Floormat physiological sensor
a sensor and physiological technology, applied in the field of sensors, can solve the problems of nullifying the value of such measurements, affecting treatment, and measurement errors, and achieve the effects of simple form factor, simple use, and compliance of patients
- Summary
- Abstract
- Description
- Claims
- Application Information
AI Technical Summary
Benefits of technology
Problems solved by technology
Method used
Image
Examples
Embodiment Construction
1. Product Overview
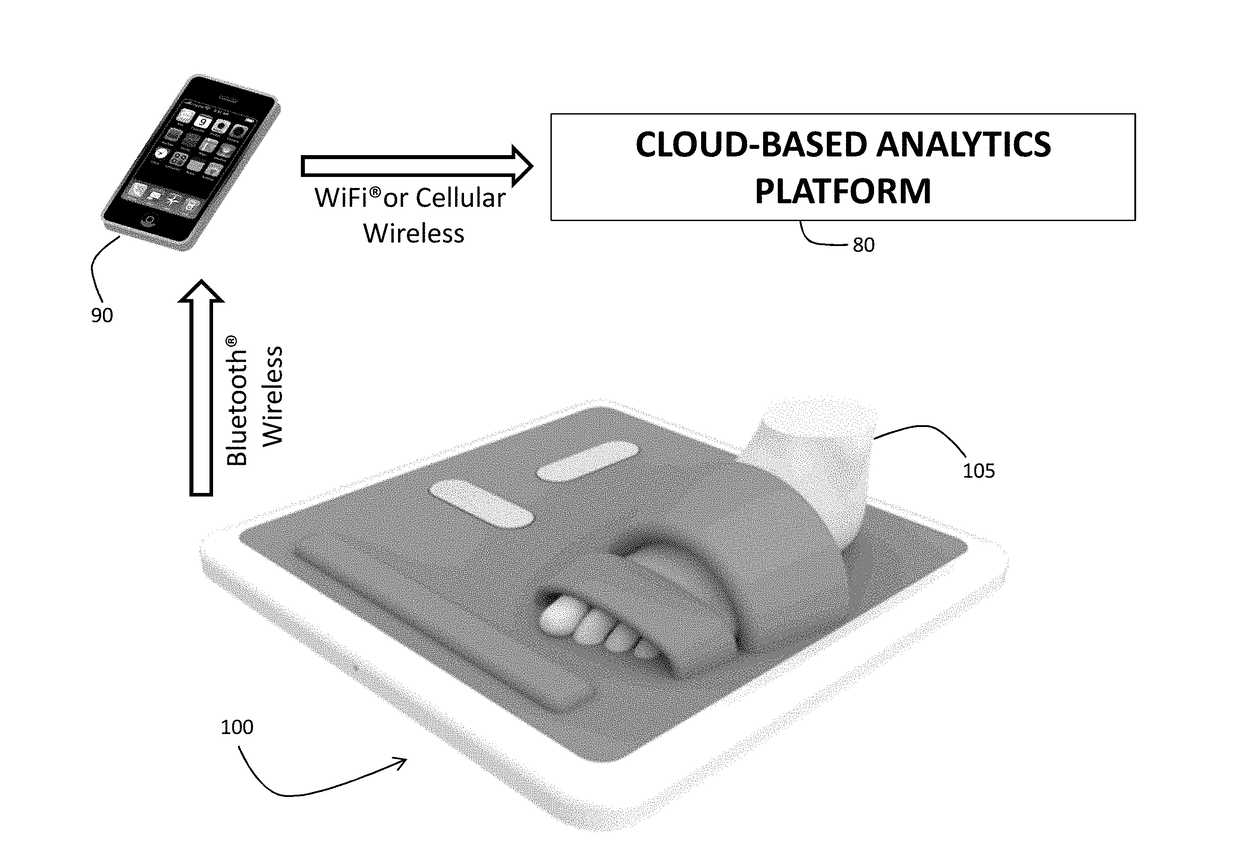
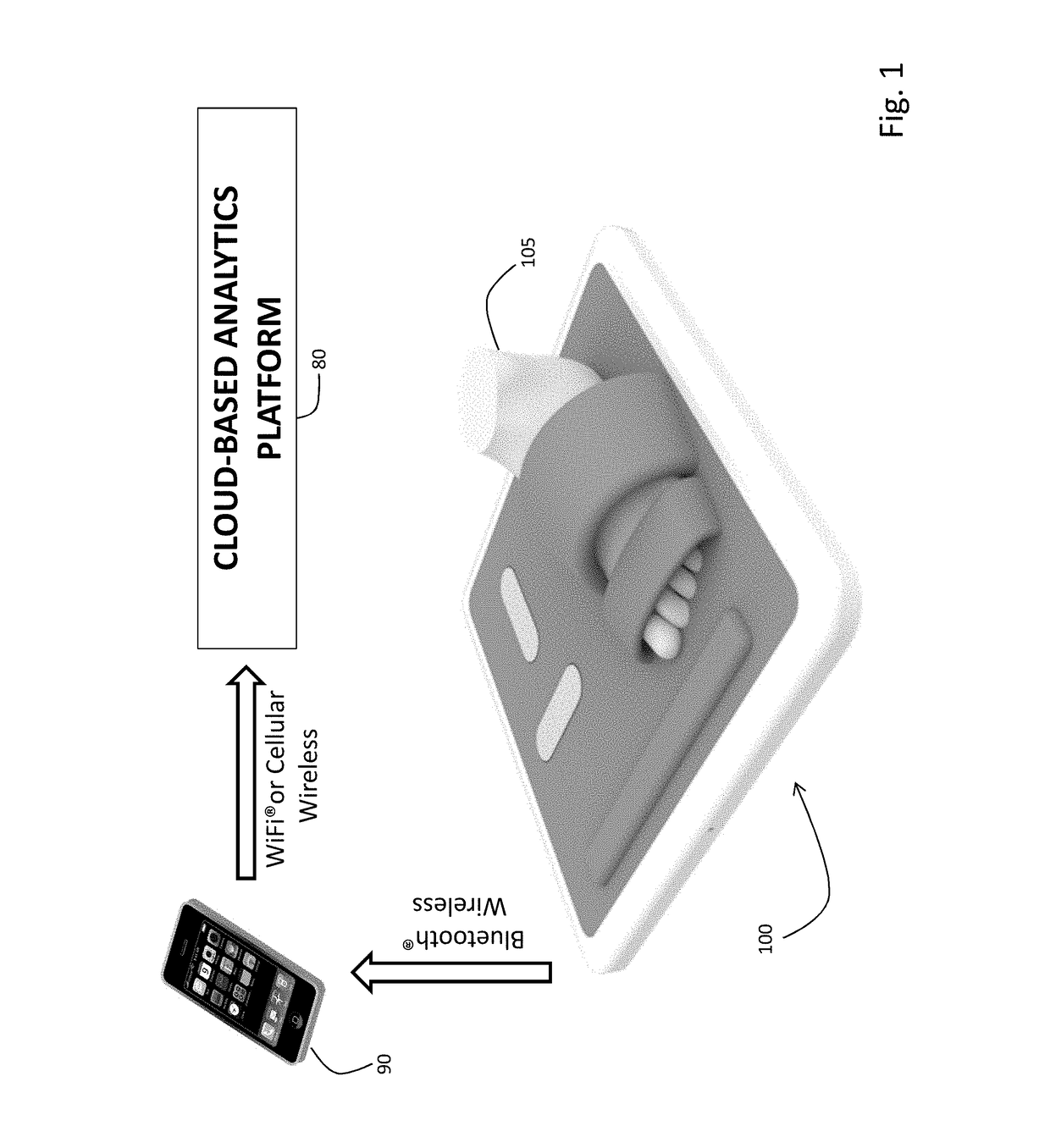
