Brain-Computer Interfaces for enhancing motor imagery-based rehabilitation
SEP 2, 20259 MIN READ
Generate Your Research Report Instantly with AI Agent
PatSnap Eureka helps you evaluate technical feasibility & market potential.
BCI Rehabilitation Technology Background and Objectives
Brain-Computer Interfaces (BCIs) represent a revolutionary technology that establishes direct communication pathways between the brain and external devices, bypassing conventional neuromuscular routes. The concept of BCIs emerged in the 1970s, but significant advancements have occurred over the past two decades due to breakthroughs in neuroscience, signal processing, and machine learning algorithms. The evolution of BCI technology has progressed from invasive methods requiring surgical implantation to non-invasive approaches utilizing electroencephalography (EEG), functional magnetic resonance imaging (fMRI), and near-infrared spectroscopy (NIRS).
Motor imagery-based rehabilitation, a therapeutic approach where patients mentally rehearse movements without physical execution, has gained substantial attention in neurorehabilitation. This technique leverages neuroplasticity—the brain's ability to reorganize neural pathways—to facilitate motor recovery. When combined with BCI technology, motor imagery rehabilitation offers unprecedented opportunities for patients with neurological disorders such as stroke, spinal cord injury, and cerebral palsy to regain motor function through targeted neural feedback.
The primary objective of BCI-enhanced motor imagery rehabilitation is to develop systems that accurately detect, interpret, and provide feedback on motor imagery signals, thereby creating closed-loop rehabilitation protocols that promote neuroplasticity and functional recovery. These systems aim to overcome limitations of conventional rehabilitation methods by providing real-time neurofeedback that reinforces neural reorganization and motor learning processes.
Current technological objectives include improving signal acquisition accuracy, developing more sophisticated algorithms for decoding neural patterns, creating more intuitive user interfaces, and designing portable, affordable BCI systems suitable for clinical and home environments. Research goals focus on enhancing the specificity of motor imagery detection, reducing signal-to-noise ratios, and developing adaptive algorithms that accommodate the variability in neural responses across different patients and over time.
Long-term objectives extend to creating personalized rehabilitation protocols that dynamically adjust to patient progress, integrating BCI systems with other rehabilitation technologies such as functional electrical stimulation and robotic assistive devices, and developing predictive models that can forecast recovery trajectories based on neural activity patterns.
The field is rapidly evolving toward more sophisticated hybrid BCI systems that combine multiple signal acquisition methods and integrate artificial intelligence to optimize rehabilitation outcomes. Future directions point toward fully implantable wireless systems with enhanced longevity and biocompatibility, as well as cloud-based platforms that enable remote monitoring and therapy adjustment.
Motor imagery-based rehabilitation, a therapeutic approach where patients mentally rehearse movements without physical execution, has gained substantial attention in neurorehabilitation. This technique leverages neuroplasticity—the brain's ability to reorganize neural pathways—to facilitate motor recovery. When combined with BCI technology, motor imagery rehabilitation offers unprecedented opportunities for patients with neurological disorders such as stroke, spinal cord injury, and cerebral palsy to regain motor function through targeted neural feedback.
The primary objective of BCI-enhanced motor imagery rehabilitation is to develop systems that accurately detect, interpret, and provide feedback on motor imagery signals, thereby creating closed-loop rehabilitation protocols that promote neuroplasticity and functional recovery. These systems aim to overcome limitations of conventional rehabilitation methods by providing real-time neurofeedback that reinforces neural reorganization and motor learning processes.
Current technological objectives include improving signal acquisition accuracy, developing more sophisticated algorithms for decoding neural patterns, creating more intuitive user interfaces, and designing portable, affordable BCI systems suitable for clinical and home environments. Research goals focus on enhancing the specificity of motor imagery detection, reducing signal-to-noise ratios, and developing adaptive algorithms that accommodate the variability in neural responses across different patients and over time.
Long-term objectives extend to creating personalized rehabilitation protocols that dynamically adjust to patient progress, integrating BCI systems with other rehabilitation technologies such as functional electrical stimulation and robotic assistive devices, and developing predictive models that can forecast recovery trajectories based on neural activity patterns.
The field is rapidly evolving toward more sophisticated hybrid BCI systems that combine multiple signal acquisition methods and integrate artificial intelligence to optimize rehabilitation outcomes. Future directions point toward fully implantable wireless systems with enhanced longevity and biocompatibility, as well as cloud-based platforms that enable remote monitoring and therapy adjustment.
