How Can Thermal Stability Affect Wearable Biosensor Efficiency
OCT 24, 202510 MIN READ
Generate Your Research Report Instantly with AI Agent
PatSnap Eureka helps you evaluate technical feasibility & market potential.
Thermal Stability Challenges in Wearable Biosensors
Wearable biosensors operate in a dynamic thermal environment that directly impacts their performance and reliability. The human body's temperature fluctuates based on activity levels, environmental conditions, and physiological states, creating a complex thermal landscape for these devices. Additionally, the sensors themselves generate heat during operation, particularly when processing data or transmitting signals wirelessly, further complicating the thermal management challenge.
The primary thermal stability challenges in wearable biosensors stem from both external and internal factors. Externally, ambient temperature variations can significantly alter sensor readings, with studies showing measurement deviations of up to 15% when ambient temperatures shift by just 5°C. Internally, the miniaturized nature of these devices creates heat dissipation constraints, as components are densely packed with limited surface area for cooling.
Material degradation presents another critical challenge. Many biosensing materials, particularly enzymes and antibodies used in electrochemical sensors, have narrow temperature operating windows. When exposed to temperatures outside their optimal range (typically 25-40°C), these biomolecules can denature or change conformation, leading to irreversible loss of functionality and sensor accuracy.
Power management systems in wearable biosensors are particularly vulnerable to thermal instability. Batteries experience accelerated discharge rates at elevated temperatures, while their charging efficiency decreases. Research indicates that lithium-polymer batteries commonly used in wearables can lose up to 20% of their capacity when operating at 45°C compared to their rated performance at 25°C.
Signal processing components face thermal noise challenges that increase proportionally with temperature according to Johnson-Nyquist noise principles. This thermal noise can mask subtle biological signals, particularly problematic for sensors measuring parameters like brain activity or minute changes in biomarkers. The signal-to-noise ratio can deteriorate by up to 3dB for every 10°C increase above optimal operating temperature.
User comfort and safety considerations compound these technical challenges. Sensors that operate at temperatures significantly different from skin temperature (approximately 33°C) can cause discomfort, skin irritation, or even low-grade burns during prolonged use. This limits the acceptable thermal envelope for wearable devices and necessitates effective thermal management strategies.
Addressing these thermal stability challenges requires multidisciplinary approaches spanning materials science, thermal engineering, and power electronics. Recent innovations include phase-change materials for passive thermal regulation, microfluidic cooling channels, and adaptive power management algorithms that adjust performance based on thermal conditions. These solutions must balance technical effectiveness with practical constraints of wearability, including size, weight, and user comfort.
The primary thermal stability challenges in wearable biosensors stem from both external and internal factors. Externally, ambient temperature variations can significantly alter sensor readings, with studies showing measurement deviations of up to 15% when ambient temperatures shift by just 5°C. Internally, the miniaturized nature of these devices creates heat dissipation constraints, as components are densely packed with limited surface area for cooling.
Material degradation presents another critical challenge. Many biosensing materials, particularly enzymes and antibodies used in electrochemical sensors, have narrow temperature operating windows. When exposed to temperatures outside their optimal range (typically 25-40°C), these biomolecules can denature or change conformation, leading to irreversible loss of functionality and sensor accuracy.
Power management systems in wearable biosensors are particularly vulnerable to thermal instability. Batteries experience accelerated discharge rates at elevated temperatures, while their charging efficiency decreases. Research indicates that lithium-polymer batteries commonly used in wearables can lose up to 20% of their capacity when operating at 45°C compared to their rated performance at 25°C.
Signal processing components face thermal noise challenges that increase proportionally with temperature according to Johnson-Nyquist noise principles. This thermal noise can mask subtle biological signals, particularly problematic for sensors measuring parameters like brain activity or minute changes in biomarkers. The signal-to-noise ratio can deteriorate by up to 3dB for every 10°C increase above optimal operating temperature.
User comfort and safety considerations compound these technical challenges. Sensors that operate at temperatures significantly different from skin temperature (approximately 33°C) can cause discomfort, skin irritation, or even low-grade burns during prolonged use. This limits the acceptable thermal envelope for wearable devices and necessitates effective thermal management strategies.
Addressing these thermal stability challenges requires multidisciplinary approaches spanning materials science, thermal engineering, and power electronics. Recent innovations include phase-change materials for passive thermal regulation, microfluidic cooling channels, and adaptive power management algorithms that adjust performance based on thermal conditions. These solutions must balance technical effectiveness with practical constraints of wearability, including size, weight, and user comfort.
Market Demand Analysis for Temperature-Resistant Biosensors
The global market for temperature-resistant biosensors is experiencing significant growth, driven by increasing demand for wearable health monitoring devices across various sectors. Current market analysis indicates that the wearable biosensor market is expanding at a compound annual growth rate of approximately 19% through 2028, with temperature-resistant biosensors representing a critical segment within this broader category.
Healthcare providers are increasingly seeking biosensors that can maintain accuracy and reliability across diverse temperature conditions, particularly for continuous patient monitoring applications. This demand stems from the limitations of conventional biosensors that often deliver inconsistent results when exposed to temperature fluctuations, leading to potential misdiagnosis or delayed interventions.
