Coaxial catheter instruments for ablation with radiant energy
- Summary
- Abstract
- Description
- Claims
- Application Information
AI Technical Summary
Benefits of technology
Problems solved by technology
Method used
Image
Examples
Embodiment Construction
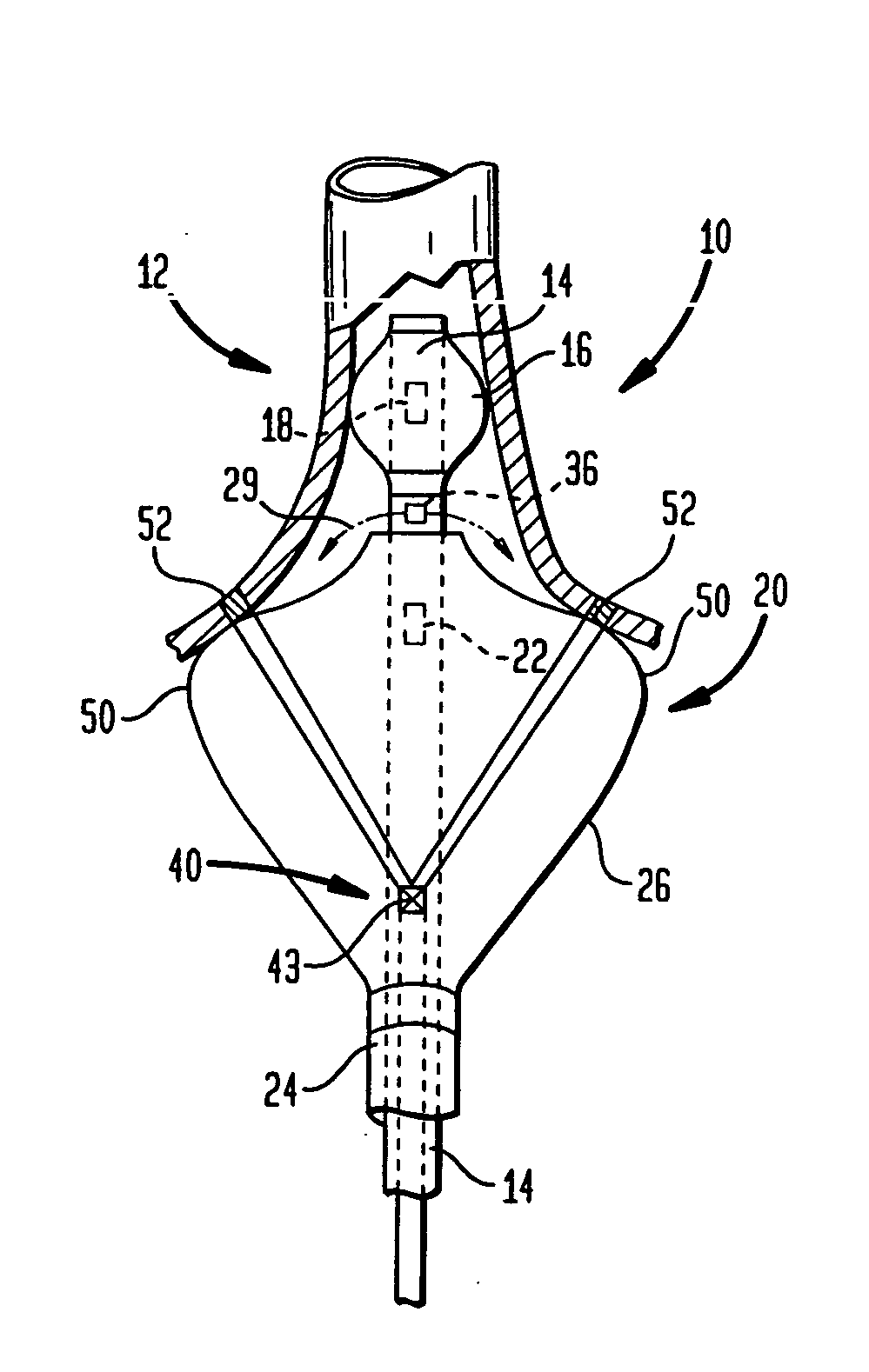
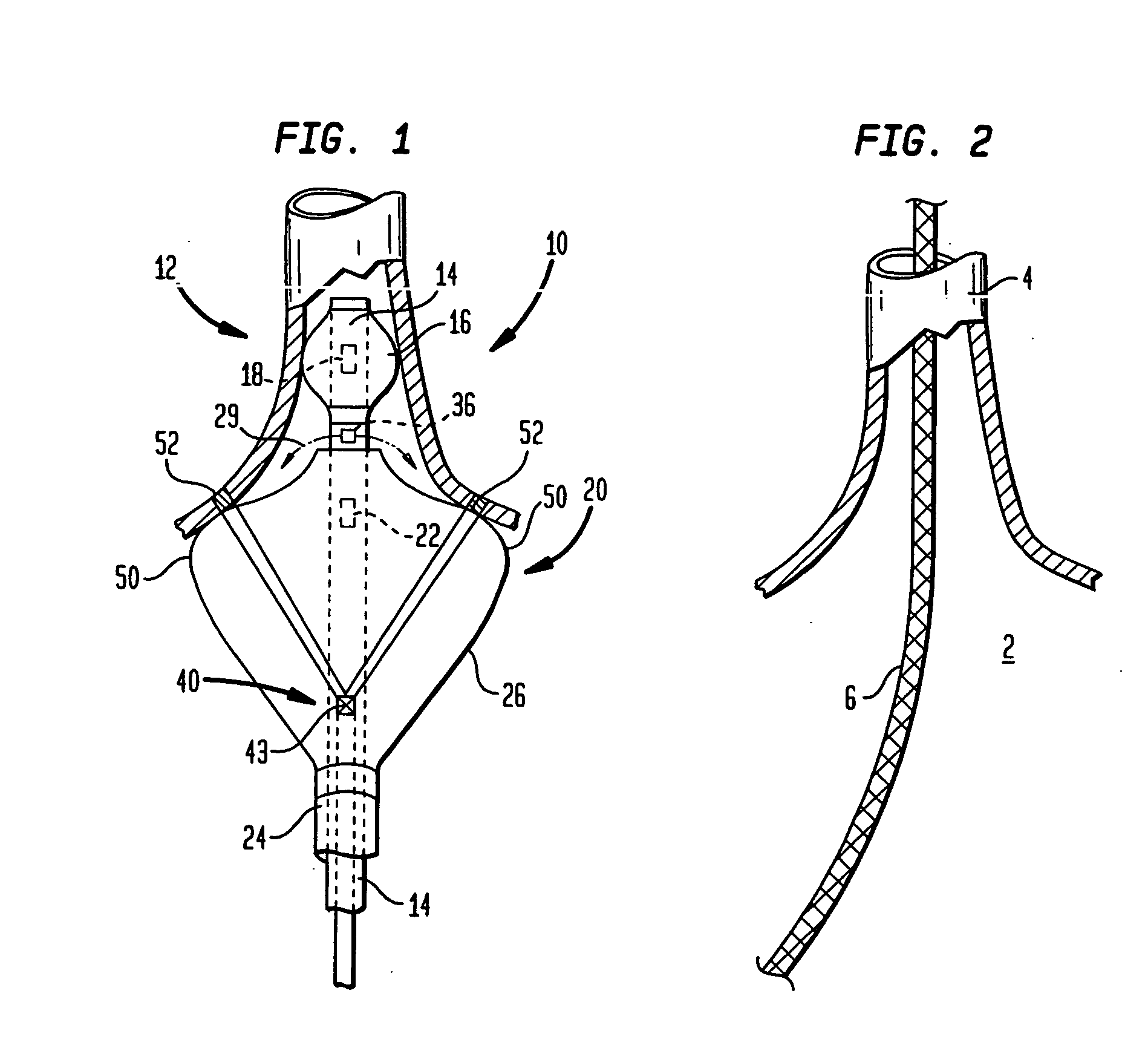
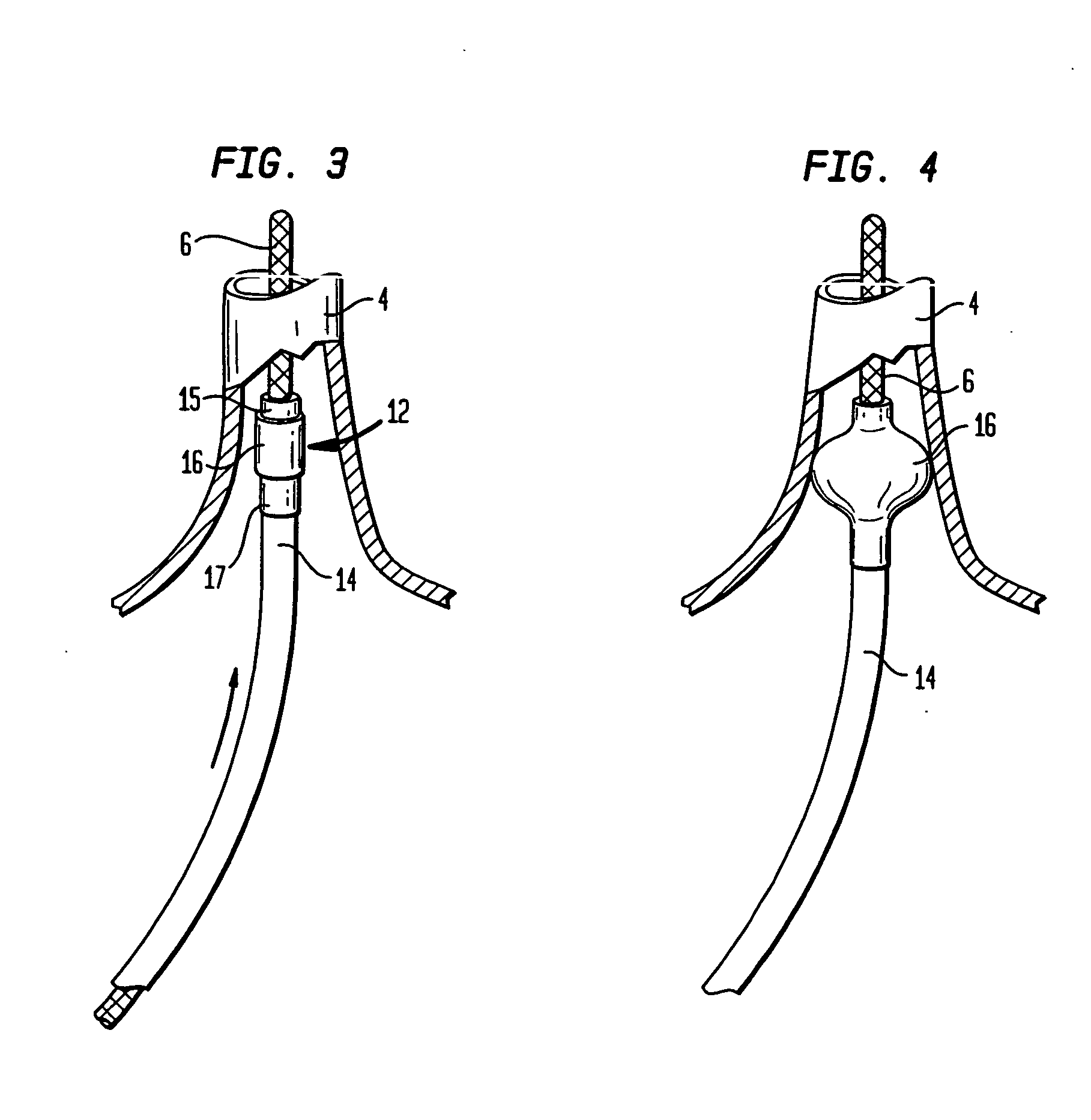
[0069]FIG. 1 provides a schematic, cross-sectional view of a coaxial catheter ablation instrument 10 according to the invention, including a first, inner catheter 12 having an elongate body 14 and an anchor balloon 16, inflatable via one or more ports 18. A fluid for inflating the anchor balloon can be delivered through a passageway (not shown) within the elongate body or via one or more of the lumens of the device, as discussed in more detail below. The device can further include a second, coaxial, outer catheter 20 having an elongate body 24 and a projection balloon 26 inflatable via one or more ports 22. The instrument is preferably designed such that upon anchorage of the anchor balloon 16 within the heart (e.g., within a pulmonary vein), the projection balloon can be inflated such a shoulder portion 50 of the balloon 26 will be urged into close proximity with a target region 52 of cardiac tissue (e.g. an annular region of the atrial heart wall surrounding the ostium of a pulmon...
PUM
| Property | Measurement | Unit |
|---|---|---|
| Luminous flux | aaaaa | aaaaa |
| Frequency | aaaaa | aaaaa |
| Frequency | aaaaa | aaaaa |
Abstract
Description
Claims
Application Information
 Login to View More
Login to View More