Market Analysis for Motor Imagery-Based Rehabilitation Solutions
The global market for motor imagery-based rehabilitation solutions is experiencing significant growth, driven by the increasing prevalence of neurological disorders and stroke cases worldwide. According to recent market research, the neurorehabilitation devices market, which includes BCI-based rehabilitation systems, is projected to reach $3.2 billion by 2026, with a compound annual growth rate of 15.5% from 2021.
The primary market segments for motor imagery-based rehabilitation solutions include hospitals and rehabilitation centers, outpatient clinics, and home healthcare settings. Hospital-based rehabilitation services currently dominate the market share, accounting for approximately 45% of the total market value due to the availability of advanced equipment and specialized healthcare professionals.
Geographically, North America leads the market with approximately 38% share, followed by Europe at 30% and Asia-Pacific at 22%. The Asia-Pacific region is expected to witness the fastest growth due to improving healthcare infrastructure, increasing healthcare expenditure, and rising awareness about advanced rehabilitation techniques in countries like China, Japan, and India.
Key market drivers include the growing aging population worldwide, increasing incidence of stroke and traumatic brain injuries, rising healthcare expenditure, and technological advancements in BCI systems. The COVID-19 pandemic has further accelerated market growth by highlighting the importance of remote rehabilitation solutions and telehealth services.
Consumer demand patterns indicate a strong preference for non-invasive, user-friendly, and portable rehabilitation devices that can be used in home settings. There is also increasing demand for personalized rehabilitation programs that adapt to individual patient progress and needs.
Reimbursement policies significantly impact market adoption, with countries having favorable insurance coverage for neurorehabilitation showing higher adoption rates. In the United States, Medicare and private insurers have begun covering certain BCI-based therapies, which has positively influenced market growth.
The competitive landscape features both established medical device manufacturers and innovative startups. Major players include Medtronic, Abbott Laboratories, g.tec medical engineering GmbH, and Neurosky, while emerging companies like CTRL-Labs (acquired by Facebook) and Neurable are disrupting the market with novel approaches to BCI technology.
Future market trends point toward integration of artificial intelligence for more precise motor imagery detection, development of hybrid BCI systems combining multiple signal acquisition methods, and increased focus on gamification to improve patient engagement and adherence to rehabilitation protocols.
The primary market segments for motor imagery-based rehabilitation solutions include hospitals and rehabilitation centers, outpatient clinics, and home healthcare settings. Hospital-based rehabilitation services currently dominate the market share, accounting for approximately 45% of the total market value due to the availability of advanced equipment and specialized healthcare professionals.
Geographically, North America leads the market with approximately 38% share, followed by Europe at 30% and Asia-Pacific at 22%. The Asia-Pacific region is expected to witness the fastest growth due to improving healthcare infrastructure, increasing healthcare expenditure, and rising awareness about advanced rehabilitation techniques in countries like China, Japan, and India.
Key market drivers include the growing aging population worldwide, increasing incidence of stroke and traumatic brain injuries, rising healthcare expenditure, and technological advancements in BCI systems. The COVID-19 pandemic has further accelerated market growth by highlighting the importance of remote rehabilitation solutions and telehealth services.
Consumer demand patterns indicate a strong preference for non-invasive, user-friendly, and portable rehabilitation devices that can be used in home settings. There is also increasing demand for personalized rehabilitation programs that adapt to individual patient progress and needs.
Reimbursement policies significantly impact market adoption, with countries having favorable insurance coverage for neurorehabilitation showing higher adoption rates. In the United States, Medicare and private insurers have begun covering certain BCI-based therapies, which has positively influenced market growth.
The competitive landscape features both established medical device manufacturers and innovative startups. Major players include Medtronic, Abbott Laboratories, g.tec medical engineering GmbH, and Neurosky, while emerging companies like CTRL-Labs (acquired by Facebook) and Neurable are disrupting the market with novel approaches to BCI technology.
Future market trends point toward integration of artificial intelligence for more precise motor imagery detection, development of hybrid BCI systems combining multiple signal acquisition methods, and increased focus on gamification to improve patient engagement and adherence to rehabilitation protocols.