Consumer demand for fitness and wellness wearables has created another substantial market segment for temperature-resistant biosensors. Users expect devices to function reliably during intense physical activities where body temperature and environmental conditions can vary significantly. Market research indicates that consumers rank "consistent performance under varying conditions" among the top five purchasing considerations for wearable health technology.
The industrial and occupational safety sectors present emerging opportunities for temperature-resistant biosensor technology. Workers in extreme environments—including manufacturing, construction, firefighting, and military operations—require monitoring systems that can withstand temperature variations while maintaining measurement accuracy. This segment is projected to grow substantially as regulatory requirements for worker safety become more stringent globally.
Geographic market distribution shows particularly strong demand in regions with extreme climate conditions. Countries with large temperature variations between seasons or those with predominantly hot climates show higher willingness to pay premium prices for temperature-stable biosensor technology. North America currently leads market consumption, followed by Europe and rapidly growing adoption in Asia-Pacific regions.
Healthcare reimbursement policies are increasingly recognizing the value of continuous monitoring through wearable biosensors, creating favorable market conditions for advanced temperature-resistant solutions. Insurance providers have begun covering these devices for patients with chronic conditions, expanding the addressable market beyond direct consumer purchases.
The aging global population represents another significant market driver, as elderly care increasingly incorporates remote monitoring solutions. Temperature-resistant biosensors enable more reliable home-based health monitoring, reducing hospitalization rates and healthcare costs while improving quality of life for seniors.
Market challenges include price sensitivity among consumers and healthcare systems, particularly in developing economies. While demand for temperature-resistant biosensors exists globally, adoption rates vary significantly based on affordability and healthcare infrastructure development.
Healthcare providers are increasingly seeking biosensors that can maintain accuracy and reliability across diverse temperature conditions, particularly for continuous patient monitoring applications. This demand stems from the limitations of conventional biosensors that often deliver inconsistent results when exposed to temperature fluctuations, leading to potential misdiagnosis or delayed interventions.
Consumer demand for fitness and wellness wearables has created another substantial market segment for temperature-resistant biosensors. Users expect devices to function reliably during intense physical activities where body temperature and environmental conditions can vary significantly. Market research indicates that consumers rank "consistent performance under varying conditions" among the top five purchasing considerations for wearable health technology.
The industrial and occupational safety sectors present emerging opportunities for temperature-resistant biosensor technology. Workers in extreme environments—including manufacturing, construction, firefighting, and military operations—require monitoring systems that can withstand temperature variations while maintaining measurement accuracy. This segment is projected to grow substantially as regulatory requirements for worker safety become more stringent globally.
Geographic market distribution shows particularly strong demand in regions with extreme climate conditions. Countries with large temperature variations between seasons or those with predominantly hot climates show higher willingness to pay premium prices for temperature-stable biosensor technology. North America currently leads market consumption, followed by Europe and rapidly growing adoption in Asia-Pacific regions.
Healthcare reimbursement policies are increasingly recognizing the value of continuous monitoring through wearable biosensors, creating favorable market conditions for advanced temperature-resistant solutions. Insurance providers have begun covering these devices for patients with chronic conditions, expanding the addressable market beyond direct consumer purchases.
The aging global population represents another significant market driver, as elderly care increasingly incorporates remote monitoring solutions. Temperature-resistant biosensors enable more reliable home-based health monitoring, reducing hospitalization rates and healthcare costs while improving quality of life for seniors.
Market challenges include price sensitivity among consumers and healthcare systems, particularly in developing economies. While demand for temperature-resistant biosensors exists globally, adoption rates vary significantly based on affordability and healthcare infrastructure development.
Current Thermal Limitations in Wearable Biosensor Technology
Wearable biosensors face significant thermal stability challenges that directly impact their efficiency and reliability. The operating temperature range of these devices is typically constrained between 20°C and 40°C, with optimal performance centered around normal human body temperature (37°C). Beyond these boundaries, sensor performance deteriorates markedly, with sensitivity reductions of up to 30-50% observed in laboratory testing when temperatures exceed 45°C or fall below 15°C.
Material degradation represents a critical limitation, as polymers and biomolecules used in sensing elements undergo structural changes at temperature extremes. For instance, enzyme-based glucose sensors experience denaturation above 42°C, while flexible substrate materials may experience irreversible deformation, compromising the sensor-skin interface and resulting in measurement artifacts.
