Patents
Literature
362results about "Wrist joints" patented technology
Efficacy Topic
Property
Owner
Technical Advancement
Application Domain
Technology Topic
Technology Field Word
Patent Country/Region
Patent Type
Patent Status
Application Year
Inventor
Osteogenic implants derived from bone
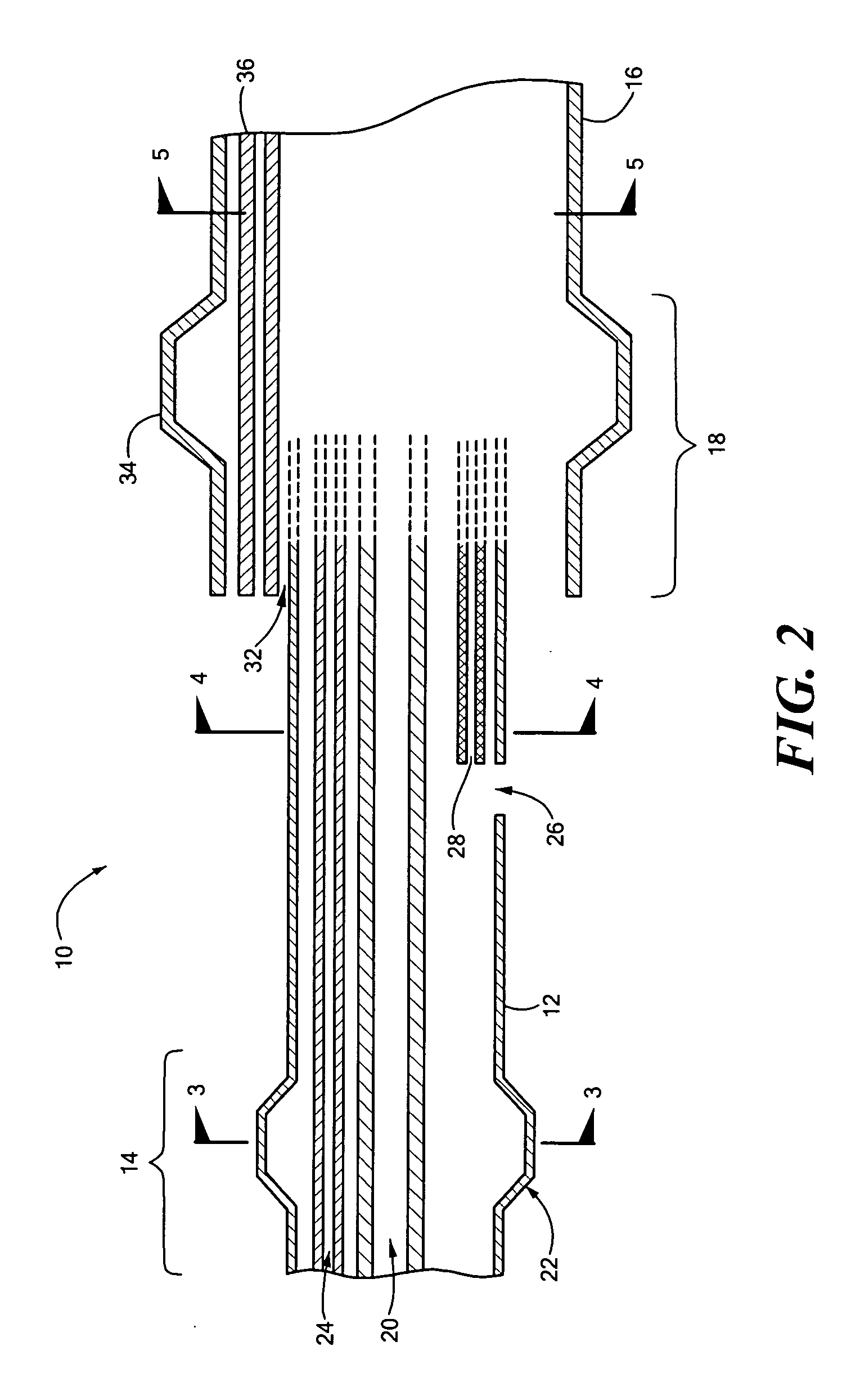
An osteogenic osteoimplant in the form of a flexible sheet comprising a coherent mass of bone-derived particles, the osteoimplant having a void volume not greater than about 32% and a method of making an osteogenic osteoimplant having not greater than about 32% void volume, the method comprising: providing a coherent mass of bone-derived particles; and, mechanically shaping the coherent mass of bone-derived particles to form an osteogenic osteoimplant in the form of a flexible sheet.
Owner:WARSAW ORTHOPEDIC INC
Patient selectable joint arthroplasty devices and surgical tools facilitating increased accuracy, speed and simplicity in performing total and partial joint arthroplasty
Disclosed herein are methods, compositions and tools for repairing articular surfaces repair materials and for repairing an articular surface. The articular surface repairs are customizable or highly selectable by patient and geared toward providing optimal fit and function. The surgical tools are designed to be customizable or highly selectable by patient to increase the speed, accuracy and simplicity of performing total or partial arthroplasty.
Owner:CONFORMIS
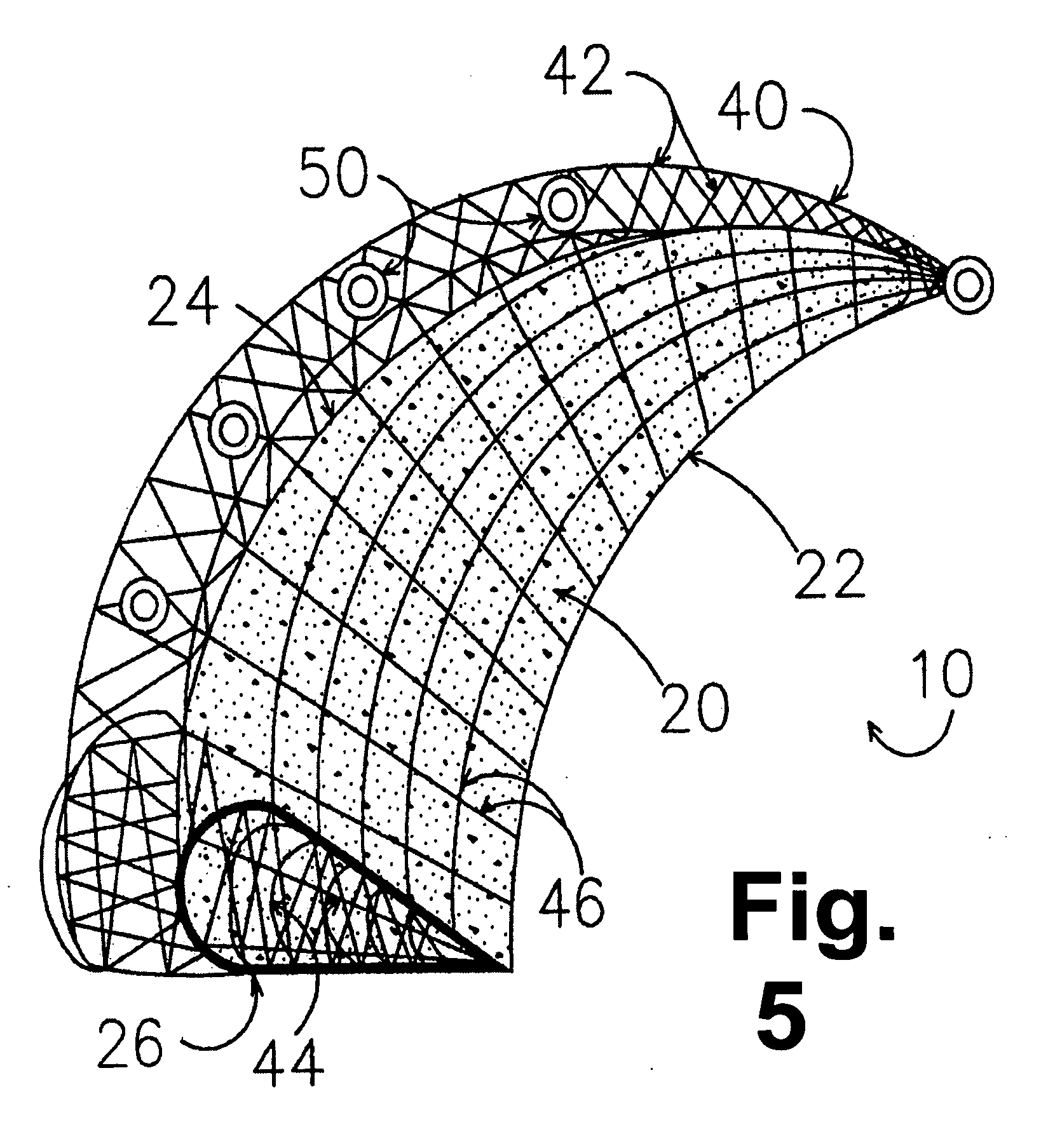
Implants for replacing cartilage, with negatively-charged hydrogel surfaces and flexible matrix reinforcement
ActiveUS9314339B2Strong and durableStrong and secure anchoringFinger jointsWrist jointsFiberChemical agent
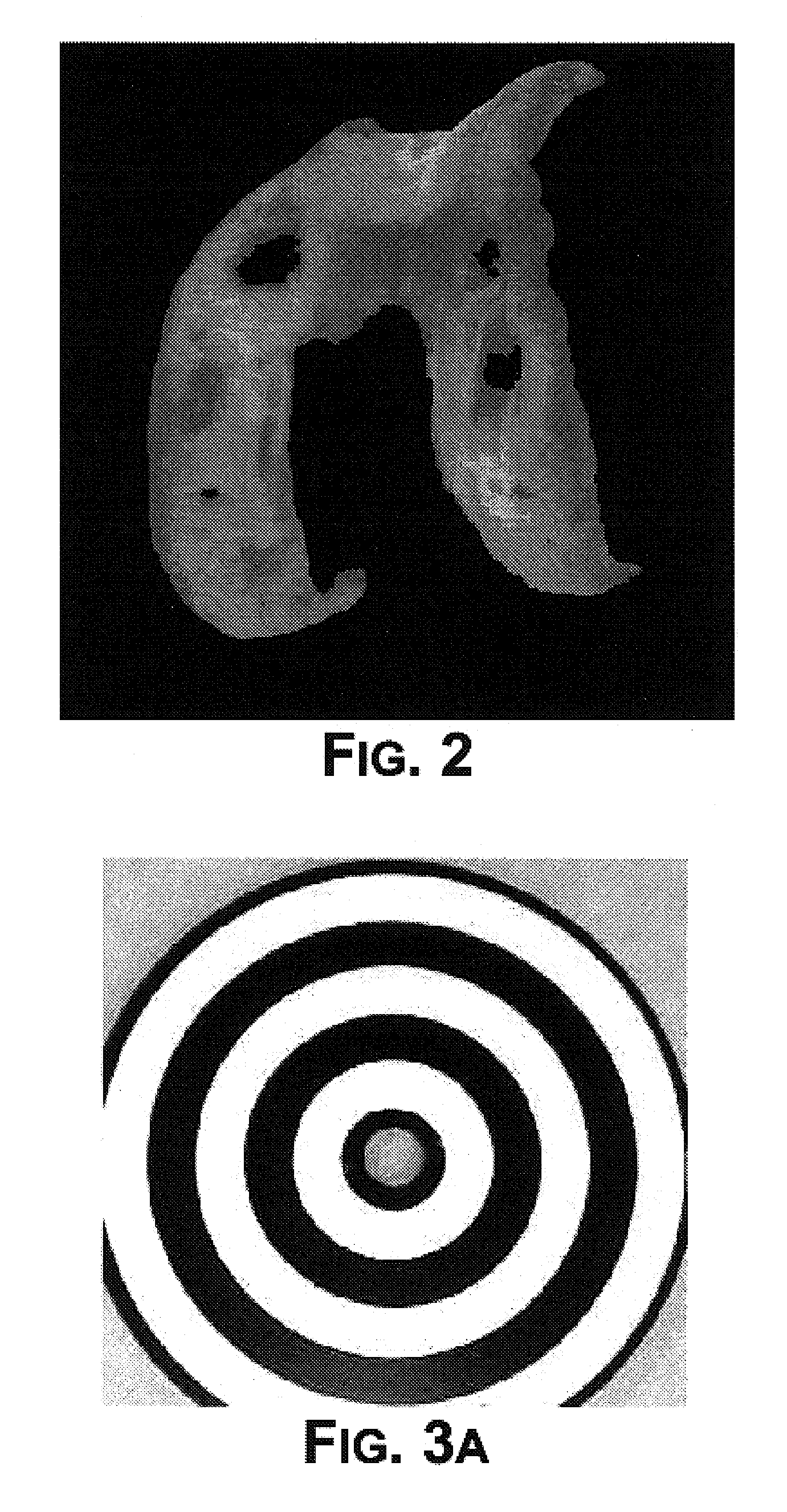
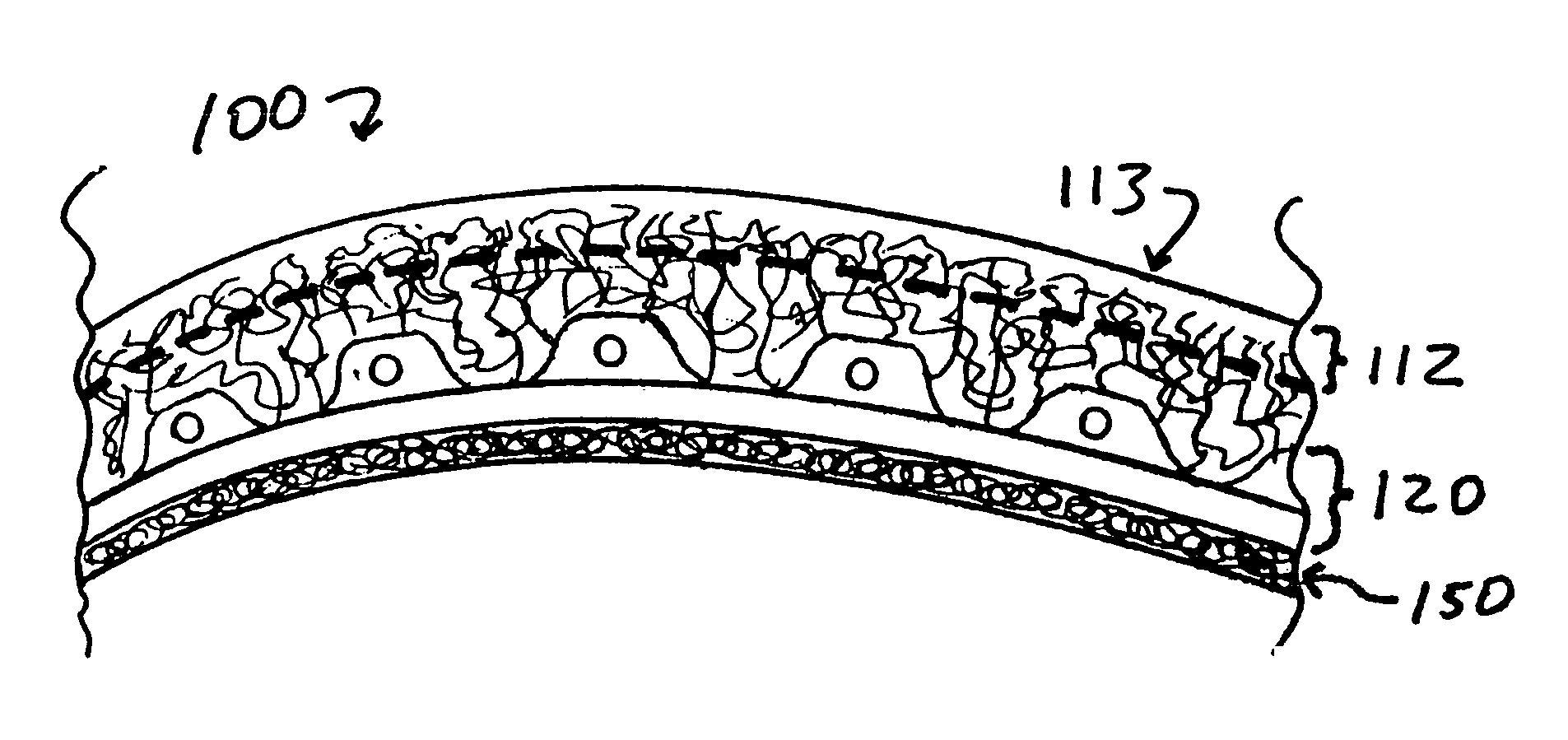
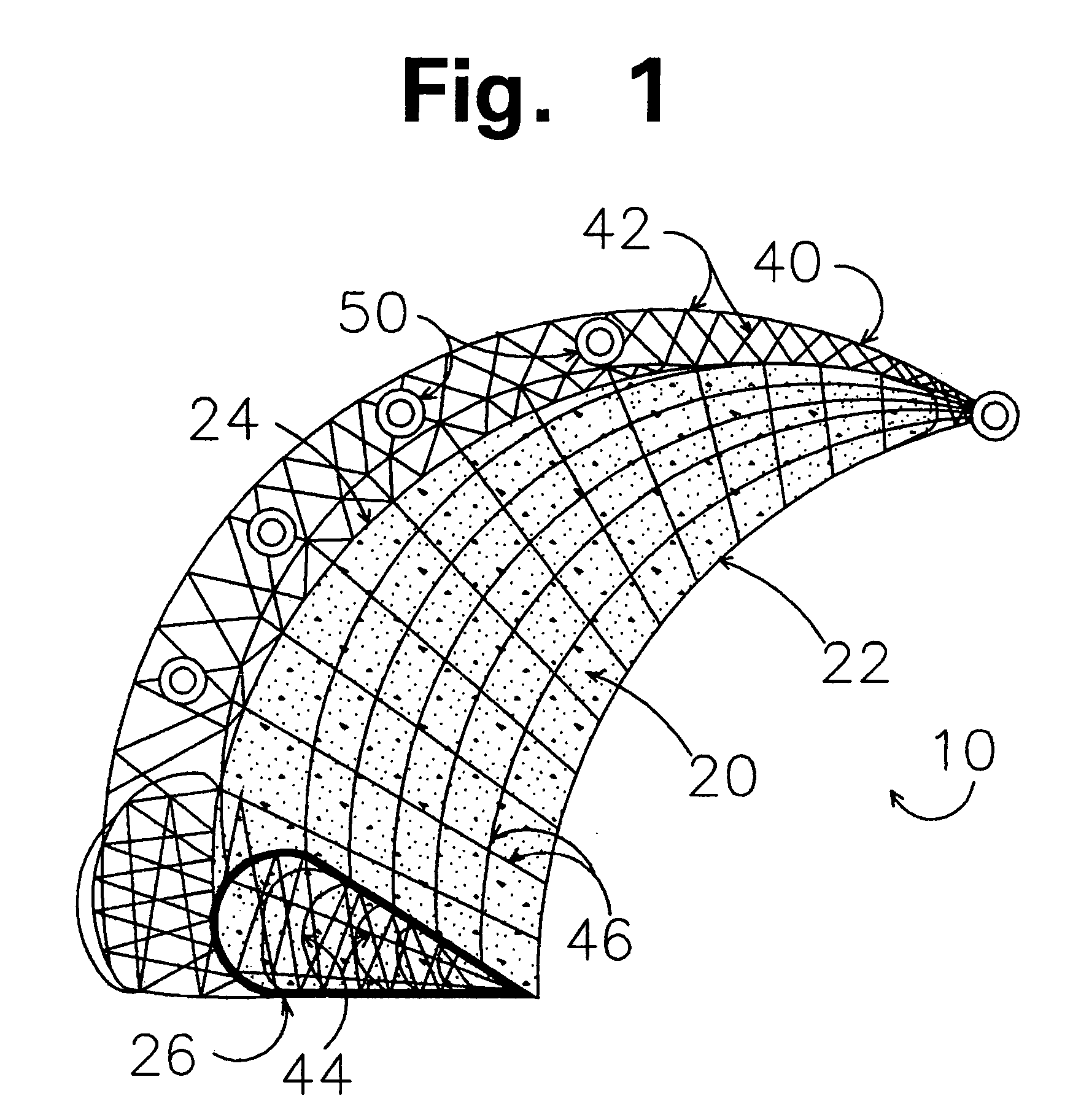
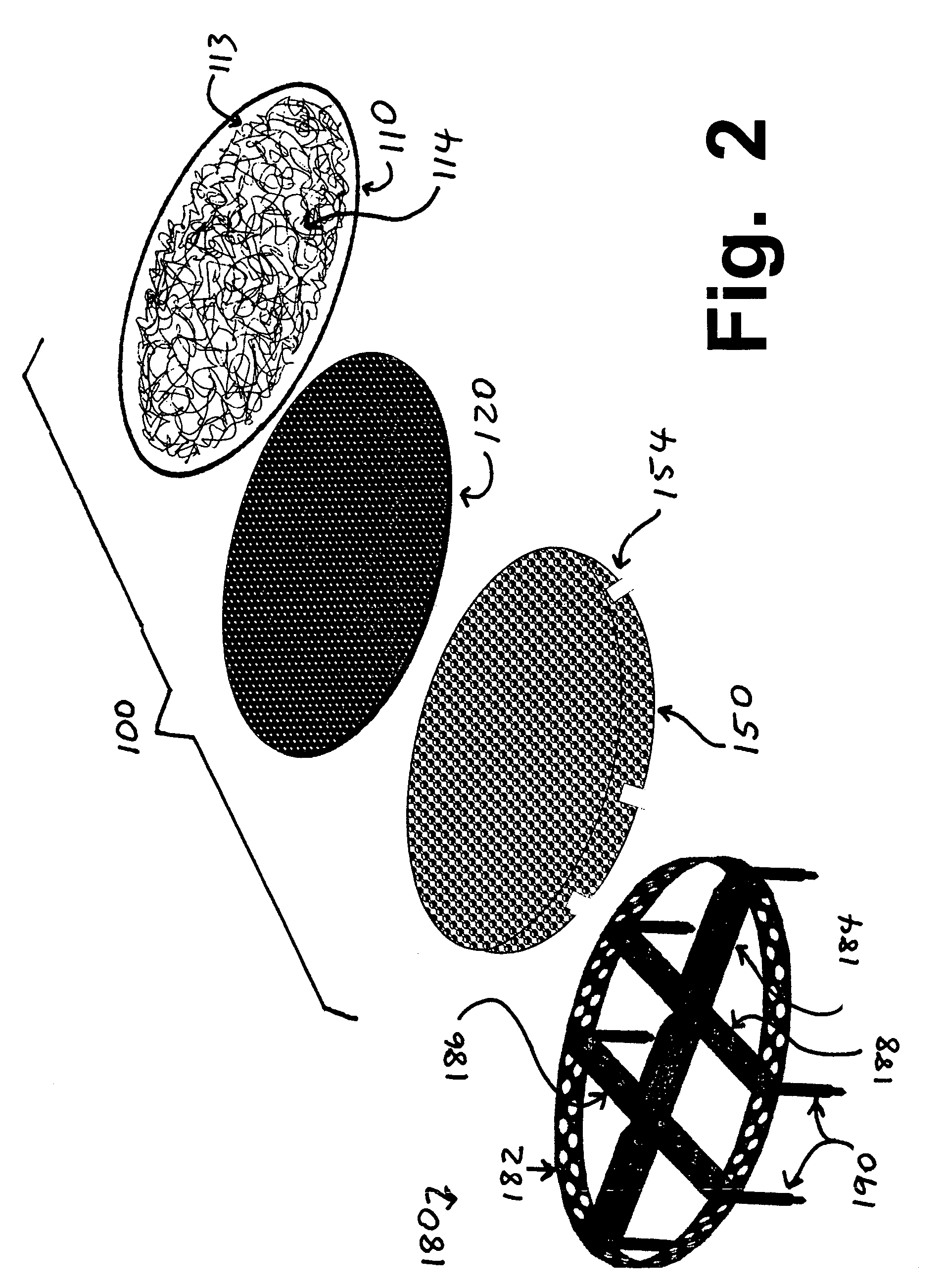
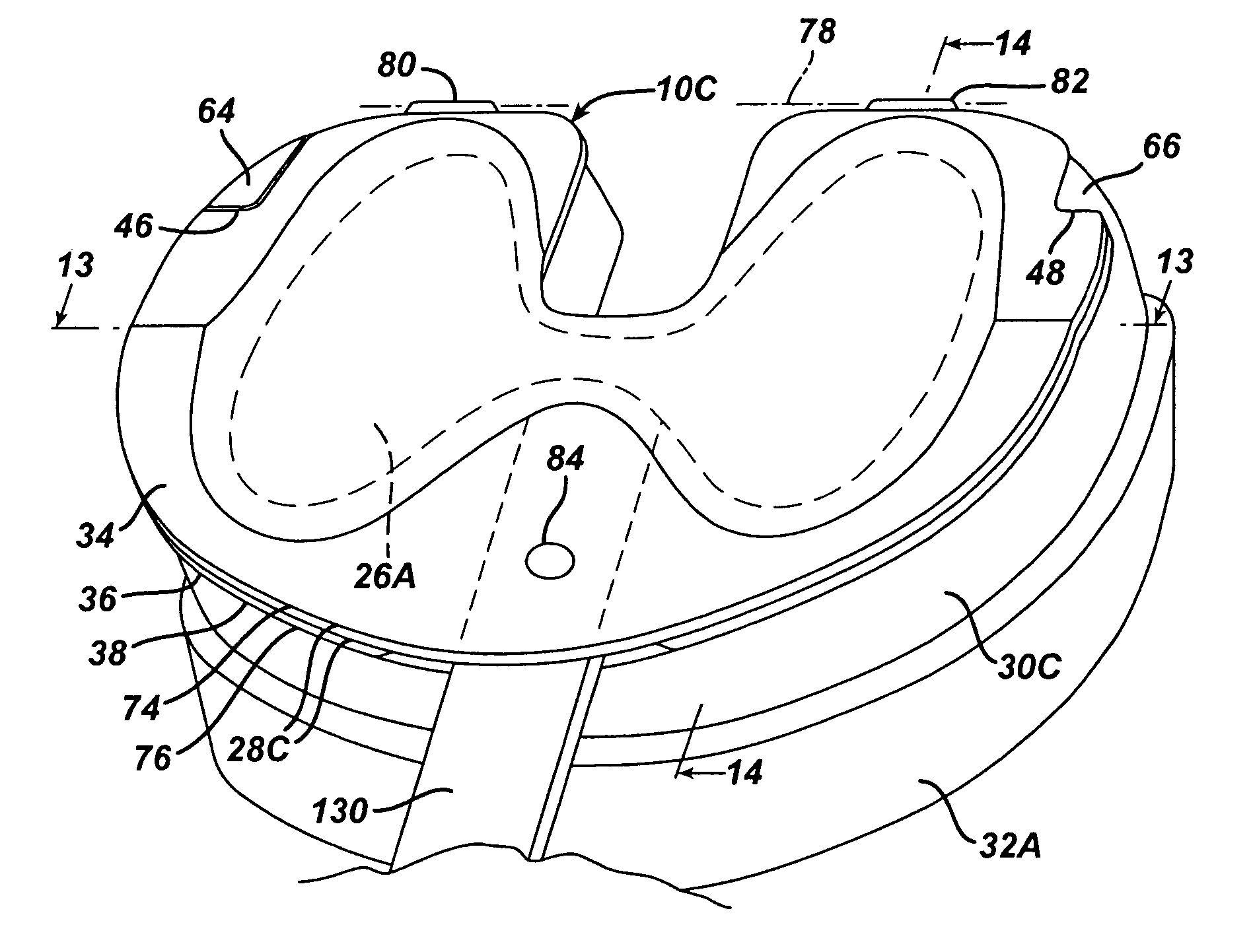
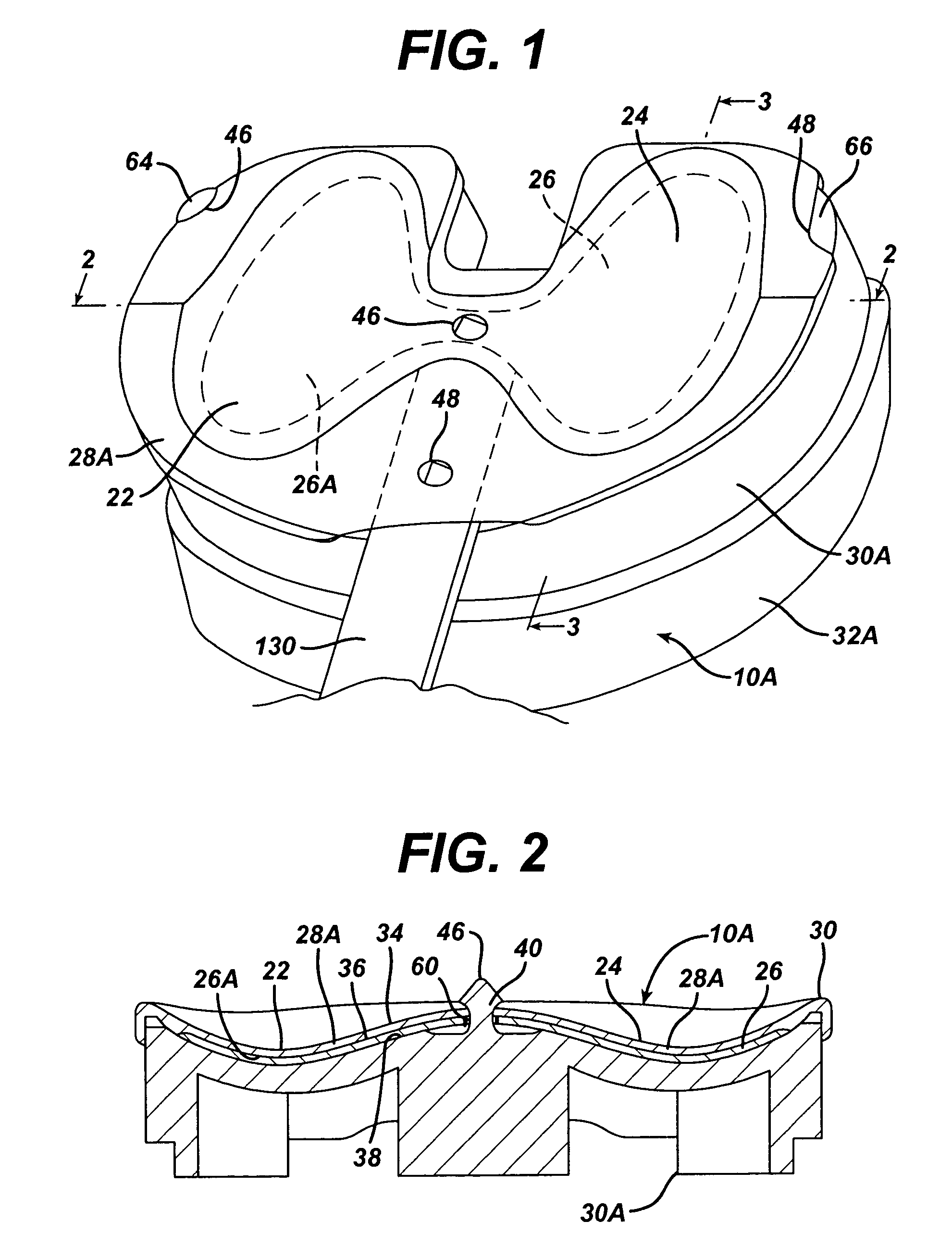
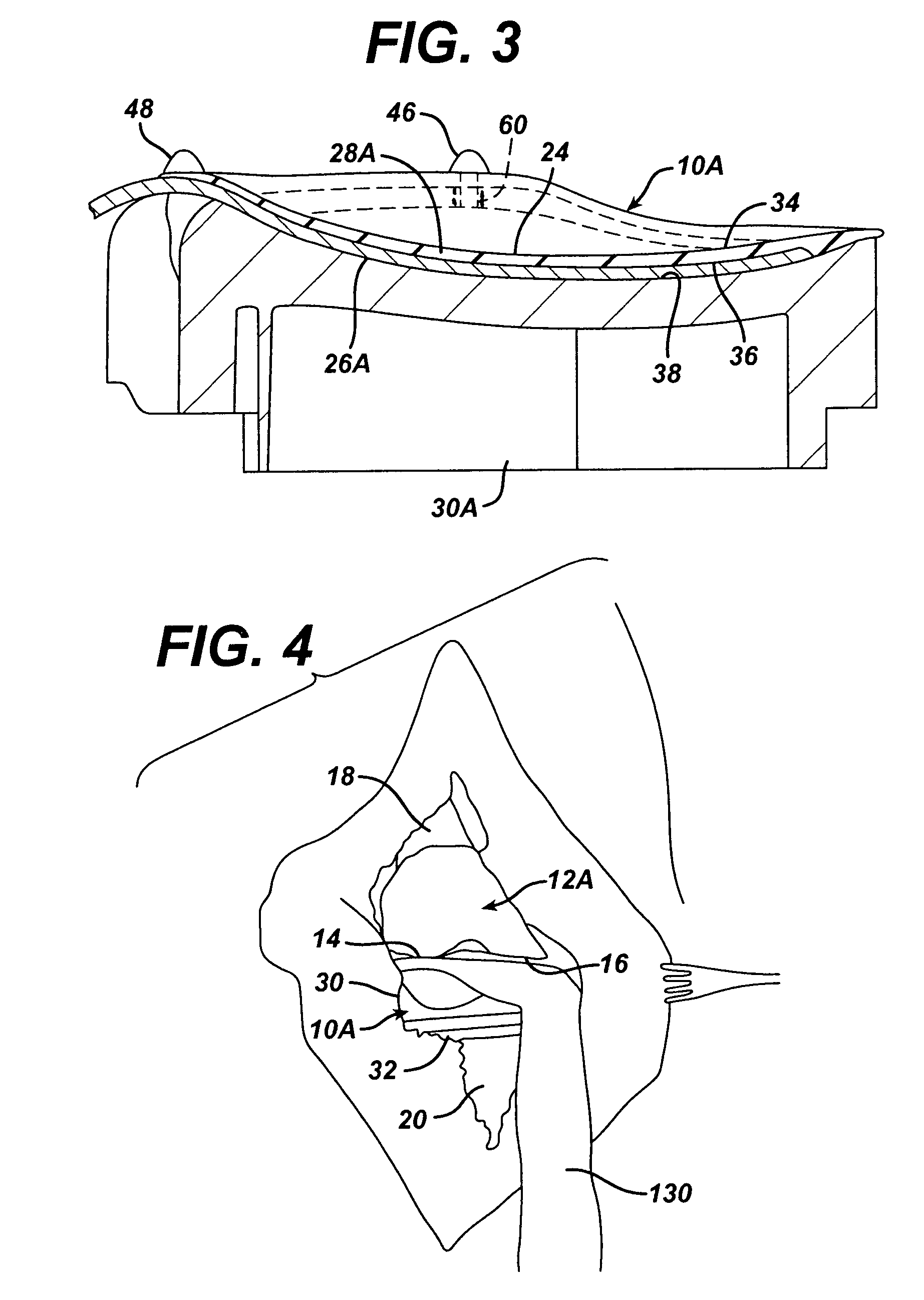
A permanent non-resorbable implant allows surgical replacement of cartilage in articulating joints, using a hydrogel material (such as a synthetic polyacrylonitrile polymer) reinforced by a flexible fibrous matrix. Articulating hydrogel surface(s) are chemically treated to provide a negative electrical charge that emulates the negative charge of natural cartilage, and also can be treated with halogenating, cross-linking, or other chemical agents for greater strength. For meniscal-type implants, the reinforcing matrix can extend out from the peripheral rim of the hydrogel, to allow secure anchoring to soft tissue such as a joint capsule. For bone-anchored implants, a porous anchoring layer enables tissue ingrowth, and a non-planer perforated layer can provide a supportive interface between the hard anchoring material and the softer hydrogel material.
