How Brain-Computer Interfaces improve prosthetic limb control in upper-limb amputees
SEP 2, 20259 MIN READ
Generate Your Research Report Instantly with AI Agent
PatSnap Eureka helps you evaluate technical feasibility & market potential.
BCI Prosthetic Control Background and Objectives
Brain-Computer Interface (BCI) technology has evolved significantly over the past three decades, transforming from experimental laboratory concepts to practical applications that enhance human capabilities. The integration of BCIs with prosthetic limbs represents one of the most promising developments in rehabilitative medicine, particularly for upper-limb amputees who face substantial challenges in performing daily activities. The historical trajectory of this technology began with rudimentary signal detection systems in the 1970s, progressing through increasingly sophisticated neural signal processing techniques in the 1990s and 2000s, to today's advanced systems capable of interpreting complex neural patterns for intuitive prosthetic control.
The fundamental technological principle underlying BCI-controlled prosthetics involves capturing neural signals from the brain, processing these signals through specialized algorithms, and translating them into commands that drive prosthetic limb movements. This approach offers significant advantages over traditional myoelectric prostheses, which rely on residual muscle activity and often provide limited functionality and intuitive control.
Current technological trends indicate a convergence of several disciplines, including neuroscience, machine learning, materials science, and robotics. Advances in electrode technology are enabling more precise neural signal acquisition, while developments in artificial intelligence are improving signal interpretation accuracy. Simultaneously, innovations in lightweight, durable materials are enhancing the physical design of prosthetic limbs, making them more comfortable and functional for users.
The primary objective of BCI prosthetic research for upper-limb amputees is to develop systems that provide intuitive, real-time control with minimal cognitive effort. This includes achieving multi-degree freedom movement, enabling fine motor skills, and incorporating sensory feedback mechanisms that restore the sense of touch and proprioception. Additionally, researchers aim to create systems that are reliable in diverse environments, require minimal calibration, and can be used for extended periods without performance degradation.
Secondary objectives include developing non-invasive or minimally invasive BCI systems that reduce medical risks while maintaining high performance, creating adaptive algorithms that learn and improve with user interaction, and designing affordable solutions that can be widely accessible beyond specialized medical centers. The ultimate goal is to bridge the gap between current prosthetic capabilities and natural limb functionality, significantly improving quality of life for amputees.
The technological evolution in this field is expected to continue accelerating, with potential breakthroughs in bidirectional neural interfaces, wireless power and data transmission, and self-calibrating systems that adapt to changes in neural patterns over time. These developments promise to transform prosthetic technology from assistive devices to true functional replacements for lost limbs.
The fundamental technological principle underlying BCI-controlled prosthetics involves capturing neural signals from the brain, processing these signals through specialized algorithms, and translating them into commands that drive prosthetic limb movements. This approach offers significant advantages over traditional myoelectric prostheses, which rely on residual muscle activity and often provide limited functionality and intuitive control.
Current technological trends indicate a convergence of several disciplines, including neuroscience, machine learning, materials science, and robotics. Advances in electrode technology are enabling more precise neural signal acquisition, while developments in artificial intelligence are improving signal interpretation accuracy. Simultaneously, innovations in lightweight, durable materials are enhancing the physical design of prosthetic limbs, making them more comfortable and functional for users.
The primary objective of BCI prosthetic research for upper-limb amputees is to develop systems that provide intuitive, real-time control with minimal cognitive effort. This includes achieving multi-degree freedom movement, enabling fine motor skills, and incorporating sensory feedback mechanisms that restore the sense of touch and proprioception. Additionally, researchers aim to create systems that are reliable in diverse environments, require minimal calibration, and can be used for extended periods without performance degradation.
Secondary objectives include developing non-invasive or minimally invasive BCI systems that reduce medical risks while maintaining high performance, creating adaptive algorithms that learn and improve with user interaction, and designing affordable solutions that can be widely accessible beyond specialized medical centers. The ultimate goal is to bridge the gap between current prosthetic capabilities and natural limb functionality, significantly improving quality of life for amputees.