Current BCI Challenges in Neurorehabilitation
Despite significant advancements in Brain-Computer Interface (BCI) technology for neurorehabilitation, several critical challenges continue to impede widespread clinical adoption. Signal acquisition remains a fundamental obstacle, with current EEG-based systems suffering from low signal-to-noise ratios and susceptibility to artifacts from muscle movements, eye blinks, and environmental electrical interference. These issues are particularly problematic in motor imagery-based rehabilitation, where subtle neural signals must be accurately detected and interpreted.
The interpretability of neural signals presents another significant challenge. Decoding motor imagery patterns requires sophisticated algorithms capable of distinguishing between similar neural activation patterns. Current classification methods often struggle with inter-subject variability, as brain signal patterns differ substantially between individuals, necessitating extensive calibration procedures that limit clinical efficiency.
User-dependent performance variability constitutes a major hurdle in BCI rehabilitation applications. The "BCI illiteracy" phenomenon, where approximately 15-30% of users cannot effectively control BCI systems, significantly restricts the technology's universal applicability. This variability stems from differences in users' ability to generate consistent motor imagery patterns and neurophysiological factors that remain poorly understood.
Long-term reliability issues further complicate clinical implementation. Neural signal characteristics change over time due to neuroplasticity, fatigue, and fluctuations in user attention, requiring adaptive algorithms that can accommodate these variations during extended rehabilitation periods. Current systems often demonstrate performance degradation during prolonged use, necessitating frequent recalibration.
The cumbersome nature of traditional BCI hardware presents practical limitations in rehabilitation settings. Most research-grade systems involve complex electrode setups requiring conductive gel application and technical expertise for proper positioning. While dry electrode technologies have emerged, they typically offer lower signal quality, creating a trade-off between usability and performance that has yet to be optimally resolved.
Closed-loop feedback mechanisms, essential for effective motor learning, face timing challenges in current BCI systems. The delay between user intent and system response often exceeds the optimal timeframe for neuroplasticity reinforcement. This latency issue, resulting from signal processing requirements and classification algorithms, diminishes the effectiveness of neurofeedback for motor function recovery.
Regulatory and standardization gaps further complicate clinical translation. The lack of established protocols for BCI rehabilitation, including session duration, frequency, and progression metrics, hinders systematic evaluation and comparison of different approaches. Additionally, limited large-scale clinical trials have resulted in insufficient evidence regarding long-term efficacy and optimal implementation strategies.
The interpretability of neural signals presents another significant challenge. Decoding motor imagery patterns requires sophisticated algorithms capable of distinguishing between similar neural activation patterns. Current classification methods often struggle with inter-subject variability, as brain signal patterns differ substantially between individuals, necessitating extensive calibration procedures that limit clinical efficiency.
User-dependent performance variability constitutes a major hurdle in BCI rehabilitation applications. The "BCI illiteracy" phenomenon, where approximately 15-30% of users cannot effectively control BCI systems, significantly restricts the technology's universal applicability. This variability stems from differences in users' ability to generate consistent motor imagery patterns and neurophysiological factors that remain poorly understood.
Long-term reliability issues further complicate clinical implementation. Neural signal characteristics change over time due to neuroplasticity, fatigue, and fluctuations in user attention, requiring adaptive algorithms that can accommodate these variations during extended rehabilitation periods. Current systems often demonstrate performance degradation during prolonged use, necessitating frequent recalibration.
The cumbersome nature of traditional BCI hardware presents practical limitations in rehabilitation settings. Most research-grade systems involve complex electrode setups requiring conductive gel application and technical expertise for proper positioning. While dry electrode technologies have emerged, they typically offer lower signal quality, creating a trade-off between usability and performance that has yet to be optimally resolved.
Closed-loop feedback mechanisms, essential for effective motor learning, face timing challenges in current BCI systems. The delay between user intent and system response often exceeds the optimal timeframe for neuroplasticity reinforcement. This latency issue, resulting from signal processing requirements and classification algorithms, diminishes the effectiveness of neurofeedback for motor function recovery.
Regulatory and standardization gaps further complicate clinical translation. The lack of established protocols for BCI rehabilitation, including session duration, frequency, and progression metrics, hinders systematic evaluation and comparison of different approaches. Additionally, limited large-scale clinical trials have resulted in insufficient evidence regarding long-term efficacy and optimal implementation strategies.