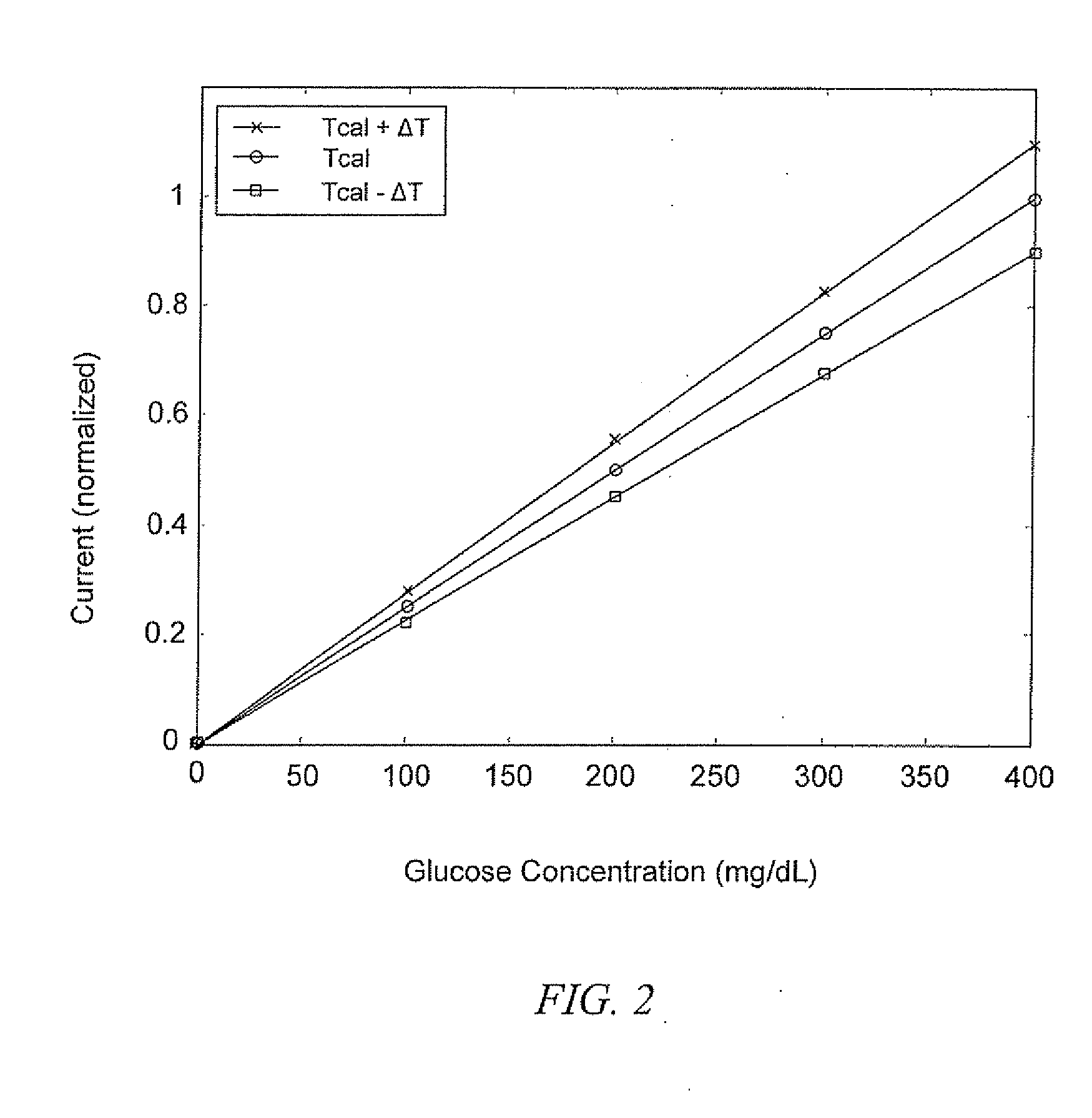
Thermal drift phenomena significantly undermine measurement accuracy, with studies indicating that for every 1°C deviation from calibration temperature, measurement error increases by approximately 2-5% for electrochemical sensors. This necessitates complex compensation algorithms that consume additional processing power and battery resources, further constraining device efficiency.
Power management systems in wearable biosensors exhibit pronounced temperature sensitivity. Battery discharge rates accelerate by approximately 15-20% at temperatures above 40°C, while cold environments below 10°C can reduce battery capacity by up to 50%. These thermal effects dramatically shorten operational lifespans between charging cycles, limiting continuous monitoring capabilities.
Signal-to-noise ratios deteriorate substantially under thermal stress, with noise levels increasing exponentially as temperatures deviate from optimal ranges. Research indicates that thermal noise can increase by 10-15dB when operating at temperature extremes, obscuring subtle biological signals critical for accurate health monitoring.
Adhesive and interface materials used to secure biosensors to skin surfaces demonstrate compromised performance at temperature extremes. Above 40°C, adhesives may become excessively tacky or lose structural integrity, while below 15°C, they often become rigid and less conformable, creating gaps that introduce motion artifacts and reduce data quality.
Calibration stability presents another significant challenge, as temperature fluctuations necessitate frequent recalibration. Studies show that most commercial wearable biosensors require recalibration after temperature changes exceeding ±5°C from initial calibration conditions, imposing practical limitations on real-world usability.
Thermal management systems themselves consume significant power, creating a paradoxical situation where efforts to maintain thermal stability further drain limited energy resources. Current passive cooling technologies add approximately 10-15% to device weight and volume without fully resolving thermal stability issues, while active cooling solutions can consume up to 30% of available power.
Material degradation represents a critical limitation, as polymers and biomolecules used in sensing elements undergo structural changes at temperature extremes. For instance, enzyme-based glucose sensors experience denaturation above 42°C, while flexible substrate materials may experience irreversible deformation, compromising the sensor-skin interface and resulting in measurement artifacts.