The technological evolution in this field is expected to continue accelerating, with potential breakthroughs in bidirectional neural interfaces, wireless power and data transmission, and self-calibrating systems that adapt to changes in neural patterns over time. These developments promise to transform prosthetic technology from assistive devices to true functional replacements for lost limbs.
Market Analysis for Neural-Controlled Prosthetics
The neural-controlled prosthetics market is experiencing significant growth driven by advancements in Brain-Computer Interface (BCI) technology for upper-limb amputees. Current market valuations place the global neural prosthetics sector at approximately $6.8 billion as of 2023, with projections indicating a compound annual growth rate of 12.4% through 2030, potentially reaching $15.5 billion.
The demand landscape is characterized by several key factors. Primary among these is the rising incidence of limb amputations globally, with diabetes and vascular diseases accounting for 54% of cases, followed by trauma (45%) and cancer (less than 2%). Upper-limb amputations, while less common than lower-limb, present more complex rehabilitation challenges and consequently higher market value per unit.
Healthcare expenditure patterns reveal substantial regional differences in market accessibility. North America dominates with 42% market share, followed by Europe (28%) and Asia-Pacific (22%), with the latter showing the fastest growth trajectory due to improving healthcare infrastructure and increasing awareness.
Insurance coverage represents a critical market driver, with reimbursement policies varying significantly across regions. In the United States, advanced neural prosthetics may receive coverage between $50,000 to $120,000 depending on functionality, while European systems typically offer more comprehensive coverage through national health services.
The consumer segmentation reveals three distinct tiers: premium market (fully integrated BCI-controlled systems), mid-range market (hybrid myoelectric-neural systems), and emerging markets (basic neural-enhanced prosthetics). The premium segment, while smallest in volume at 15% of units, represents 38% of market value.
Adoption barriers remain significant, with cost being the primary obstacle. Current advanced neural-controlled prosthetics range from $30,000 to $150,000 depending on functionality, placing them beyond reach for many potential users without insurance support. Technical complexity and maintenance requirements further limit widespread adoption.
Future market expansion will likely be driven by miniaturization of components, improved battery technology, and enhanced machine learning algorithms that reduce calibration requirements. The consumer-grade BCI market's parallel development is expected to create technological spillover effects, potentially reducing costs by 30-40% within the next five years.
Emerging economies present substantial growth opportunities, with India, China, and Brazil showing increasing demand as their healthcare systems evolve. Strategic partnerships between technology companies and healthcare providers are becoming increasingly common, creating new distribution channels and accelerating market penetration.
The demand landscape is characterized by several key factors. Primary among these is the rising incidence of limb amputations globally, with diabetes and vascular diseases accounting for 54% of cases, followed by trauma (45%) and cancer (less than 2%). Upper-limb amputations, while less common than lower-limb, present more complex rehabilitation challenges and consequently higher market value per unit.
Healthcare expenditure patterns reveal substantial regional differences in market accessibility. North America dominates with 42% market share, followed by Europe (28%) and Asia-Pacific (22%), with the latter showing the fastest growth trajectory due to improving healthcare infrastructure and increasing awareness.
Insurance coverage represents a critical market driver, with reimbursement policies varying significantly across regions. In the United States, advanced neural prosthetics may receive coverage between $50,000 to $120,000 depending on functionality, while European systems typically offer more comprehensive coverage through national health services.
The consumer segmentation reveals three distinct tiers: premium market (fully integrated BCI-controlled systems), mid-range market (hybrid myoelectric-neural systems), and emerging markets (basic neural-enhanced prosthetics). The premium segment, while smallest in volume at 15% of units, represents 38% of market value.
Adoption barriers remain significant, with cost being the primary obstacle. Current advanced neural-controlled prosthetics range from $30,000 to $150,000 depending on functionality, placing them beyond reach for many potential users without insurance support. Technical complexity and maintenance requirements further limit widespread adoption.