Owner:FORMAE
Implant Device and Method for Manufacture
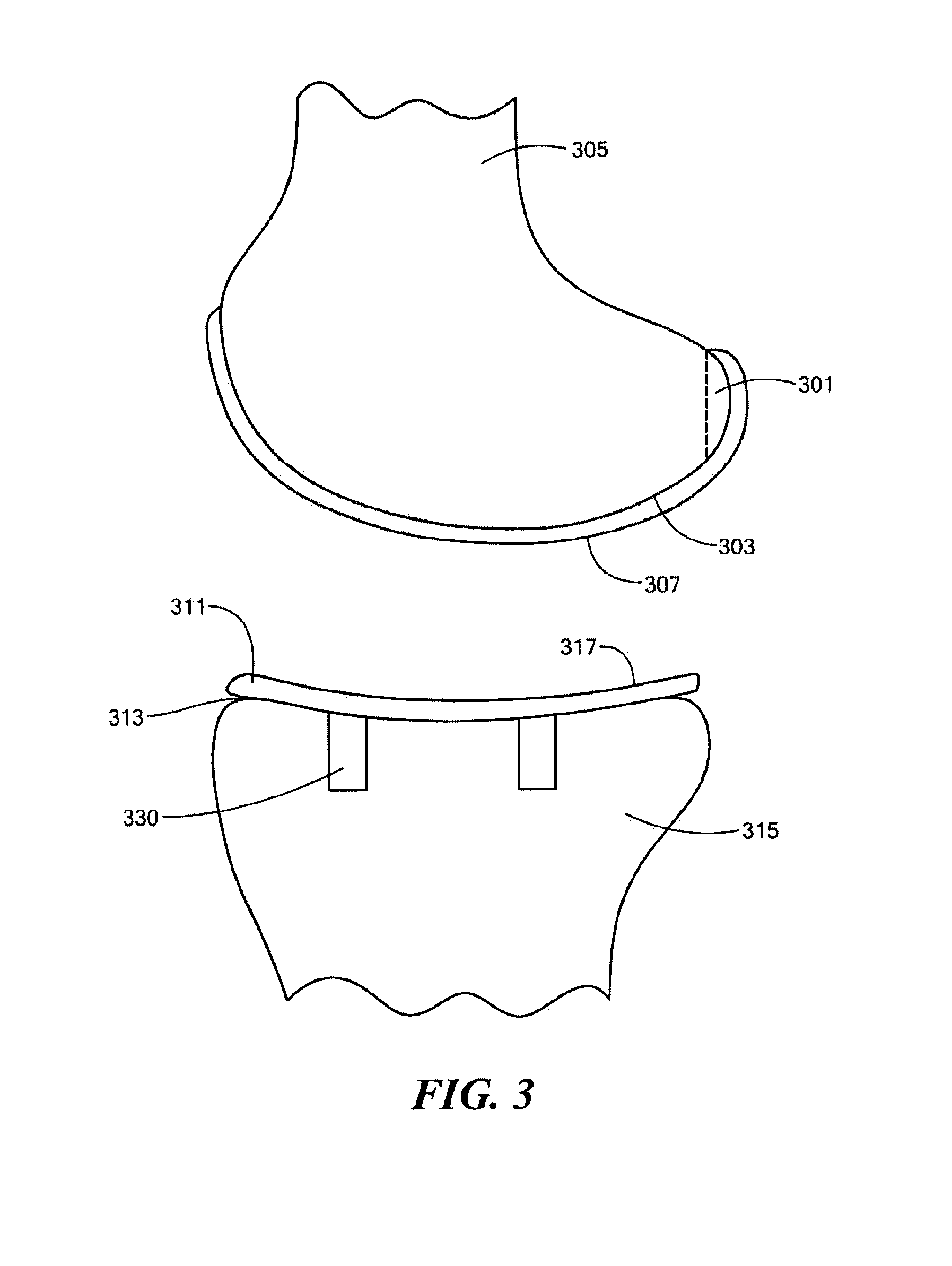
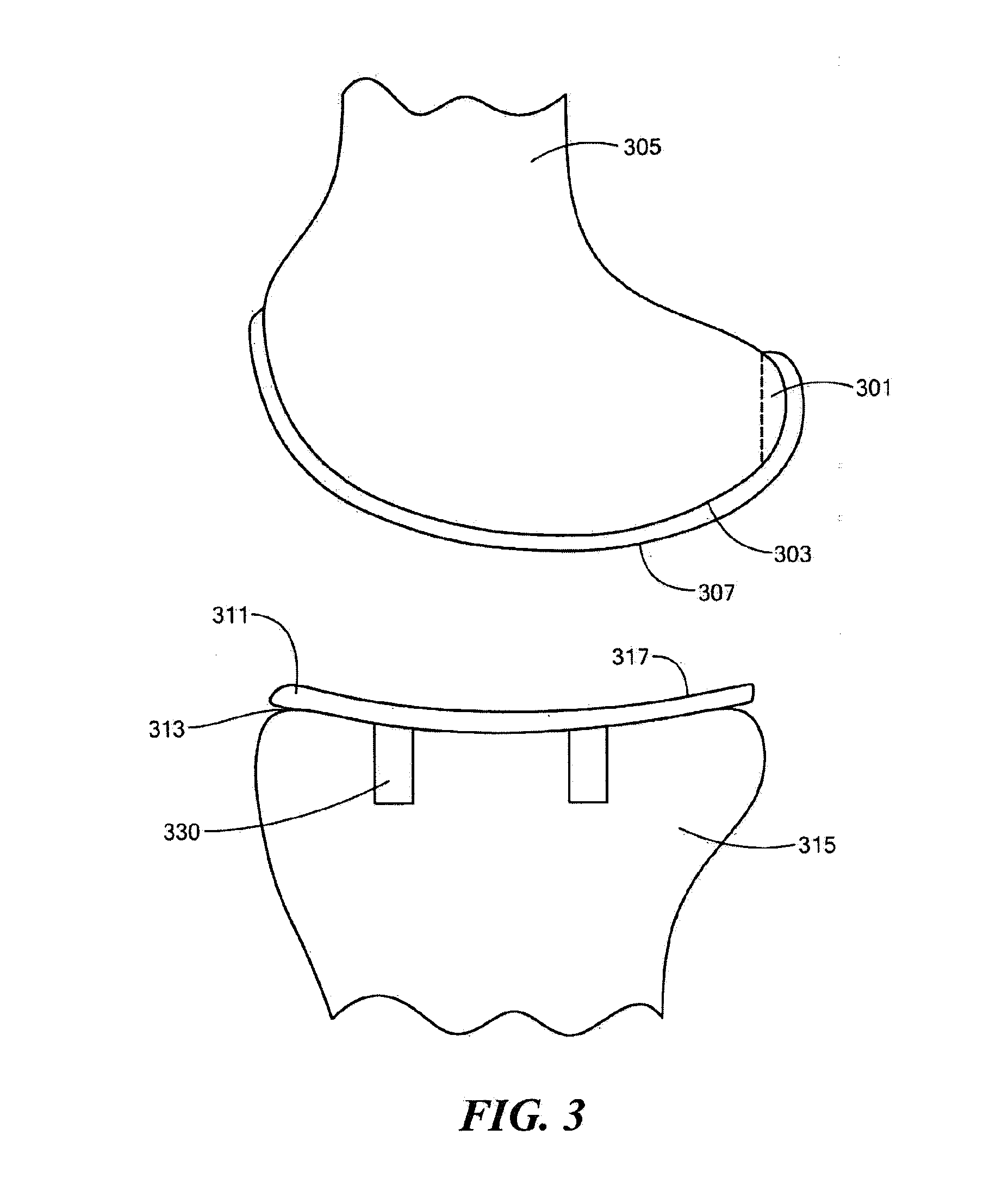
A knee implant includes a femoral component having first and second femoral component surfaces. The first femoral component surface is for securing to a surgically prepared compartment of a distal end of a femur. The second femoral component surface is configured to replicate the femoral condyle. The knee implant further includes a tibial component having first and second tibial component surfaces. The first tibial component surface is for contacting a proximal surface of the tibia that is substantially uncut subchondral bone. At least a portion of the first tibial component surface is a mirror image of the proximal tibial surface. The second tibial component surface articulates with the second femoral component surface.
Owner:CONFORMIS
Prosthetic hip joint having sintered polycrystalline diamond compact articulation surfaces
InactiveUS6290726B1Improve wear resistanceReduce coefficient of frictionFinger jointsWrist jointsArticular surfacesProsthesis
Prosthetic joints, components for prosthetic joints, superhard bearing and articulation surfaces, diamond bearing and articulation surfaces, substrate surface topographical features, materials for making joints, bearing and articulation surfaces, and methods for manufacturing and finishing the same, and related information are disclosed, including a prosthetic hip joint having sintered polycrystalline diamond articulation.
Owner:DIAMICRON
Joint arthroplasty devices formed in situ
InactiveUS20070250169A1Improve accuracyImage analysisWrist jointsArticular surfacesJoint arthroplasty
Disclosed herein are methods and devices for repairing articular surfaces. The articular surface repairs are customizable or highly selectable by patient and geared toward providing optimal fit and function.
Owner:CONFORMIS
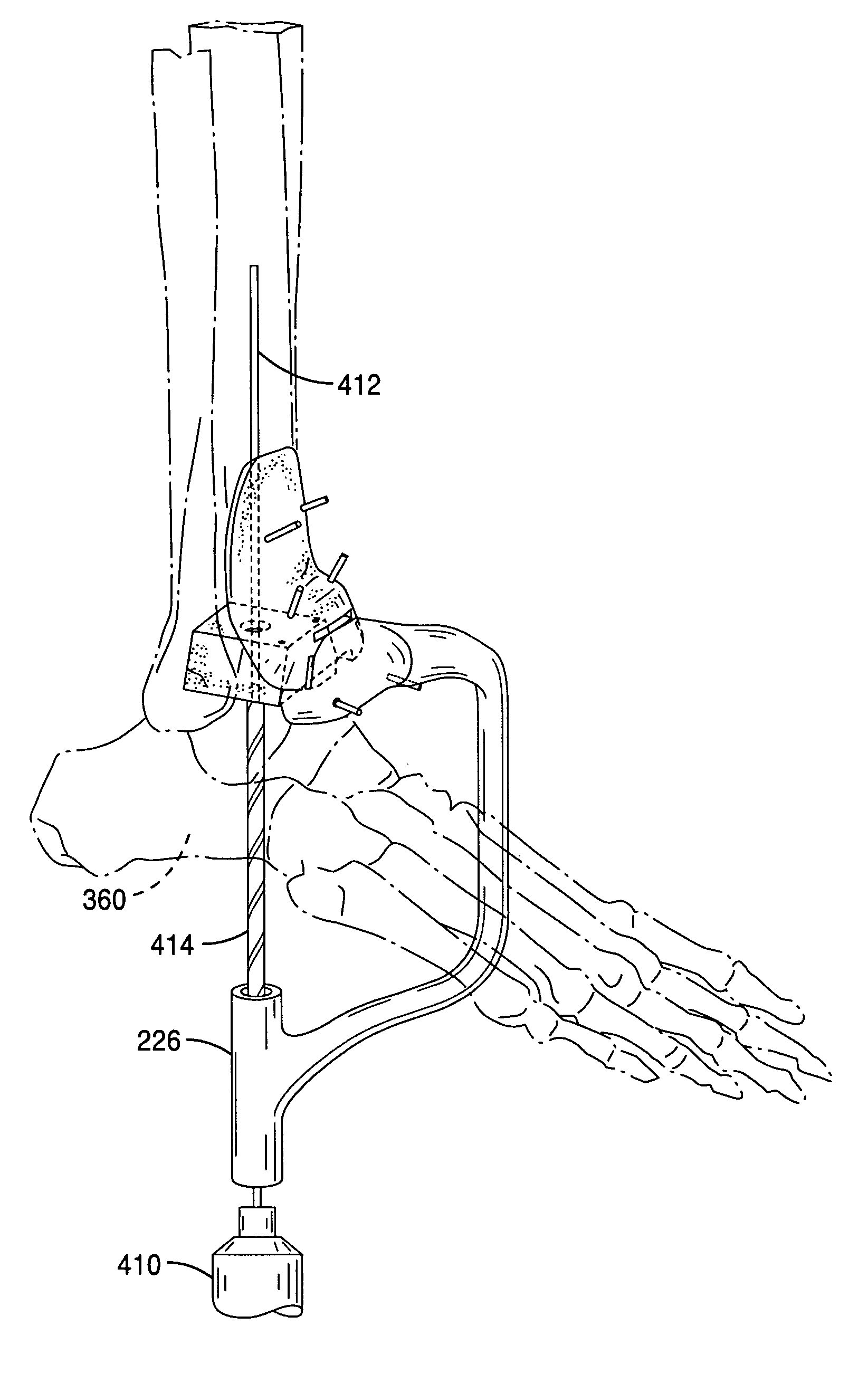
Custom radiographically designed cutting guides and instruments for use in total ankle replacement surgery
ActiveUS20100262150A1High precisionSimplify operating proceduresWrist jointsAnkle jointsTibiaSacroiliac joint
A system comprised of custom radiographically designed tibial and talar cutting guides, a tibial reaming guide and bit, and instrumentalities for use in total ankle replacement surgery and a computer-based system and method for making the custom radiographically designed tibial and talar cutting guides.
Owner:LIAN GEORGE JOHN
Minimally invasive joint implant with 3-dimensional geometry matching the articular surfaces
ActiveUS7799077B2Increase successFacilitating the integration of a wide variety of cartilageFinger jointsWrist jointsArticular surfacesArticular surface
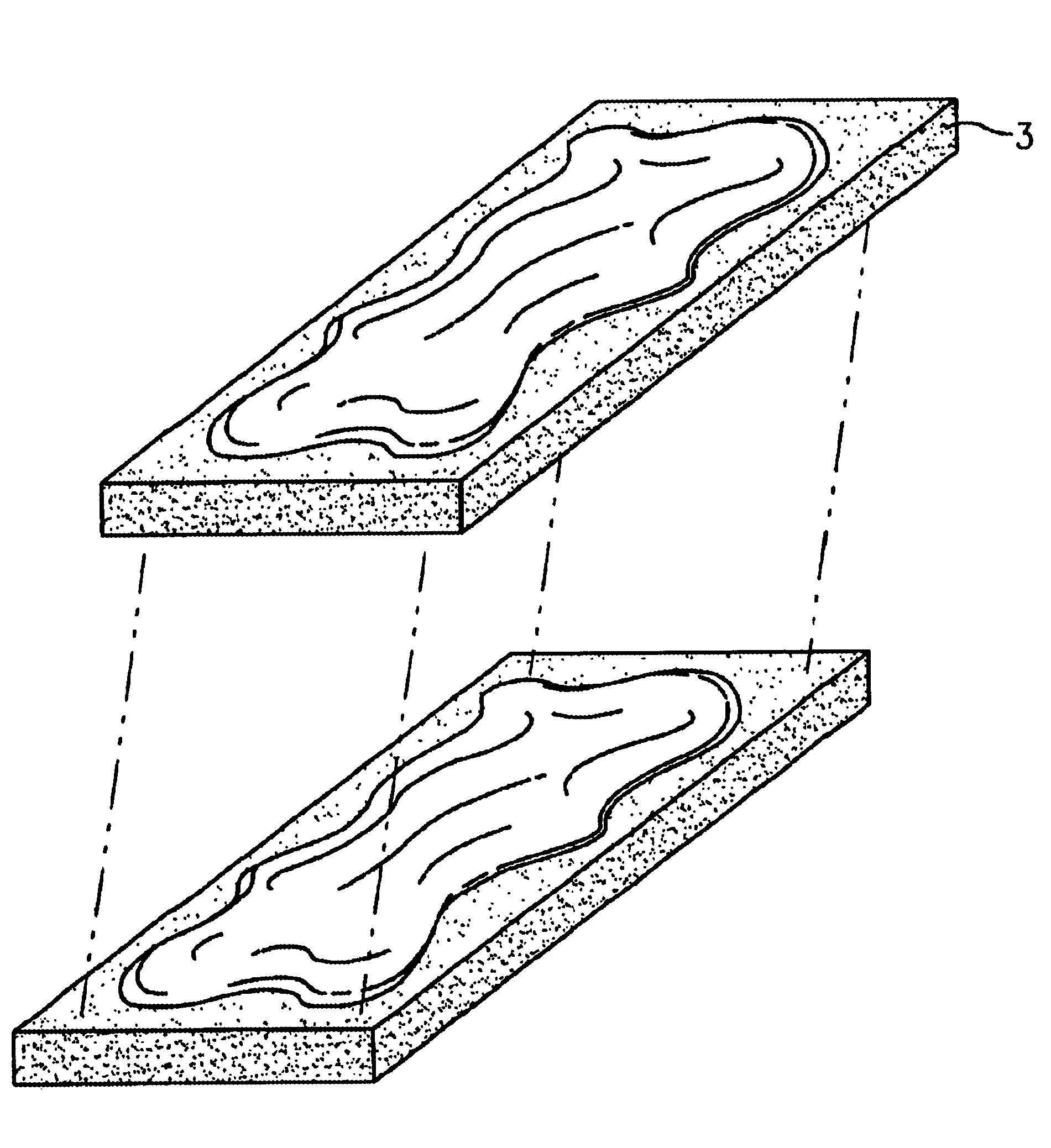
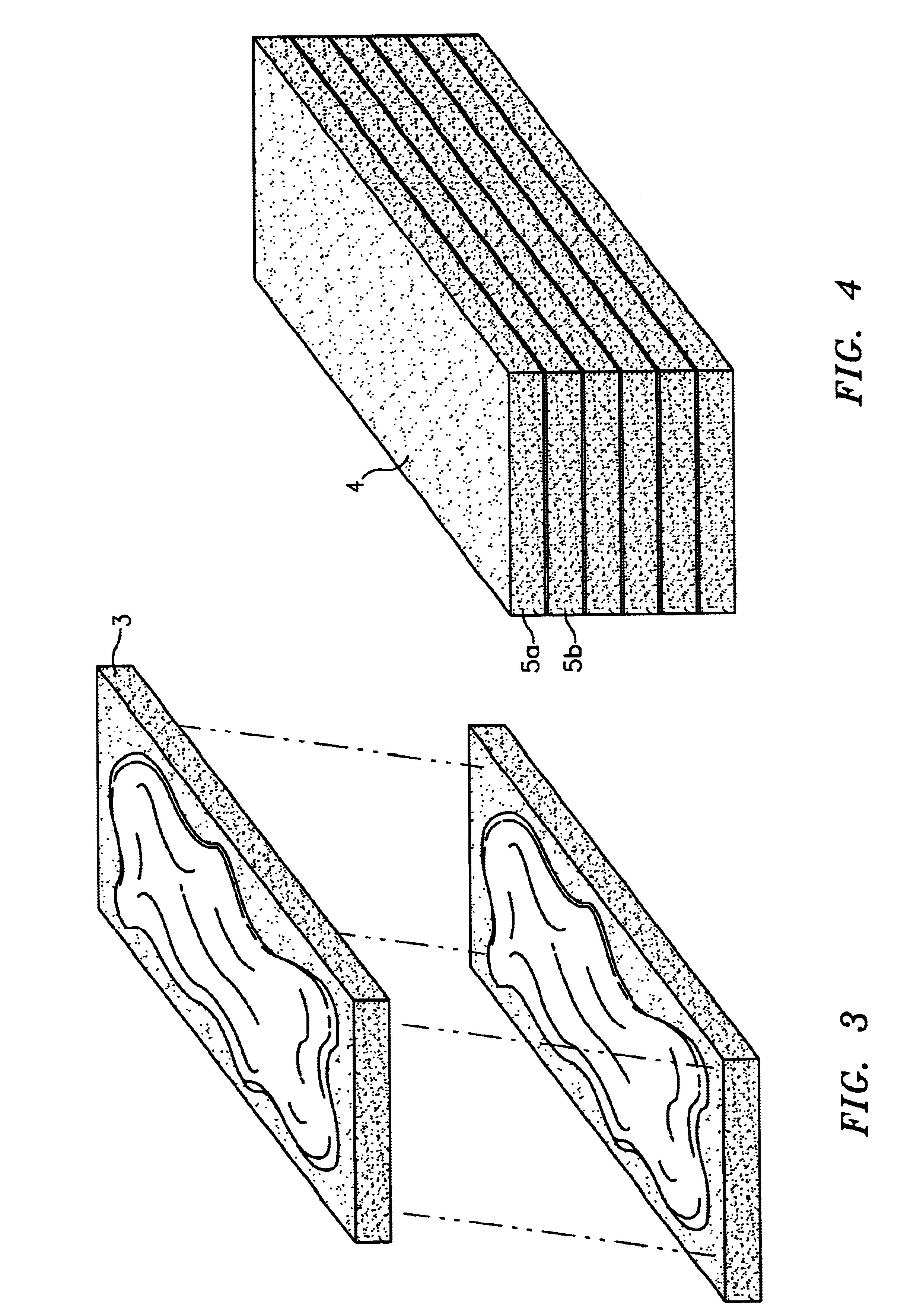
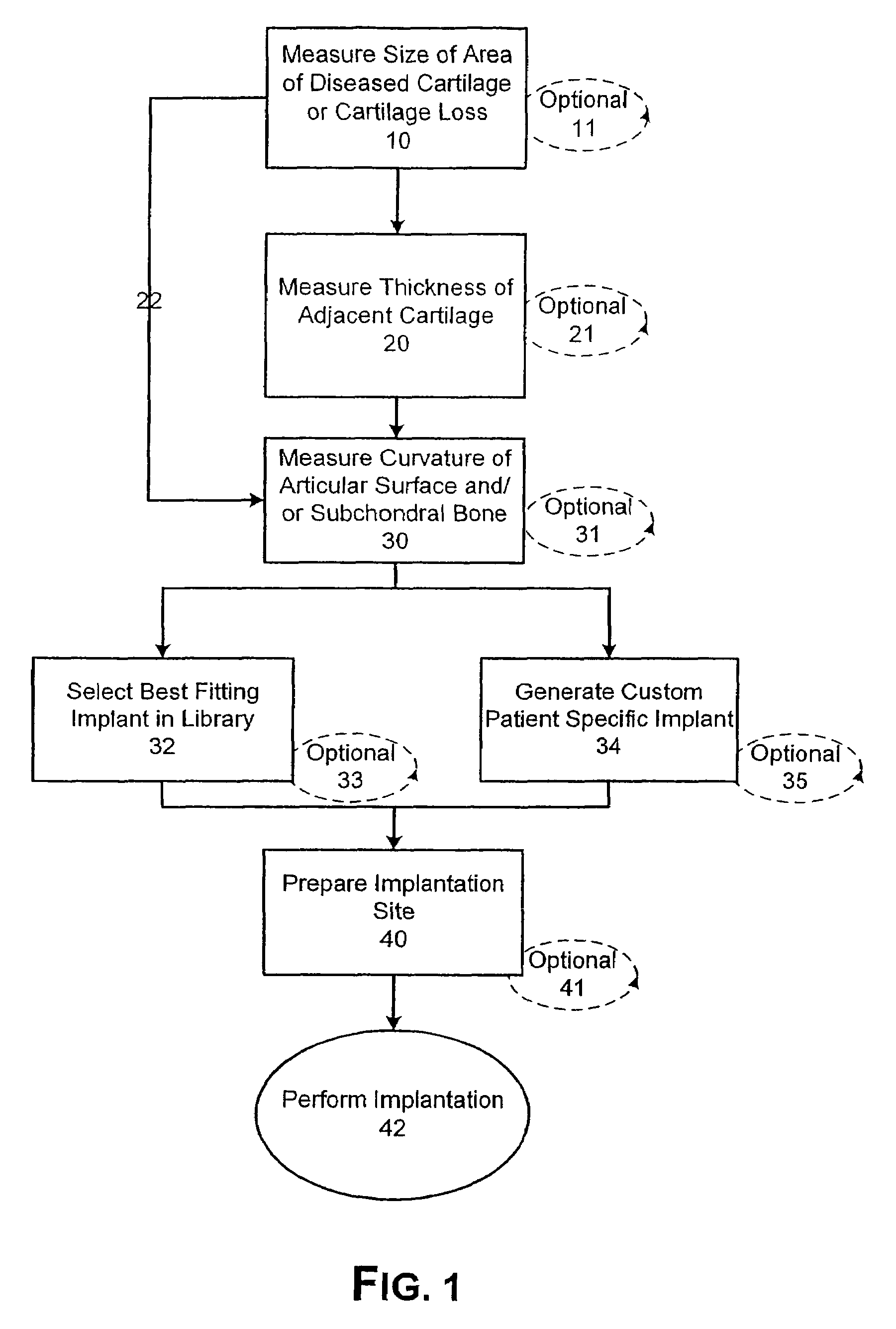
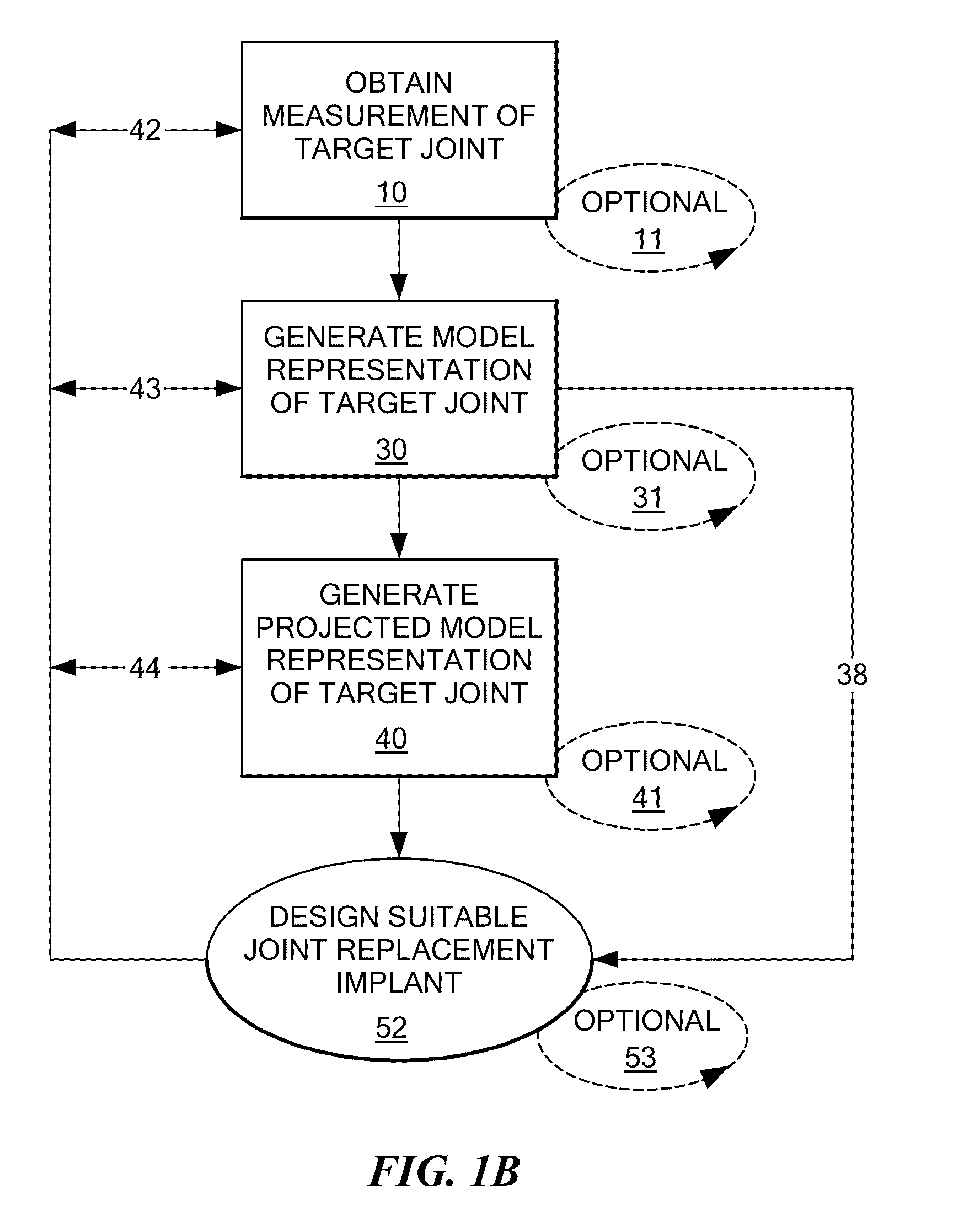
This invention is directed to orthopedic implants and systems. The invention also relates to methods of implant design, manufacture, modeling and implantation as well as to surgical tools and kits used therewith. The implants are designed by analyzing the articular surface to be corrected and creating a device with an anatomic or near anatomic fit; or selecting a pre-designed implant having characteristics that give the implant the best fit to the existing defect.