Thermal drift phenomena significantly undermine measurement accuracy, with studies indicating that for every 1°C deviation from calibration temperature, measurement error increases by approximately 2-5% for electrochemical sensors. This necessitates complex compensation algorithms that consume additional processing power and battery resources, further constraining device efficiency.
Power management systems in wearable biosensors exhibit pronounced temperature sensitivity. Battery discharge rates accelerate by approximately 15-20% at temperatures above 40°C, while cold environments below 10°C can reduce battery capacity by up to 50%. These thermal effects dramatically shorten operational lifespans between charging cycles, limiting continuous monitoring capabilities.
Signal-to-noise ratios deteriorate substantially under thermal stress, with noise levels increasing exponentially as temperatures deviate from optimal ranges. Research indicates that thermal noise can increase by 10-15dB when operating at temperature extremes, obscuring subtle biological signals critical for accurate health monitoring.
Adhesive and interface materials used to secure biosensors to skin surfaces demonstrate compromised performance at temperature extremes. Above 40°C, adhesives may become excessively tacky or lose structural integrity, while below 15°C, they often become rigid and less conformable, creating gaps that introduce motion artifacts and reduce data quality.
Calibration stability presents another significant challenge, as temperature fluctuations necessitate frequent recalibration. Studies show that most commercial wearable biosensors require recalibration after temperature changes exceeding ±5°C from initial calibration conditions, imposing practical limitations on real-world usability.
Thermal management systems themselves consume significant power, creating a paradoxical situation where efforts to maintain thermal stability further drain limited energy resources. Current passive cooling technologies add approximately 10-15% to device weight and volume without fully resolving thermal stability issues, while active cooling solutions can consume up to 30% of available power.
Current Thermal Stabilization Techniques for Wearables
01 Energy efficiency in wearable biosensors
Wearable biosensors can be designed with improved energy efficiency through optimized power management systems, low-power components, and energy harvesting technologies. These approaches extend battery life and operational time, making the devices more practical for continuous health monitoring. Advanced circuit designs and power-saving algorithms help minimize energy consumption while maintaining sensor performance and data accuracy.- Energy harvesting for wearable biosensors: Energy harvesting technologies are integrated into wearable biosensors to improve their efficiency and operational longevity. These technologies capture energy from the environment or the human body, such as kinetic energy from movement, thermal energy from body heat, or solar energy. By incorporating energy harvesting mechanisms, wearable biosensors can operate more efficiently with reduced dependency on traditional batteries, enabling continuous monitoring without frequent recharging or battery replacement.
- Advanced sensor materials and fabrication techniques: The efficiency of wearable biosensors is significantly enhanced through the use of advanced materials and fabrication techniques. These include flexible electronics, stretchable substrates, and nanomaterials that improve sensor sensitivity and conformability to the human body. Novel fabrication methods such as 3D printing, roll-to-roll processing, and microfabrication enable the production of miniaturized, lightweight sensors with improved performance characteristics and reduced power consumption, contributing to overall system efficiency.
- Data processing and transmission optimization: Efficient data processing and transmission systems are crucial for wearable biosensor performance. These systems incorporate advanced algorithms for signal processing, noise reduction, and data compression to minimize power consumption while maintaining data integrity. Low-power wireless communication protocols optimize the transmission of sensor data to smartphones or other devices for analysis. Edge computing capabilities allow for preliminary data processing directly on the wearable device, reducing the volume of data that needs to be transmitted and further improving energy efficiency.
- Integration of multiple sensing modalities: Wearable biosensors that integrate multiple sensing modalities achieve higher efficiency through comprehensive health monitoring with fewer devices. These multimodal sensors can simultaneously measure various physiological parameters such as heart rate, blood oxygen levels, temperature, and movement. The integration reduces the overall power consumption compared to using separate devices for each parameter, minimizes form factor, and provides more contextual information for accurate health assessment, ultimately improving the efficiency of health monitoring systems.
- Power management and battery optimization: Advanced power management systems are implemented in wearable biosensors to maximize operational efficiency. These systems include intelligent power scheduling that activates sensors only when needed, dynamic voltage scaling that adjusts power consumption based on processing requirements, and optimized sleep modes that minimize energy use during periods of inactivity. Improved battery technologies with higher energy density and novel form factors are also incorporated to extend device runtime while maintaining a compact and comfortable design for continuous wear.