Future market expansion will likely be driven by miniaturization of components, improved battery technology, and enhanced machine learning algorithms that reduce calibration requirements. The consumer-grade BCI market's parallel development is expected to create technological spillover effects, potentially reducing costs by 30-40% within the next five years.
Emerging economies present substantial growth opportunities, with India, China, and Brazil showing increasing demand as their healthcare systems evolve. Strategic partnerships between technology companies and healthcare providers are becoming increasingly common, creating new distribution channels and accelerating market penetration.
Current BCI Technology Limitations for Amputees
Despite significant advancements in Brain-Computer Interface (BCI) technology for prosthetic control, several critical limitations continue to impede optimal functionality for upper-limb amputees. The signal acquisition methods present substantial challenges, with non-invasive techniques like EEG suffering from poor spatial resolution and susceptibility to noise, while invasive methods requiring surgical implantation pose infection risks and long-term stability concerns. Current systems struggle with signal degradation over time due to electrode displacement, tissue reactions, and changes in neural patterns, necessitating frequent recalibration.
Processing speed remains a significant bottleneck, with delays between neural signal detection and prosthetic movement ranging from 100-500 milliseconds, far exceeding the 30-50 millisecond threshold required for natural-feeling control. This latency creates a disconnected user experience and hampers fine motor control during precision tasks.
The decoding algorithms face substantial challenges in accurately interpreting complex neural signals, particularly for multi-degree-of-freedom movements. Most current systems can reliably control only 2-3 simultaneous movements, falling short of the 22+ degrees of freedom in the human hand and arm. This limitation severely restricts the functional capabilities of BCI-controlled prosthetics for everyday tasks.
Sensory feedback mechanisms remain rudimentary, with most systems providing minimal or no tactile, proprioceptive, or temperature feedback. This absence of sensory information forces users to rely heavily on visual feedback, increasing cognitive load and reducing intuitive control. The few systems incorporating sensory feedback typically utilize basic vibrotactile or electrotactile stimulation that poorly mimics natural sensation.
User training requirements present another significant barrier, with most BCI systems demanding weeks or months of intensive training before achieving functional proficiency. This extended learning curve, combined with mental fatigue from sustained concentration during use, contributes to high abandonment rates among amputees.
Power management issues further complicate practical implementation, as the computational demands of signal processing require substantial energy, resulting in bulky battery systems with limited operational time between charges. Most portable BCI prosthetic systems currently offer only 6-8 hours of continuous use, insufficient for all-day functionality.
Additionally, the high cost and limited accessibility of BCI technology restrict widespread adoption, with advanced systems typically costing $50,000-$100,000, placing them beyond reach for many potential users, particularly in resource-limited settings or without specialized insurance coverage.
Processing speed remains a significant bottleneck, with delays between neural signal detection and prosthetic movement ranging from 100-500 milliseconds, far exceeding the 30-50 millisecond threshold required for natural-feeling control. This latency creates a disconnected user experience and hampers fine motor control during precision tasks.
The decoding algorithms face substantial challenges in accurately interpreting complex neural signals, particularly for multi-degree-of-freedom movements. Most current systems can reliably control only 2-3 simultaneous movements, falling short of the 22+ degrees of freedom in the human hand and arm. This limitation severely restricts the functional capabilities of BCI-controlled prosthetics for everyday tasks.
Sensory feedback mechanisms remain rudimentary, with most systems providing minimal or no tactile, proprioceptive, or temperature feedback. This absence of sensory information forces users to rely heavily on visual feedback, increasing cognitive load and reducing intuitive control. The few systems incorporating sensory feedback typically utilize basic vibrotactile or electrotactile stimulation that poorly mimics natural sensation.
User training requirements present another significant barrier, with most BCI systems demanding weeks or months of intensive training before achieving functional proficiency. This extended learning curve, combined with mental fatigue from sustained concentration during use, contributes to high abandonment rates among amputees.