Owner:CONFORMIS
Minimally Invasive Joint Implant with 3-Dimensional Geometry Matching the Articular Surfaces
InactiveUS20110066245A1Facilitating the integration of a wide variety of cartilageIncrease successFinger jointsWrist jointsArticular surfacesArticular surface
This invention is directed to orthopedic implants and systems. The invention also relates to methods of implant design, manufacture, modeling and implantation as well as to surgical tools and kits used therewith. The implants are designed by analyzing the articular surface to be corrected and creating a device with an anatomic or near anatomic fit; or selecting a pre-designed implant having characteristics that give the implant the best fit to the existing defect.
Owner:CONFORMIS
Diamond-surfaced cup for use in a prosthetic joint
InactiveUS6488715B1Improve wear resistanceReduce coefficient of frictionFinger jointsWrist jointsArticular surfacesSacroiliac joint
Prosthetic joints, components for prosthetic joints, superhard bearing and articulation surfaces, diamond bearing and articulation surfaces, substrate surface topographical features, materials for making joints, bearing and articulation surfaces, and methods for manufacturing and finishing the same, and related information are disclosed, including a diamond-surfaced cup for use in a prosthetic joint.
Owner:DIAMICRON
Custom radiographically designed cutting guides and instruments for use in total ankle replacement surgery
ActiveUS8337503B2High precisionSimplify operating proceduresWrist jointsAnkle jointsTibiaSacroiliac joint
A system comprised of custom radiographically designed tibial and talar cutting guides, a tibial reaming guide and bit, and instrumentalities for use in total ankle replacement surgery and a computer-based system and method for making the custom radiographically designed tibial and talar cutting guides.
Owner:LIAN GEORGE JOHN
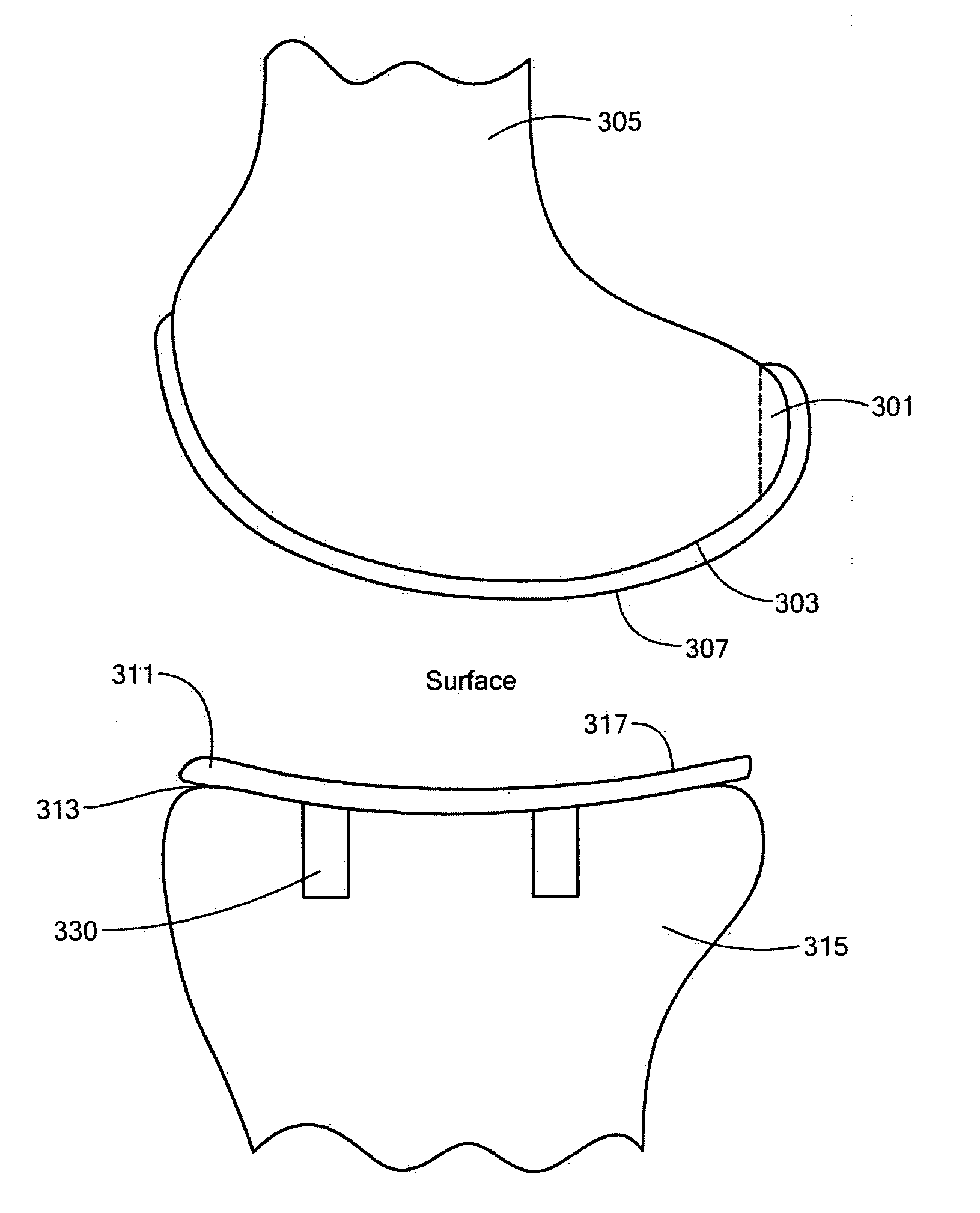
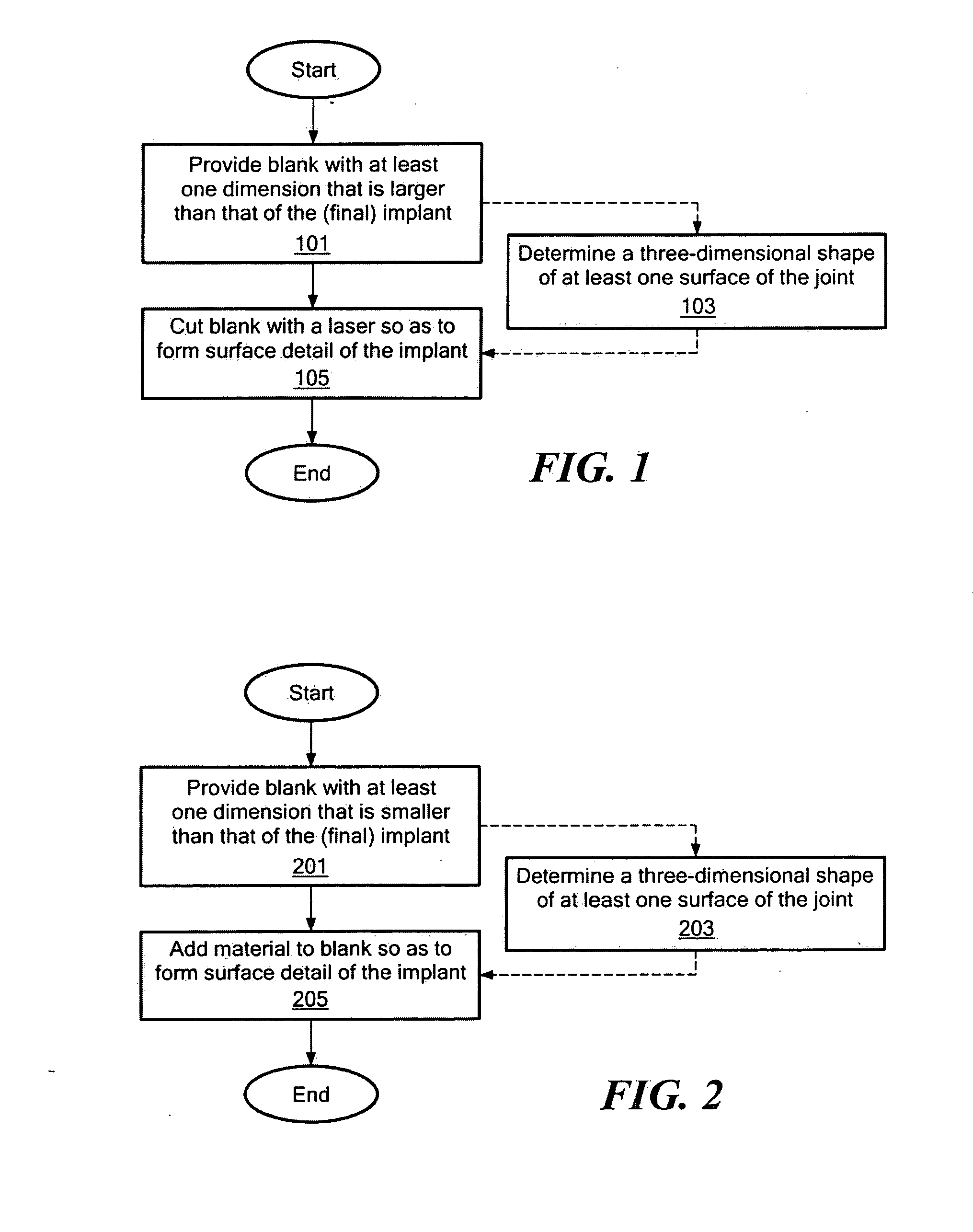
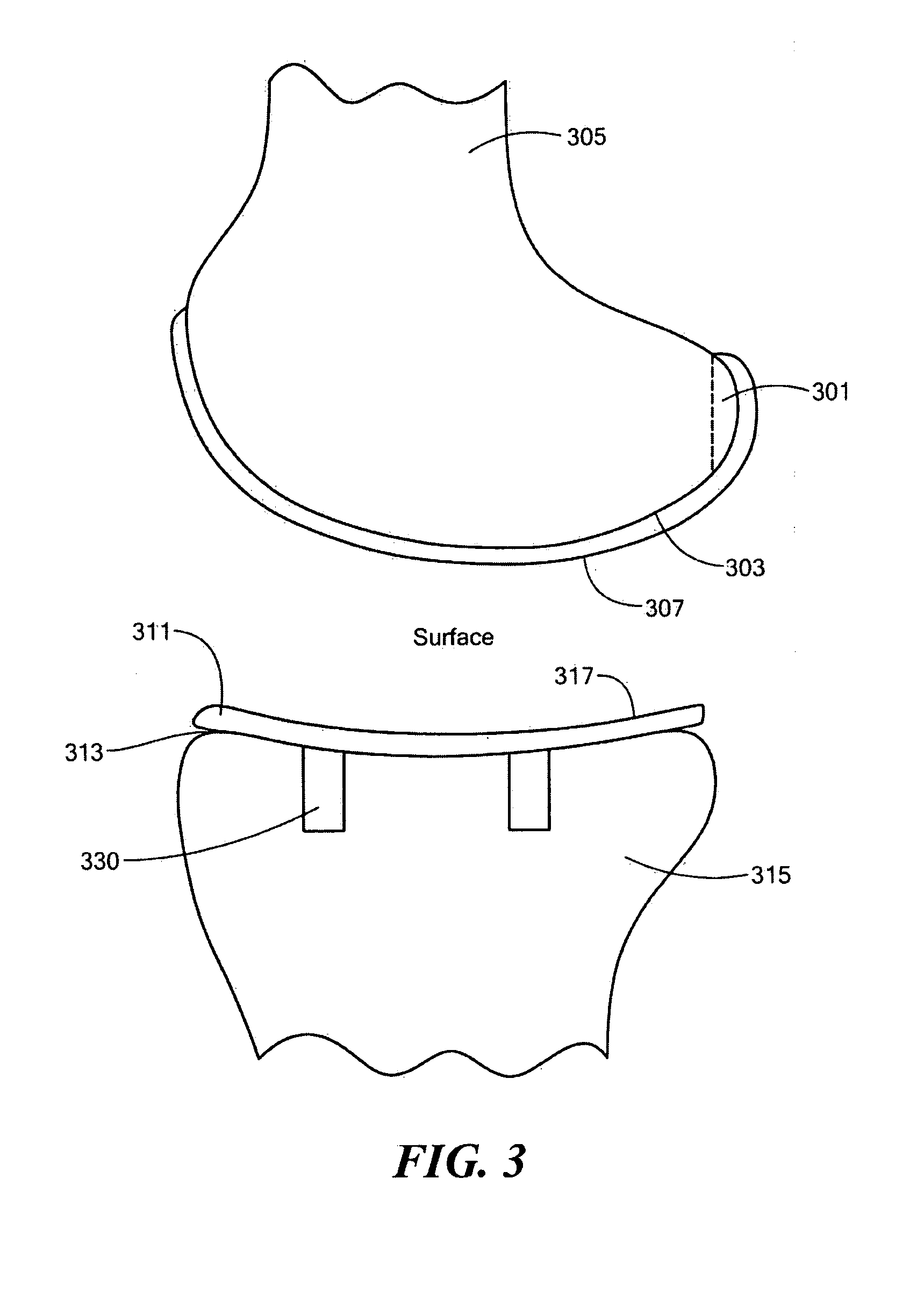
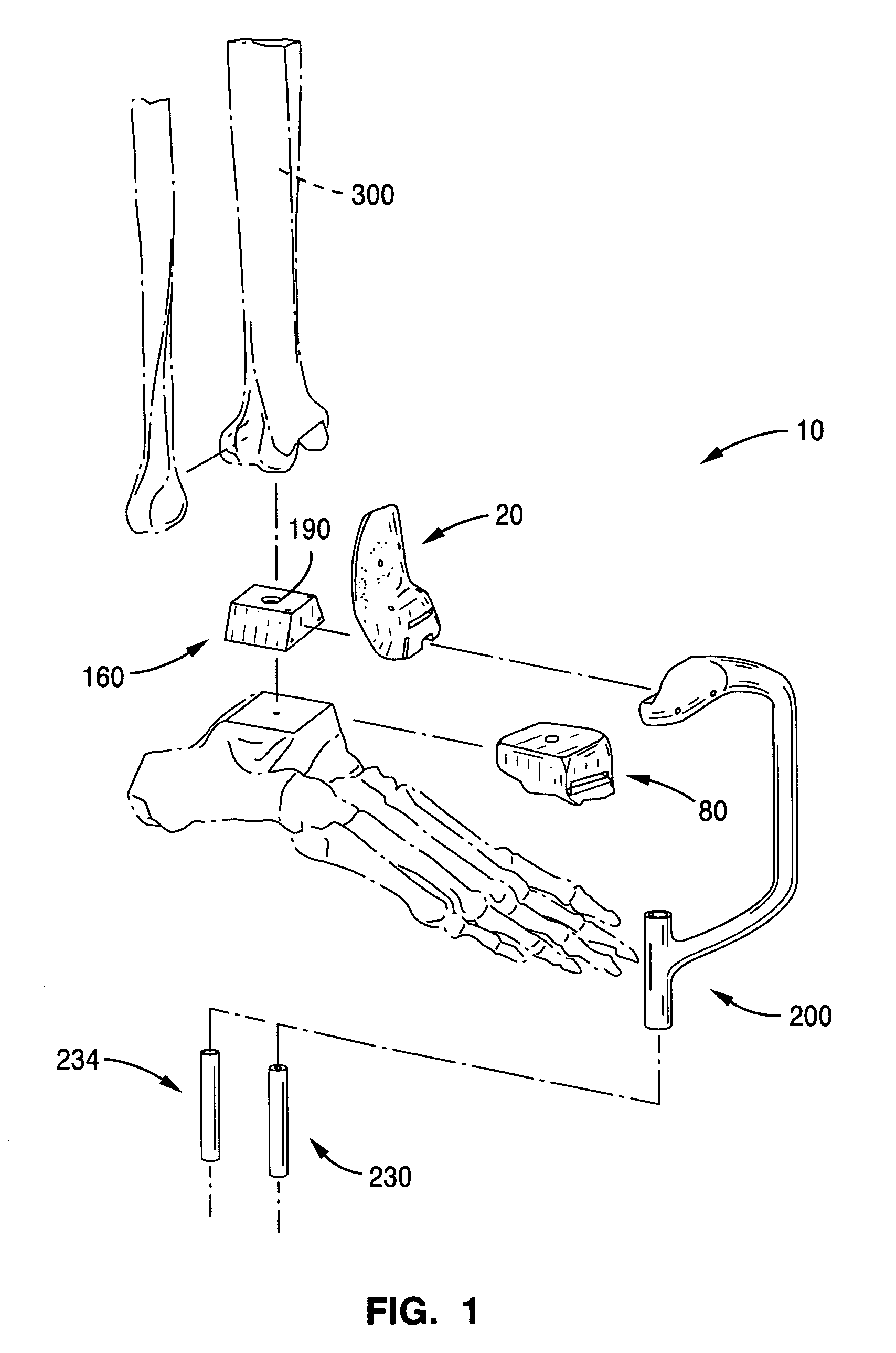
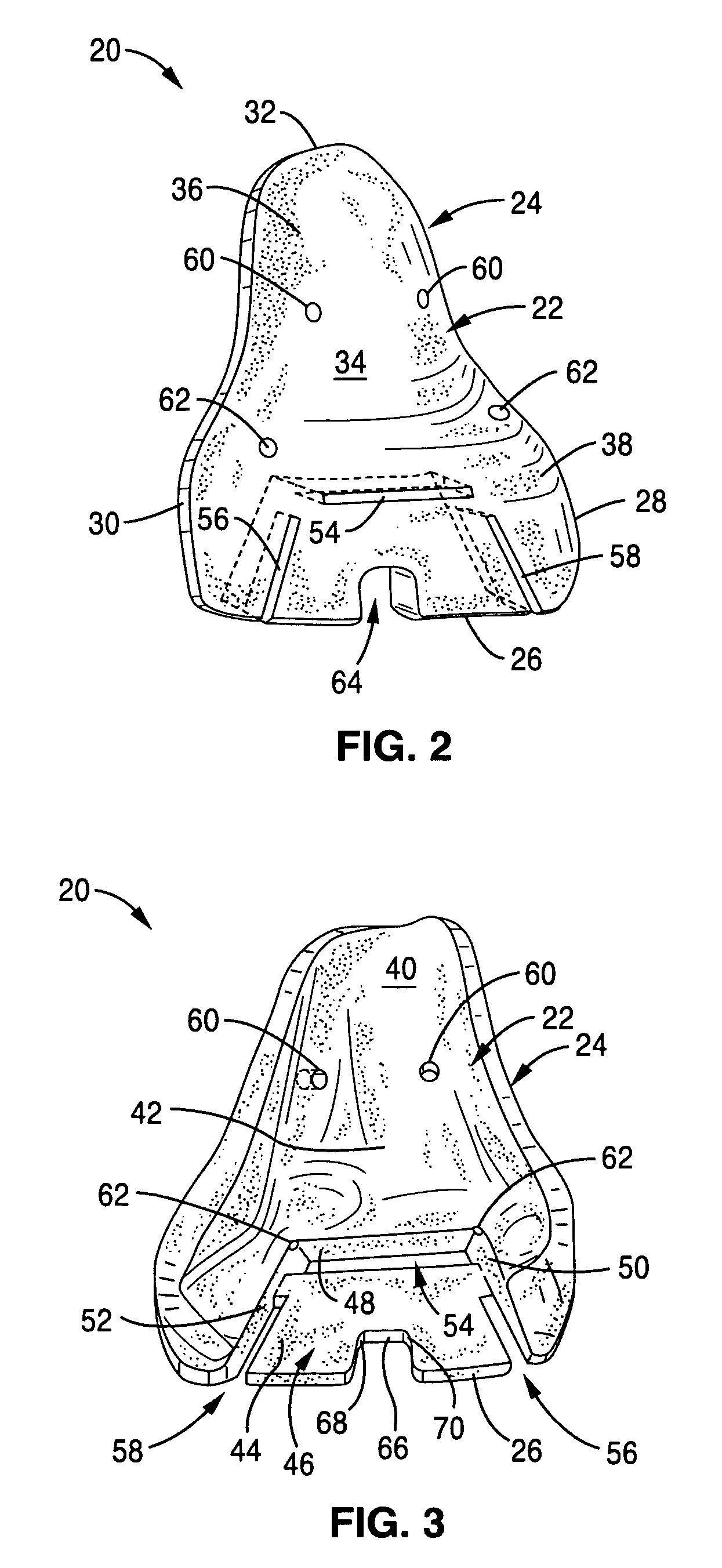
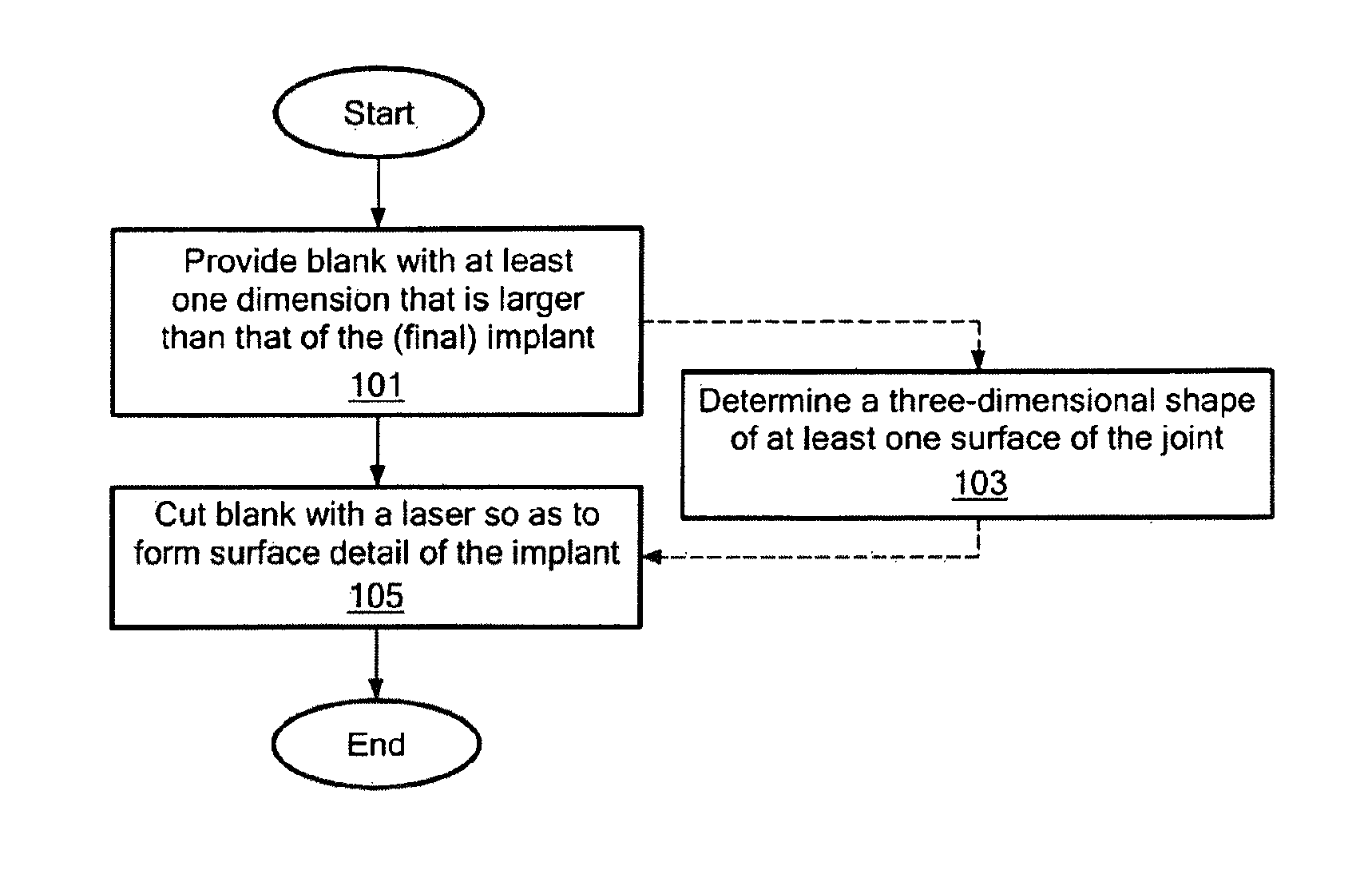
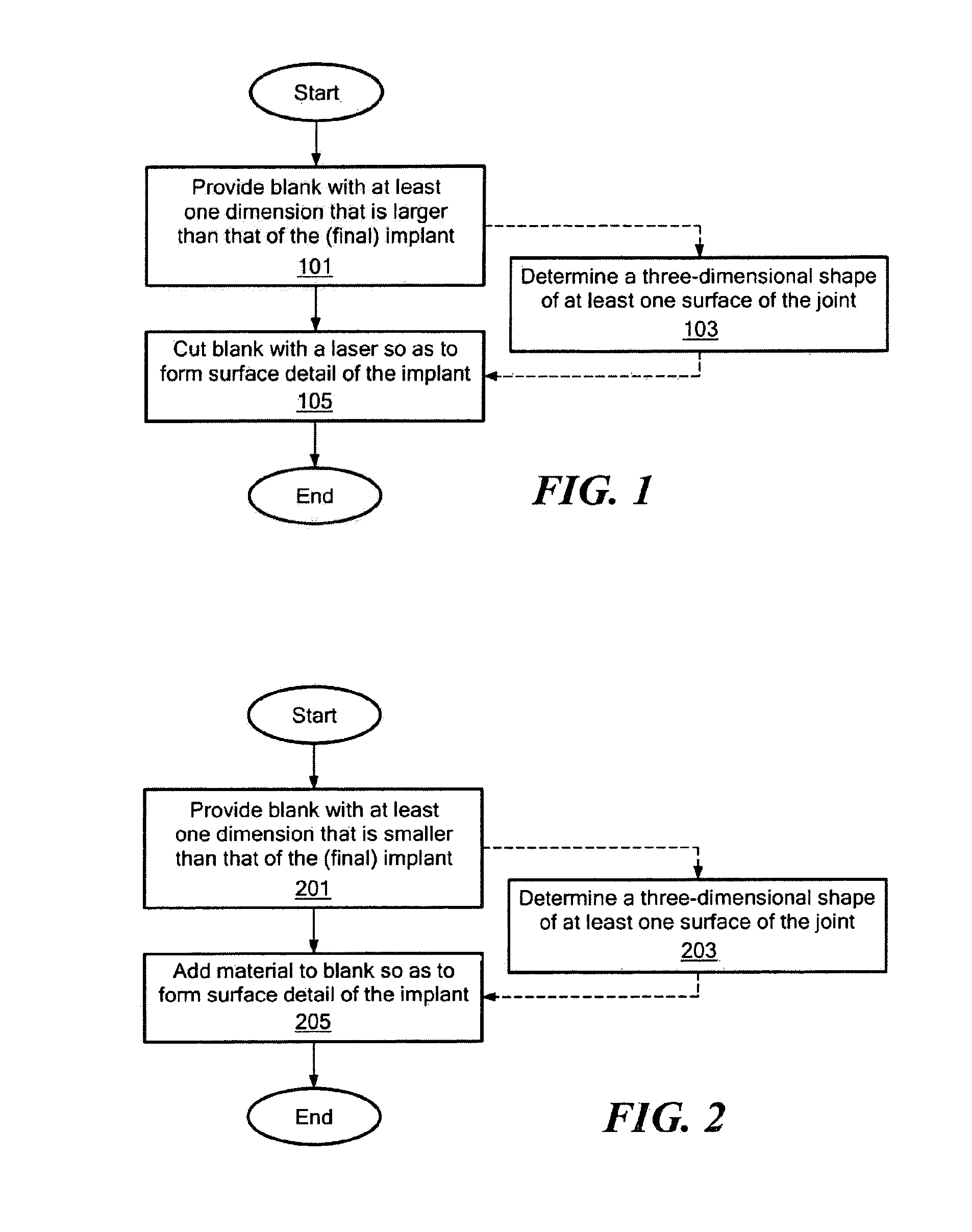
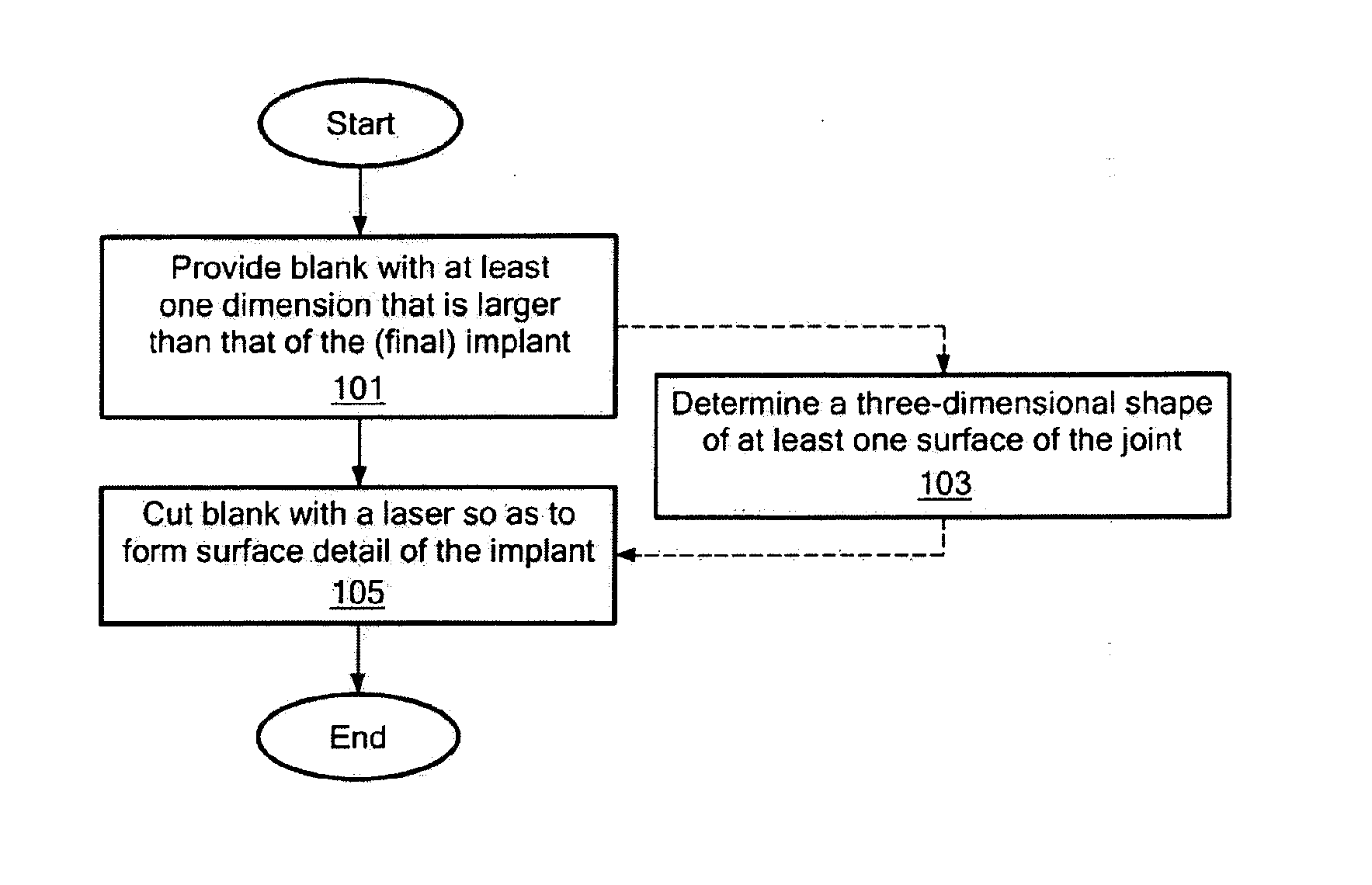
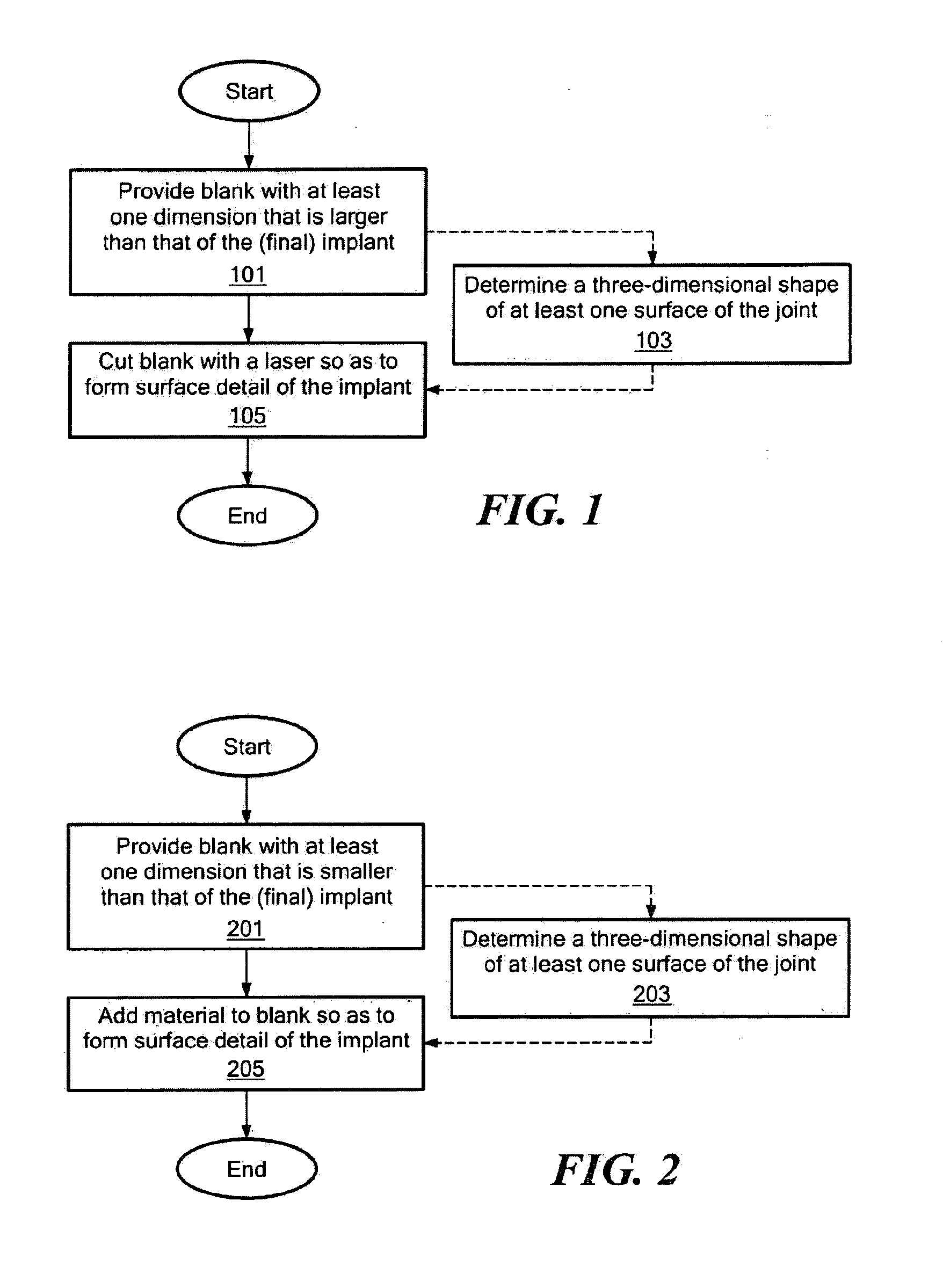
Implant device and method for manufacture
Disclosed are systems, devices and methods for optimizing the manufacture and / or production of patient-specific orthopedic implants. The methods include obtaining image data of a patient, selecting a blank implant to be optimized for the patient, and modifying the blank implant utilizing techniques disclosed herein to alter specific features of the implant to conform to the patient's anatomy.