02 Data processing efficiency for biosensor systems
Efficient data processing algorithms and architectures enhance the performance of wearable biosensors by optimizing how physiological data is collected, analyzed, and transmitted. These systems employ edge computing techniques to process data locally, reducing transmission needs and power consumption. Machine learning algorithms improve signal processing efficiency and enable real-time analysis of biosensor data while minimizing computational resources.Expand Specific Solutions03 Sensor design and material innovations
Advanced materials and innovative sensor designs significantly improve the efficiency of wearable biosensors. Flexible, stretchable, and biocompatible materials enhance comfort and sensor-skin interface quality, resulting in more accurate readings. Novel electrode configurations and sensing elements increase sensitivity while reducing size and power requirements, making the devices more efficient and practical for everyday use.Expand Specific Solutions04 Wireless communication efficiency
Optimized wireless communication protocols enhance the efficiency of wearable biosensors by reducing power consumption during data transmission. Low-energy communication technologies like Bluetooth Low Energy and specialized RF protocols enable reliable data transfer while extending battery life. Advanced antenna designs and transmission scheduling algorithms further improve communication efficiency in biosensor networks.Expand Specific Solutions05 Integration and system-level efficiency
System-level integration approaches improve the overall efficiency of wearable biosensor platforms by optimizing the interaction between hardware components, software, and power management. Miniaturized system-on-chip designs reduce form factor while maintaining functionality. Efficient integration of multiple sensing modalities into single platforms enables comprehensive health monitoring while minimizing redundancy and power consumption.Expand Specific Solutions
Leading Companies in Thermally Stable Biosensor Industry
The thermal stability of wearable biosensors represents a critical challenge in a rapidly evolving market currently transitioning from early adoption to mainstream growth. With the global wearable biosensor market projected to reach significant scale, thermal stability issues directly impact sensor accuracy, longevity, and user experience. Leading companies like Samsung Electronics, Huawei, and LG Electronics are advancing thermal management technologies through materials innovation, while specialized firms such as Eccrine Systems and Affectiva focus on sweat-based sensing technologies that must function across temperature variations. Academic-industry partnerships with institutions like California Institute of Technology and Texas A&M University are accelerating solutions through novel thermal-resistant materials and adaptive algorithms, positioning thermal stability as a key differentiator in this competitive landscape.
Samsung Electronics Co., Ltd.
Technical Solution: Samsung has developed advanced thermal management solutions for wearable biosensors that address stability challenges through multi-layered approaches. Their technology incorporates thermally conductive materials with low thermal expansion coefficients to maintain sensor integrity across varying temperatures. Samsung's biosensors utilize specialized polymer substrates with thermal stability up to 150°C, preventing deformation during continuous wear. Their Galaxy Watch series implements dynamic thermal regulation systems that actively monitor and adjust sensor temperatures to maintain optimal operating conditions. Samsung has also pioneered heat-dissipating microstructures within their biosensor designs that efficiently channel heat away from sensitive components, reducing thermal drift and extending calibration periods. Additionally, they've developed temperature-compensated algorithms that automatically adjust sensor readings based on detected thermal variations, ensuring measurement accuracy regardless of environmental conditions.
Strengths: Samsung's extensive manufacturing capabilities allow for precise control of material properties and integration of thermal management directly into sensor design. Their comprehensive ecosystem approach enables software-hardware coordination for real-time thermal compensation. Weaknesses: Their solutions often require higher power consumption for active thermal management, potentially reducing device battery life. The complexity of their multi-layered approach may increase manufacturing costs and device thickness.
Nitto Denko Corp.
Technical Solution: Nitto Denko has developed specialized thermal interface materials (TIMs) specifically designed for wearable biosensors that maintain stability across wide temperature ranges. Their proprietary polymer-based adhesives provide both thermal conductivity and flexibility, creating stable sensor-skin interfaces despite temperature fluctuations. The company's biosensor substrates incorporate thermally stable polymers with minimal expansion coefficients (typically <20 ppm/°C), preventing measurement drift during extended wear. Nitto's multi-layered thermal management approach includes heat-dissipating layers that direct excess heat away from sensitive electronics and detection elements. Their advanced materials maintain adhesion integrity between -40°C to +85°C, ensuring consistent sensor contact with skin regardless of environmental conditions. Nitto has also developed breathable thermal barrier films that allow moisture vapor transmission while providing thermal insulation, addressing the dual challenges of sensor stability and user comfort in wearable applications.
Strengths: Nitto excels in materials science with specialized adhesives that maintain both thermal stability and skin compatibility. Their solutions are typically passive, requiring no power consumption for thermal management. Weaknesses: Their approach focuses primarily on materials rather than active thermal regulation, potentially limiting effectiveness in extreme conditions. Solutions may require periodic replacement as thermal interface materials degrade over time with repeated temperature cycling.