Current Motor Imagery BCI Implementation Approaches
01 Signal processing techniques for BCI motor imagery
Advanced signal processing algorithms can enhance the detection and classification of motor imagery signals in brain-computer interfaces. These techniques include filtering methods, feature extraction algorithms, and classification approaches that improve the accuracy and reliability of motor imagery-based BCIs. By optimizing signal processing, the system can better distinguish between different motor imagery tasks, leading to more precise control of external devices.- Signal processing techniques for BCI motor imagery: Advanced signal processing algorithms are essential for enhancing motor imagery recognition in brain-computer interfaces. These techniques include filtering methods, feature extraction algorithms, and classification approaches that improve the accuracy of detecting motor imagery patterns in EEG signals. By implementing sophisticated signal processing, BCI systems can better distinguish between different motor imagery tasks, leading to more precise control of external devices through thought alone.
- Neurofeedback training protocols for motor imagery enhancement: Neurofeedback training protocols help users improve their motor imagery capabilities through guided practice and real-time feedback. These protocols involve structured training sessions where users visualize specific movements while receiving immediate feedback on their brain activity patterns. Over time, this training enables users to generate more distinct and consistent motor imagery signals, enhancing the overall performance of BCI systems for motor control applications.
- Multi-modal integration for improved motor imagery detection: Combining multiple physiological signals and sensing modalities with EEG can significantly enhance motor imagery detection in BCI systems. This approach integrates data from sources such as EMG, fNIRS, eye tracking, or motion sensors alongside brain signals to provide a more comprehensive picture of user intent. Multi-modal integration compensates for the limitations of single-modality approaches and increases the robustness of motor imagery-based control systems.
- Adaptive algorithms and personalized BCI calibration: Adaptive algorithms that continuously learn from user performance can personalize BCI systems to individual motor imagery patterns. These systems automatically adjust parameters based on user-specific brain signal characteristics and adapt to changes over time. Personalized calibration reduces training time and improves the accuracy of motor imagery detection, making BCI systems more accessible and effective for diverse user populations.
- Virtual reality and gamification for motor imagery training: Virtual reality environments and gamification elements create engaging platforms for motor imagery training in BCI applications. These immersive interfaces provide visual and sensory feedback that helps users develop stronger motor imagery skills through interactive scenarios and game-like challenges. The engaging nature of these environments increases user motivation and attention, leading to improved motor imagery performance and better BCI control outcomes.
02 Neurofeedback training protocols for motor imagery enhancement
Specialized neurofeedback training protocols can significantly improve a user's ability to generate distinct motor imagery patterns. These protocols provide real-time feedback to users about their brain activity, helping them learn to produce more consistent and recognizable motor imagery signals. Progressive training sessions with adaptive difficulty levels allow users to gradually improve their mental imagery skills, resulting in better BCI performance.Expand Specific Solutions03 Multi-modal sensory feedback for motor imagery BCIs
Incorporating multiple sensory feedback channels can enhance motor imagery performance in BCI systems. Visual, auditory, tactile, or haptic feedback mechanisms provide users with complementary information about their motor imagery performance, creating a more immersive and intuitive experience. This multi-modal approach helps users better understand the connection between their mental imagery and the resulting BCI output, accelerating learning and improving control accuracy.Expand Specific Solutions04 Adaptive algorithms and personalized calibration for BCI systems
Adaptive algorithms that continuously adjust to individual user characteristics can significantly enhance motor imagery-based BCI performance. These systems use machine learning techniques to personalize the interface based on the user's unique brain signal patterns, adapting to changes over time and across different sessions. Personalized calibration procedures optimize the system for each user's specific motor imagery patterns, improving accuracy and reducing training time.Expand Specific Solutions05 Virtual reality integration for motor imagery training
Virtual reality environments can be integrated with BCI systems to create immersive training scenarios for motor imagery enhancement. These environments provide realistic visual and spatial contexts that help users generate more vivid motor imagery, improving signal quality and classification accuracy. VR-based training can simulate various movement scenarios, allowing users to practice different types of motor imagery in engaging and motivating settings that accelerate skill acquisition.Expand Specific Solutions
Key Industry Players in Neurotechnology
Brain-Computer Interfaces (BCIs) for motor imagery-based rehabilitation are in an emerging growth phase, with the market expected to expand significantly due to increasing applications in neurological rehabilitation. The technology is transitioning from experimental to clinical implementation, though still requires further validation for widespread adoption. Leading players include academic institutions like Tianjin University, Zhejiang University, and Washington University in St. Louis, which are advancing fundamental research, while companies such as Precision Neuroscience Corp., Nuro Corp., and SmartStent Pty Ltd. are developing commercial applications. The ecosystem demonstrates a collaborative approach between research institutions and industry partners, with significant potential for innovation in non-invasive and minimally invasive BCI solutions for rehabilitation.