Owner:CONFORMIS
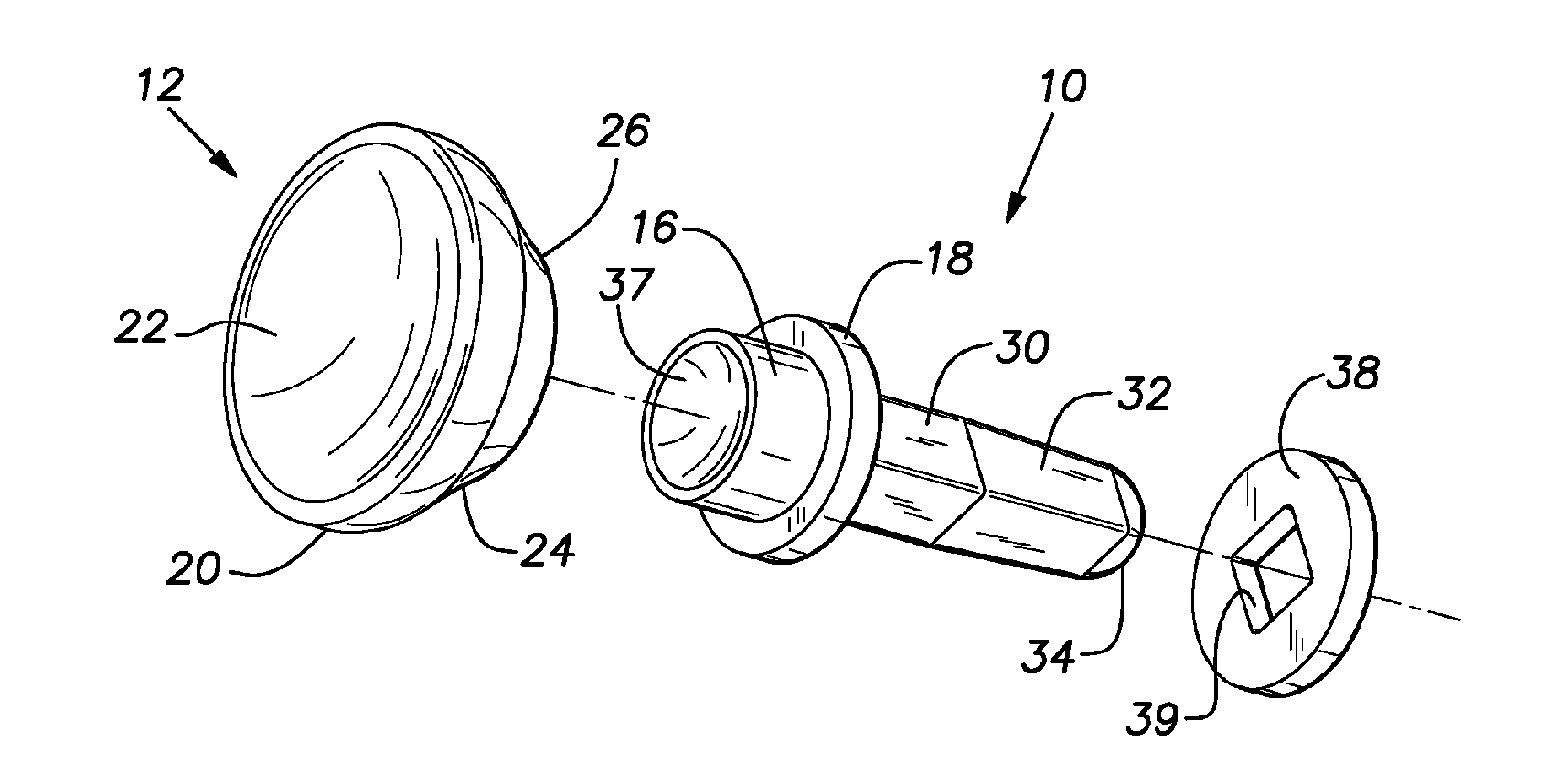
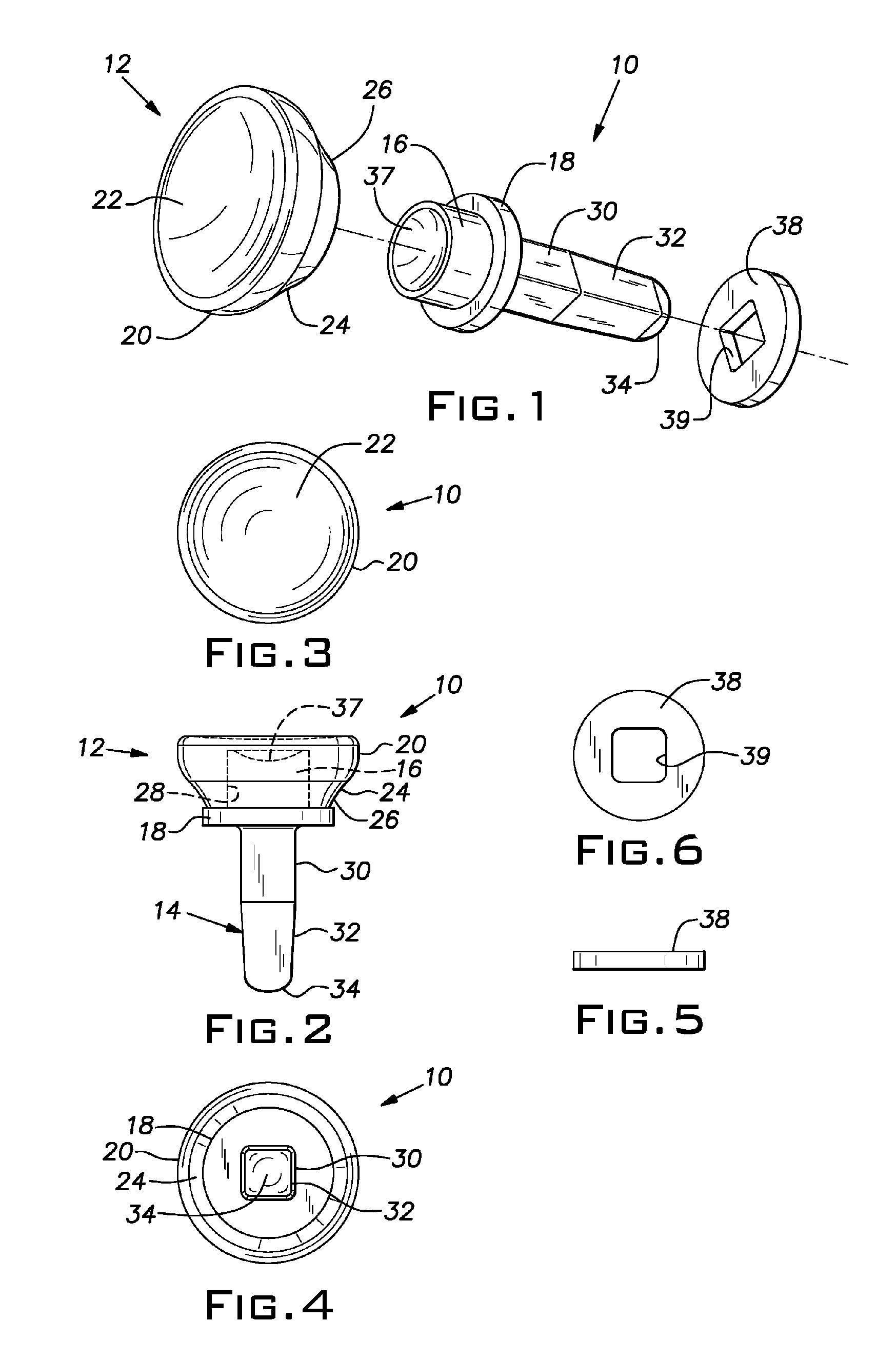
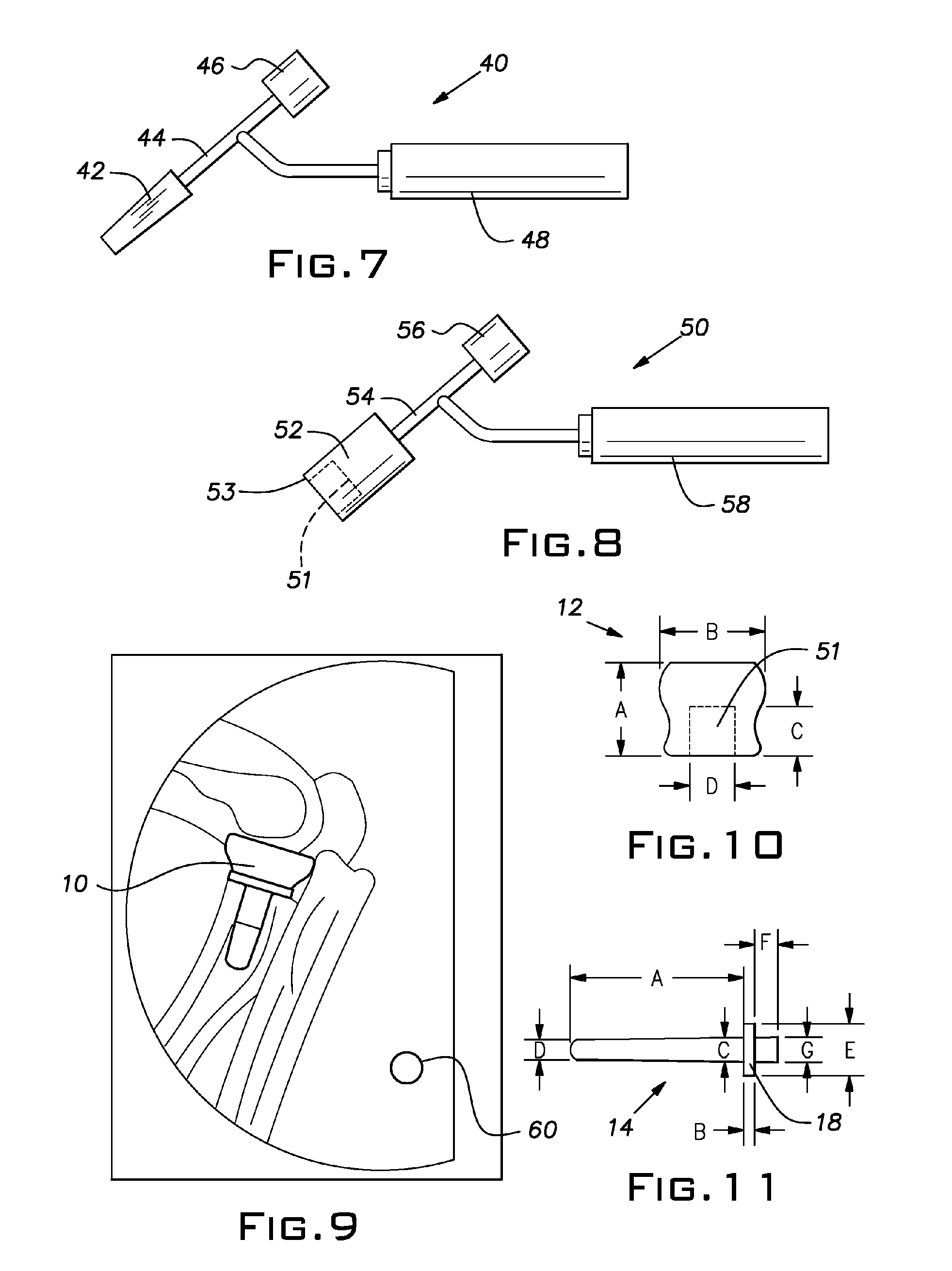
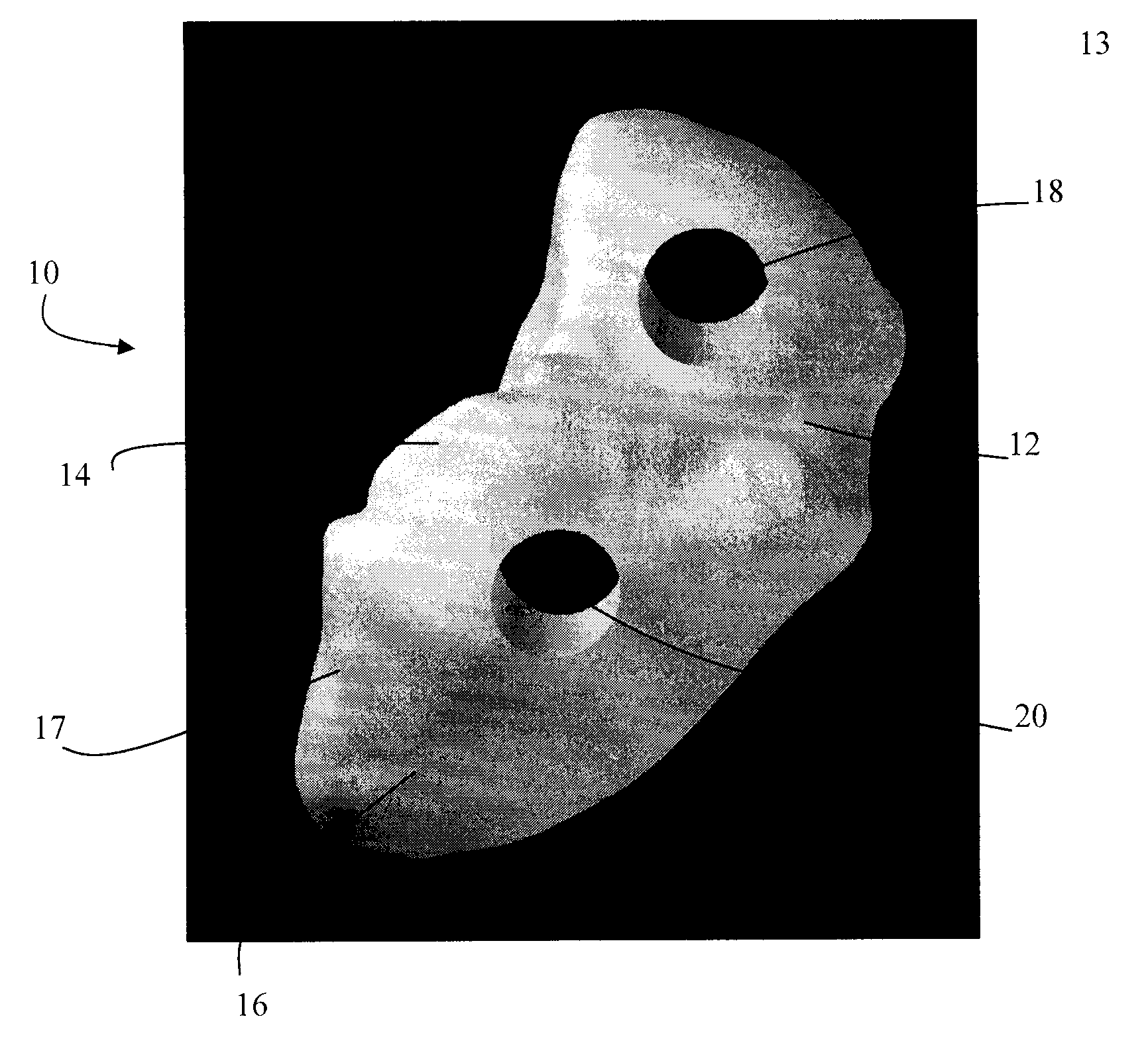
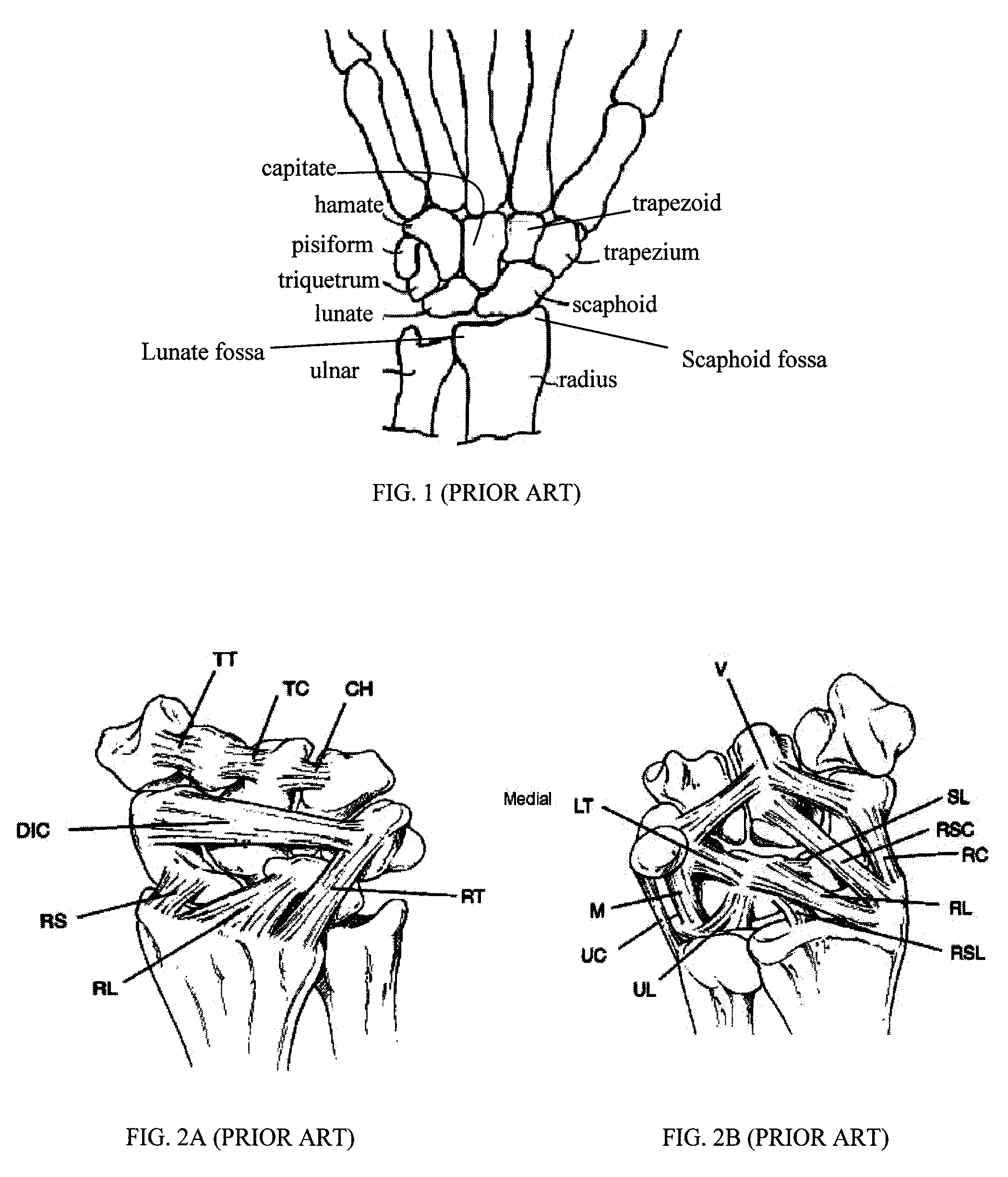
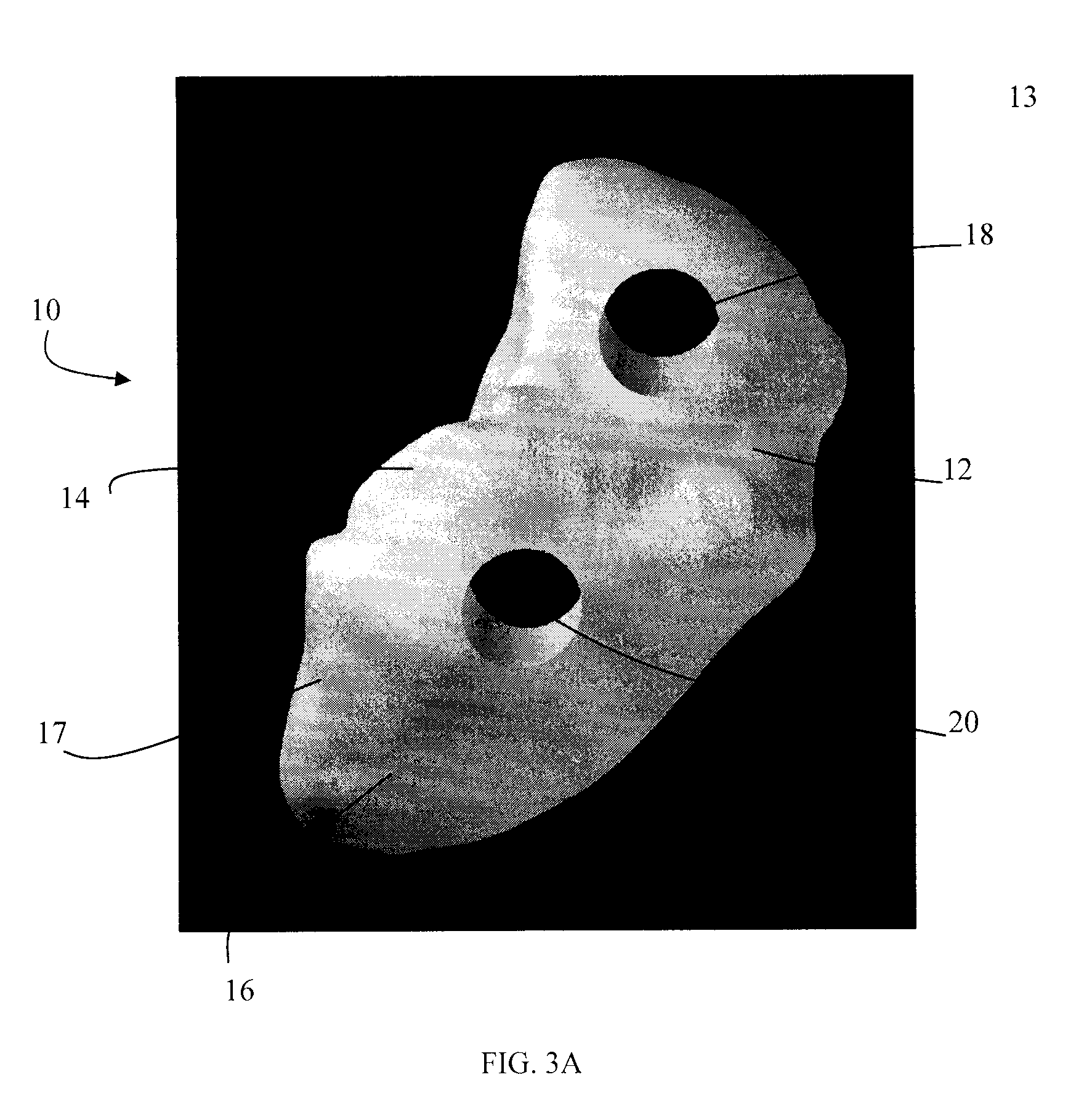
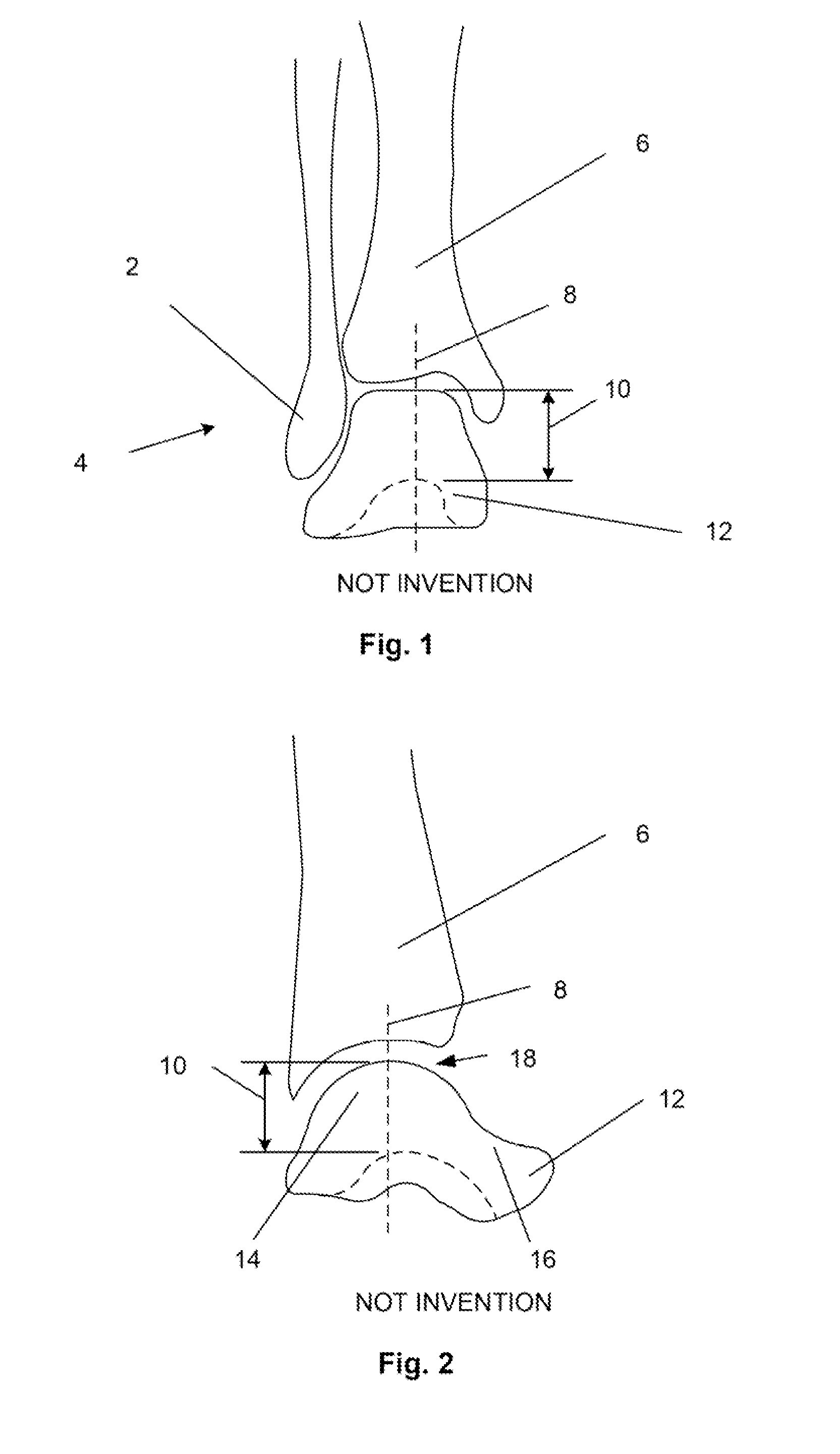
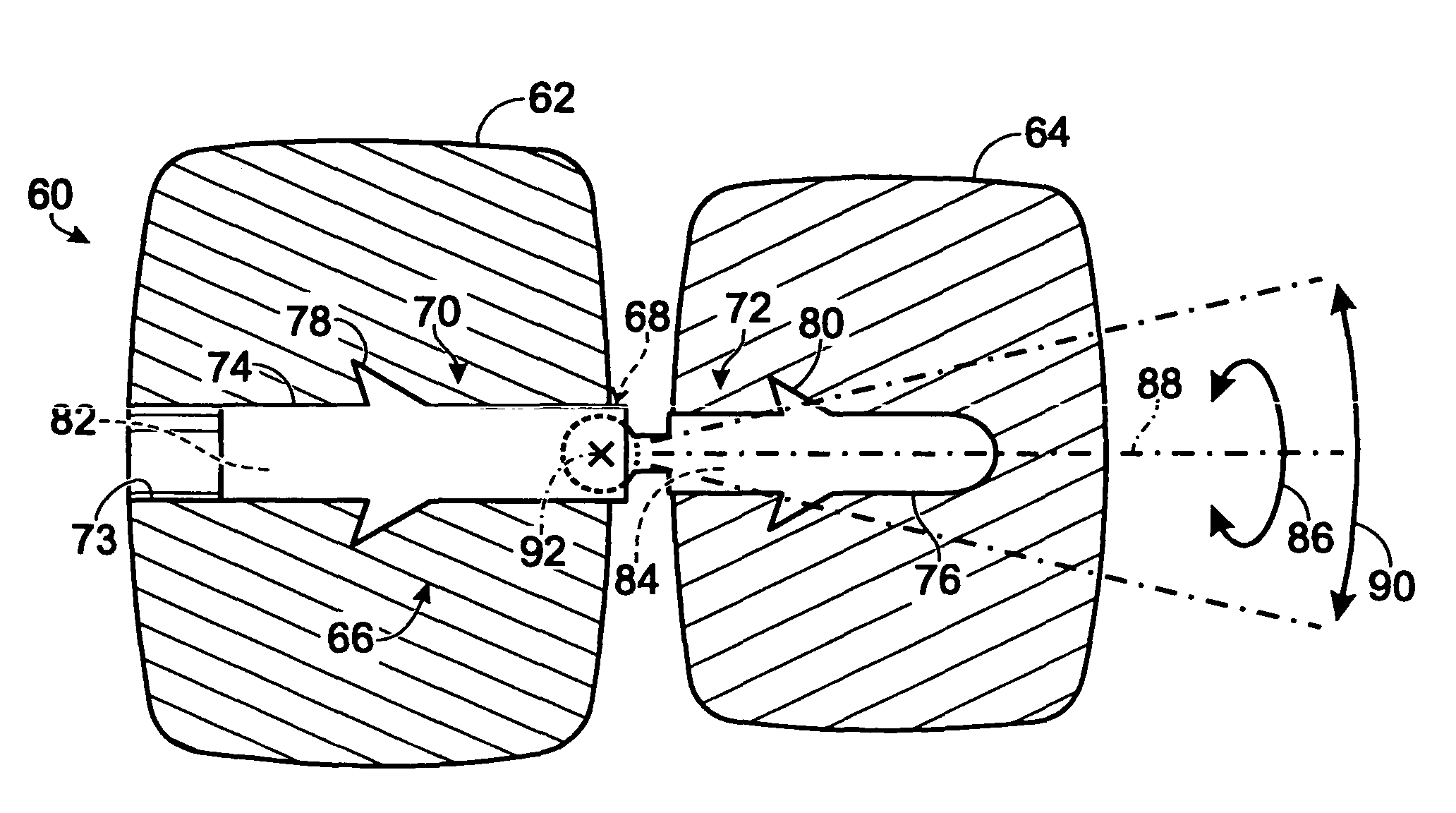
Small joint orthopedic implants and their manufacture
ActiveUS20060052725A1Simple processLarge inventoryFinger jointsWrist jointsBone CortexCancellous bone
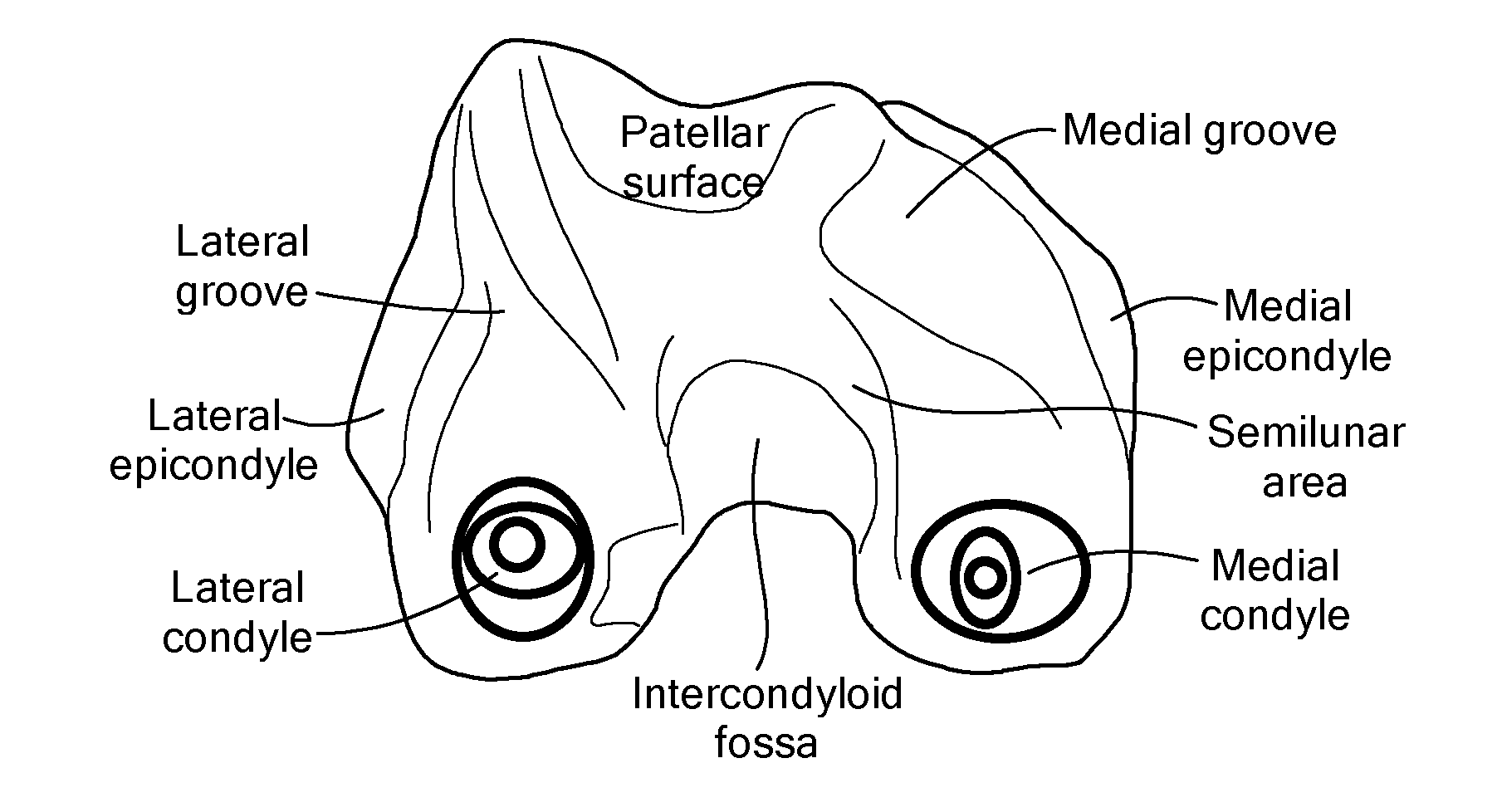
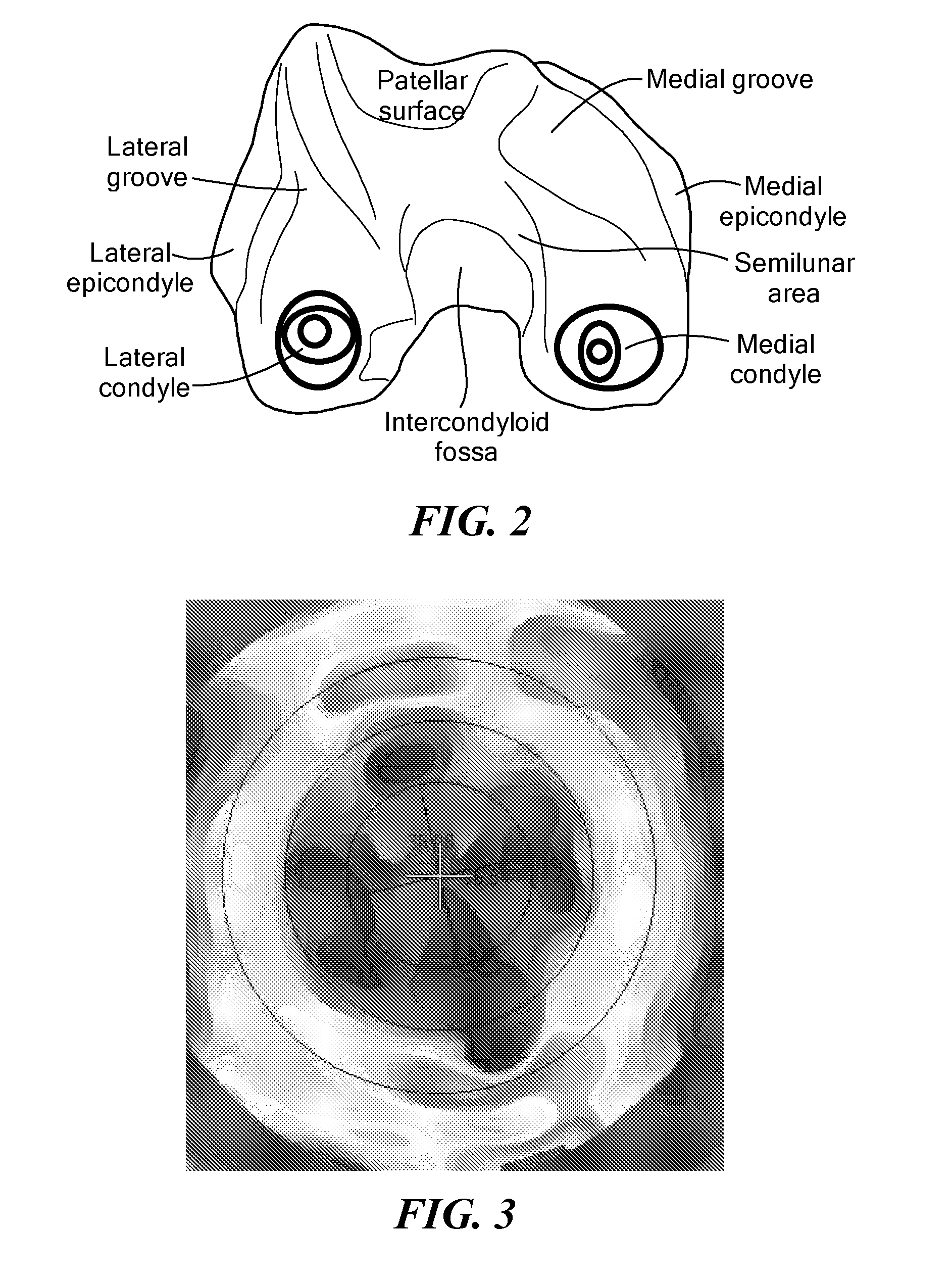
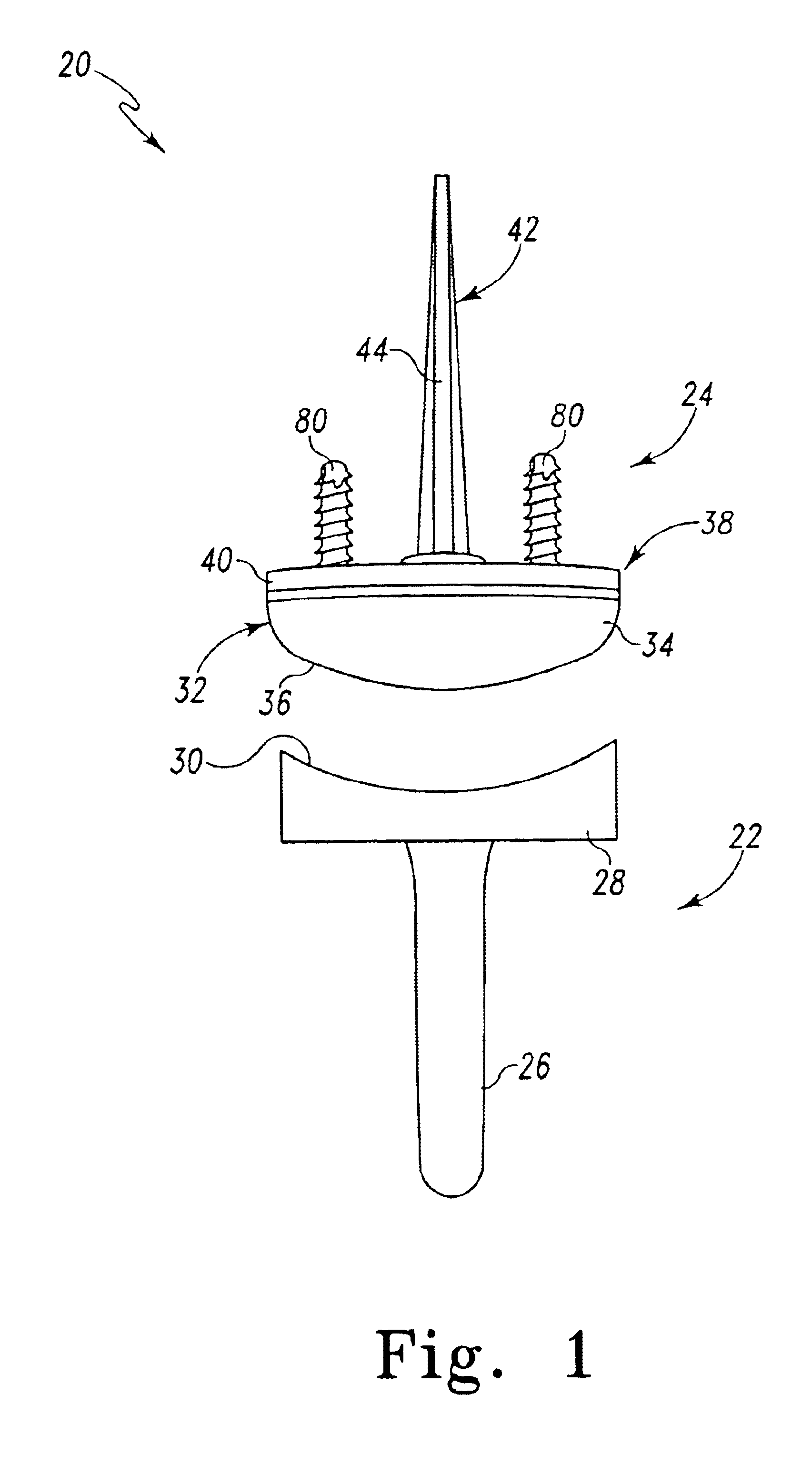
A technique to manufacture small joint orthopedic implants includes the steps of taking standard radiographs of a pathologic joint and the corresponding non-pathologic joint. In order to provide an accurate frame of reference, a specialized marker is placed in the radiographic field. By inspection of the radiographs and by comparison with the marker, the dimensions of the cortical bone and the cancellous bone can be quickly and accurately determined. These dimensions can be used to manufacture a suitable implant and installation tool. Typically, the implant will include a stem from which a post projects. A radially extending collar is located at the intersection between the stem and the post. A mating head is attached to the post. The head closely approximates the size and shape of the natural head being replaced. The stem will be non-round in cross-section to prevent rotation of the stem in the bone. For many applications, the head will not be fixedly attached to the post, but will be rotatable about the longitudinal axis of the post. One or more spacers that fit about the stem also can be provided in order to adjust the distance that the head projects from the bone.
Owner:SEITZ JR WILLIAM H +1
Orthopaedic implants
InactiveUS20110004317A1Reduce difficultyReduce disadvantagesAdditive manufacturing apparatusWrist jointsPlastic surgerySurgical department
