing ultrasound equipment further complicate accurate quantification. Time-gain compensation settings, which are routinely adjusted during scanning to optimize image quality, directly affect the intensity values in posterior regions, making raw pixel intensity measurements unreliable without proper normalization. Additionally, beam focusing characteristics and acoustic attenuation properties vary significantly across different transducer frequencies and imaging depths, introducing systematic biases that are difficult to compensate for retrospectively.
The heterogeneous nature of biological tissues presents another fundamental challenge. Variations in tissue composition, fat content, and structural organization create baseline echogenicity differences that must be distinguished from true posterior enhancement effects. This becomes particularly problematic when evaluating small lesions or those located in acoustically complex environments where multiple tissue interfaces contribute to the overall echo pattern.
Current image processing algorithms struggle to separate genuine posterior enhancement from artifacts such as reverberation, side lobe effects, and speckle noise. These confounding factors can mimic or mask true enhancement patterns, reducing diagnostic specificity. Moreover, the lack of validated quantitative metrics that correlate reliably with clinical outcomes limits the translation of measurement techniques into routine practice.
The absence of comprehensive reference databases containing standardized posterior enhancement measurements across diverse pathologies further impedes progress. Without established threshold values or classification criteria derived from large-scale studies, clinicians cannot confidently interpret quantitative results, maintaining reliance on subjective visual assessment despite its known limitations in reproducibility and diagnostic accuracy.
Technical limitations of existing ultrasound equipment further complicate accurate quantification. Time-gain compensation settings, which are routinely adjusted during scanning to optimize image quality, directly affect the intensity values in posterior regions, making raw pixel intensity measurements unreliable without proper normalization. Additionally, beam focusing characteristics and acoustic attenuation properties vary significantly across different transducer frequencies and imaging depths, introducing systematic biases that are difficult to compensate for retrospectively.
The heterogeneous nature of biological tissues presents another fundamental challenge. Variations in tissue composition, fat content, and structural organization create baseline echogenicity differences that must be distinguished from true posterior enhancement effects. This becomes particularly problematic when evaluating small lesions or those located in acoustically complex environments where multiple tissue interfaces contribute to the overall echo pattern.
Current image processing algorithms struggle to separate genuine posterior enhancement from artifacts such as reverberation, side lobe effects, and speckle noise. These confounding factors can mimic or mask true enhancement patterns, reducing diagnostic specificity. Moreover, the lack of validated quantitative metrics that correlate reliably with clinical outcomes limits the translation of measurement techniques into routine practice.
The absence of comprehensive reference databases containing standardized posterior enhancement measurements across diverse pathologies further impedes progress. Without established threshold values or classification criteria derived from large-scale studies, clinicians cannot confidently interpret quantitative results, maintaining reliance on subjective visual assessment despite its known limitations in reproducibility and diagnostic accuracy.
Existing Echogenicity Quantification Methods
01 Contrast agents for enhancing ultrasound echogenicity
Ultrasound contrast agents are formulated to enhance echogenicity in imaging by introducing microbubbles or nanoparticles that reflect ultrasound waves more effectively. These agents improve visualization of blood vessels, tissues, and organs by increasing the acoustic impedance mismatch between different tissue types. The contrast agents can be gas-filled microbubbles, lipid-based formulations, or polymer-encapsulated particles that provide enhanced signal intensity and improved diagnostic accuracy.- Contrast agents for enhancing ultrasound echogenicity: Ultrasound contrast agents are formulated to enhance echogenicity in imaging by introducing microbubbles or nanoparticles that reflect ultrasound waves more effectively. These agents improve visualization of blood vessels, tissues, and organs by increasing the acoustic impedance mismatch between different tissue types. The contrast agents can be gas-filled microbubbles, lipid-based formulations, or polymer-encapsulated particles that provide enhanced signal intensity and improved diagnostic accuracy.
- Image processing techniques for echogenicity analysis: Advanced image processing algorithms are employed to analyze and quantify echogenicity patterns in ultrasound images. These techniques include texture analysis, histogram evaluation, and machine learning-based classification methods to differentiate between hypoechoic, isoechoic, and hyperechoic regions. Signal processing methods enhance the contrast and resolution of ultrasound images, enabling better identification of tissue characteristics and pathological conditions based on their echogenic properties.
- Transducer design and frequency optimization for echogenicity detection: Ultrasound transducer configurations and frequency selection play a crucial role in optimizing echogenicity detection. Higher frequency transducers provide better resolution for superficial structures, while lower frequencies offer deeper penetration. Multi-frequency transducers and adaptive beamforming techniques are utilized to optimize the detection of echogenic structures across different tissue depths. Transducer array designs and focusing mechanisms are engineered to maximize the reflection of ultrasound waves from tissues with varying acoustic properties.
- Tissue characterization based on echogenic properties: Echogenicity serves as a fundamental parameter for tissue characterization in diagnostic ultrasound. Different tissues exhibit distinct echogenic patterns based on their cellular composition, density, and structural organization. Quantitative ultrasound techniques measure backscatter coefficients and attenuation properties to classify tissues as hyperechoic, hypoechoic, or anechoic. These characterization methods are applied in identifying normal versus pathological tissues, including tumors, cysts, and inflammatory lesions.