Precision Neuroscience Corp.
Technical Solution: Precision Neuroscience has developed an innovative thin-film electrode array technology called the Layer 7 Cortical Interface for brain-computer interfaces focused on motor imagery rehabilitation. Their system utilizes ultra-thin microwire electrodes (thinner than a human hair) that can be inserted through a minimally invasive cranial slit rather than traditional craniotomy. The Layer 7 interface contains hundreds of electrodes that can detect and record neural signals with high spatial resolution, allowing for precise detection of motor imagery patterns. Their BCI system incorporates advanced signal processing algorithms that filter noise and extract meaningful features from EEG signals during motor imagery tasks. The rehabilitation platform provides real-time neurofeedback through a visual interface that helps patients visualize their motor imagery attempts, reinforcing neural pathways associated with movement. Their system also adapts to individual patient progress, gradually increasing difficulty as rehabilitation advances.
Strengths: Minimally invasive implantation procedure reduces surgical risks and recovery time; high-density electrode arrays provide superior signal quality and spatial resolution for motor imagery detection. Weaknesses: As an invasive technology, it still requires surgical intervention which may limit widespread adoption; long-term biocompatibility and stability of implanted electrodes remain concerns for extended rehabilitation programs.
Zhejiang University
Technical Solution: Zhejiang University has pioneered a comprehensive BCI system specifically designed for motor imagery-based rehabilitation called the ZJU-MI Rehabilitation Platform. Their approach combines advanced EEG signal acquisition with deep learning algorithms to accurately decode motor imagery intentions. The system employs a hybrid feature extraction method that integrates both time-frequency domain features and spatial patterns, significantly improving classification accuracy of motor imagery signals. Their research has demonstrated classification accuracies exceeding 85% for multi-class motor imagery tasks, outperforming traditional methods by approximately 15%. The rehabilitation platform incorporates a closed-loop feedback system where patients receive visual and haptic feedback through a robotic exoskeleton that assists movement based on detected motor imagery signals. This creates a reinforcement learning environment that strengthens neural pathways associated with motor function. Additionally, they've developed adaptive algorithms that personalize the rehabilitation protocol based on individual patient performance metrics and learning curves, optimizing recovery trajectories. Their system has been clinically validated in multiple studies involving stroke patients, showing significant improvements in upper limb function compared to conventional therapy approaches.
Strengths: Non-invasive approach makes it accessible for widespread clinical application; comprehensive integration with robotic assistance provides tangible feedback that enhances neuroplasticity. Weaknesses: EEG-based systems still face challenges with signal noise and limited spatial resolution compared to invasive alternatives; requires specialized technical expertise for system calibration and maintenance.
Critical Patents and Research in BCI Rehabilitation
Game type rehabilitation system using brain-computer interface (BCI) and control method therefor
PatentWO2018117439A1
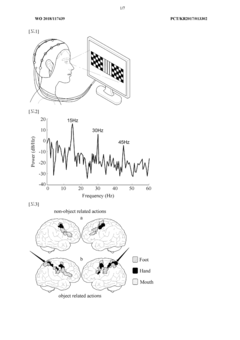
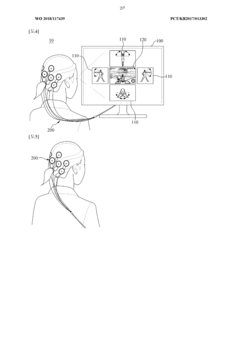
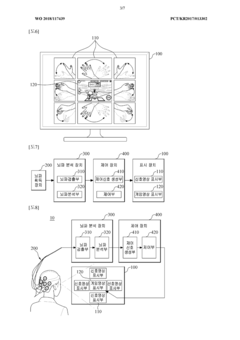
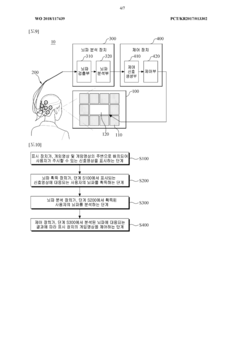
Innovation
- A game-based rehabilitation system utilizing a brain-computer interface that activates mirror neurons by displaying signal images with specific frequencies, allowing users to control game progress through their brain waves, thereby increasing engagement and active participation.