A method for making an orthopaedic implant, the method comprising: characterizing at least a portion of a bone corresponding to the bone to be replaced, said corresponding bone being on the contralateral side of the patient; providing a model of the orthopaedic implant based on a mirror image of the contralateral bone; and forming the orthopaedic implant based on the model.
Owner:MCGILL UNIV
Implant for treating ailments of a joint or a bone
InactiveUS6436146B1Increase coefficient of frictionImprove stabilityFinger jointsWrist jointsDiseasePyrolytic carbon
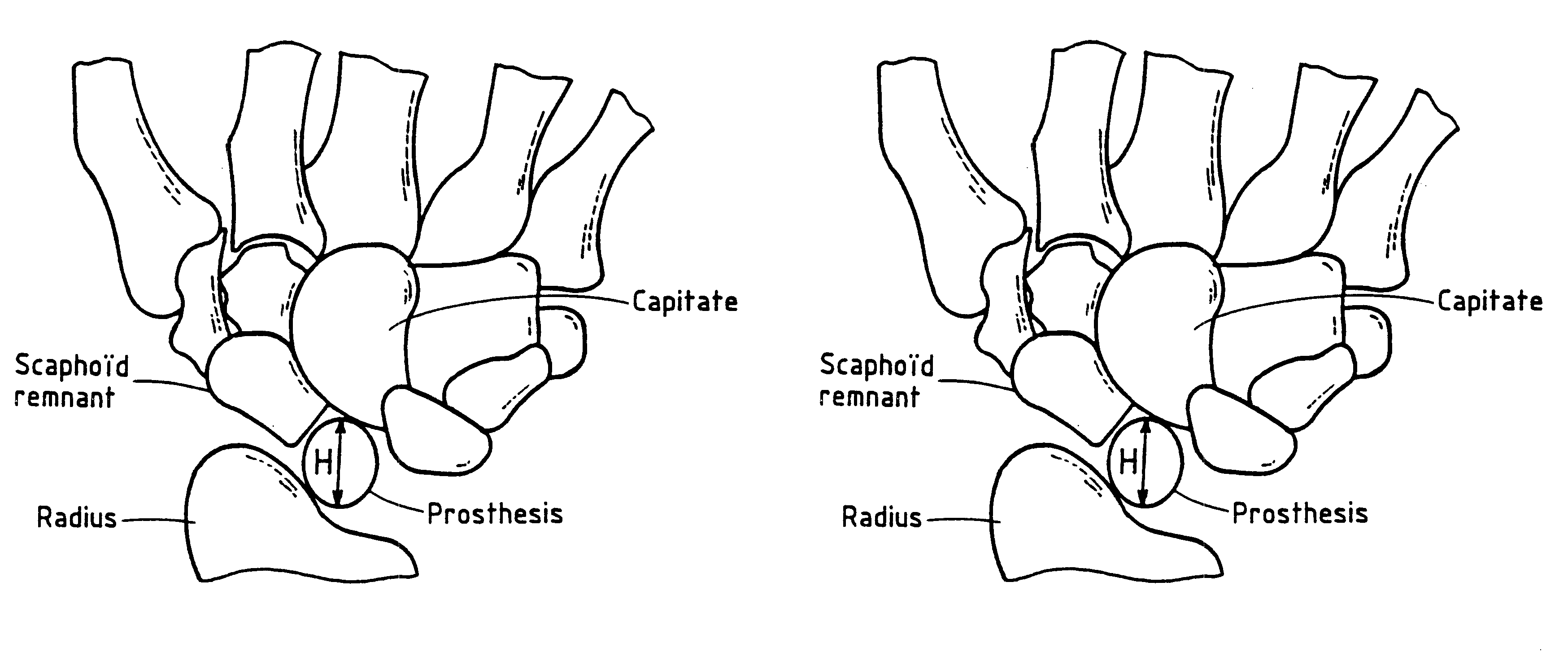
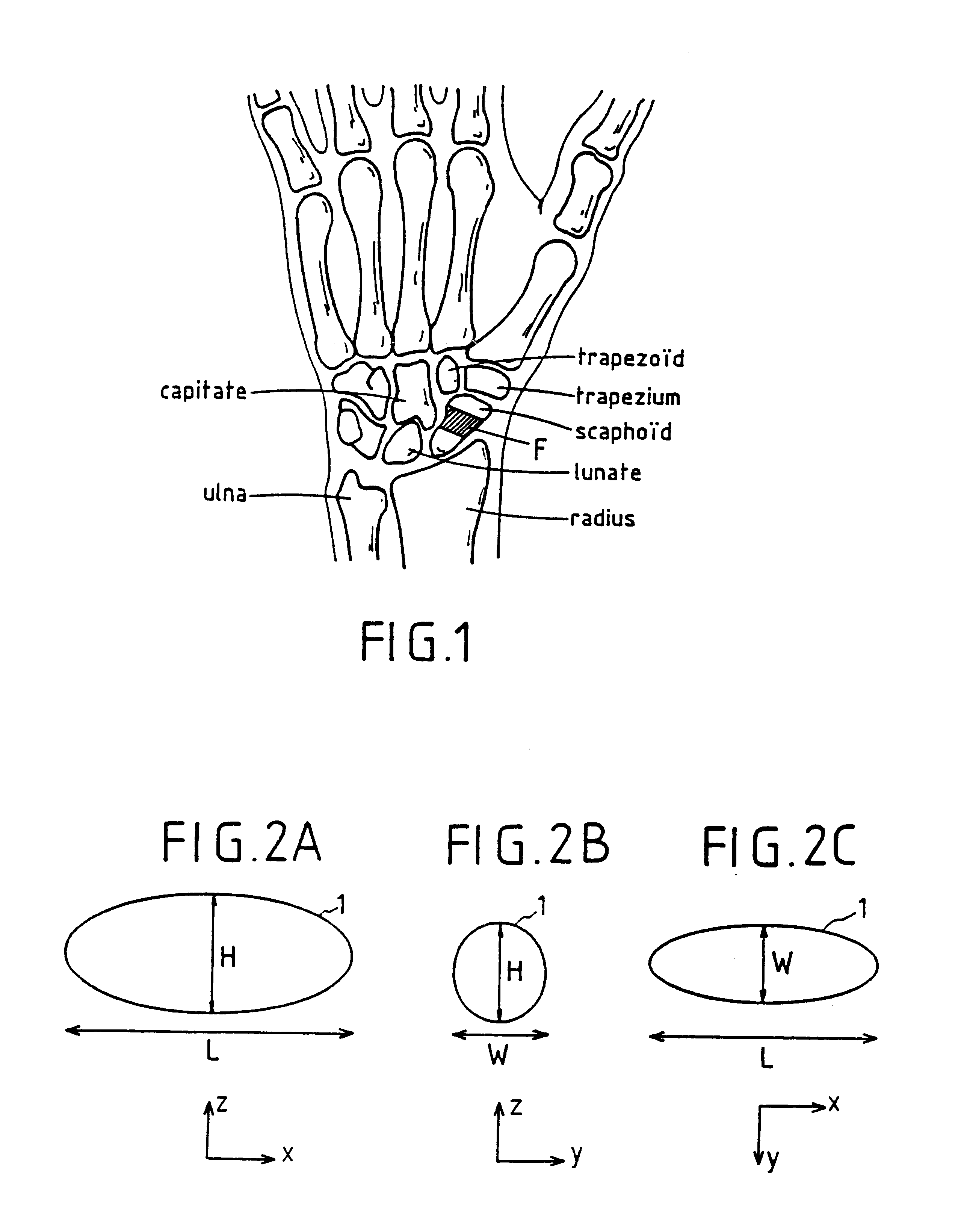
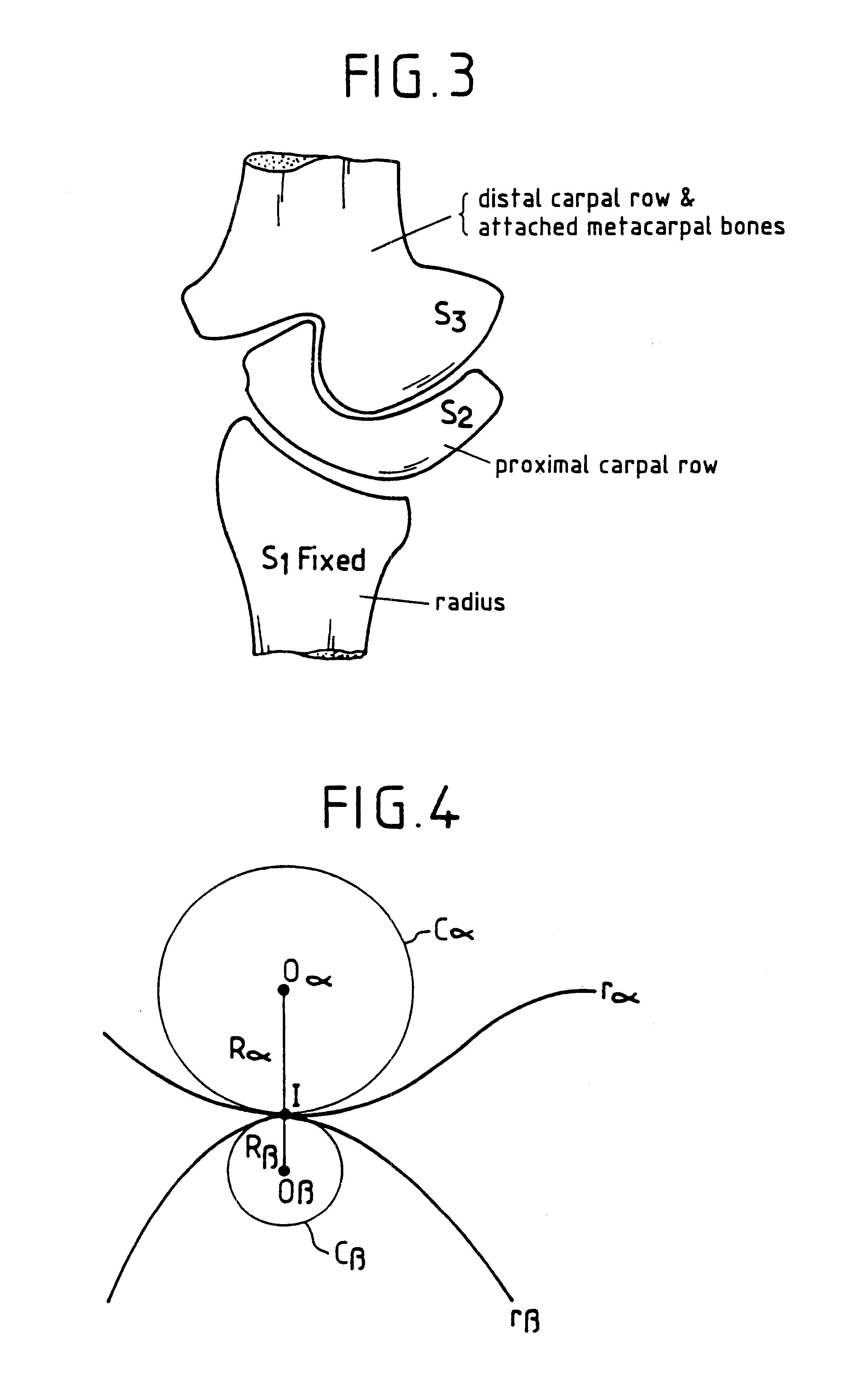
The implant has at least one contact surface portion, made of pyrolytic carbon, designed to be in mobile contact with at least one bony surface when the implant is implanted in a patient. Furthermore, the implant is free from any attaching means, so that it remains free with respect to the at least one bony surface when implanted in the patient.
Owner:TORNIER SA SAINT ISMIER
Methods and devices for deploying biological implants
InactiveUS20100318088A1Reduce decreasePrevent yaw and twist and rotationWrist jointsAnkle jointsPlastic surgeryAnkle
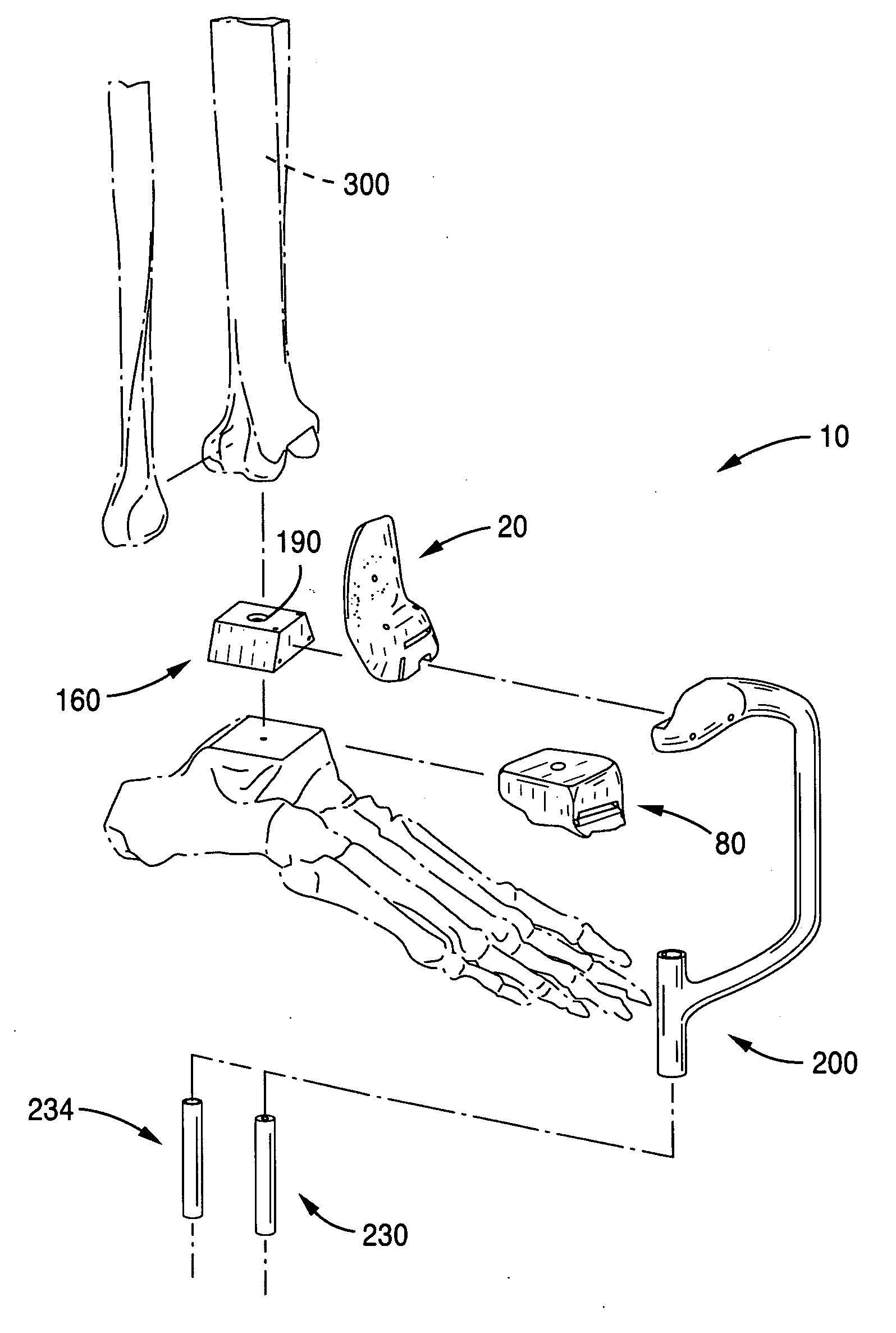
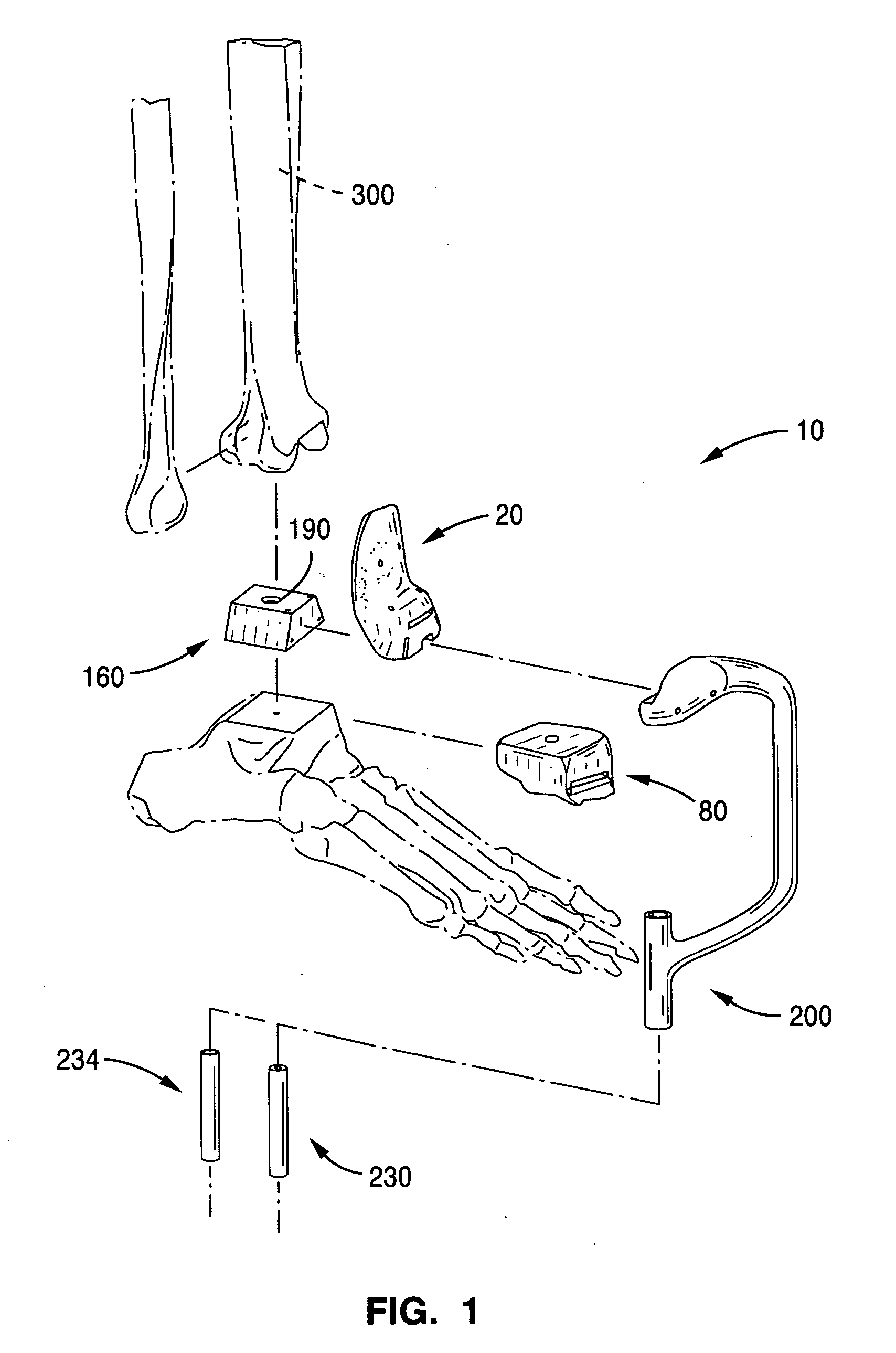
Methods and devices for deploying biological implants are disclosed. The biological implants can include orthopedic, multi-component ankle implants. The target site can be prepared by fixing a rigid, alignable guide or jig with saw holes to the bone(s). Saws configured to fit through the saw holes can then be inserted through the saw holes to cut the bone(s). The jig can then be removed. Slidable implants can be positioned. Implants needing to be forced into place can be attached to elongated members to gently hold the implant and to provide a non-implant surface on which to apply the force.