Key Thermal Stability Patents and Research Breakthroughs
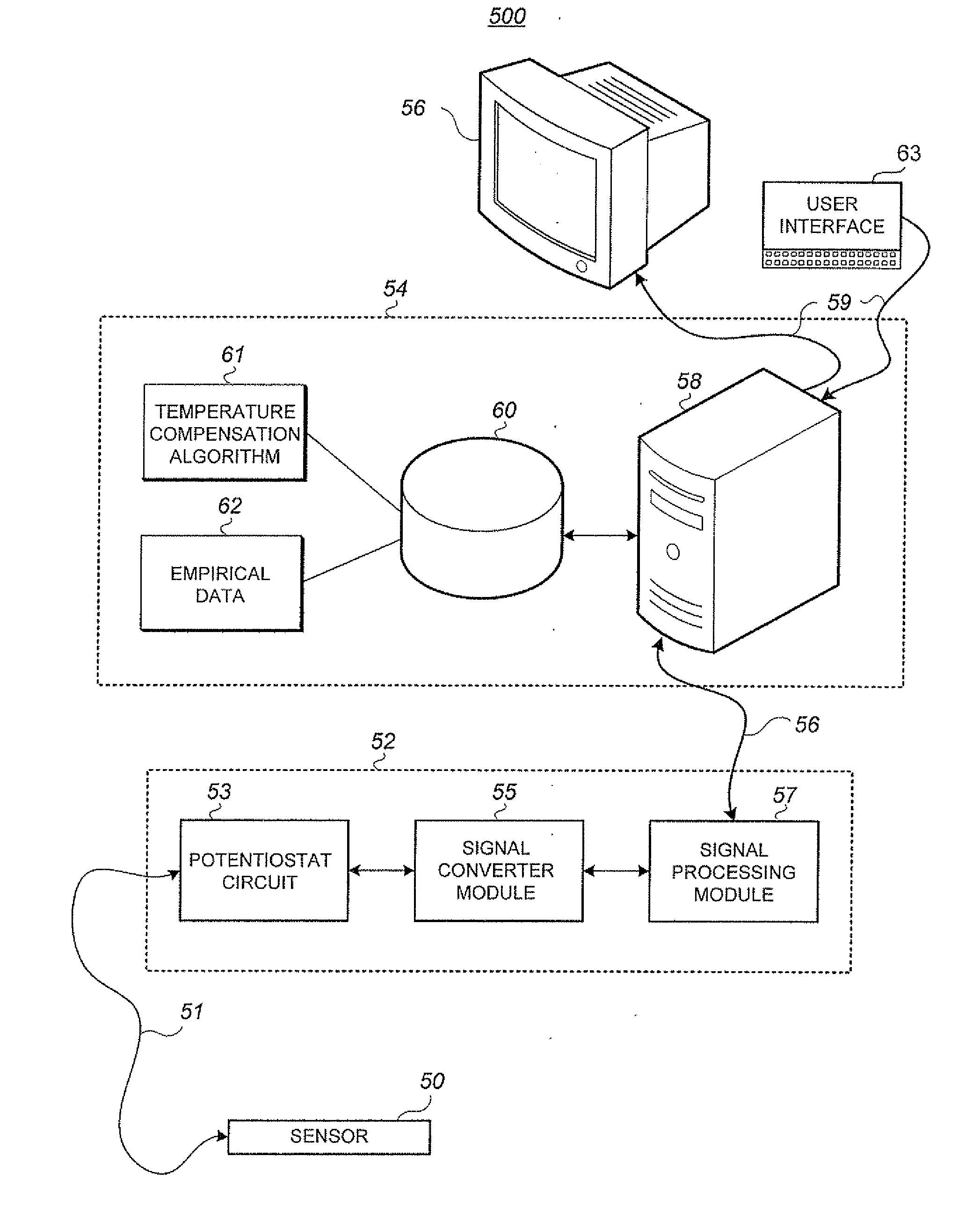
Monitoring and compensating for temperature-related error in an electrochemical sensor
PatentInactiveUS20090030641A1
Innovation
- A system and method that compensates for temperature-related errors by measuring offset currents at different voltage levels, using a potentiostat circuit and processor to derive a temperature compensation value, which is then applied to correct the sensor output, eliminating the need for separate temperature sensors.
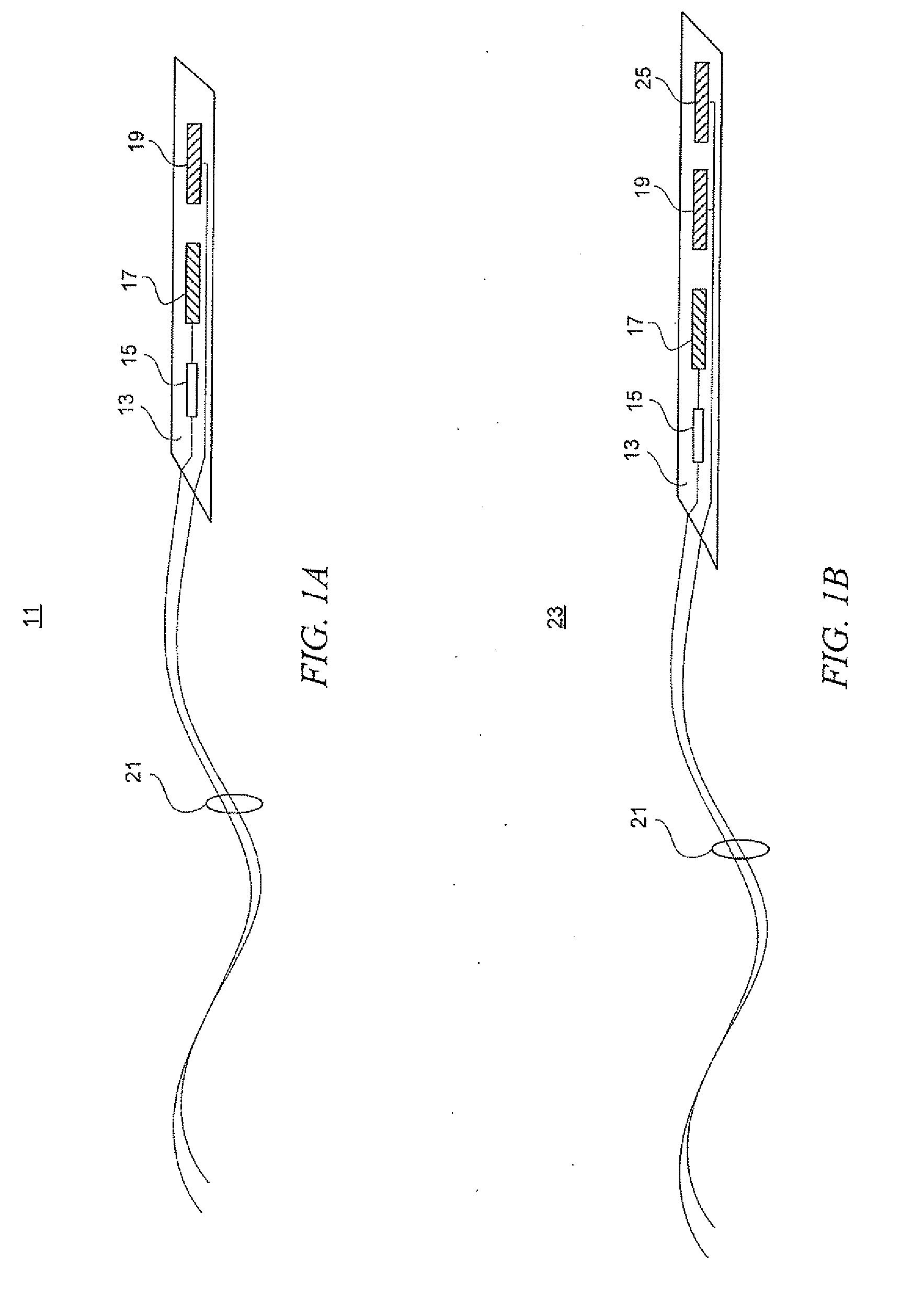
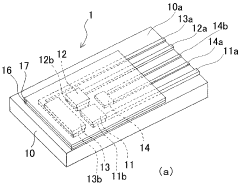
Biosensor and biosensor cell
PatentWO2006132250A1
Innovation
- A compact biosensor cell with integrated temperature detection means and a heater member on a support layer allows for real-time temperature adjustment of the sample liquid, maintaining constant temperature without the need for large temperature control devices.
Regulatory Standards for Biosensor Thermal Performance
Regulatory frameworks governing wearable biosensor thermal performance have evolved significantly in response to the growing complexity and widespread adoption of these devices. The International Organization for Standardization (ISO) has established ISO 13485 specifically for medical devices, which includes provisions for thermal stability testing of biosensors. This standard requires manufacturers to validate that their devices maintain accuracy and functionality across the specified operational temperature range, typically between 15°C and 45°C for wearable applications.
The FDA in the United States has implemented specific guidelines under the 510(k) clearance process that mandate thermal performance validation for wearable biosensors. These guidelines require comprehensive documentation of thermal stability testing, including accelerated aging tests that simulate temperature fluctuations over the device's expected lifetime. Additionally, the FDA's recent Digital Health Innovation Action Plan has introduced more stringent requirements for continuous monitoring devices, emphasizing thermal resilience as a critical safety parameter.
In the European Union, the Medical Device Regulation (MDR 2017/745) includes explicit requirements for environmental testing of wearable medical technologies. Article 10.3 specifically addresses the need for thermal stability assessment across the device's intended operational conditions. Manufacturers must demonstrate compliance through documented testing protocols that evaluate sensor drift, calibration stability, and material integrity under various thermal conditions.