- Three-dimensional and real-time echogenicity mapping: Three-dimensional ultrasound imaging systems provide volumetric assessment of echogenic structures, enabling comprehensive spatial analysis of tissue properties. Real-time imaging capabilities allow dynamic evaluation of echogenicity changes during physiological processes or interventional procedures. Advanced rendering techniques and volume reconstruction algorithms create detailed maps of echogenic distributions, facilitating improved diagnostic interpretation and treatment planning. These systems integrate temporal and spatial information to track changes in tissue echogenicity over time.
02 Image processing techniques for echogenicity analysis
Advanced image processing algorithms are employed to analyze and quantify echogenicity patterns in ultrasound images. These techniques include texture analysis, histogram evaluation, and machine learning-based classification methods to differentiate between hypoechoic, isoechoic, and hyperechoic regions. The processing methods enable automated detection of abnormalities, tissue characterization, and improved diagnostic interpretation by enhancing contrast resolution and reducing artifacts.Expand Specific Solutions03 Transducer design and frequency optimization for echogenicity
Ultrasound transducer configurations and frequency selection play a critical role in optimizing echogenicity detection. Higher frequency transducers provide better spatial resolution for superficial structures, while lower frequencies offer deeper penetration. Multi-frequency and broadband transducers enable adaptive imaging based on tissue depth and composition. Transducer design innovations include phased array configurations, harmonic imaging capabilities, and beam-forming technologies that enhance echo signal quality and tissue differentiation.Expand Specific Solutions04 Tissue-specific echogenicity characterization methods
Different tissue types exhibit characteristic echogenicity patterns that can be used for diagnostic purposes. Methods for characterizing tissue-specific echogenicity include quantitative ultrasound parameters, elastography integration, and comparative analysis of echo intensity across different anatomical regions. These approaches enable differentiation between normal and pathological tissues, assessment of tissue composition, and monitoring of disease progression based on changes in acoustic properties.Expand Specific Solutions05 Real-time echogenicity enhancement and visualization systems
Real-time imaging systems incorporate dynamic echogenicity enhancement features to improve visualization during diagnostic procedures. These systems utilize adaptive gain control, dynamic range optimization, and compound imaging techniques to maximize echo signal detection. Integration of color-coded echogenicity mapping, three-dimensional reconstruction, and fusion imaging with other modalities provides comprehensive visualization tools for clinical applications, enabling better guidance during interventional procedures and improved diagnostic confidence.Expand Specific Solutions
Major Players in Ultrasound Imaging Technology
The field of quantifying posterior enhancement through echogenicity evaluation represents an emerging area within medical ultrasound imaging, currently in its early-to-mid development stage. The competitive landscape encompasses diverse players spanning medical device manufacturers like Boston Scientific Scimed and Carestream Health, technology giants such as Huawei Technologies and Baidu Online Network Technology, specialized AI-driven healthcare companies including Shanghai Shenzhi Information Technology, and leading research institutions like Massachusetts General Hospital and Huazhong University of Science & Technology. Market potential remains substantial as ultrasound imaging continues expanding globally, particularly in point-of-care diagnostics. Technology maturity varies significantly across participants, with established medical device companies leveraging proven imaging platforms while newer entrants like Shanghai Shenzhi focus on AI-enhanced diagnostic capabilities, indicating a transitional phase toward intelligent, automated echogenicity assessment systems.
Boston Scientific Scimed, Inc.
Technical Solution: Boston Scientific has developed advanced ultrasound imaging technologies incorporating echogenicity evaluation methods for assessing posterior acoustic enhancement in medical devices and tissue characterization. Their approach utilizes quantitative analysis of echo signal intensity in regions posterior to structures of interest, employing automated algorithms to measure the differential echogenicity between target areas and surrounding tissues. The technology integrates real-time signal processing to calculate enhancement ratios and generate parametric maps that visualize posterior shadowing or enhancement patterns. This is particularly applied in their intravascular ultrasound (IVUS) and endoscopic ultrasound systems for identifying tissue composition, detecting calcifications, and characterizing lesions based on their acoustic properties. The quantification methodology helps clinicians differentiate between fluid-filled structures, solid masses, and calcified regions by analyzing the transmission characteristics of ultrasound waves through different tissue types.
Strengths: Established clinical validation in cardiovascular and gastrointestinal applications with FDA-approved devices; robust integration with existing ultrasound platforms. Weaknesses: Limited applicability in highly attenuating tissues; requires standardized imaging protocols for consistent quantification across different operators and systems.
Carestream Health, Inc.
Technical Solution: Carestream Health has implemented posterior enhancement quantification techniques primarily in their digital radiography and ultrasound imaging solutions. Their technology employs computational algorithms that analyze grayscale intensity distributions in posterior regions relative to anterior reference zones. The system automatically identifies regions of interest and calculates enhancement indices based on pixel intensity ratios, compensating for depth-dependent attenuation. Their approach includes machine learning components trained on large datasets to recognize characteristic enhancement patterns associated with cystic lesions, fluid collections, and other pathological conditions. The quantification metrics are integrated into their PACS workflow, providing radiologists with objective numerical values alongside traditional B-mode images. This technology is designed to reduce inter-observer variability in ultrasound interpretation and support standardized reporting protocols.