Owner:TALUS MEDICAL
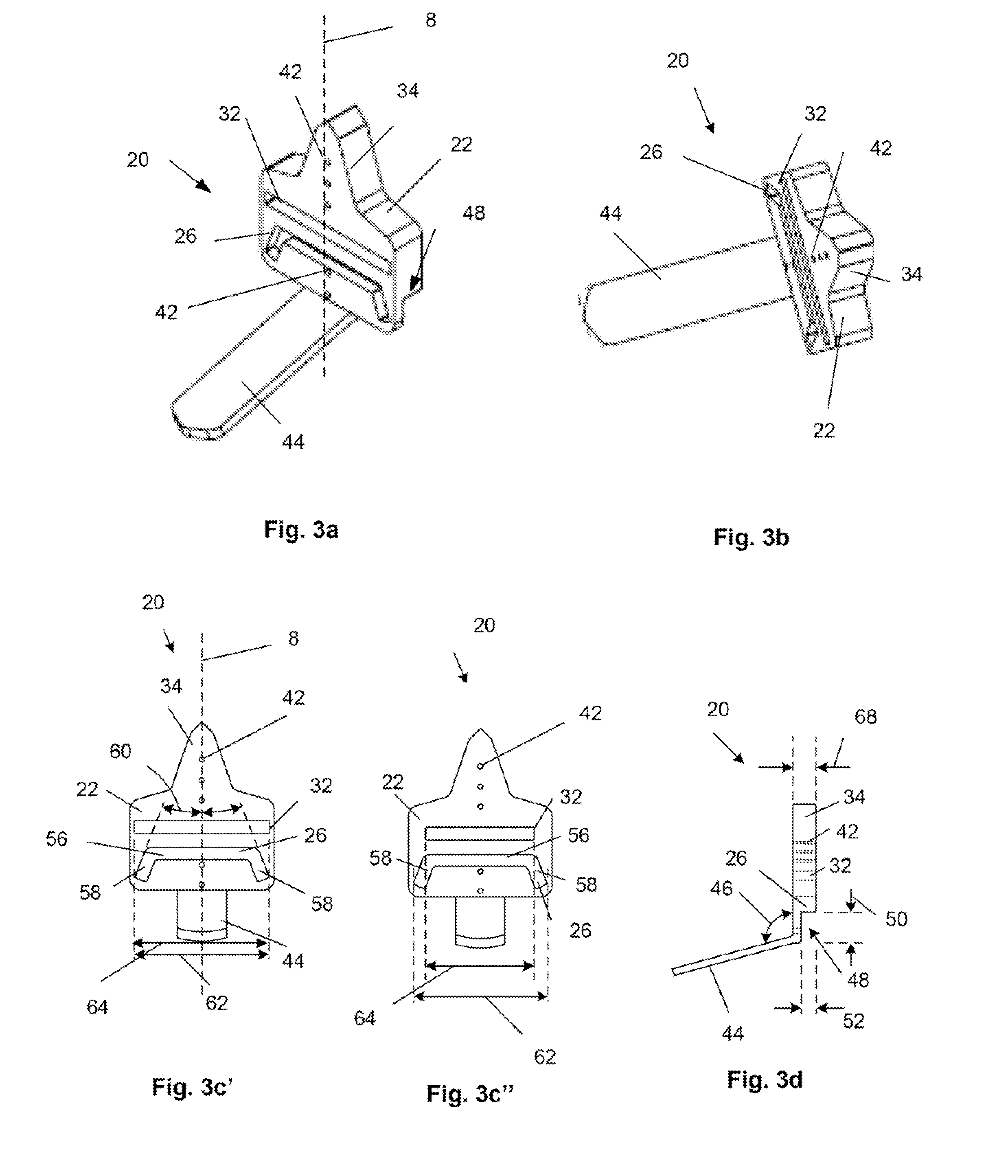
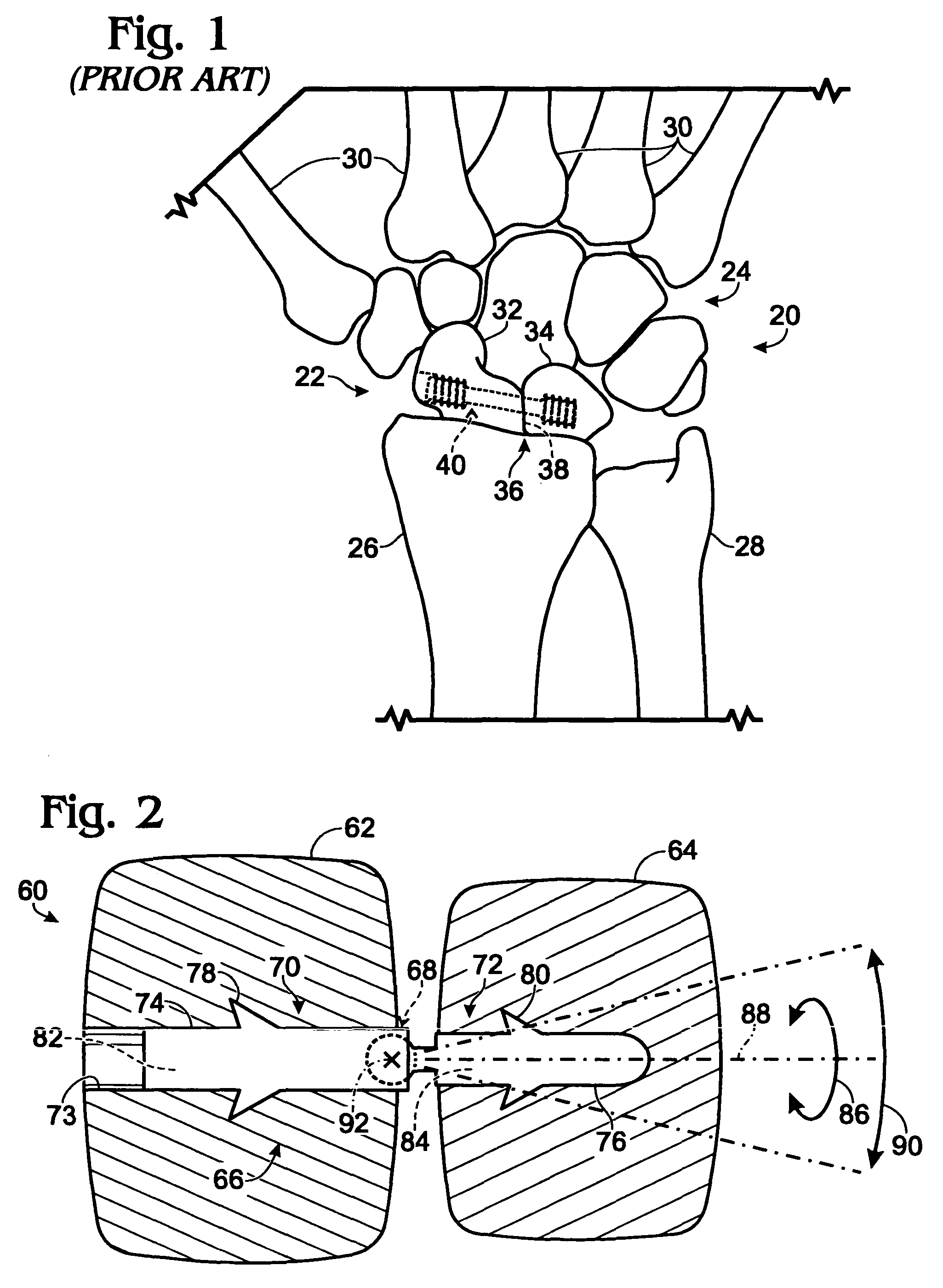
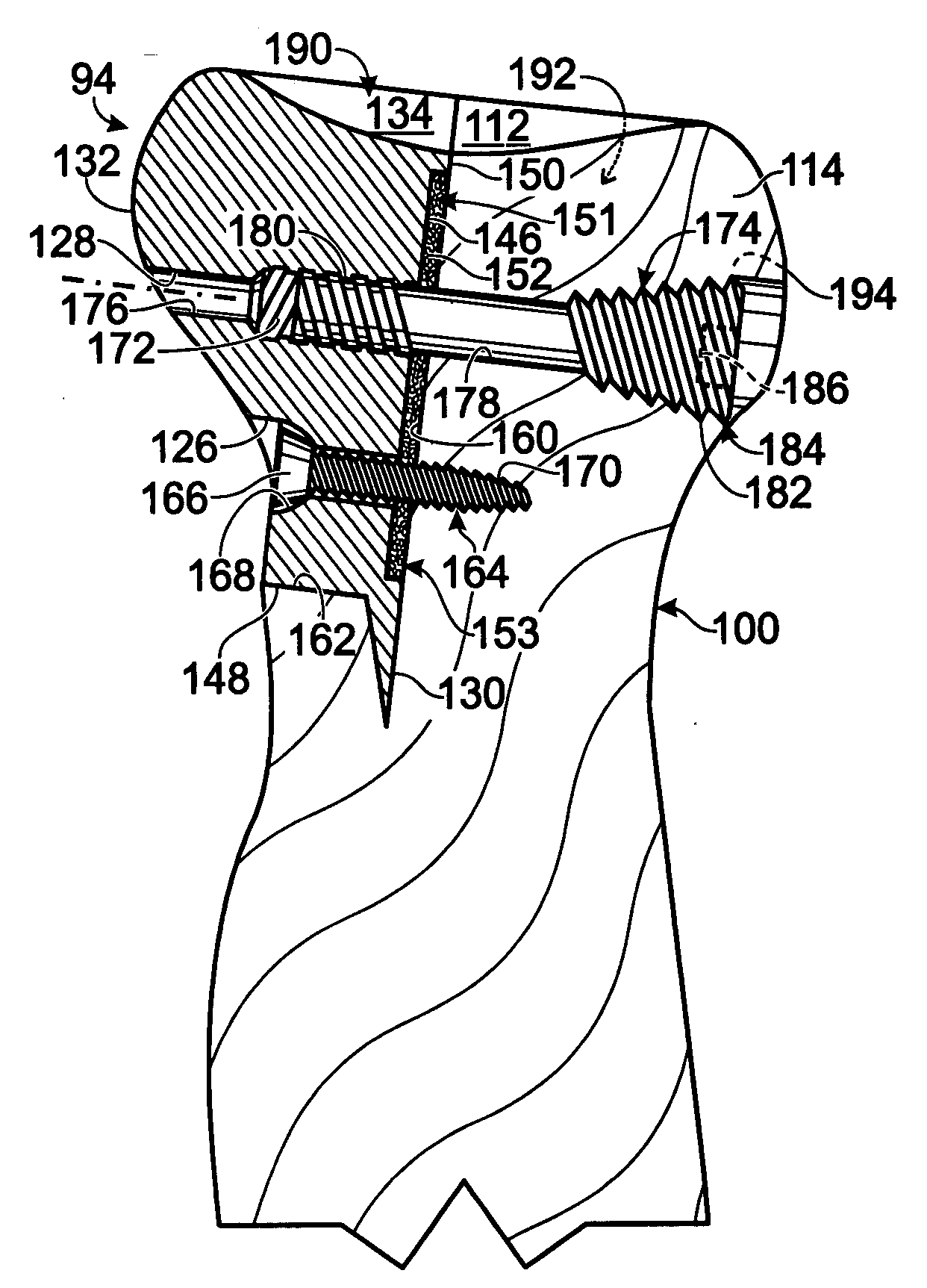
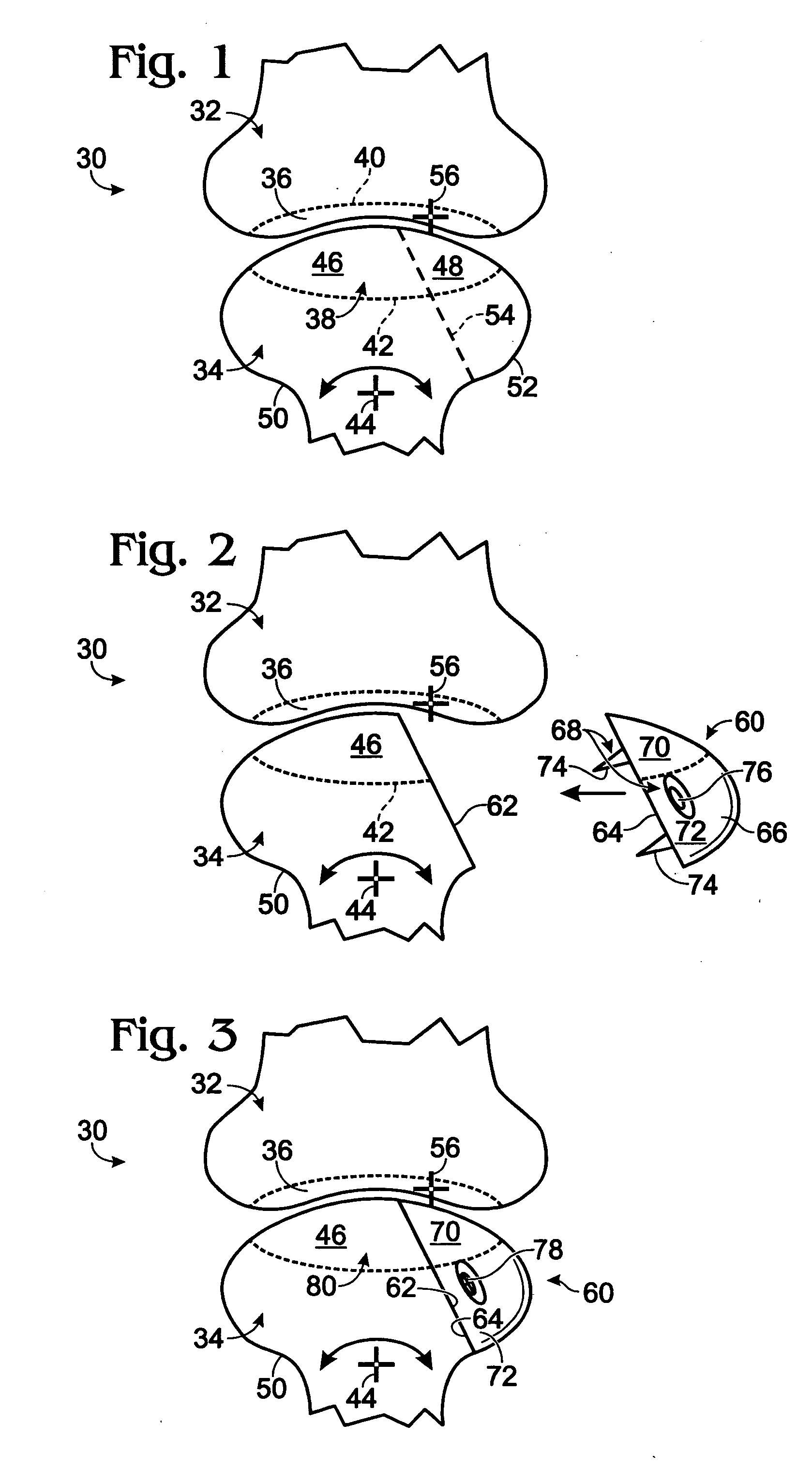
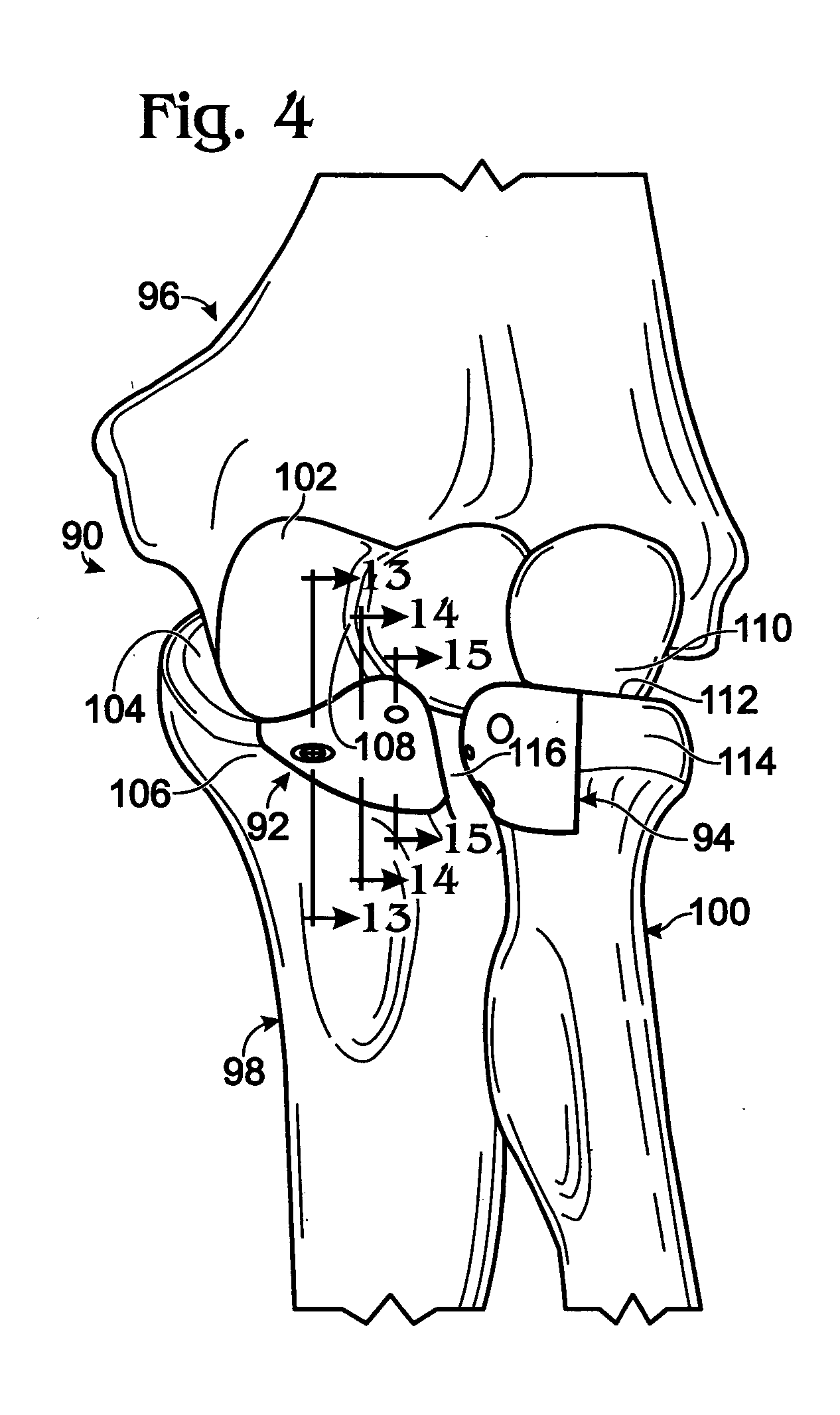
Bone connector with pivotable joint
System, including methods, apparatus, and kits, for connecting bones and / or bone portions using a bone connector with a pivotable ball and socket joint.
Owner:ACUMED
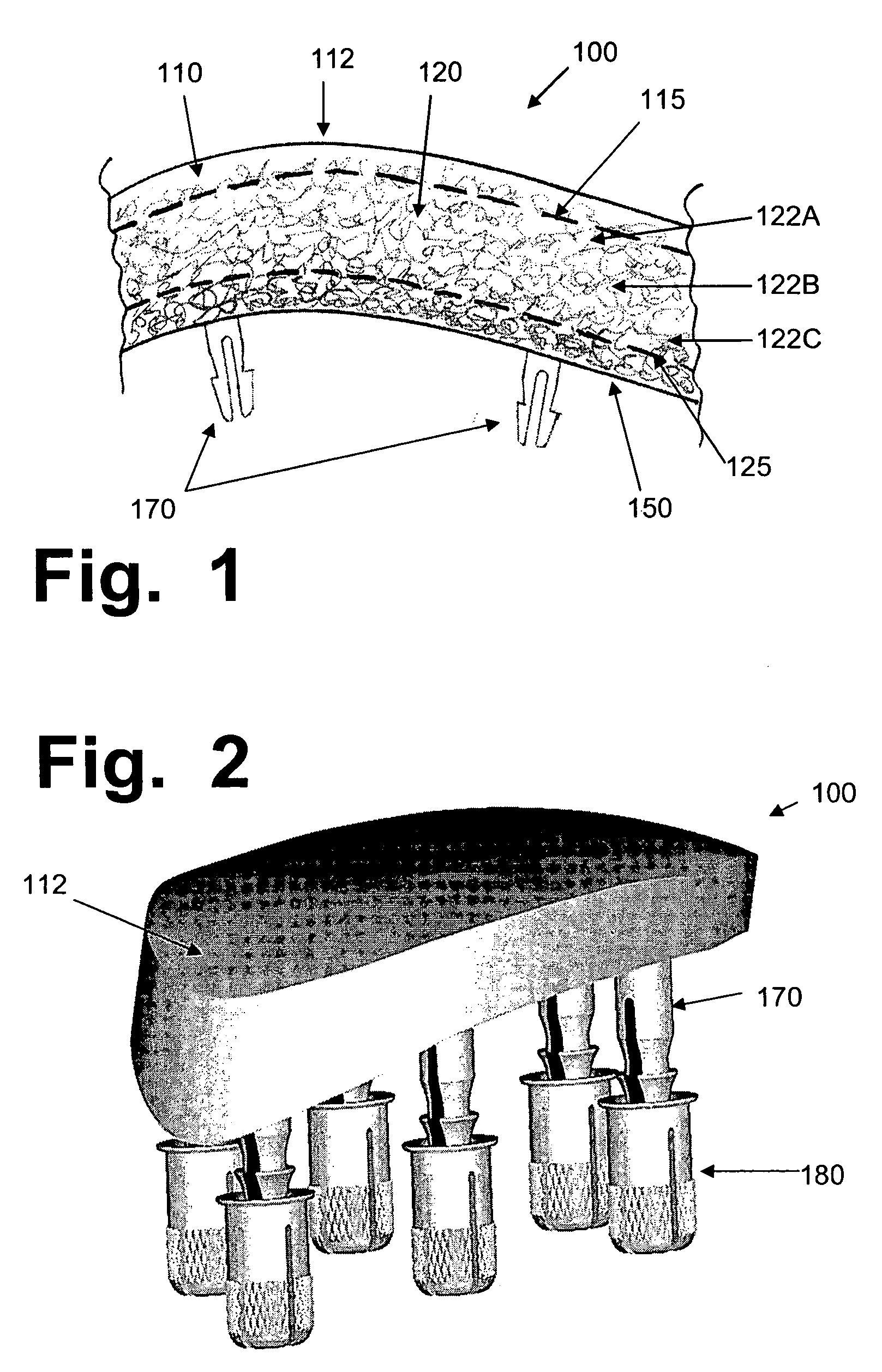
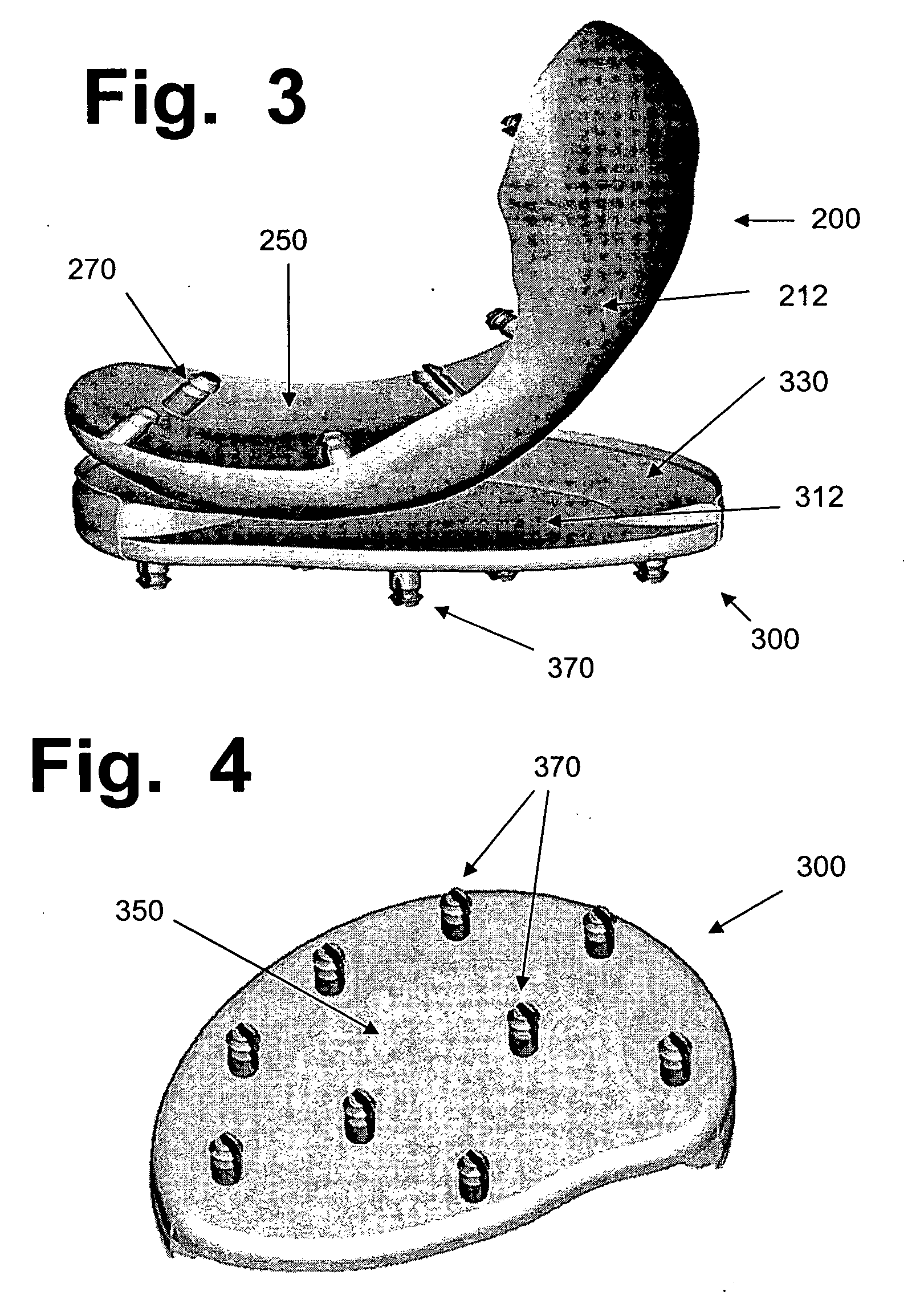
Hydrogel implants for replacing hyaline cartilage, with charged surfaces and improved anchoring
InactiveUS20050287187A1High strengthIncreased durabilityFinger jointsWrist jointsKnee JointVolumetric Mass Density
Hydrogel devices for surgical implantation to replace damaged cartilage in a mammalian joint (such as a knee, hip, shoulder, etc.) are disclosed, with one or more of the following enhancements: (1) articulating surfaces that have been given negative surface charge densities that emulate natural cartilage and that interact with positively charged components of synovial fluid; (2) anchoring systems with affixed pegs that will lock into accommodating receptacles, which will be anchored into hard bone before the implant is inserted into a joint; (3) a three-dimensional reinforcing mesh made of strong but flexible fibers, embedded within at least a portion of the hydrogel.
Owner:MANSMANN KEVIN A
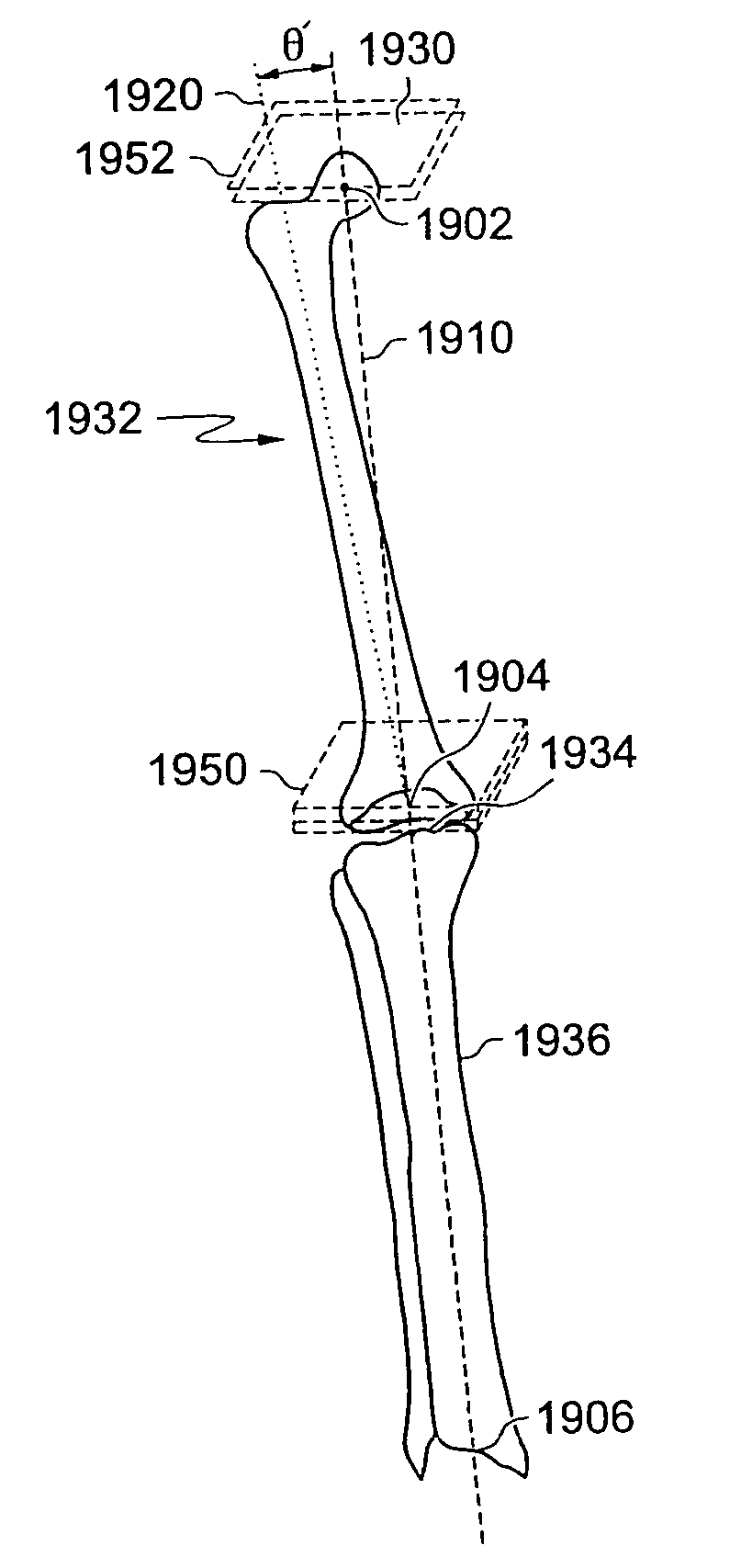
Methods for determining meniscal size and shape and for devising treatment
The present invention relates to methods for determining meniscal size and shape for use in designing therapies for the treatment of various joint diseases. The invention uses an image of a joint that is processed for analysis. Analysis can include, for example, generating a thickness map, a cartilage curve, or a point cloud. This information is used to determine the extent of the cartilage defect or damage and to design an appropriate therapy, including, for example, an implant. Adjustments to the designed therapy are made to account for the materials used.