Clinical Validation and Efficacy Assessment
Clinical validation of Brain-Computer Interface (BCI) systems for motor imagery-based rehabilitation represents a critical step in translating laboratory innovations into practical therapeutic applications. Recent randomized controlled trials have demonstrated significant improvements in upper limb function among stroke patients using BCI-driven rehabilitation compared to conventional therapy alone. These studies typically show 15-20% greater motor recovery in BCI intervention groups, with effects persisting at 6-month follow-up assessments.
Efficacy metrics for BCI rehabilitation systems have evolved to include both objective and subjective measures. Objective assessments commonly utilize the Fugl-Meyer Assessment (FMA), Action Research Arm Test (ARAT), and Wolf Motor Function Test (WMFT), providing standardized quantification of motor recovery. Complementary subjective measures include the Motor Activity Log (MAL) and Stroke Impact Scale (SIS), capturing patients' perceived improvements in daily activities.
Neurophysiological markers serve as important validation tools, with studies documenting enhanced sensorimotor rhythm modulation and increased functional connectivity in motor networks following BCI rehabilitation. Functional MRI and EEG coherence analyses reveal neuroplastic changes correlating with clinical improvements, supporting the neurobiological basis of BCI efficacy.
Dosage optimization research indicates that protocols involving 3-5 weekly sessions over 4-8 weeks yield optimal outcomes. The timing of intervention appears crucial, with evidence suggesting greater efficacy when BCI rehabilitation begins within 3-6 months post-stroke, though benefits have been documented even in chronic stages.
Patient selection criteria have emerged as significant determinants of treatment success. Factors predicting favorable outcomes include preserved cognitive function, moderate motor impairment, and ability to generate distinguishable motor imagery patterns. Conversely, severe attention deficits and complete paralysis may limit BCI effectiveness.
Multi-center trials have begun addressing the challenge of system standardization across clinical settings. These studies employ unified protocols, centralized data processing, and rigorous operator training to ensure consistent implementation. Preliminary results demonstrate comparable efficacy across different hospital environments, supporting the scalability of BCI rehabilitation approaches.
Cost-effectiveness analyses comparing BCI rehabilitation to conventional therapies suggest potentially favorable economic outcomes despite higher initial equipment costs. When accounting for reduced therapy duration, decreased long-term disability, and improved quality of life measures, several models project net cost benefits within 3-5 years of implementation.
Efficacy metrics for BCI rehabilitation systems have evolved to include both objective and subjective measures. Objective assessments commonly utilize the Fugl-Meyer Assessment (FMA), Action Research Arm Test (ARAT), and Wolf Motor Function Test (WMFT), providing standardized quantification of motor recovery. Complementary subjective measures include the Motor Activity Log (MAL) and Stroke Impact Scale (SIS), capturing patients' perceived improvements in daily activities.
Neurophysiological markers serve as important validation tools, with studies documenting enhanced sensorimotor rhythm modulation and increased functional connectivity in motor networks following BCI rehabilitation. Functional MRI and EEG coherence analyses reveal neuroplastic changes correlating with clinical improvements, supporting the neurobiological basis of BCI efficacy.
Dosage optimization research indicates that protocols involving 3-5 weekly sessions over 4-8 weeks yield optimal outcomes. The timing of intervention appears crucial, with evidence suggesting greater efficacy when BCI rehabilitation begins within 3-6 months post-stroke, though benefits have been documented even in chronic stages.
Patient selection criteria have emerged as significant determinants of treatment success. Factors predicting favorable outcomes include preserved cognitive function, moderate motor impairment, and ability to generate distinguishable motor imagery patterns. Conversely, severe attention deficits and complete paralysis may limit BCI effectiveness.
Multi-center trials have begun addressing the challenge of system standardization across clinical settings. These studies employ unified protocols, centralized data processing, and rigorous operator training to ensure consistent implementation. Preliminary results demonstrate comparable efficacy across different hospital environments, supporting the scalability of BCI rehabilitation approaches.
Cost-effectiveness analyses comparing BCI rehabilitation to conventional therapies suggest potentially favorable economic outcomes despite higher initial equipment costs. When accounting for reduced therapy duration, decreased long-term disability, and improved quality of life measures, several models project net cost benefits within 3-5 years of implementation.