Strengths: Seamless integration with hospital information systems and existing radiology workflows; user-friendly interface with automated measurement tools. Weaknesses: Performance may vary with different ultrasound frequencies and imaging depths; requires adequate training data for machine learning optimization in specialized applications.
Key Innovations in Posterior Enhancement Algorithms
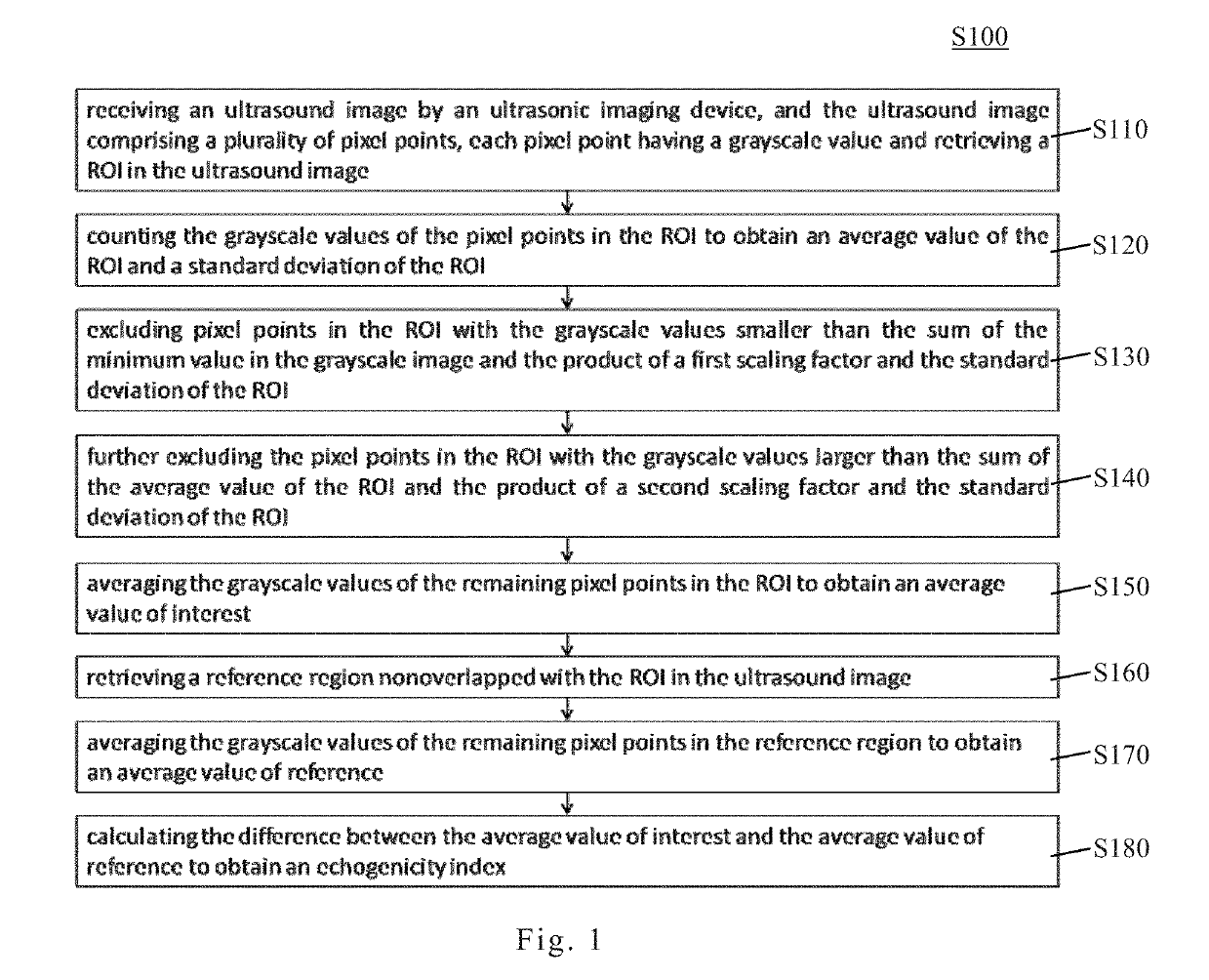
Echogenicity quantification method and calibration method for ultrasonic device using echogenicity index
PatentActiveUS10249037B2
Innovation
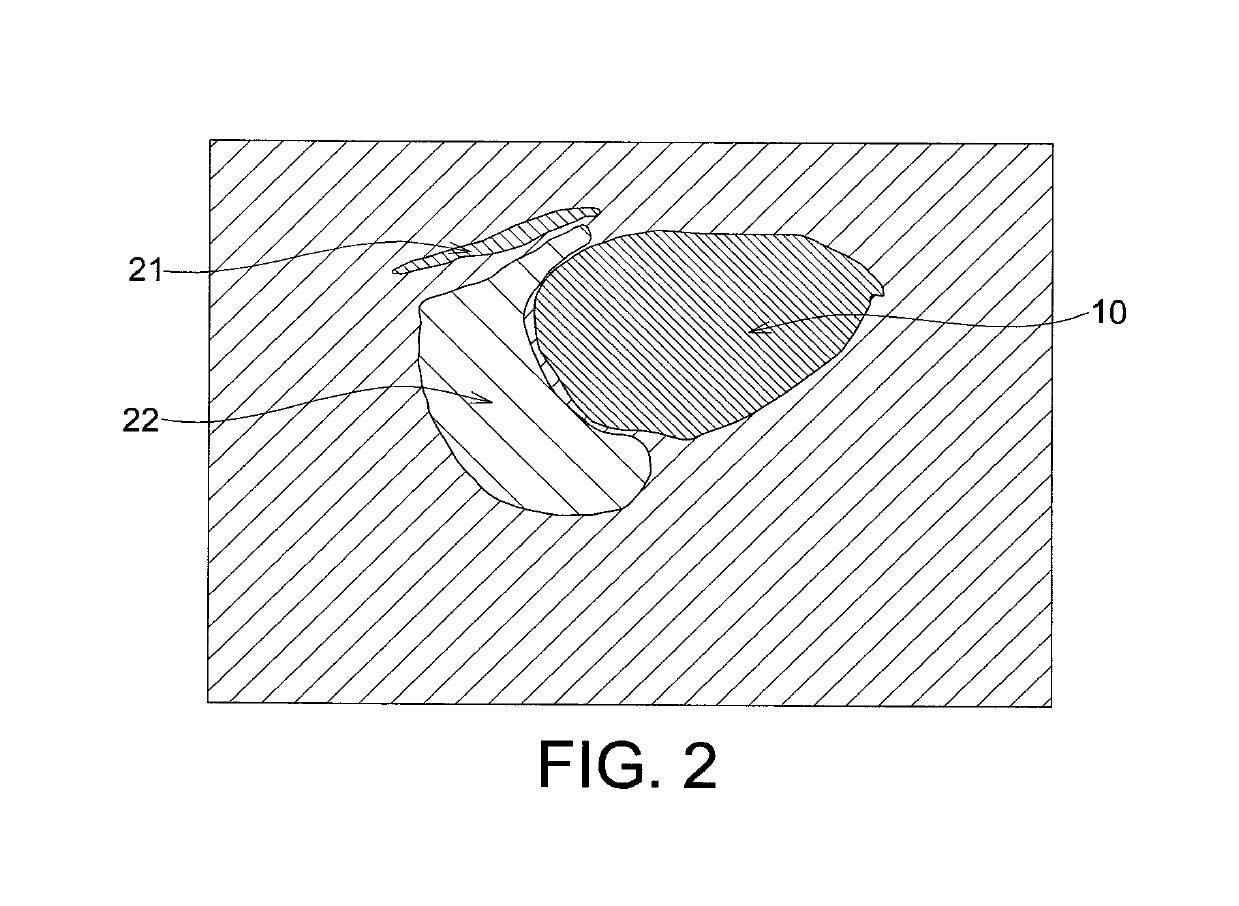
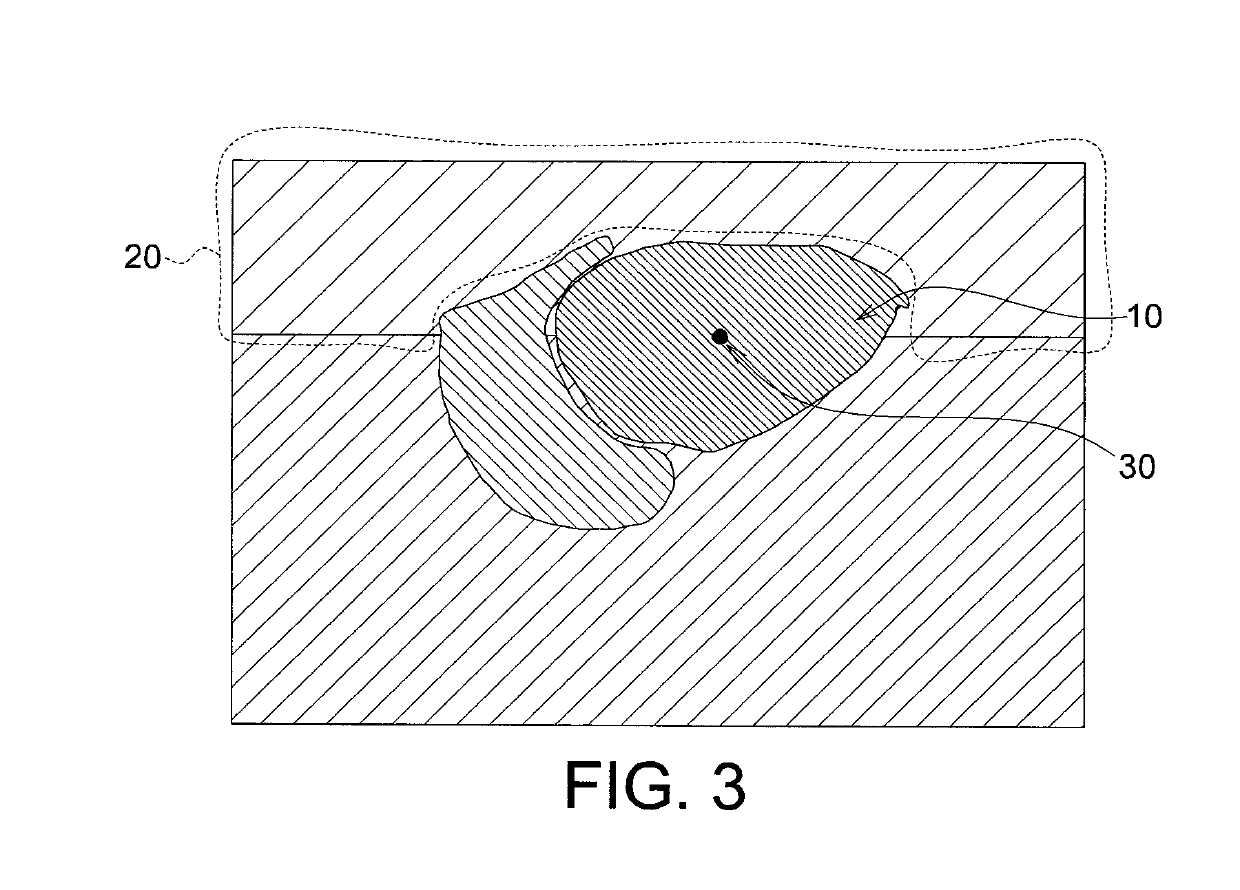
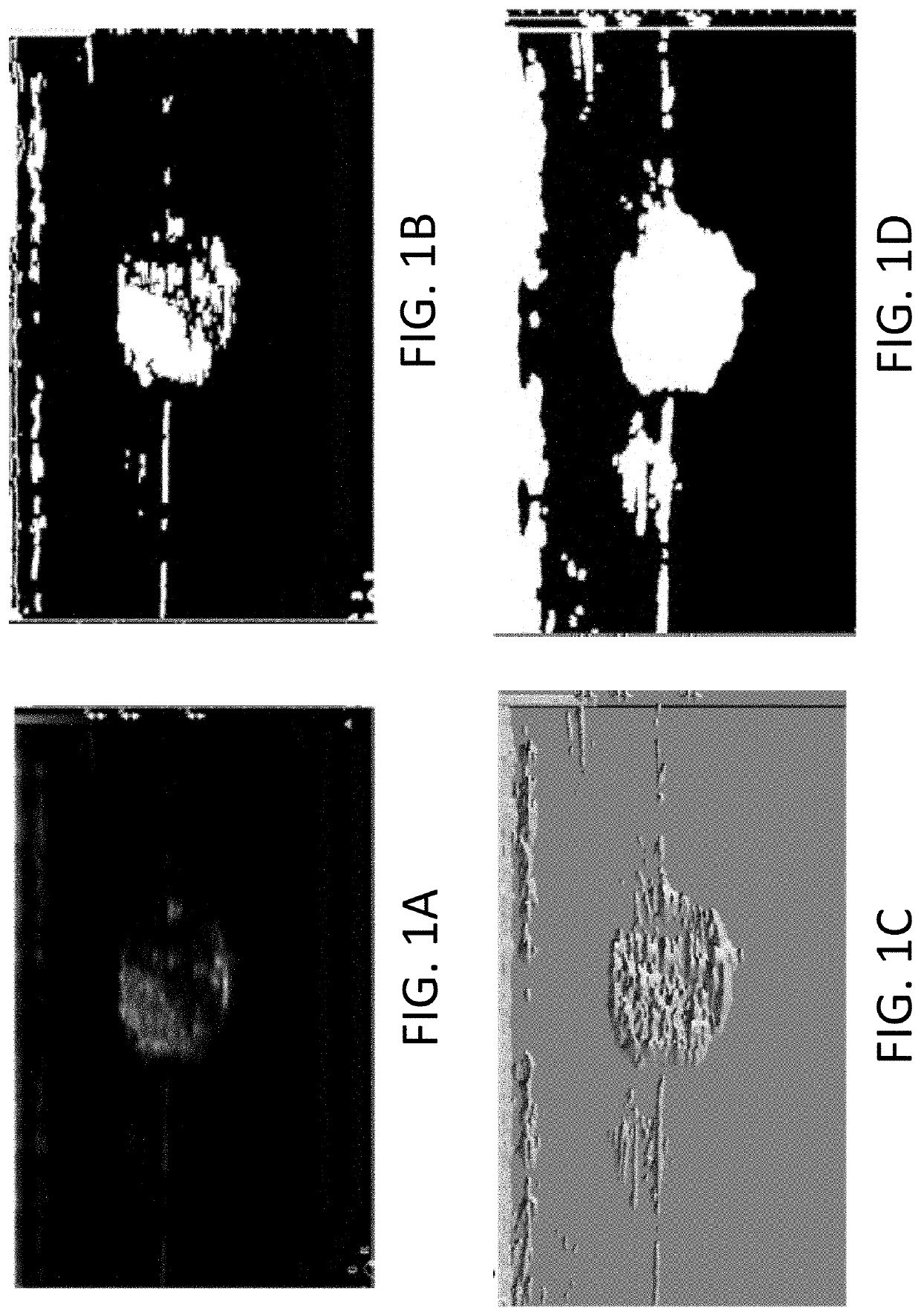
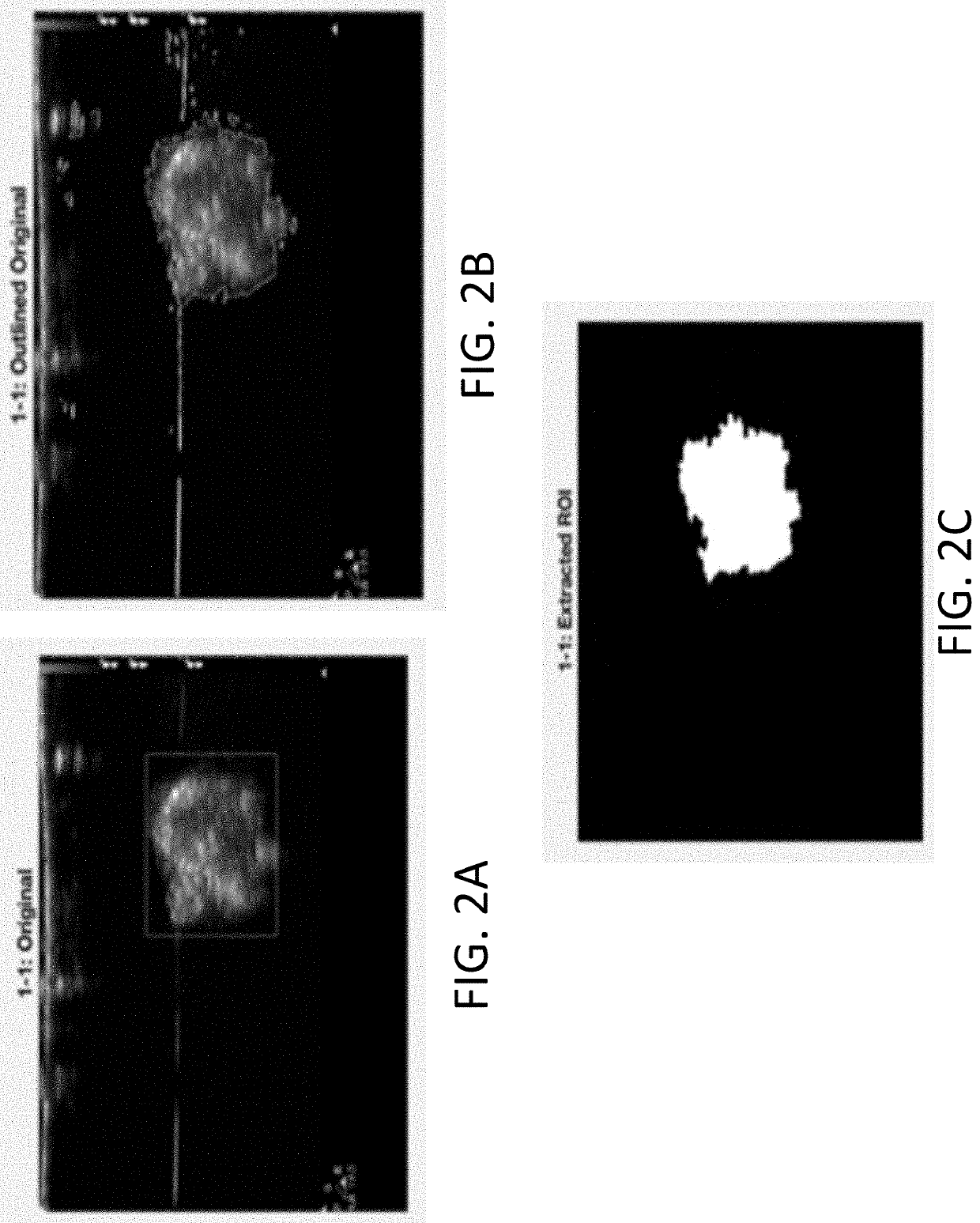
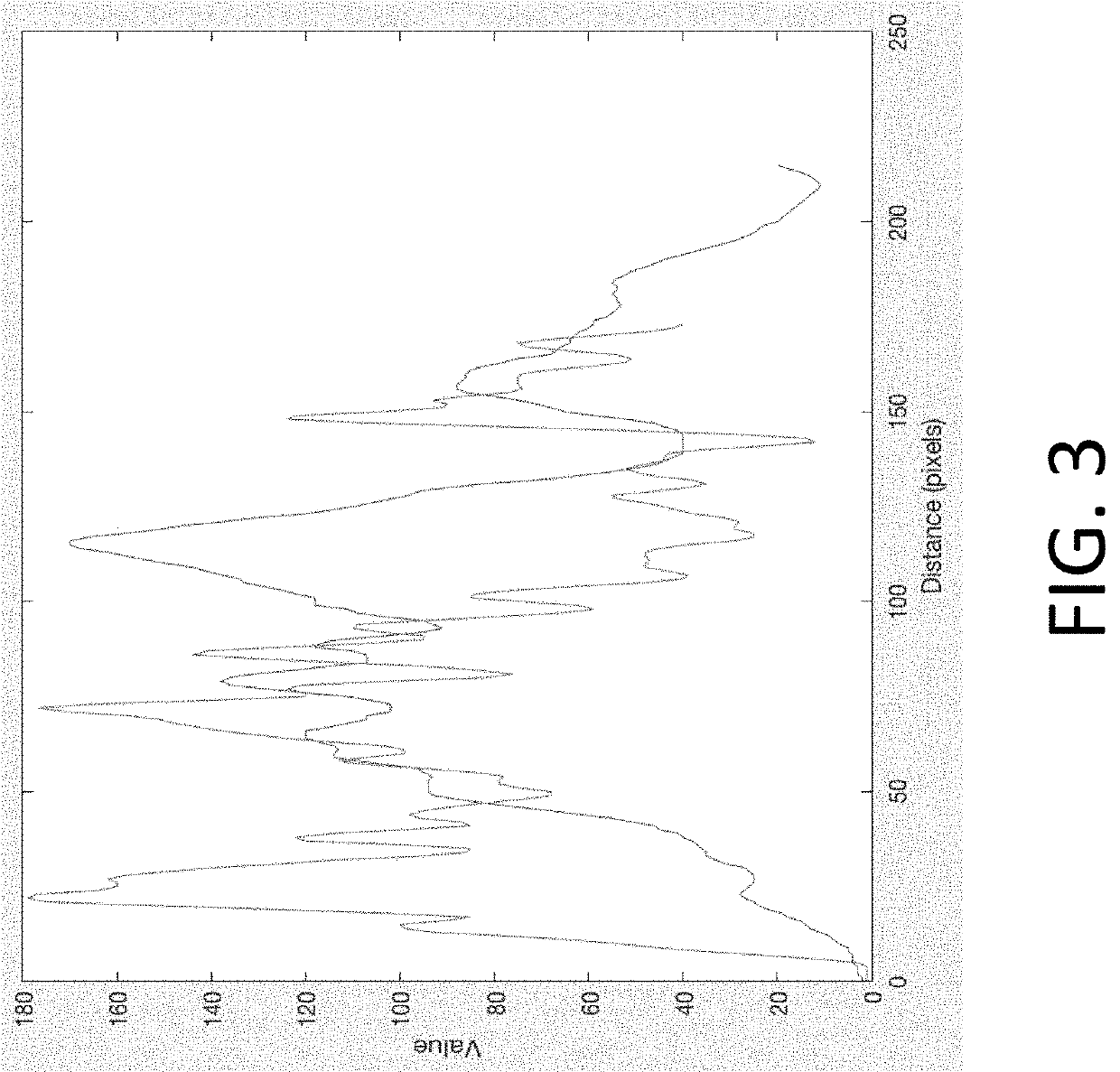
