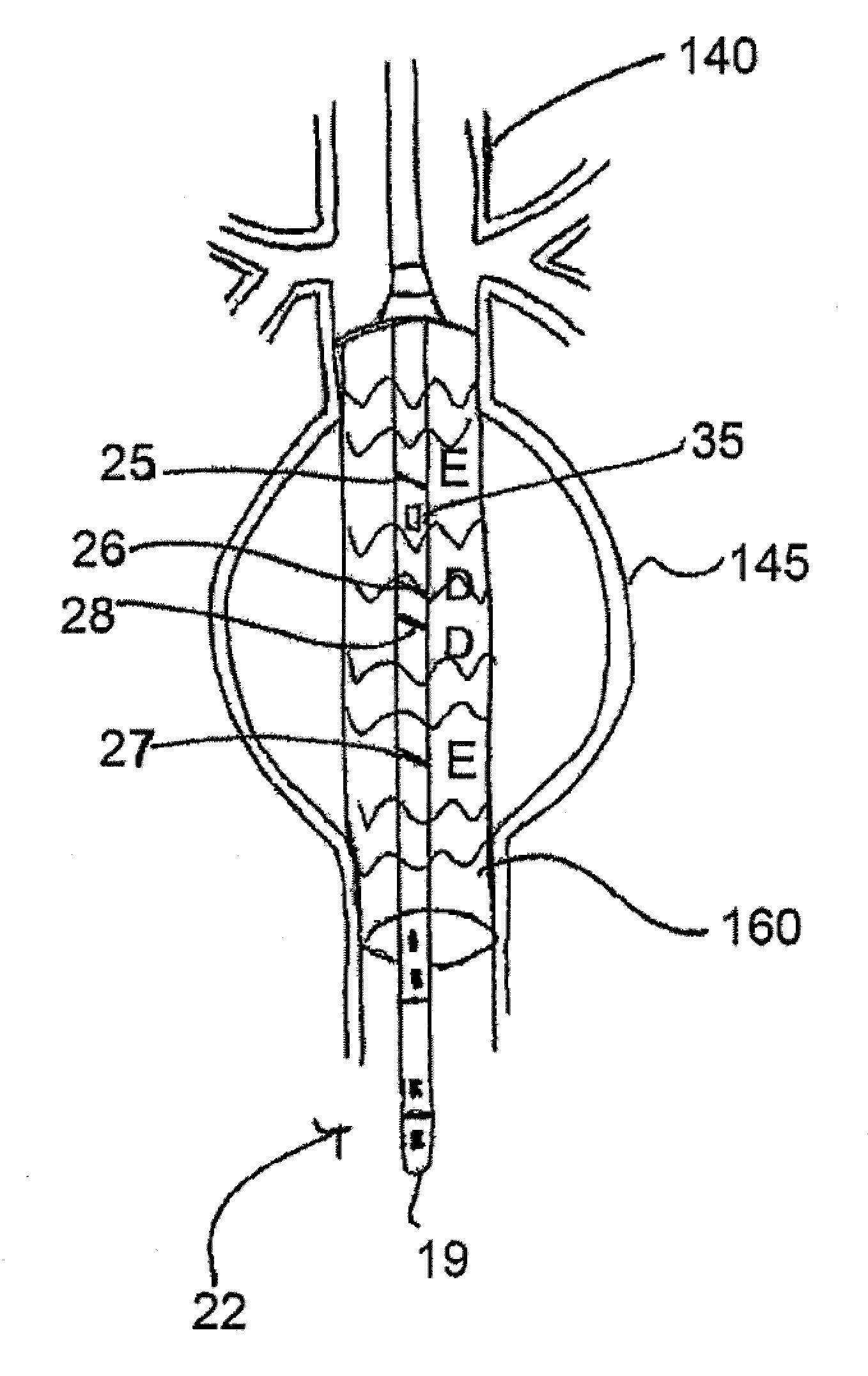
Such procedures require precise placement of the implanted devices within the target lumens, and can result in severe complications if such implantations are inaccurate.
When an area of the
aortic wall weakens, the pressure of the blood flowing through the weakened area causes the vessel wall to
balloon out, forming a blood-filled
aneurysm sack.
Although most aneurysms are initially small, aneurysms tend to enlarge over time.
Left untreated, the
aneurysm will frequently rupture, resulting in loss of blood through the rupture.
Left untreated, the AAA may rupture, resulting in rapid and usually fatal hemorrhaging.
In addition, substantial morbidity accompanies the procedure, resulting in a protracted
recovery period.
While surgical intervention may be required in
spite of these risks, certain patients may not be able to tolerate the stress of intra-
abdominal surgery.
For example, securing the
stent to a diseased region of the
aorta will result in a faulty seal that will not adequately reroute the
blood flow away from the aneurysmic region, thereby resulting in a reoccurrence of the condition.
As accurate placement of the
stent is critical,
visualization of the aortic structure has been an obstacle for proper navigation during delivery of the
stent.
CHF is a
disease condition in which the heart fails to function efficiently as a pump and cannot provide sufficient
blood flow and / or pressure to satisfy the normal circulatory needs of a patient.
A patient with acute CHF often experiences sudden shortness of breath,
fainting, and irregular heart beats that require frequent emergency room treatments.