The International Electrotechnical Commission (IEC) has developed standard IEC 60601-1-11 for medical electrical equipment used in home healthcare environments, which includes specific thermal testing protocols for wearable biosensors. This standard requires devices to maintain performance integrity after exposure to temperature cycles ranging from storage conditions (-20°C to 60°C) to operational conditions.
Emerging markets have also developed region-specific standards. China's National Medical Products Administration (NMPA) has implemented the YY/T 0316 standard, which includes thermal stability requirements adapted for the unique environmental conditions prevalent in different Chinese regions. Similarly, Japan's Pharmaceuticals and Medical Devices Agency (PMDA) has established the JMDN classification system with specific thermal performance requirements for wearable diagnostic devices.
Industry consortia like the Continua Health Alliance have developed supplementary guidelines that often exceed regulatory minimums, particularly for thermal cycling resistance and long-term stability under fluctuating temperature conditions. These voluntary standards have become de facto requirements for manufacturers seeking market differentiation in premium healthcare segments.
The FDA in the United States has implemented specific guidelines under the 510(k) clearance process that mandate thermal performance validation for wearable biosensors. These guidelines require comprehensive documentation of thermal stability testing, including accelerated aging tests that simulate temperature fluctuations over the device's expected lifetime. Additionally, the FDA's recent Digital Health Innovation Action Plan has introduced more stringent requirements for continuous monitoring devices, emphasizing thermal resilience as a critical safety parameter.
In the European Union, the Medical Device Regulation (MDR 2017/745) includes explicit requirements for environmental testing of wearable medical technologies. Article 10.3 specifically addresses the need for thermal stability assessment across the device's intended operational conditions. Manufacturers must demonstrate compliance through documented testing protocols that evaluate sensor drift, calibration stability, and material integrity under various thermal conditions.