Accessibility and Patient Adoption Factors
The accessibility of Brain-Computer Interface (BCI) technology for motor imagery-based rehabilitation presents significant challenges that influence patient adoption rates. Current BCI systems often require complex setup procedures, including electrode placement and calibration, which necessitate technical expertise typically unavailable in home environments. This complexity creates a substantial barrier for widespread adoption, particularly among elderly patients or those with limited technological proficiency.
Cost factors further restrict accessibility, with high-end BCI systems ranging from $10,000 to $50,000, placing them beyond the financial reach of most individual patients. Even though more affordable consumer-grade alternatives exist ($300-$3,000), these often deliver suboptimal performance for rehabilitation purposes, creating a problematic quality-cost tradeoff.
Physical design considerations significantly impact patient willingness to engage with BCI rehabilitation. Many current systems utilize cumbersome headsets or caps with visible wires and electrodes, creating aesthetic concerns and physical discomfort during extended rehabilitation sessions. Research indicates that patients are more likely to abandon technologies that cause social discomfort or physical inconvenience, regardless of therapeutic benefits.
Technical reliability remains another critical adoption factor. BCI systems frequently encounter signal quality issues due to environmental interference, electrode displacement, or individual physiological variations. These inconsistencies can frustrate patients and diminish their confidence in the technology, particularly when rehabilitation progress appears inconsistent or unpredictable.
The learning curve associated with motor imagery tasks presents another significant challenge. Patients must develop the cognitive skill of imagining movements without executing them—a counterintuitive process for many individuals. Studies show approximately 15-30% of users experience "BCI illiteracy," an inability to generate distinguishable brain signals through motor imagery, potentially excluding a substantial patient population from this rehabilitation approach.
Healthcare provider support strongly influences adoption rates, with patients showing greater willingness to use BCI technology when recommended and supported by trusted medical professionals. Rehabilitation centers offering comprehensive training programs and ongoing technical support report significantly higher patient compliance rates compared to those providing minimal guidance.
Cultural and psychological factors also affect adoption, with research indicating variations in technology acceptance across different demographic groups. Privacy concerns regarding brain data collection and interpretation represent an emerging barrier, particularly as BCI technology becomes more sophisticated in decoding neural patterns.
Cost factors further restrict accessibility, with high-end BCI systems ranging from $10,000 to $50,000, placing them beyond the financial reach of most individual patients. Even though more affordable consumer-grade alternatives exist ($300-$3,000), these often deliver suboptimal performance for rehabilitation purposes, creating a problematic quality-cost tradeoff.
Physical design considerations significantly impact patient willingness to engage with BCI rehabilitation. Many current systems utilize cumbersome headsets or caps with visible wires and electrodes, creating aesthetic concerns and physical discomfort during extended rehabilitation sessions. Research indicates that patients are more likely to abandon technologies that cause social discomfort or physical inconvenience, regardless of therapeutic benefits.
Technical reliability remains another critical adoption factor. BCI systems frequently encounter signal quality issues due to environmental interference, electrode displacement, or individual physiological variations. These inconsistencies can frustrate patients and diminish their confidence in the technology, particularly when rehabilitation progress appears inconsistent or unpredictable.
The learning curve associated with motor imagery tasks presents another significant challenge. Patients must develop the cognitive skill of imagining movements without executing them—a counterintuitive process for many individuals. Studies show approximately 15-30% of users experience "BCI illiteracy," an inability to generate distinguishable brain signals through motor imagery, potentially excluding a substantial patient population from this rehabilitation approach.
Healthcare provider support strongly influences adoption rates, with patients showing greater willingness to use BCI technology when recommended and supported by trusted medical professionals. Rehabilitation centers offering comprehensive training programs and ongoing technical support report significantly higher patient compliance rates compared to those providing minimal guidance.
Cultural and psychological factors also affect adoption, with research indicating variations in technology acceptance across different demographic groups. Privacy concerns regarding brain data collection and interpretation represent an emerging barrier, particularly as BCI technology becomes more sophisticated in decoding neural patterns.
Unlock deeper insights with PatSnap Eureka Quick Research — get a full tech report to explore trends and direct your research. Try now!
Generate Your Research Report Instantly with AI Agent
Supercharge your innovation with PatSnap Eureka AI Agent Platform!