In its chronic form, CHF leads to repeated hospital stays, a deterioration in
quality of life, and significant costs to the healthcare
system.
In about 30% of CHF patients, the
disease process compromises the myocardium's ability to contract, which thereby alters the conduction pathways through the heart.
When a patient exhibits damage to the electrical
system of the heart, as is often seen in patients with CHF, severe issues may arise.
Disruption of the conductance pathways through the heart can cause a
delay in the beginning of right or left ventricular
systole and thereby induce asynchronous atrial and ventricular activation.
Alterations in ventricular
contractility frequently compromise the ability of the
failing heart to eject blood and may consequently increase the severity of the regurgitant flow through the
mitral valve.
In patients exhibiting these severe symptoms, the intraventricular conduction delays lead to clinical
instability associated with a greatly
increased risk of death.
Due to the required placement of the third lead, the implantation and maintenance of a CRT device are associated with a greater risk than the implantation and maintenance of a standard pacemaker device.
Primarily, it is a difficult procedure to advance the pacing lead into the
coronary sinus and cardiac veins and, thus, implantation fails in approximately 8% of patients.
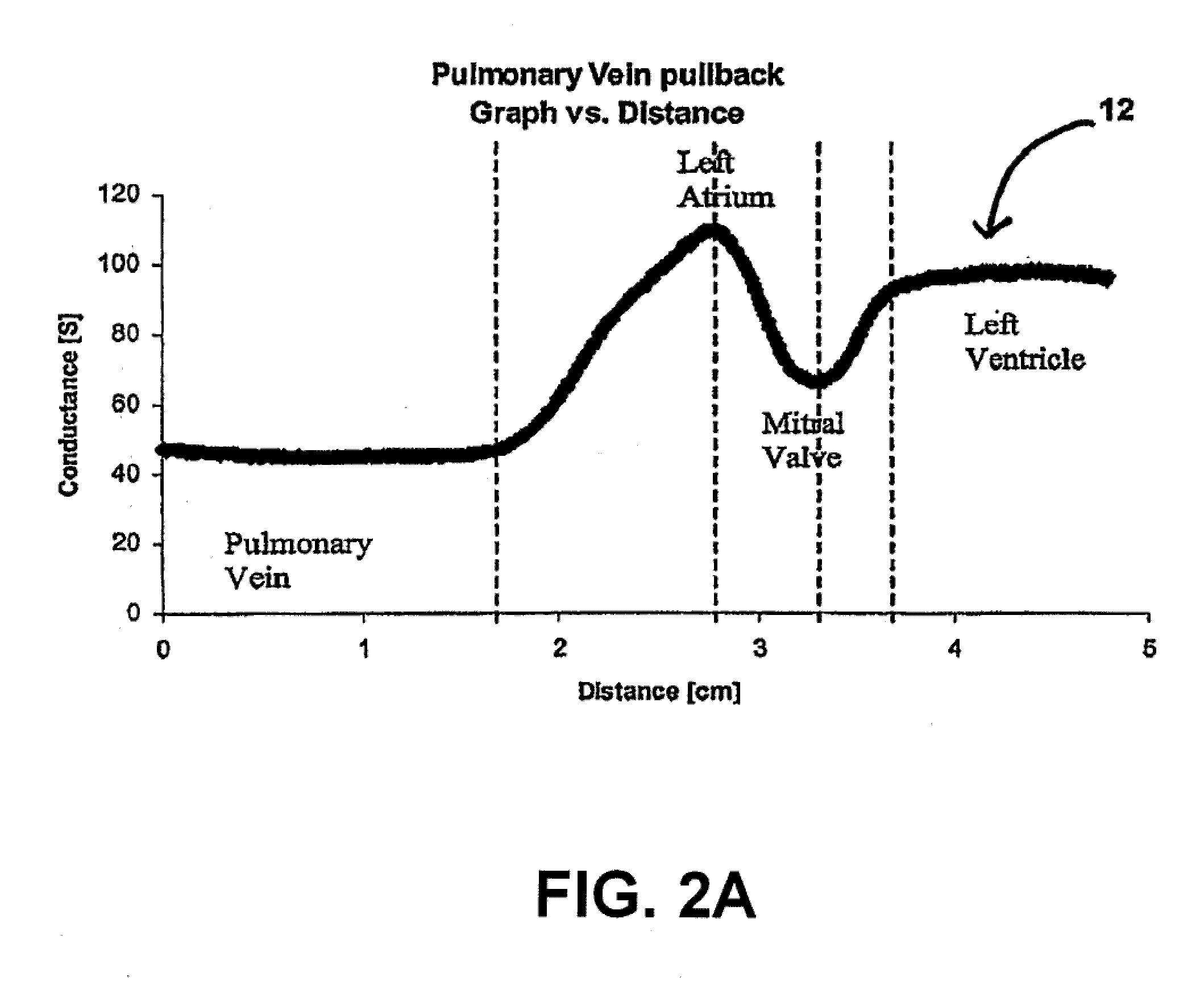
This process, however, is not particularly accurate and does not provide a detailed profile of the
coronary sinus.
 Login to View More
Login to View More  Login to View More
Login to View More