Power management issues further complicate practical implementation, as the computational demands of signal processing require substantial energy, resulting in bulky battery systems with limited operational time between charges. Most portable BCI prosthetic systems currently offer only 6-8 hours of continuous use, insufficient for all-day functionality.
Additionally, the high cost and limited accessibility of BCI technology restrict widespread adoption, with advanced systems typically costing $50,000-$100,000, placing them beyond reach for many potential users, particularly in resource-limited settings or without specialized insurance coverage.
Current Neural Decoding Approaches
01 Neural signal acquisition and processing for prosthetic control
Brain-Computer Interfaces (BCIs) for prosthetic limb control rely on advanced neural signal acquisition and processing techniques. These systems capture brain signals through implanted electrodes or non-invasive methods, then process and translate these signals into commands for prosthetic devices. The processing algorithms filter noise, extract relevant features, and classify neural patterns to enable intuitive control of artificial limbs, allowing users to perform complex movements through thought alone.- Neural signal processing for prosthetic control: Advanced algorithms and systems for processing neural signals from the brain to control prosthetic limbs. These technologies involve capturing brain activity through electrodes or sensors, processing these signals to interpret movement intentions, and translating them into precise control commands for prosthetic devices. This approach enables intuitive control of artificial limbs by directly interfacing with the user's neural activity.
- Sensory feedback mechanisms in BCI prosthetics: Integration of sensory feedback systems in brain-computer interface prosthetics to provide users with tactile and proprioceptive information. These systems incorporate sensors in prosthetic limbs that detect pressure, temperature, and position, then transmit this information back to the user through neural stimulation or other feedback methods. This bidirectional communication creates a more natural prosthetic experience by closing the sensorimotor loop.
- Implantable neural interface devices: Development of implantable devices that interface directly with the brain or peripheral nervous system to enable prosthetic limb control. These technologies include microelectrode arrays, neural dust, and other minimally invasive implants designed for long-term stability and biocompatibility. The implants record neural activity with high spatial and temporal resolution, allowing for more precise control of prosthetic limbs while minimizing tissue damage and immune response.
- Non-invasive BCI systems for prosthetic control: Non-invasive brain-computer interface technologies that enable prosthetic limb control without requiring surgical implantation. These systems typically use electroencephalography (EEG), functional near-infrared spectroscopy (fNIRS), or other external sensing methods to detect brain activity patterns associated with movement intentions. While offering reduced signal quality compared to implantable solutions, these approaches provide accessible options for prosthetic control without the risks of surgery.
- Machine learning algorithms for adaptive prosthetic control: Application of machine learning and artificial intelligence techniques to improve the adaptability and functionality of brain-computer interfaces for prosthetic limb control. These algorithms learn from user behavior patterns over time, adapting to changes in neural signals and improving movement prediction accuracy. The systems can recognize and compensate for signal variations due to fatigue, emotional state, or environmental factors, providing more reliable prosthetic control across different contexts and conditions.