- An echogenicity quantification method that calculates an echogenicity index by averaging and normalizing grayscale values within a Region Of Interest (ROI) and a reference region, excluding outliers, to provide an objective and consistent measure across different ultrasonic devices and operators.
Systems and methods for automated image recognition of implants and compositions with long-lasting echogenicity
PatentInactiveUS20220015742A1
Innovation
- The development of systems and methods for automatically detecting and analyzing bodily implants using algorithms that extract Regions of Interest (ROIs) from medical images, combined with the use of non-gas ultrasound contrast agents that maintain echogenicity for extended periods, allowing for long-term visualization and tracking of implants.
Medical Imaging Standards and Regulatory Requirements
The quantification of posterior enhancement through echogenicity evaluation in medical ultrasound imaging operates within a complex framework of standards and regulatory requirements that ensure diagnostic accuracy, patient safety, and clinical reliability. These requirements span multiple jurisdictions and are enforced by various regulatory bodies, each establishing specific criteria for imaging equipment performance, measurement protocols, and quality assurance procedures.
In the United States, the Food and Drug Administration (FDA) regulates ultrasound devices as Class II medical devices under 21 CFR Part 892, requiring manufacturers to demonstrate substantial equivalence through 510(k) premarket notification or obtain premarket approval for novel technologies. The FDA mandates compliance with acoustic output standards, particularly the Output Display Standard (ODS) specified in Track 3 of the FDA guidance, which limits mechanical index and thermal index values to prevent tissue damage. For posterior enhancement quantification specifically, imaging systems must adhere to measurement accuracy standards that ensure reproducible echogenicity assessments across different operators and clinical settings.
Internationally, the International Electrotechnical Commission (IEC) provides comprehensive standards through IEC 60601-2-37, which specifies safety and performance requirements for ultrasound diagnostic equipment. This standard addresses acoustic output limitations, image quality metrics, and measurement precision requirements essential for quantitative echogenicity analysis. The European Union enforces these requirements through the Medical Device Regulation (MDR 2017/745), which mandates conformity assessment procedures and clinical evaluation documentation before market authorization.
Quality assurance protocols established by the American Institute of Ultrasound in Medicine (AIUM) and the American College of Radiology (ACR) provide practical guidelines for implementing posterior enhancement quantification in clinical practice. These organizations recommend regular phantom testing, calibration verification, and standardized measurement protocols to maintain consistency in echogenicity evaluation. The ACR Ultrasound Accreditation Program specifically requires documentation of quality control procedures and adherence to established imaging protocols for facilities performing quantitative ultrasound assessments.