Owner:CONFORMIS
Prosthetic joint having at least one superhard articulation surface
InactiveUS6398815B1Less disruptiveImprove overall utilizationFinger jointsWrist jointsArticular surfacesTarsal Joint
Prosthetic joints, components for prosthetic joints, superhard bearing and articulation surfaces, diamond bearing and articulation surfaces, substrate surface topographical features, materials for making joints, bearing and articulation surfaces, and methods for manufacturing and finishing the same, and related information are disclosed, including a prosthetic joint having at least one superhard articulation surface.
Owner:DIAMICRON
Modified system and method for intraoperative tension assessment during joint arthroplasty
A modified system for assessing tension intraoperatively during joint arthroplasty includes a discrete sensor array, protector and trial. The protector is mechanically connected to the joint trial and covers the sensor array to protect it from wear. The sensor array can be positively located to prevent it from moving during use. In assembly of the modified system, the sensor array and protector are sterilized as discrete elements. After sterilization, the protector is removably attached to one of the trials with the sensor array substantially covered by the protector to protect the sensor from wear.
Owner:DEPUY PROD INC
Modular total ankle prosthesis apparatuses, systems and methods, and systems and methods for bone resection and prosthetic implantation
Ankle prosthesis apparatuses, systems and methods are provided as disclosed herein. Additionally, systems and methods for bone resection and implantation of prosthetics are provided, including surgical techniques and related instrumentation. An ankle prosthesis apparatus can include a talar component having a lower surface with a bone fixation portion for fixation to a talus bone and an upper surface designed for articulation with a bearing component. The bearing component can have a lower surface for articulation with the talar component and an upper surface for articulation with a tibial component. The tibial component can have a lower surface for articulation with the bearing component and an upper surface with a bone fixation portion for fixation to a tibia bone and / or a fibula bone. The bearing component can have a protrusion on its upper surface adapted for engagement with a recess on the tibial component to allow desired rotational and translational movement. Methods and systems can be used to prepare a bone surface for implantation of a prosthesis including determining a location for a curved cut line on the bone surface and drilling a series of holes tangent to the curved cut line to create a curved bone resection surface. Methods and systems can be used for the implantation of an ankle joint prosthesis including the use of an alignment guide, tibia and talus drill guides, tibia and talus saw guides, and tibia and talus broach guides, all components of which can be placed on and removed from a plurality of alignment anchor pins throughout the implantation procedure. A method for medially to laterally implanting an ankle joint prosthesis can include exposing tibia and talus bones from the medial side, resection of the tibia and talus bones, broaching the tibia and talus bones, and positioning and affixing the ankle joint prosthesis components.
Owner:INTEGRA LIFESCI
Resorbable interposition arthroplasty implant
InactiveUS6017366AImprove permeabilityAvoid collisionFinger jointsWrist jointsTrapezium BoneSurgical department
A resorbable implant for interposition arthroplasty which is intended to fill a void between two adjacent bone ends, providing a cushion between the bone ends to prevent impingement of the bone ends while providing time for tissue to infiltrate into the space occupied by the implant. It has a protracted resorption time of preferably at least three months to allow time for the proliferation of load-bearing host fibrous tissue in place of the resorbed implant material. The implant preferably is porous with a pore size of greater than about 80 microns in order to enhance infiltration of fibrous tissue. The implant has a modulus in the range of 0.8 to 20 MPa which is soft enough to allow it to conform to surface irregularities of the adjacent bone surfaces while being hard enough to maintain a desired separation between those bones while tissue infiltration replaces the resorbable implant material. The implant may be preformed to the desired shape or alternatively may be formable by the surgeon by methods such as carving with a scalpel. A preferred application for the implant is as a trapezium bone replacement.
Owner:WL GORE & ASSOC INC
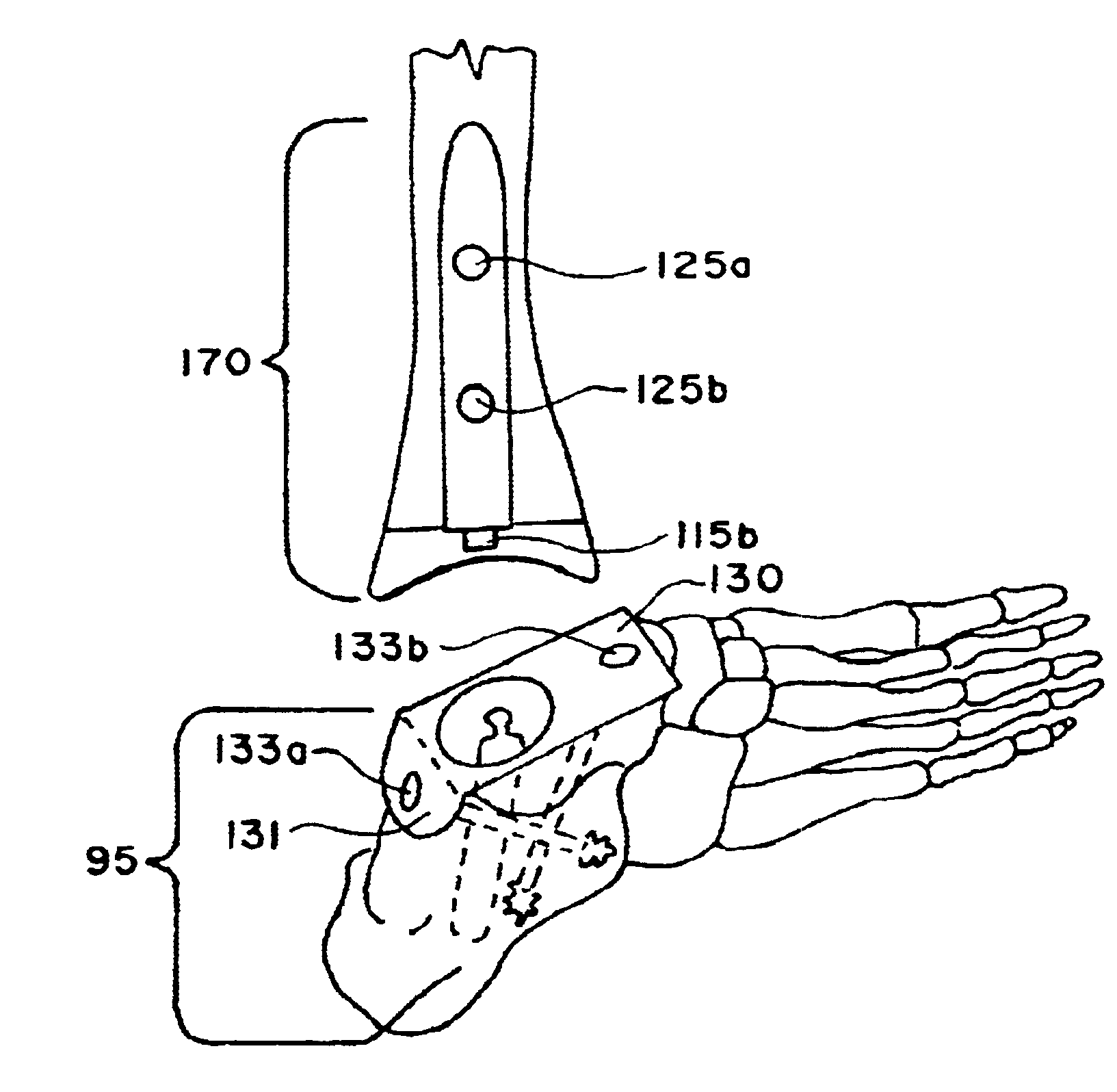
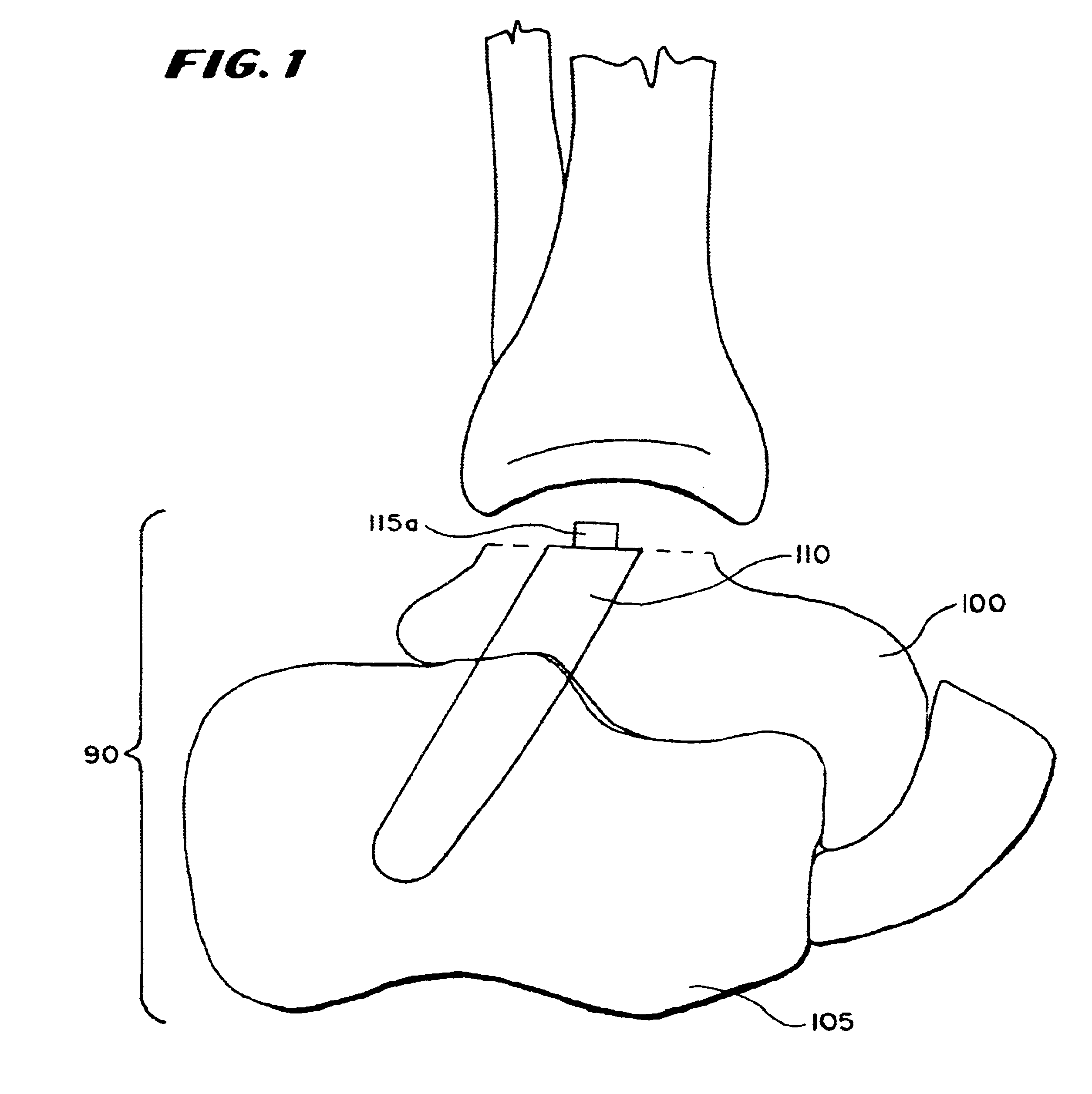
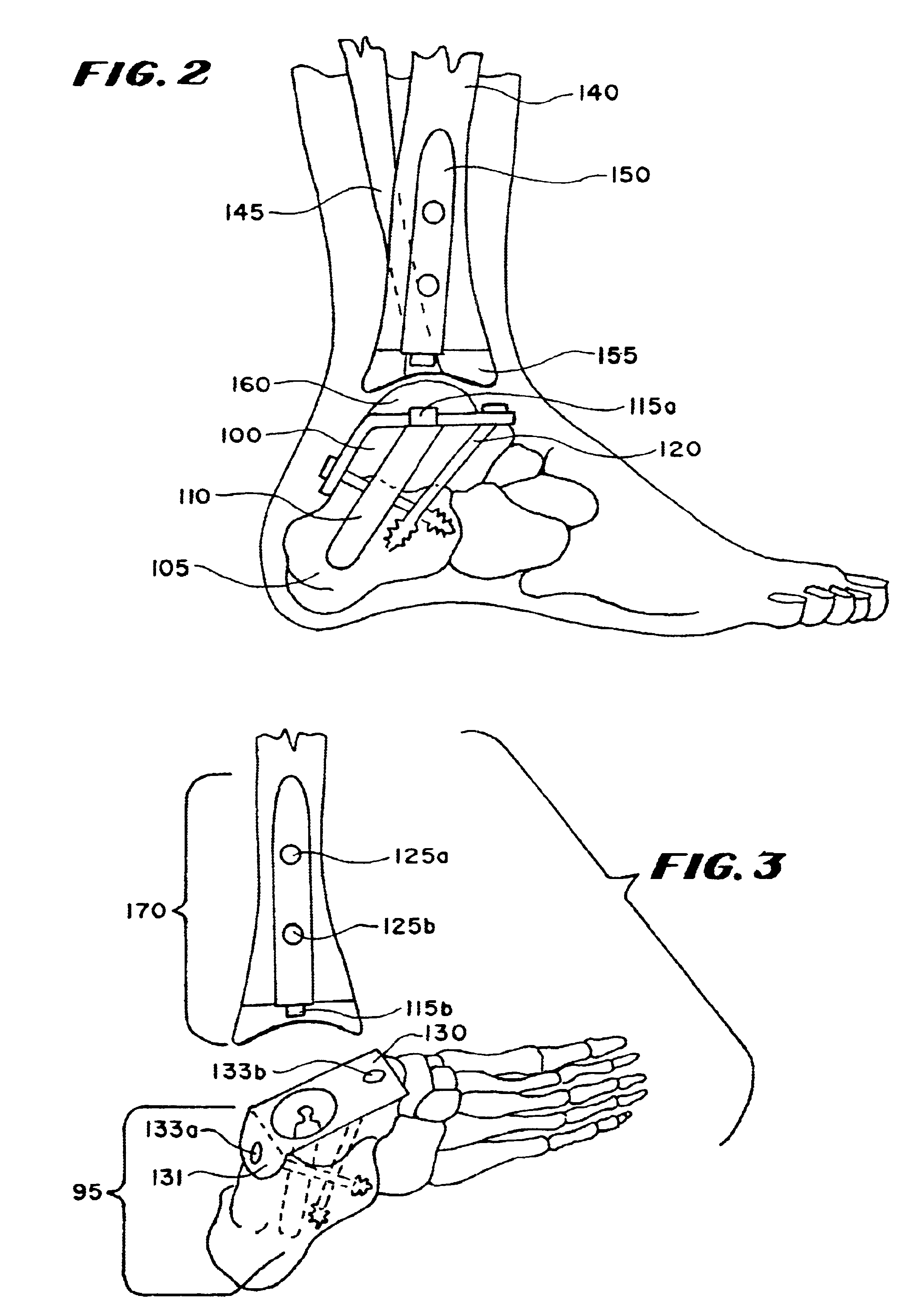
Ankle replacement system
A total ankle replacement system, novel surgical method for total ankle replacement, and novel surgical tools for performing the surgical method are described. The total ankle replacement system includes the calcaneus in fixation of a lower prosthesis body, thereby significantly increasing the amount of bone available for fixation of the lower prosthesis body and allowing the lower prosthesis body to be anchored with screws. The total ankle replacement system further includes a long tibial stem which can also be anchored into the tibia with, for example, screws, nails, anchors, or some other means of attachment. The novel surgical arthroscopic method allows introduction of ankle prostheses into the ankle joint through an exposure in the tibial tubercle. Various novel surgical instruments, such as a telescoping articulating reamer and a talo-calcaneal jig, which facilitate the novel surgical method, are also described.
Owner:INBONE TECH
Implant Device and Method for Manufacture
Disclosed are systems, devices and methods for optimizing the manufacture and / or production of patient-specific orthopedic implants. The methods include obtaining image data of a patient, selecting a blank implant to be optimized for the patient, and modifying the blank implant utilizing techniques disclosed herein to alter specific features of the implant to conform to the patient's anatomy.
Owner:CONFORMIS
Polymeric joint complex and methods of use
InactiveUS20060085075A1Increase and decrease constraintEasy for flexibilityFinger jointsWrist jointsHuman bodyArtificial joints
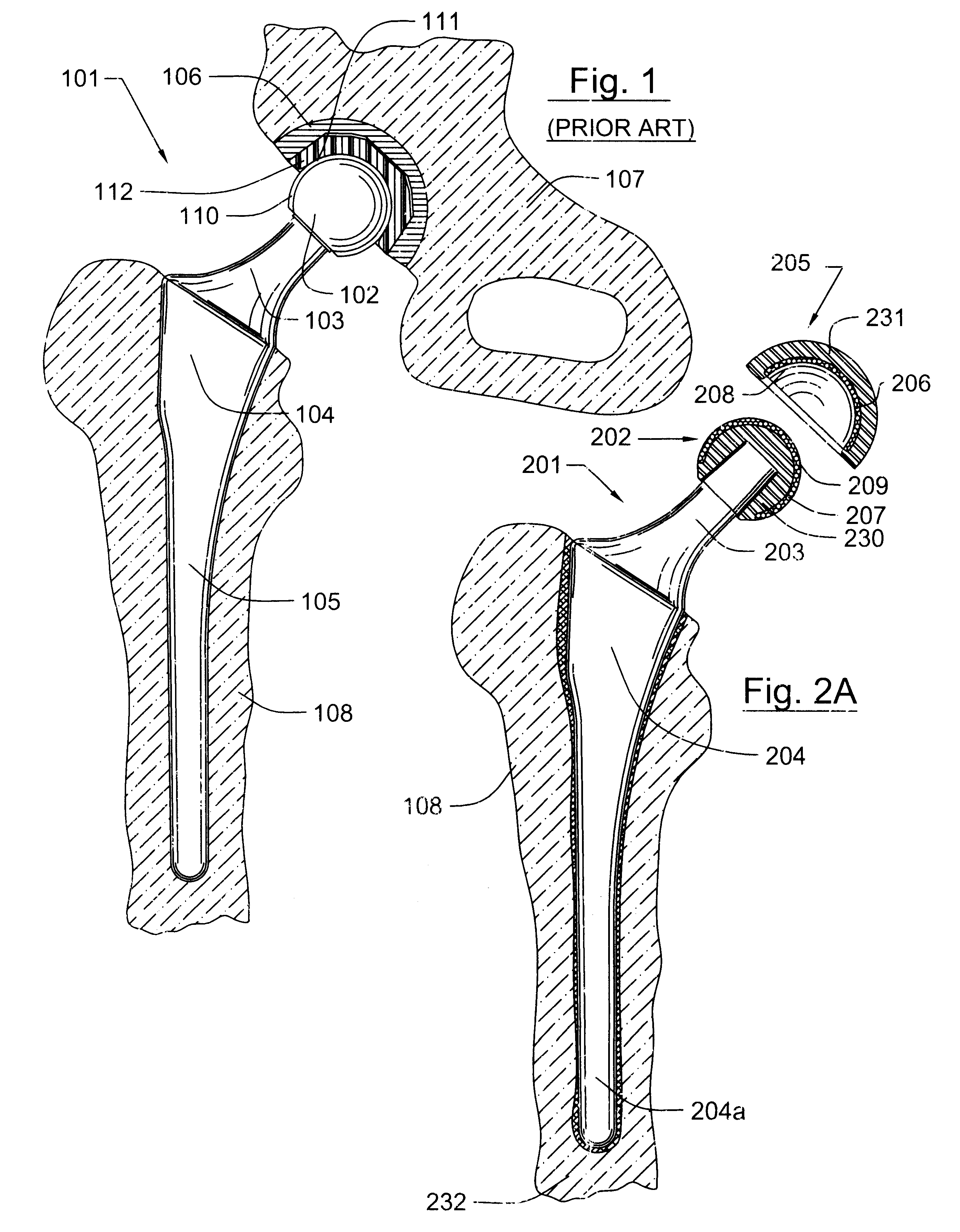
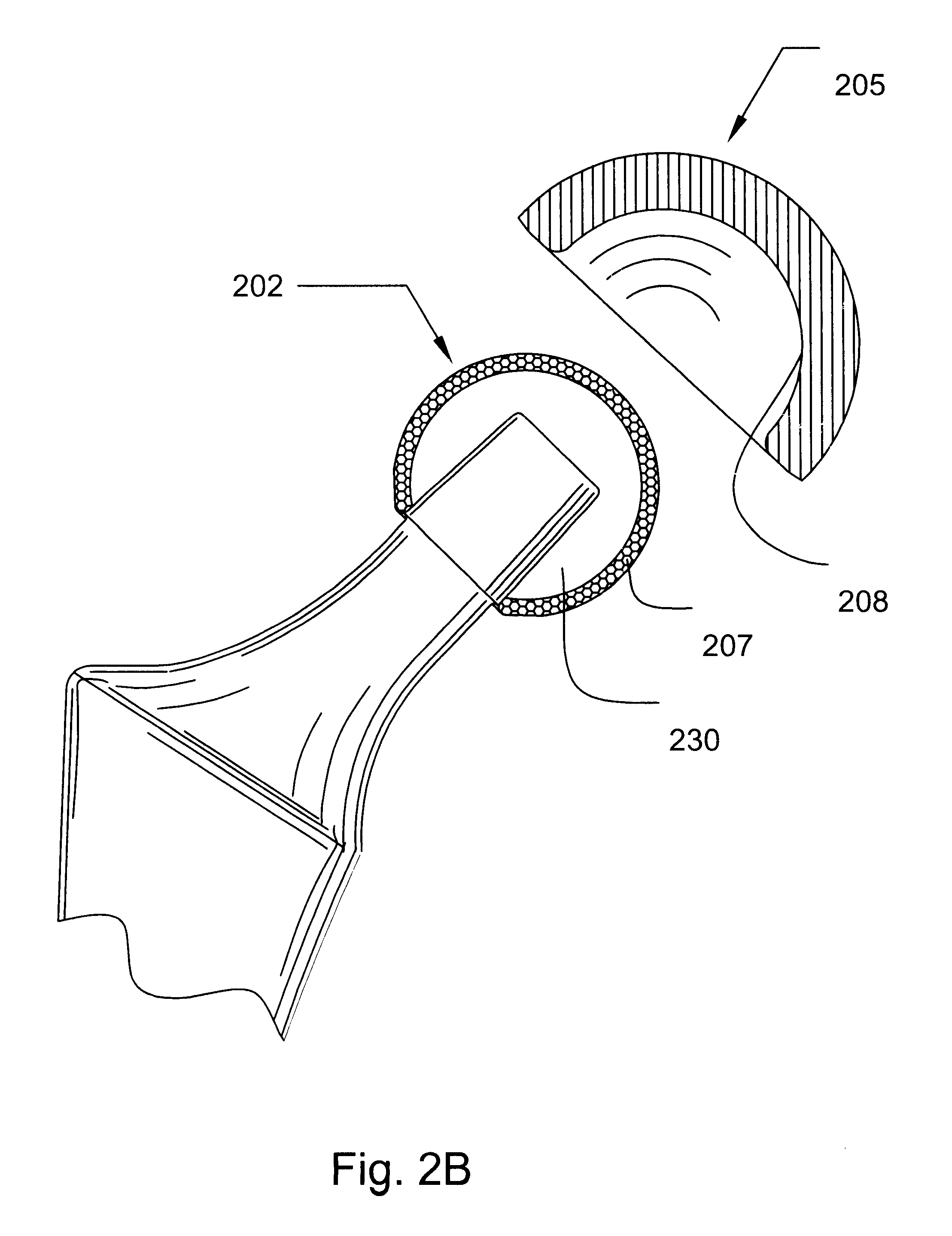
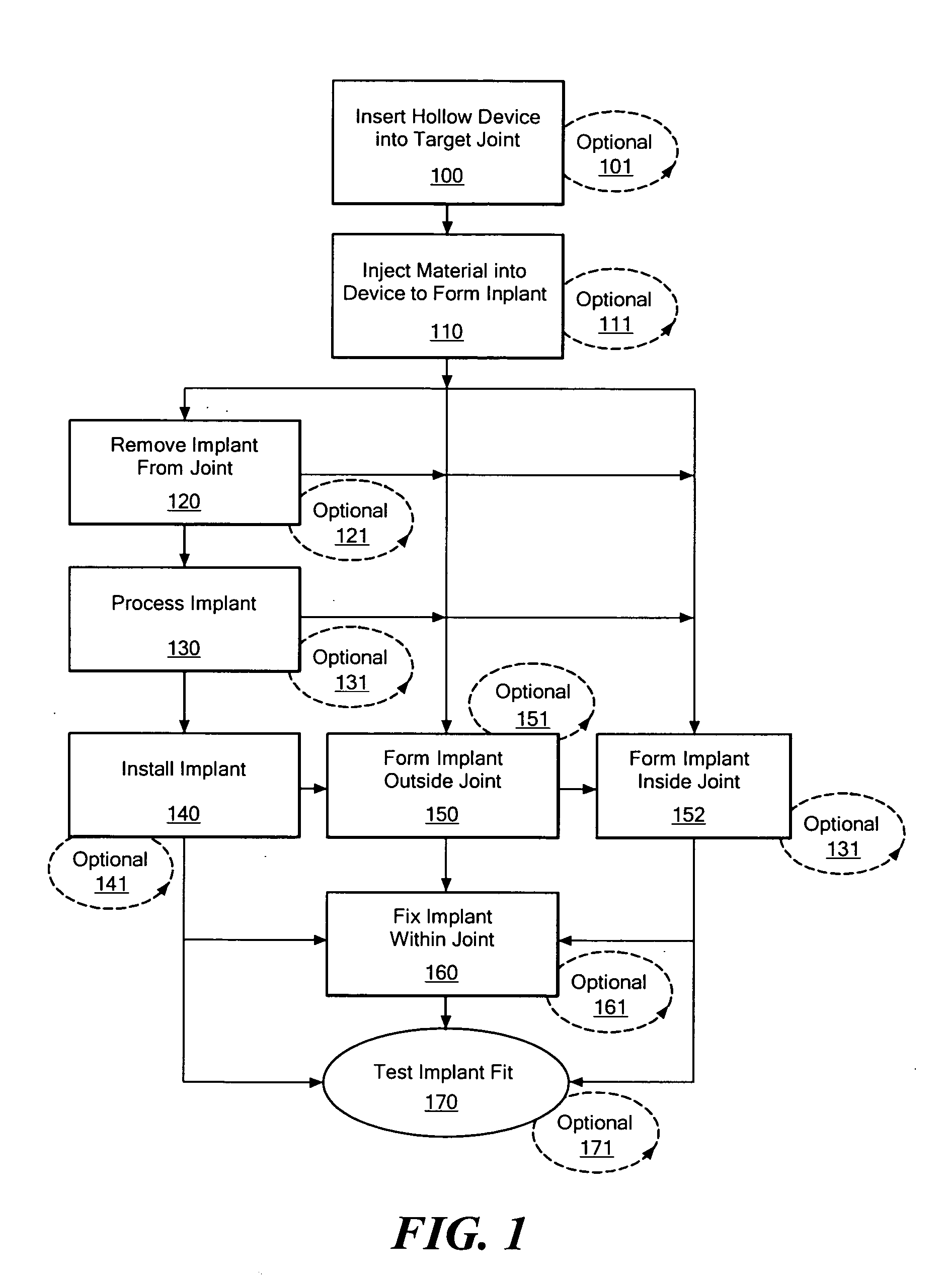
The invention describes a variety of implantable artificial joint complexes adapted for implantation within a target joint space within a human body. The joint complexes comprise: an expandable joint segment adapted to fit within the target joint space; and at least one of a first cannulated anchor adapted to engage the expandable joint segment and adapted to engage a bony structure adjacent the target joint space; and a second anchor adapted to engage the expandable joint segment and adapted to engage a bony structure adjacent a target joint space. The invention also discloses methods of implanting a patient specific artificial joint complex. The methods include the steps of: accessing a target joint space by creating an access hole through an adjacent bony structure; inserting a joint complex device having a cannulated anchor and an expandable joint segment through the access hole with the expendable joint segment being positioned between the surfaces forming the joint; injecting material into the expandable joint segment; and sealing access to the target joint space.