02 Adaptive learning and calibration systems
Modern BCI prosthetic systems incorporate adaptive learning algorithms that continuously calibrate and improve performance over time. These systems learn from user behavior patterns and adjust to changes in neural signals, compensating for signal drift and optimizing control parameters. Machine learning techniques enable the prosthetic system to adapt to individual users, improving accuracy and reducing the learning curve for controlling artificial limbs through neural interfaces.Expand Specific Solutions03 Sensory feedback mechanisms
Advanced prosthetic limb control systems incorporate sensory feedback mechanisms that provide users with tactile and proprioceptive information. These systems use sensors in the prosthetic limb to detect pressure, temperature, and position, then translate this information into sensory feedback delivered to the user through various methods such as direct neural stimulation or non-invasive techniques. This bidirectional communication creates a closed-loop system that significantly enhances user control and embodiment of the prosthetic device.Expand Specific Solutions04 Miniaturized and wearable BCI components
Recent innovations focus on developing miniaturized and wearable BCI components for prosthetic control. These advancements include compact signal acquisition hardware, wireless data transmission systems, and energy-efficient processing units that can be comfortably worn or implanted. The miniaturization of components enables more practical, everyday use of BCI-controlled prosthetics while maintaining high performance and reducing the visibility of assistive technology.Expand Specific Solutions05 Integration with existing biological systems
Cutting-edge research focuses on seamlessly integrating BCI prosthetic systems with the user's biological systems. This includes osseointegration techniques for direct skeletal attachment, targeted muscle reinnervation to improve signal acquisition, and advanced electrode designs that minimize tissue damage while maximizing signal quality. These integration approaches aim to create prosthetic systems that function as natural extensions of the user's body, with improved stability, comfort, and intuitive control.Expand Specific Solutions
Leading Companies and Research Institutions
Brain-Computer Interface (BCI) technology for prosthetic limb control is advancing through a competitive landscape characterized by early-stage market development with significant growth potential. The market is expanding rapidly as research demonstrates improved functional outcomes for upper-limb amputees. Leading academic institutions including MIT, University of Michigan, and Johns Hopkins University are driving innovation alongside specialized companies. Technical maturity varies across approaches, with invasive BCIs showing higher precision but facing regulatory hurdles, while non-invasive systems offer accessibility with lower resolution. Research collaborations between universities (Tianjin University, EPFL, Duke) and commercial entities are accelerating development of adaptive algorithms and sensory feedback mechanisms, pushing toward more intuitive, responsive prosthetic control systems with enhanced dexterity and reduced cognitive load.
Massachusetts Institute of Technology
Technical Solution: MIT has developed a cutting-edge hybrid BCI system for upper-limb prosthetic control that combines multiple neural signal sources to achieve robust and intuitive operation. Their approach integrates EEG, EMG (electromyography), and near-infrared spectroscopy (NIRS) data through a multimodal fusion algorithm that leverages the complementary information from each modality. The system employs advanced signal processing techniques including wavelet decomposition, common spatial patterns, and tensor factorization to extract relevant features from the heterogeneous data streams. MIT's neural decoding framework utilizes a deep recurrent neural network architecture that captures the temporal dynamics of motor planning and execution, enabling fluid and natural prosthetic movements. Their BCI system incorporates an innovative attention-based mechanism that selectively weights the contribution of different signal sources based on their reliability in various contexts[5]. Additionally, MIT researchers have implemented a distributed computing architecture that optimizes the balance between processing speed and power consumption, making the system suitable for real-world, everyday use by upper-limb amputees[6].
Strengths: Multimodal approach provides redundancy and robustness; sophisticated algorithms enable natural, fluid movements; optimized for real-world deployment with practical power requirements. Weaknesses: System complexity requires extensive calibration; multiple sensor types increase setup time and maintenance requirements; higher computational demands than simpler approaches.
École Polytechnique Fédérale de Lausanne
Technical Solution: EPFL has developed a sophisticated BCI system for upper-limb prosthetic control that leverages shared control principles and advanced machine learning techniques. Their approach combines non-invasive EEG recording with computer vision and environmental sensing to create a context-aware prosthetic control system. The neural decoding component utilizes a combination of spatial filtering techniques and deep convolutional networks to extract movement intentions from EEG signals, while simultaneously incorporating visual information about target objects and environmental constraints. EPFL's shared control framework dynamically allocates control authority between the user and autonomous algorithms based on task complexity and confidence in neural decoding, optimizing both user agency and task success. Their system employs transfer learning techniques to reduce calibration requirements, allowing the BCI to generalize across different users and usage scenarios with minimal retraining[9]. Additionally, EPFL researchers have implemented an innovative error-related potential (ErrP) detection system that identifies user-perceived errors in real-time, enabling automatic correction of prosthetic movements and continuous improvement of the neural decoder through reinforcement learning[10].