In the United States, the Food and Drug Administration (FDA) regulates ultrasound devices as Class II medical devices under 21 CFR Part 892, requiring manufacturers to demonstrate substantial equivalence through 510(k) premarket notification or obtain premarket approval for novel technologies. The FDA mandates compliance with acoustic output standards, particularly the Output Display Standard (ODS) specified in Track 3 of the FDA guidance, which limits mechanical index and thermal index values to prevent tissue damage. For posterior enhancement quantification specifically, imaging systems must adhere to measurement accuracy standards that ensure reproducible echogenicity assessments across different operators and clinical settings.
Internationally, the International Electrotechnical Commission (IEC) provides comprehensive standards through IEC 60601-2-37, which specifies safety and performance requirements for ultrasound diagnostic equipment. This standard addresses acoustic output limitations, image quality metrics, and measurement precision requirements essential for quantitative echogenicity analysis. The European Union enforces these requirements through the Medical Device Regulation (MDR 2017/745), which mandates conformity assessment procedures and clinical evaluation documentation before market authorization.
Quality assurance protocols established by the American Institute of Ultrasound in Medicine (AIUM) and the American College of Radiology (ACR) provide practical guidelines for implementing posterior enhancement quantification in clinical practice. These organizations recommend regular phantom testing, calibration verification, and standardized measurement protocols to maintain consistency in echogenicity evaluation. The ACR Ultrasound Accreditation Program specifically requires documentation of quality control procedures and adherence to established imaging protocols for facilities performing quantitative ultrasound assessments.
AI-Driven Ultrasound Image Interpretation Advances
The integration of artificial intelligence into ultrasound imaging has catalyzed transformative advances in diagnostic accuracy and clinical workflow efficiency. Machine learning algorithms, particularly deep learning architectures, have demonstrated remarkable capabilities in automating image interpretation tasks that traditionally required extensive operator expertise. Convolutional neural networks have been successfully deployed to identify anatomical structures, detect pathological features, and quantify tissue characteristics with precision approaching or exceeding human performance levels. These AI-driven systems address longstanding challenges in ultrasound imaging, including operator dependency, inter-observer variability, and the subjective nature of image assessment.
Recent developments have focused on enhancing the interpretability and reliability of AI models in clinical ultrasound applications. Transfer learning techniques enable models trained on large datasets to be adapted for specific diagnostic tasks with limited training data. Attention mechanisms and explainable AI frameworks provide clinicians with visual insights into model decision-making processes, fostering trust and facilitating clinical adoption. Real-time inference capabilities have been achieved through model optimization and hardware acceleration, enabling immediate feedback during scanning procedures.
The application of AI to acoustic property analysis represents a particularly promising frontier. Algorithms can now automatically segment regions of interest, extract quantitative features from B-mode images, and correlate these measurements with tissue composition and pathology. Automated assessment of echogenicity patterns, texture analysis, and acoustic shadow characterization have shown clinical utility in differentiating benign from malignant lesions. Furthermore, AI systems are being developed to standardize measurements across different ultrasound platforms and imaging protocols, addressing reproducibility concerns that have historically limited quantitative ultrasound applications.
Emerging research explores multimodal integration, combining ultrasound data with clinical information, laboratory results, and other imaging modalities to generate comprehensive diagnostic assessments. Federated learning approaches enable collaborative model development across institutions while preserving patient privacy. These technological advances position AI as an essential component of next-generation ultrasound systems, promising to democratize access to expert-level image interpretation and expand the clinical utility of ultrasound across diverse healthcare settings.
Recent developments have focused on enhancing the interpretability and reliability of AI models in clinical ultrasound applications. Transfer learning techniques enable models trained on large datasets to be adapted for specific diagnostic tasks with limited training data. Attention mechanisms and explainable AI frameworks provide clinicians with visual insights into model decision-making processes, fostering trust and facilitating clinical adoption. Real-time inference capabilities have been achieved through model optimization and hardware acceleration, enabling immediate feedback during scanning procedures.
The application of AI to acoustic property analysis represents a particularly promising frontier. Algorithms can now automatically segment regions of interest, extract quantitative features from B-mode images, and correlate these measurements with tissue composition and pathology. Automated assessment of echogenicity patterns, texture analysis, and acoustic shadow characterization have shown clinical utility in differentiating benign from malignant lesions. Furthermore, AI systems are being developed to standardize measurements across different ultrasound platforms and imaging protocols, addressing reproducibility concerns that have historically limited quantitative ultrasound applications.
Emerging research explores multimodal integration, combining ultrasound data with clinical information, laboratory results, and other imaging modalities to generate comprehensive diagnostic assessments. Federated learning approaches enable collaborative model development across institutions while preserving patient privacy. These technological advances position AI as an essential component of next-generation ultrasound systems, promising to democratize access to expert-level image interpretation and expand the clinical utility of ultrasound across diverse healthcare settings.
Unlock deeper insights with PatSnap Eureka Quick Research — get a full tech report to explore trends and direct your research. Try now!
Generate Your Research Report Instantly with AI Agent
Supercharge your innovation with PatSnap Eureka AI Agent Platform!