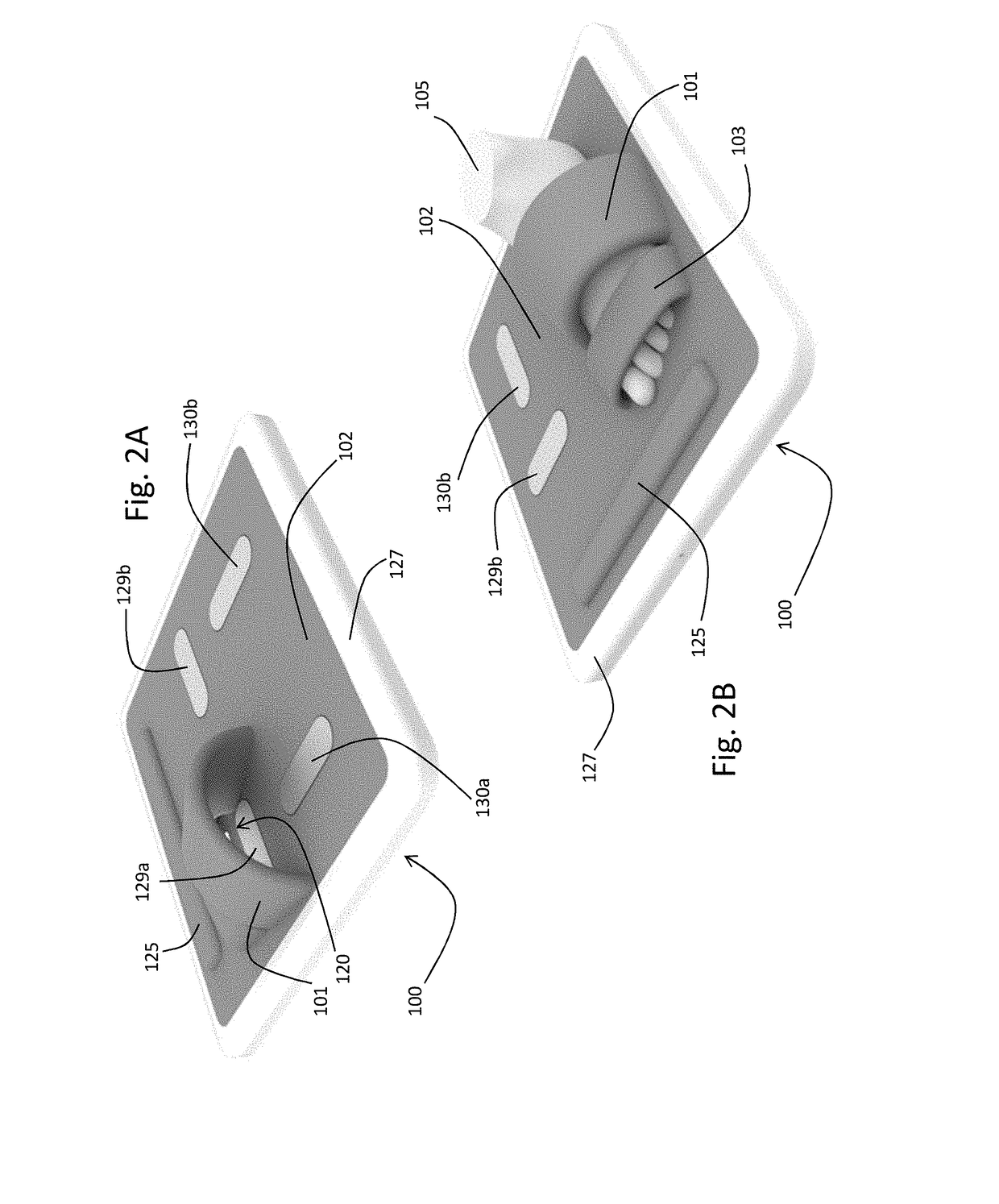
[0101]As shown in FIG. 1, the invention provides a stand-on sensor (“floormat”) 100 that measures a number of physiological parameters, e.g. vital signs (e.g. HR, RR, SpO2, SYS, DIA), hemodynamic parameters (CO, SV, TFI), and biometric parameters (weight, percent body fat, muscle mass) of a patient 105. More specifically, the floormat 100 measures these parameters from the patient's feet, as is described in more detail below. In this way, a comprehensive set of physiological data can be measured easily and on a daily basis while the patient 105 simply stands on the floormat 100, in a manner that is similar to how the patient would use a standard bathroom scale to weigh himself or herself.
[0102]Once the physiological information is obtained, the floormat 100 wirelessly transmits it, e.g., using a short-range wireless technology (suitably Bluetooth® wireless technology) to a mobile device 90, e.g., a conventional smartphone or tablet computer belonging to the patien...
PUM
 Login to View More
Login to View More Abstract
Description
Claims
Application Information
 Login to View More
Login to View More