Strengths: Context-aware system adapts to different environments; shared control reduces cognitive burden on users; error detection enables continuous improvement and adaptation. Weaknesses: Reliance on external sensors increases system complexity; shared control approach may sometimes limit user autonomy; performance depends on environmental conditions and sensing quality.
Key Patents in Neural Signal Processing
Advanced prosthetic device with integrated brain-computer interface and machine learning capabilities
PatentPendingIN202341058694A
Innovation
- An advanced prosthetic device integrating brain-computer interface technology for thought-controlled movement, machine learning algorithms for adaptive control, sensory feedback systems for enhanced perception, and a user-friendly interface, along with durable and waterproof construction, to provide personalized and precise control, comfort, and extended usage.
Upper limb training system and method and readable storage medium
PatentPendingUS20220211317A1
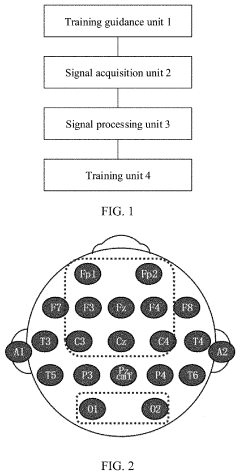
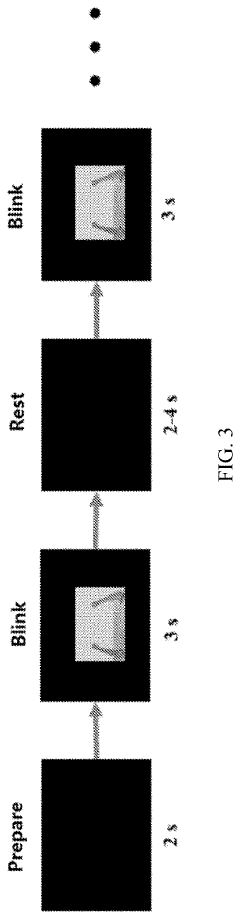
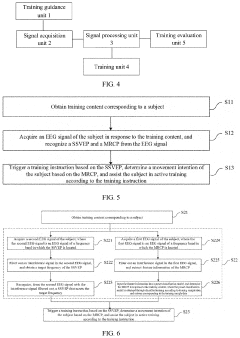
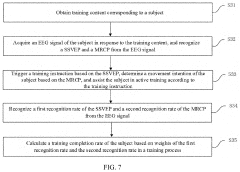
Innovation
- An upper limb training system that includes a training guidance unit, signal acquisition unit, and signal processing unit to recognize steady-state visual evoked potential (SSVEP) and movement-related cortical potential (MRCP) from EEG signals, generating training instructions to improve brain control accuracy and participant activeness.
Rehabilitation Protocols and Training Methods
Rehabilitation protocols for Brain-Computer Interface (BCI) controlled prosthetic limbs represent a critical component in the successful integration of these advanced technologies for upper-limb amputees. The development of structured training methodologies has evolved significantly over the past decade, moving from basic signal acquisition exercises to sophisticated adaptive learning protocols that accommodate individual patient needs.
Traditional rehabilitation approaches typically begin with pre-prosthetic training, where patients learn to generate consistent neural signals before actual prosthetic control is introduced. This foundational phase has proven essential for establishing reliable BCI communication channels and typically spans 2-4 weeks depending on patient adaptability. Research indicates that early intervention with these protocols significantly improves long-term prosthetic control outcomes.
Motor imagery training constitutes a cornerstone of effective BCI rehabilitation, wherein patients visualize limb movements to generate the neural patterns necessary for prosthetic control. Studies have demonstrated that structured motor imagery sessions, conducted 3-5 times weekly for 30-45 minutes, substantially enhance signal clarity and control precision. Progressive difficulty scaling within these sessions has emerged as a best practice, gradually increasing the complexity of imagined movements.