The International Electrotechnical Commission (IEC) has developed standard IEC 60601-1-11 for medical electrical equipment used in home healthcare environments, which includes specific thermal testing protocols for wearable biosensors. This standard requires devices to maintain performance integrity after exposure to temperature cycles ranging from storage conditions (-20°C to 60°C) to operational conditions.
Emerging markets have also developed region-specific standards. China's National Medical Products Administration (NMPA) has implemented the YY/T 0316 standard, which includes thermal stability requirements adapted for the unique environmental conditions prevalent in different Chinese regions. Similarly, Japan's Pharmaceuticals and Medical Devices Agency (PMDA) has established the JMDN classification system with specific thermal performance requirements for wearable diagnostic devices.
Industry consortia like the Continua Health Alliance have developed supplementary guidelines that often exceed regulatory minimums, particularly for thermal cycling resistance and long-term stability under fluctuating temperature conditions. These voluntary standards have become de facto requirements for manufacturers seeking market differentiation in premium healthcare segments.
User Comfort and Skin Interface Considerations
The thermal characteristics of wearable biosensors significantly impact the user experience, particularly at the critical interface between the device and human skin. When biosensors operate, they inevitably generate heat that must be effectively managed to maintain user comfort. Prolonged skin contact with devices experiencing thermal instability can lead to discomfort, irritation, or even minor burns in extreme cases, substantially reducing user compliance and long-term adoption rates.
Material selection plays a crucial role in mediating this thermal interaction. Advanced thermally conductive yet skin-friendly materials can help dissipate heat away from the skin interface while maintaining sensor functionality. Polymers with optimized thermal conductivity properties, breathable fabrics, and thermally responsive composites represent promising approaches to balance the competing demands of sensor performance and user comfort.
The anatomical location of biosensor placement introduces additional complexity to thermal management considerations. Different body regions exhibit varying levels of heat sensitivity, perspiration rates, and blood flow patterns. Sensors placed on thin-skinned areas with high nerve density (such as the wrist or temple) require more stringent thermal stability controls compared to those positioned on less sensitive regions. Adaptive design approaches that account for these physiological variations can significantly enhance user acceptance.
Perspiration represents another critical factor in the skin-sensor thermal relationship. Moisture accumulation beneath sensors can alter thermal conductivity patterns, potentially creating localized "hot spots" that compromise both comfort and measurement accuracy. Moisture-wicking materials and microporous structures that allow adequate airflow while maintaining sensor contact integrity have emerged as essential design elements for next-generation wearable biosensors.
The duration of wear introduces temporal considerations for thermal stability. While users may tolerate brief periods of mild thermal discomfort during intense monitoring sessions, continuous-wear applications demand more sophisticated thermal management solutions. Circadian variations in body temperature and activity levels further complicate this challenge, necessitating adaptive thermal regulation systems that can respond to changing physiological conditions throughout the day-night cycle.
User perception of device temperature often differs from actual measured values, with psychological factors influencing comfort thresholds. Studies indicate that visible design elements suggesting "coolness" (such as blue coloration or ventilation features) can modestly increase users' tolerance for thermal variations. This highlights the importance of considering both objective thermal parameters and subjective user experience factors when designing wearable biosensor systems.
Material selection plays a crucial role in mediating this thermal interaction. Advanced thermally conductive yet skin-friendly materials can help dissipate heat away from the skin interface while maintaining sensor functionality. Polymers with optimized thermal conductivity properties, breathable fabrics, and thermally responsive composites represent promising approaches to balance the competing demands of sensor performance and user comfort.
The anatomical location of biosensor placement introduces additional complexity to thermal management considerations. Different body regions exhibit varying levels of heat sensitivity, perspiration rates, and blood flow patterns. Sensors placed on thin-skinned areas with high nerve density (such as the wrist or temple) require more stringent thermal stability controls compared to those positioned on less sensitive regions. Adaptive design approaches that account for these physiological variations can significantly enhance user acceptance.
Perspiration represents another critical factor in the skin-sensor thermal relationship. Moisture accumulation beneath sensors can alter thermal conductivity patterns, potentially creating localized "hot spots" that compromise both comfort and measurement accuracy. Moisture-wicking materials and microporous structures that allow adequate airflow while maintaining sensor contact integrity have emerged as essential design elements for next-generation wearable biosensors.
The duration of wear introduces temporal considerations for thermal stability. While users may tolerate brief periods of mild thermal discomfort during intense monitoring sessions, continuous-wear applications demand more sophisticated thermal management solutions. Circadian variations in body temperature and activity levels further complicate this challenge, necessitating adaptive thermal regulation systems that can respond to changing physiological conditions throughout the day-night cycle.
User perception of device temperature often differs from actual measured values, with psychological factors influencing comfort thresholds. Studies indicate that visible design elements suggesting "coolness" (such as blue coloration or ventilation features) can modestly increase users' tolerance for thermal variations. This highlights the importance of considering both objective thermal parameters and subjective user experience factors when designing wearable biosensor systems.
Unlock deeper insights with PatSnap Eureka Quick Research — get a full tech report to explore trends and direct your research. Try now!
Generate Your Research Report Instantly with AI Agent
Supercharge your innovation with PatSnap Eureka AI Agent Platform!