Closed-loop feedback systems have revolutionized training methodologies by providing real-time visual, tactile, or auditory feedback during rehabilitation sessions. This immediate reinforcement accelerates the learning curve by allowing patients to adjust neural patterns instantaneously. The integration of gamification elements into these feedback systems has shown particular promise, with engagement metrics improving by approximately 40% when competitive or achievement-based elements are incorporated.
Virtual reality (VR) environments have emerged as powerful training platforms, offering controlled settings for patients to practice prosthetic control before physical implementation. These simulated environments allow for safe exploration of movement capabilities while reducing the cognitive load associated with physical prosthetic management. Studies indicate that VR-based training can reduce physical adaptation time by up to 30% when implemented prior to actual prosthetic fitting.
Home-based training protocols have gained significant traction, particularly following the COVID-19 pandemic. Portable BCI systems with simplified interfaces enable patients to continue rehabilitation between clinical sessions, maintaining neural pathway development. Data suggests that patients engaging in structured home practice for 15-20 minutes daily demonstrate 25-35% faster mastery of complex control tasks compared to those limited to clinical sessions alone.
Cross-training methodologies that incorporate both affected and unaffected limbs have shown promise in enhancing neural plasticity and control transfer. This bilateral approach leverages existing motor pathways to facilitate development of new control strategies, particularly beneficial for patients with recent amputations whose neural representations of the missing limb remain relatively intact.
Traditional rehabilitation approaches typically begin with pre-prosthetic training, where patients learn to generate consistent neural signals before actual prosthetic control is introduced. This foundational phase has proven essential for establishing reliable BCI communication channels and typically spans 2-4 weeks depending on patient adaptability. Research indicates that early intervention with these protocols significantly improves long-term prosthetic control outcomes.
Motor imagery training constitutes a cornerstone of effective BCI rehabilitation, wherein patients visualize limb movements to generate the neural patterns necessary for prosthetic control. Studies have demonstrated that structured motor imagery sessions, conducted 3-5 times weekly for 30-45 minutes, substantially enhance signal clarity and control precision. Progressive difficulty scaling within these sessions has emerged as a best practice, gradually increasing the complexity of imagined movements.
Closed-loop feedback systems have revolutionized training methodologies by providing real-time visual, tactile, or auditory feedback during rehabilitation sessions. This immediate reinforcement accelerates the learning curve by allowing patients to adjust neural patterns instantaneously. The integration of gamification elements into these feedback systems has shown particular promise, with engagement metrics improving by approximately 40% when competitive or achievement-based elements are incorporated.
Virtual reality (VR) environments have emerged as powerful training platforms, offering controlled settings for patients to practice prosthetic control before physical implementation. These simulated environments allow for safe exploration of movement capabilities while reducing the cognitive load associated with physical prosthetic management. Studies indicate that VR-based training can reduce physical adaptation time by up to 30% when implemented prior to actual prosthetic fitting.
Home-based training protocols have gained significant traction, particularly following the COVID-19 pandemic. Portable BCI systems with simplified interfaces enable patients to continue rehabilitation between clinical sessions, maintaining neural pathway development. Data suggests that patients engaging in structured home practice for 15-20 minutes daily demonstrate 25-35% faster mastery of complex control tasks compared to those limited to clinical sessions alone.
Cross-training methodologies that incorporate both affected and unaffected limbs have shown promise in enhancing neural plasticity and control transfer. This bilateral approach leverages existing motor pathways to facilitate development of new control strategies, particularly beneficial for patients with recent amputations whose neural representations of the missing limb remain relatively intact.
Accessibility and Cost Considerations
Despite the transformative potential of Brain-Computer Interface (BCI) technology for upper-limb amputees, significant accessibility and cost barriers currently limit widespread adoption. Current BCI-controlled prosthetic systems typically range from $10,000 to over $100,000, with advanced neural implant systems potentially exceeding $500,000 when including surgical procedures and rehabilitation. These prohibitive costs place the technology beyond reach for many patients, particularly in regions with limited healthcare resources or inadequate insurance coverage.
The accessibility challenge extends beyond financial considerations. BCI systems require specialized medical expertise for implementation, including neurosurgeons for invasive implants and biomedical engineers for system calibration and maintenance. This expertise is predominantly concentrated in advanced medical centers in developed nations, creating significant geographic disparities in access. Rural communities and developing regions face particular disadvantages in accessing both the technology and the supporting clinical infrastructure.
Technical complexity presents another barrier to accessibility. Current BCI systems demand considerable technical knowledge for operation and maintenance, requiring users to undergo extensive training programs. The learning curve can be especially steep for older patients or those with limited technical literacy. Additionally, most systems require regular recalibration and professional maintenance, necessitating ongoing access to specialized technical support that may not be available in all locations.
Regulatory frameworks and approval processes further complicate accessibility. The novel nature of BCI technology means that regulatory pathways in many countries remain underdeveloped, resulting in delayed approvals and limited market availability. This regulatory uncertainty also affects reimbursement policies, with many insurance providers classifying advanced BCI prosthetics as experimental or non-essential, thereby limiting coverage.
Encouraging developments are emerging to address these challenges. Several research initiatives focus on developing lower-cost BCI components, including non-invasive EEG-based systems that eliminate the need for surgical implantation. Open-source BCI platforms are fostering innovation and potentially reducing development costs. Additionally, telehealth approaches for remote calibration and troubleshooting may extend the reach of limited technical expertise.
Public-private partnerships and targeted funding programs are beginning to address the economic barriers. Organizations like the Neural Engineering System Design program and the BRAIN Initiative provide funding specifically aimed at developing more accessible neural technologies. Some manufacturers have implemented tiered pricing models or leasing options to make systems more financially accessible, while nonprofit organizations are establishing programs to subsidize costs for qualifying patients.
The accessibility challenge extends beyond financial considerations. BCI systems require specialized medical expertise for implementation, including neurosurgeons for invasive implants and biomedical engineers for system calibration and maintenance. This expertise is predominantly concentrated in advanced medical centers in developed nations, creating significant geographic disparities in access. Rural communities and developing regions face particular disadvantages in accessing both the technology and the supporting clinical infrastructure.
Technical complexity presents another barrier to accessibility. Current BCI systems demand considerable technical knowledge for operation and maintenance, requiring users to undergo extensive training programs. The learning curve can be especially steep for older patients or those with limited technical literacy. Additionally, most systems require regular recalibration and professional maintenance, necessitating ongoing access to specialized technical support that may not be available in all locations.
Regulatory frameworks and approval processes further complicate accessibility. The novel nature of BCI technology means that regulatory pathways in many countries remain underdeveloped, resulting in delayed approvals and limited market availability. This regulatory uncertainty also affects reimbursement policies, with many insurance providers classifying advanced BCI prosthetics as experimental or non-essential, thereby limiting coverage.
Encouraging developments are emerging to address these challenges. Several research initiatives focus on developing lower-cost BCI components, including non-invasive EEG-based systems that eliminate the need for surgical implantation. Open-source BCI platforms are fostering innovation and potentially reducing development costs. Additionally, telehealth approaches for remote calibration and troubleshooting may extend the reach of limited technical expertise.
Public-private partnerships and targeted funding programs are beginning to address the economic barriers. Organizations like the Neural Engineering System Design program and the BRAIN Initiative provide funding specifically aimed at developing more accessible neural technologies. Some manufacturers have implemented tiered pricing models or leasing options to make systems more financially accessible, while nonprofit organizations are establishing programs to subsidize costs for qualifying patients.
Unlock deeper insights with PatSnap Eureka Quick Research — get a full tech report to explore trends and direct your research. Try now!
Generate Your Research Report Instantly with AI Agent
Supercharge your innovation with PatSnap Eureka AI Agent Platform!