Owner:GMEDELAWARE 2
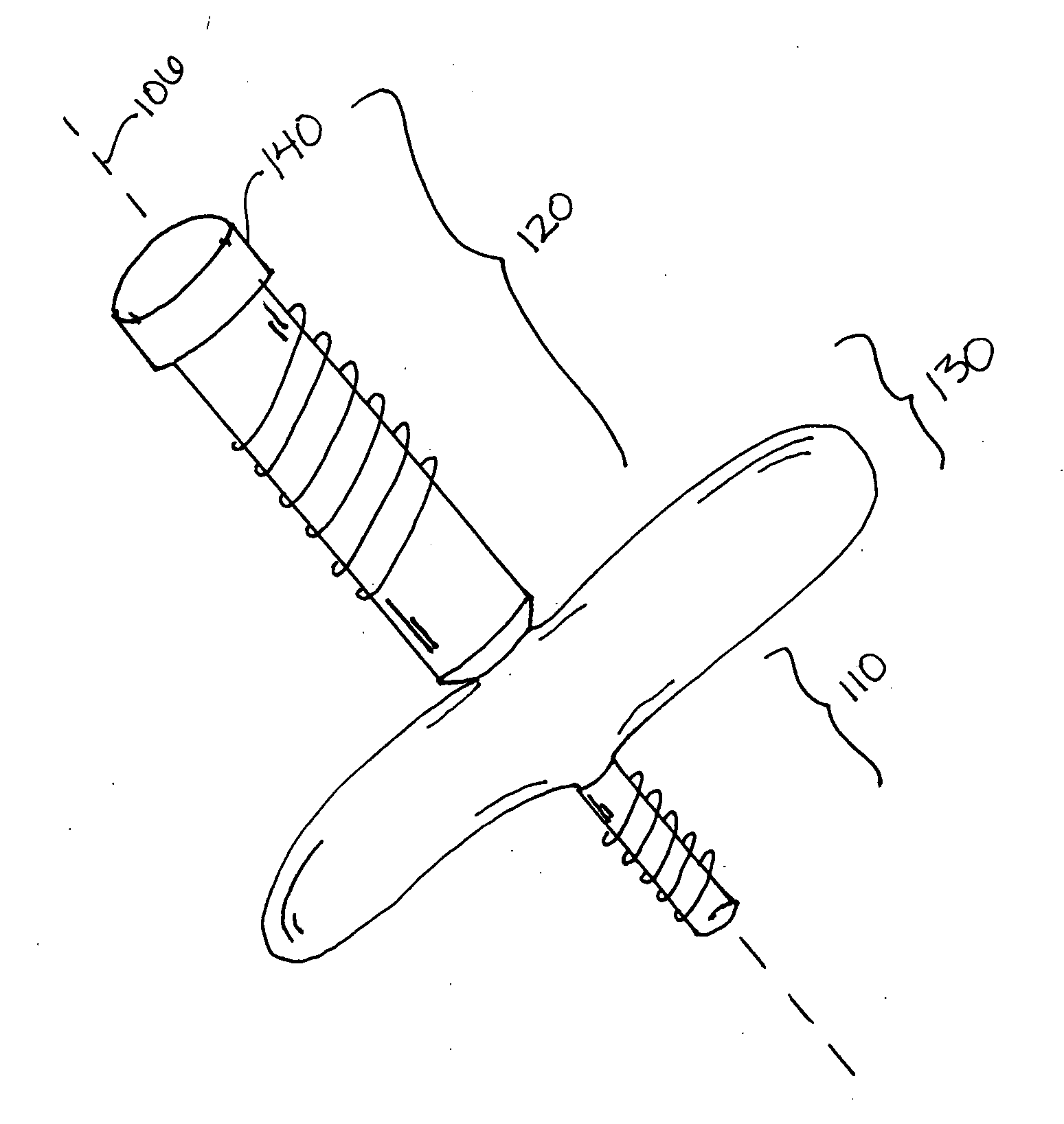
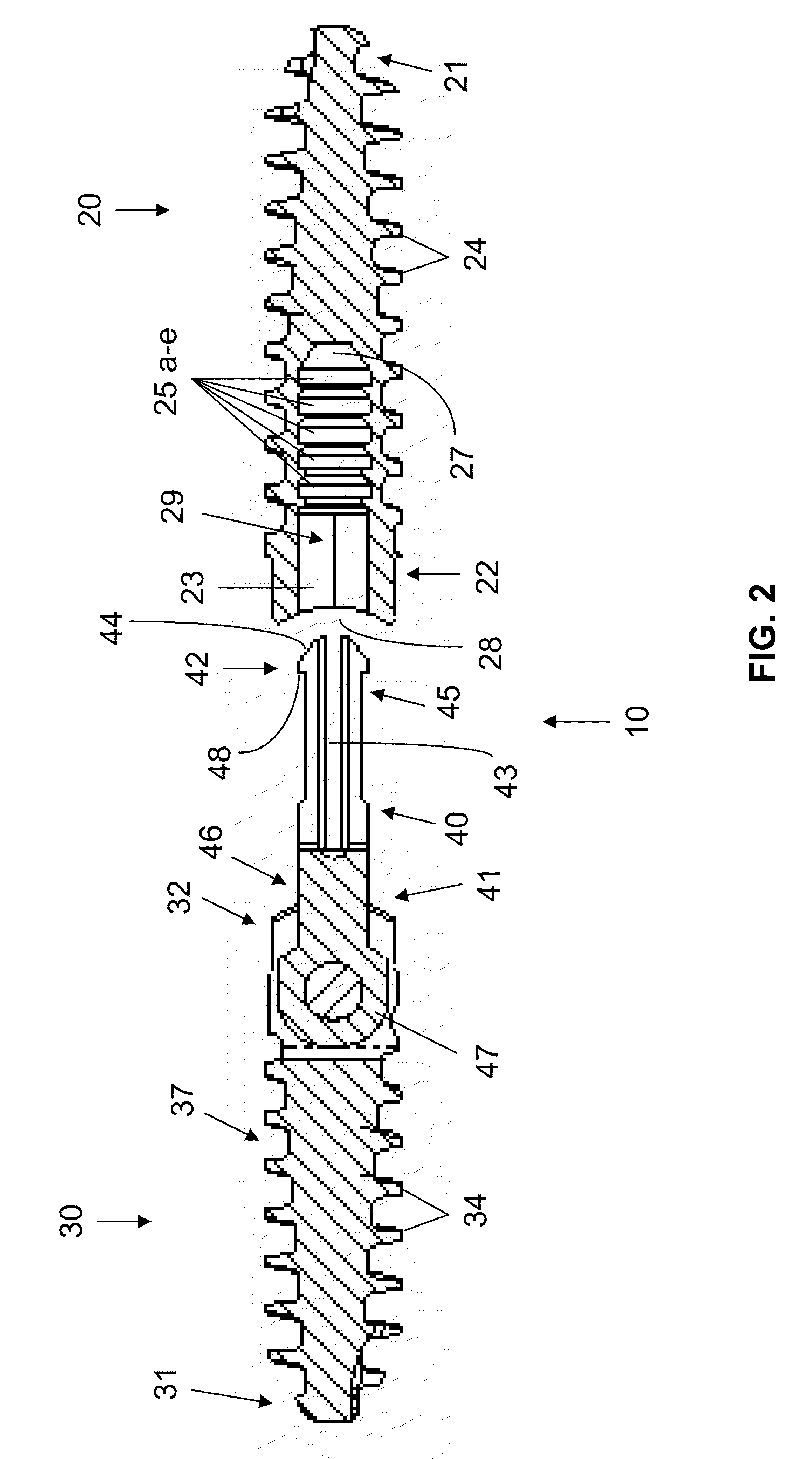
Bone joining apparatus and method
Provided is a bone joining device suitable for joining a first bone piece to a second bone piece. Also provided is a method of joining a first bone piece with a second bone piece in a living mammal. The method comprises inserting the above bone joining device between the first bone piece and the second bone piece.
Owner:ZIMMER INC
Prosthesis for partial replacement of an articulating surface on bone
Systems, including apparatus, methods, and kits, for replacing a portion of an articulating bone surface with a surface region of a partial prosthesis.
Owner:MAYO FOUND FOR MEDICAL EDUCATION & RES
Methods for Determining Meniscal Size and Shape and for Devising Treatment
The present invention relates to methods for determining meniscal size and shape for use in designing therapies for the treatment of various joint diseases. The invention uses an image of a joint that is processed for analysis. Analysis can include, for example, generating a thickness map, a cartilage curve, or a point cloud. This information is used to determine the extent of the cartilage defect or damage and to design an appropriate therapy, including, for example, an implant. Adjustments to the designed therapy are made to account for the materials used.
Owner:CONFORMIS
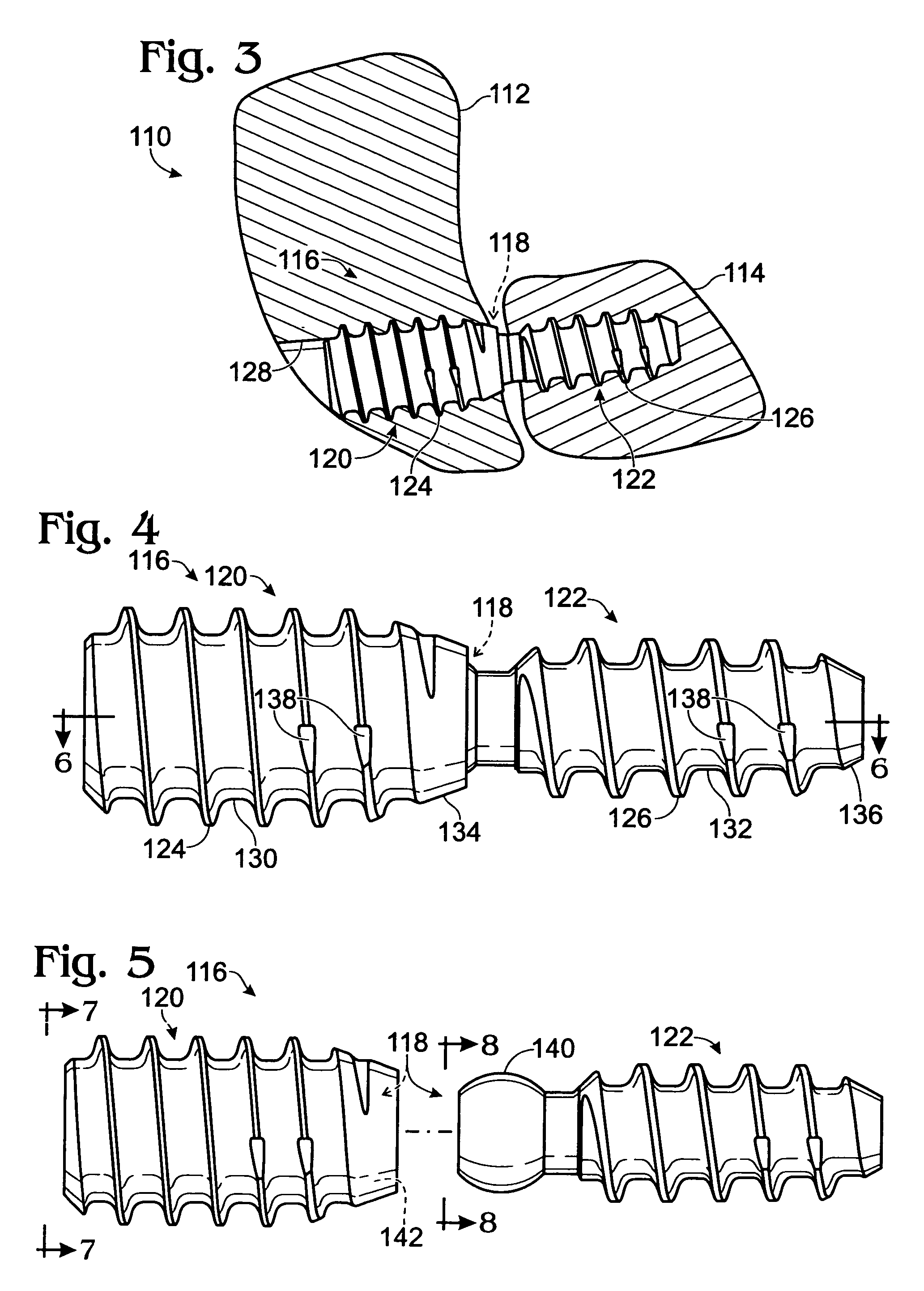
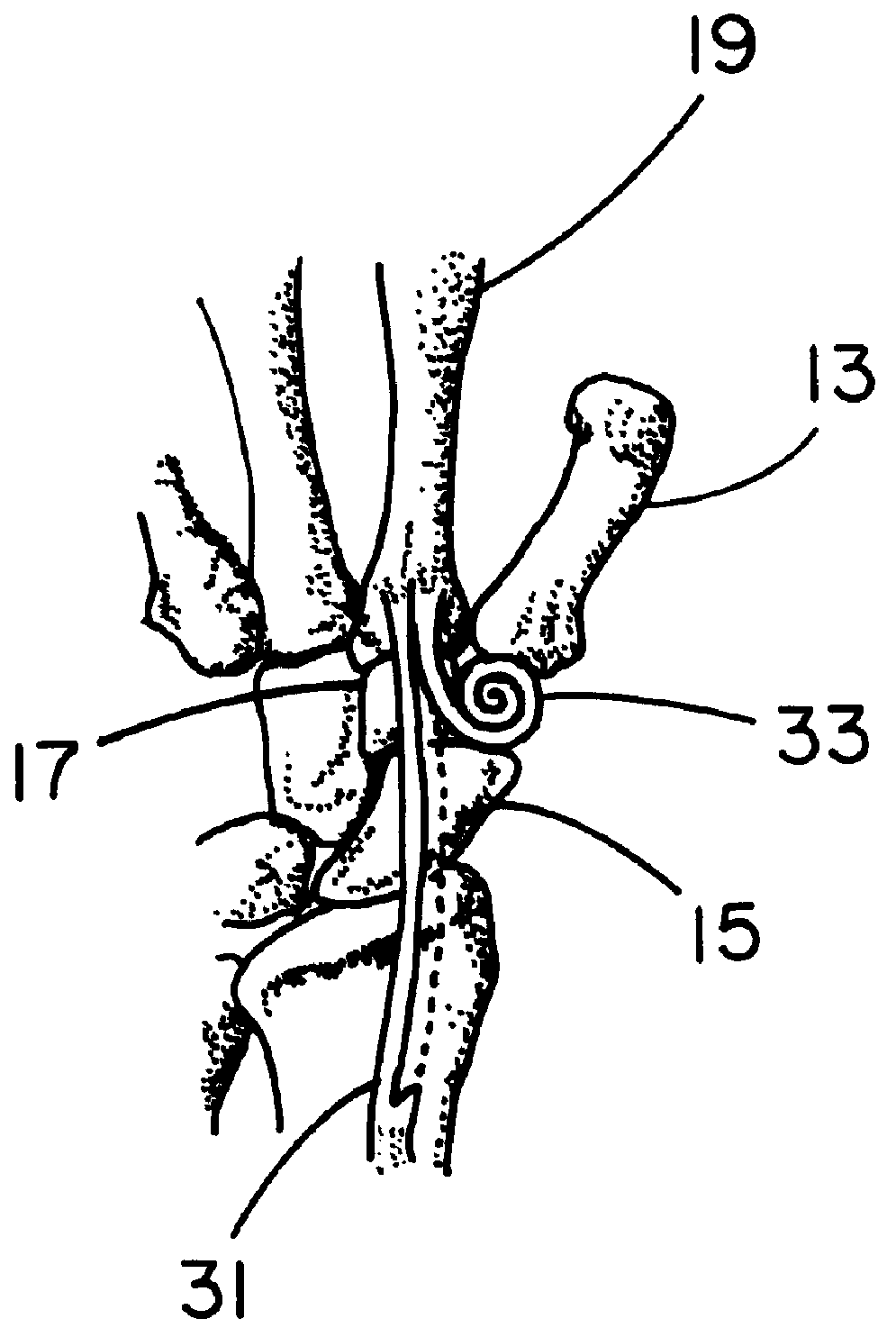
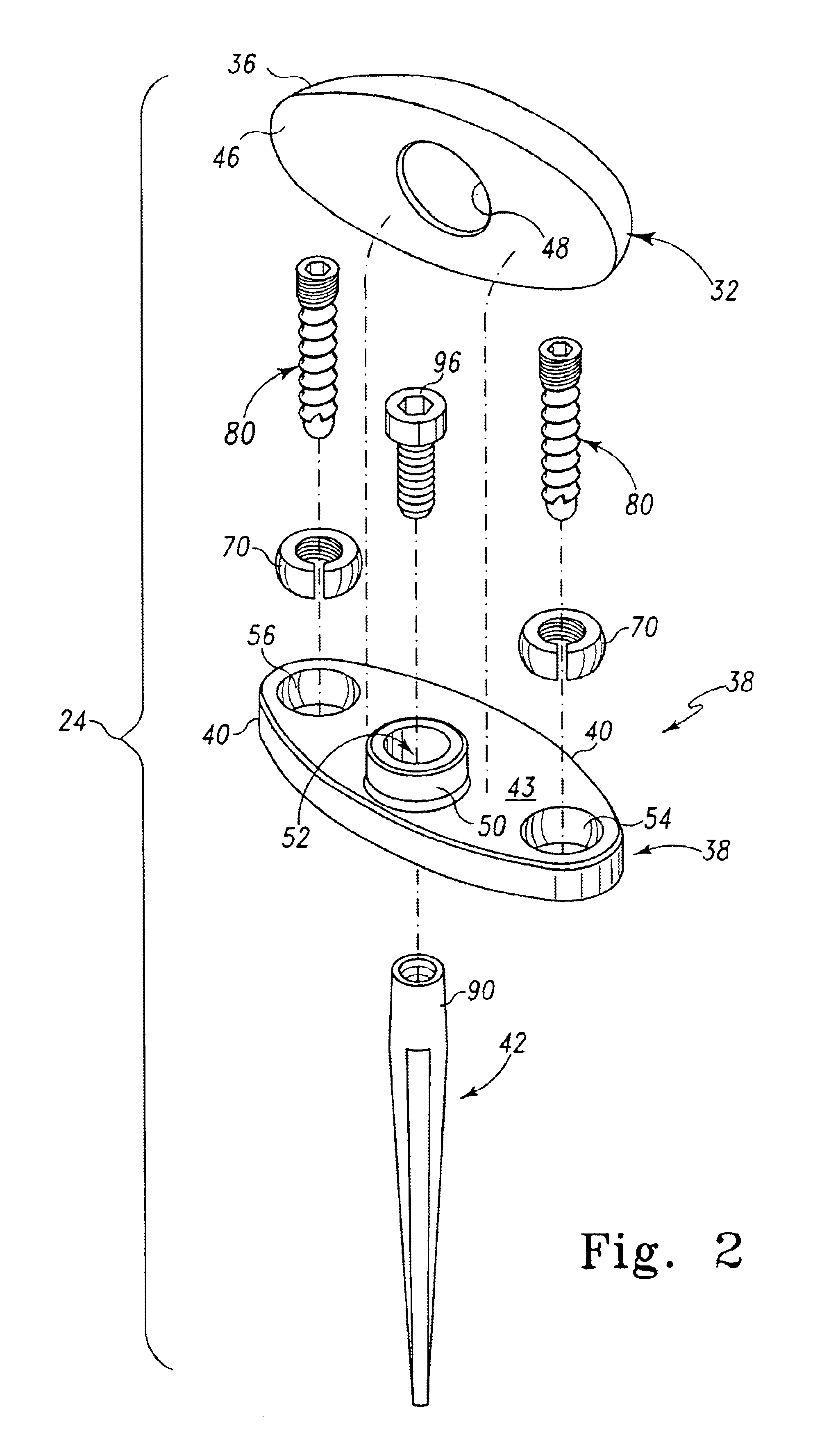
Distal component for wrist prosthesis
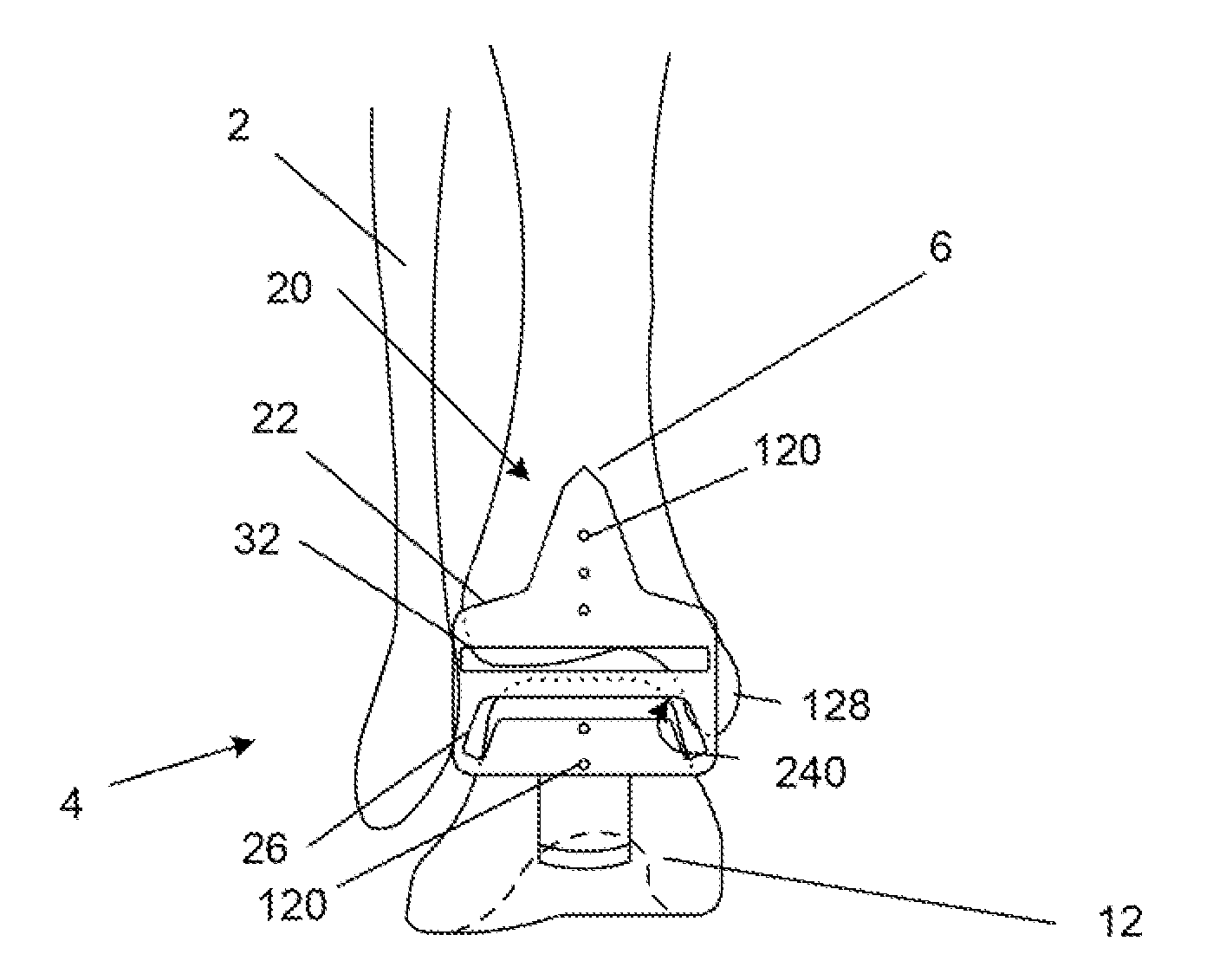
InactiveUS6890358B2Precise processingFirmer engagementWrist jointsAnkle jointsModularityCarpal bones
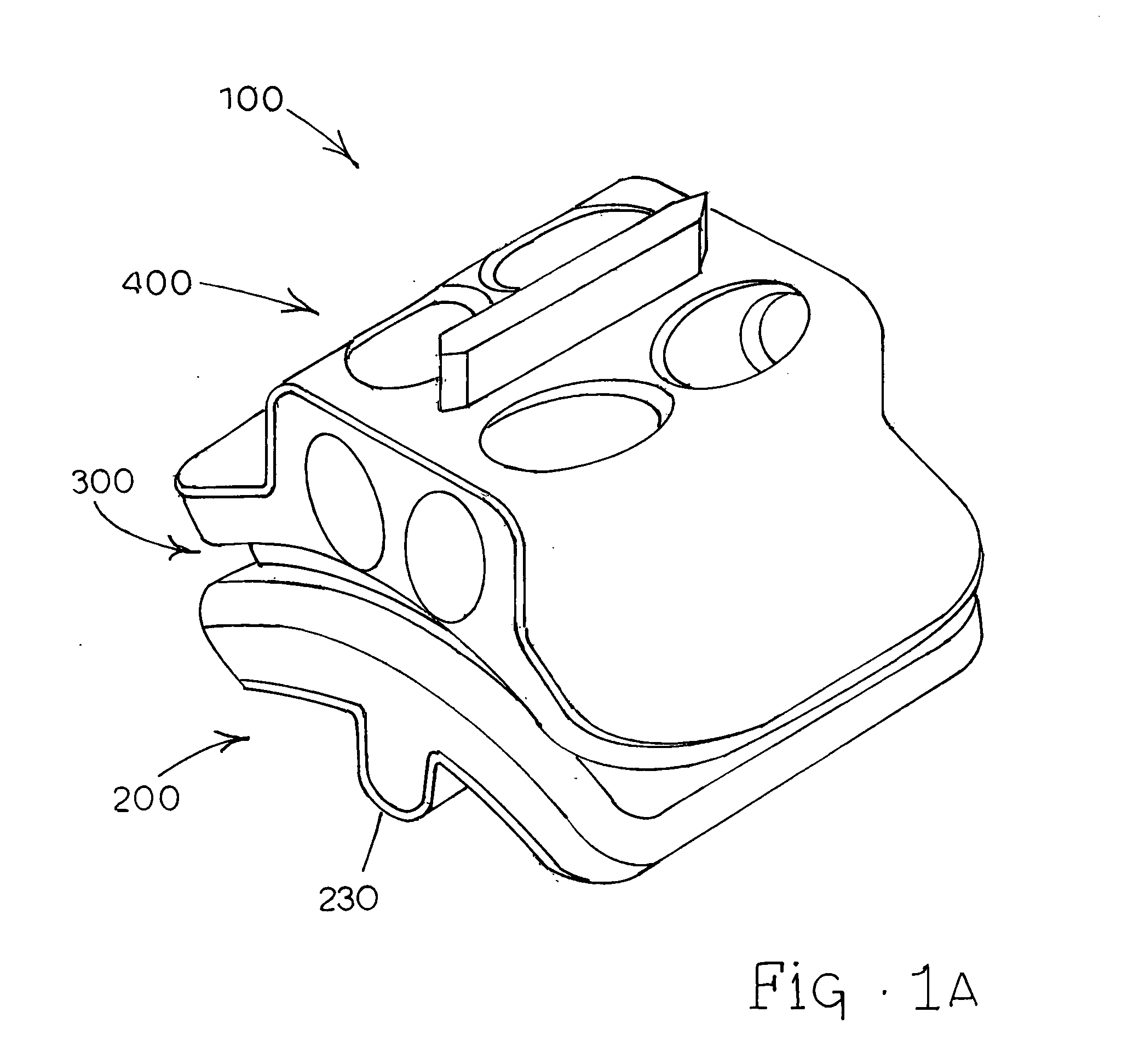
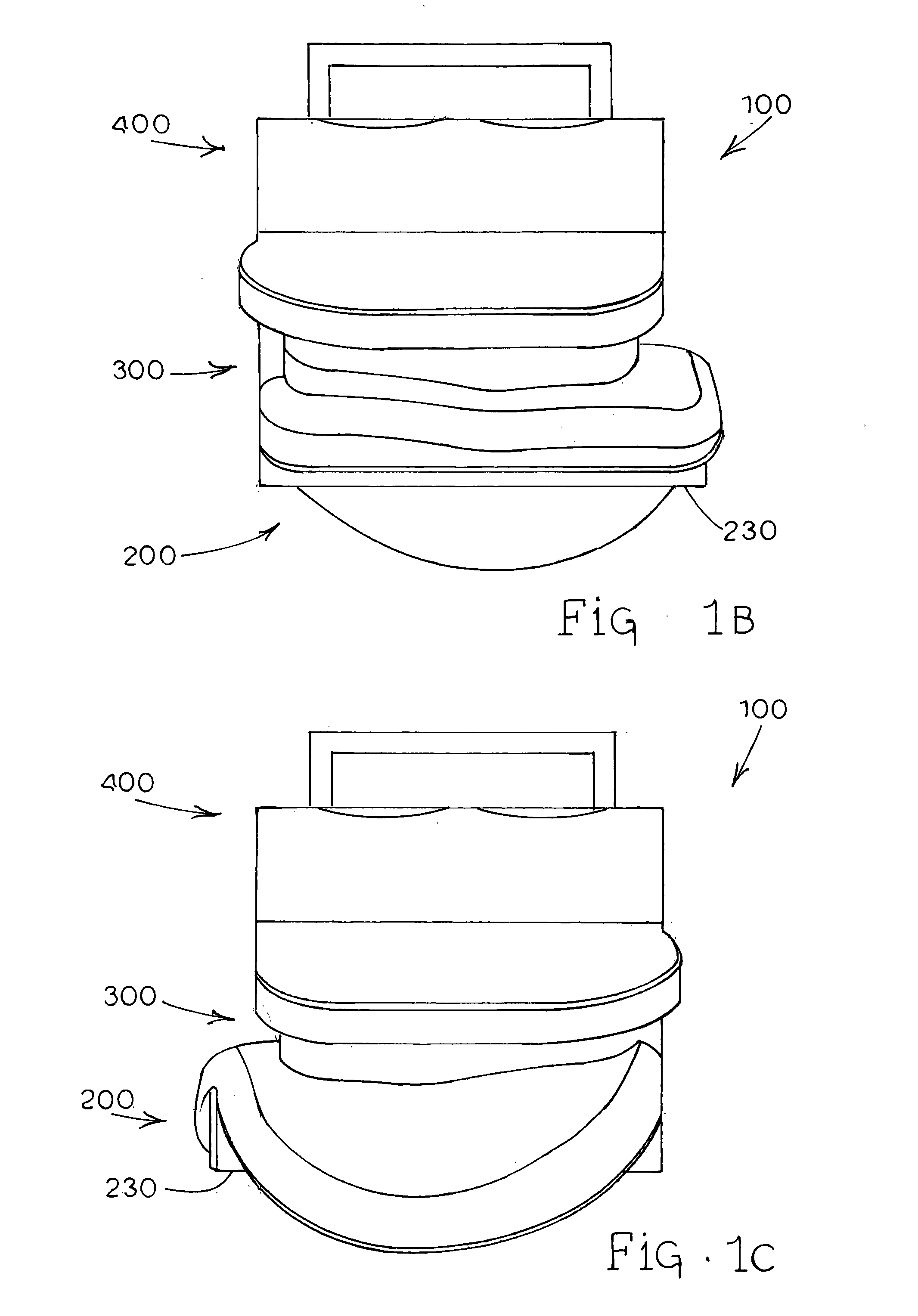
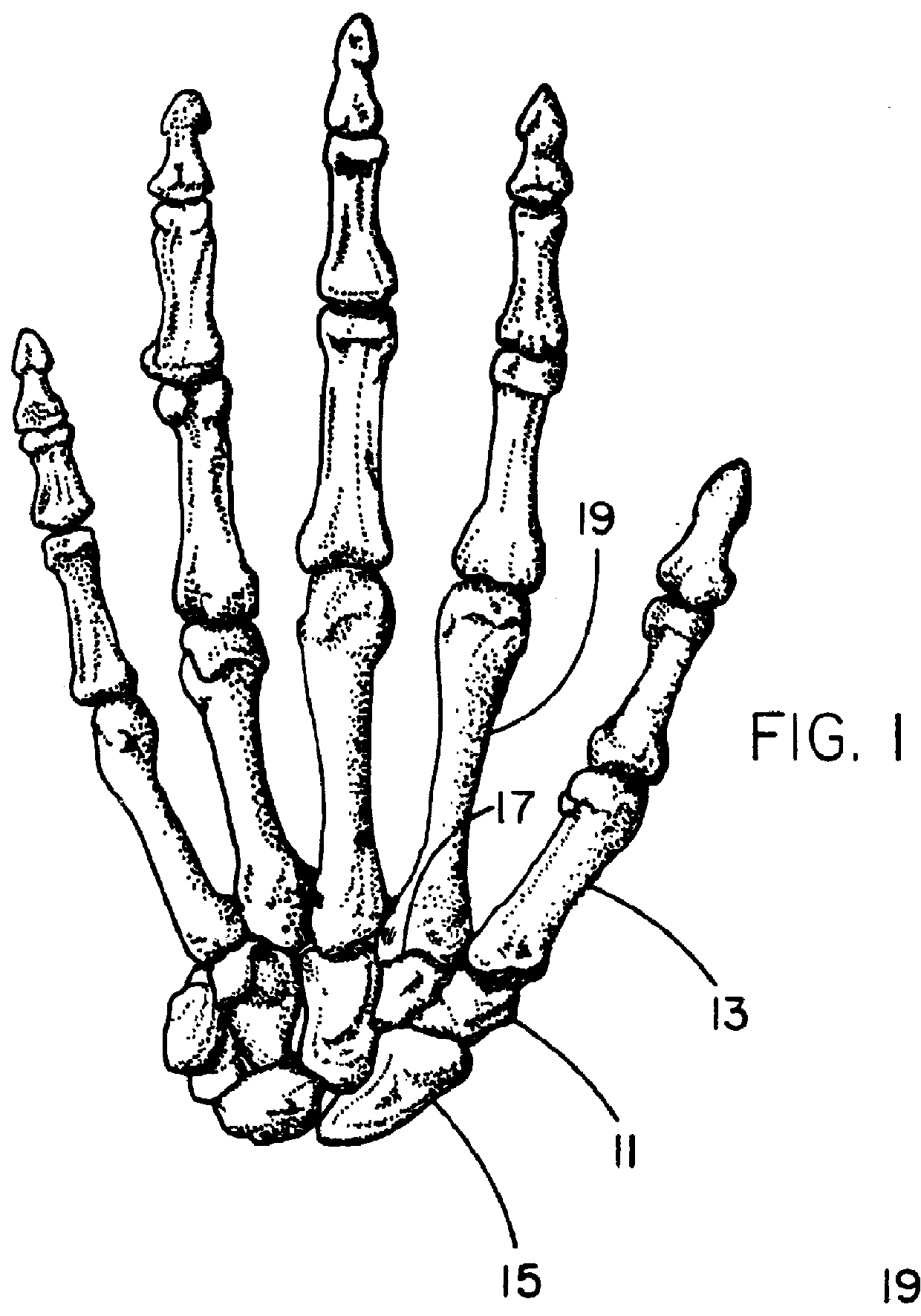
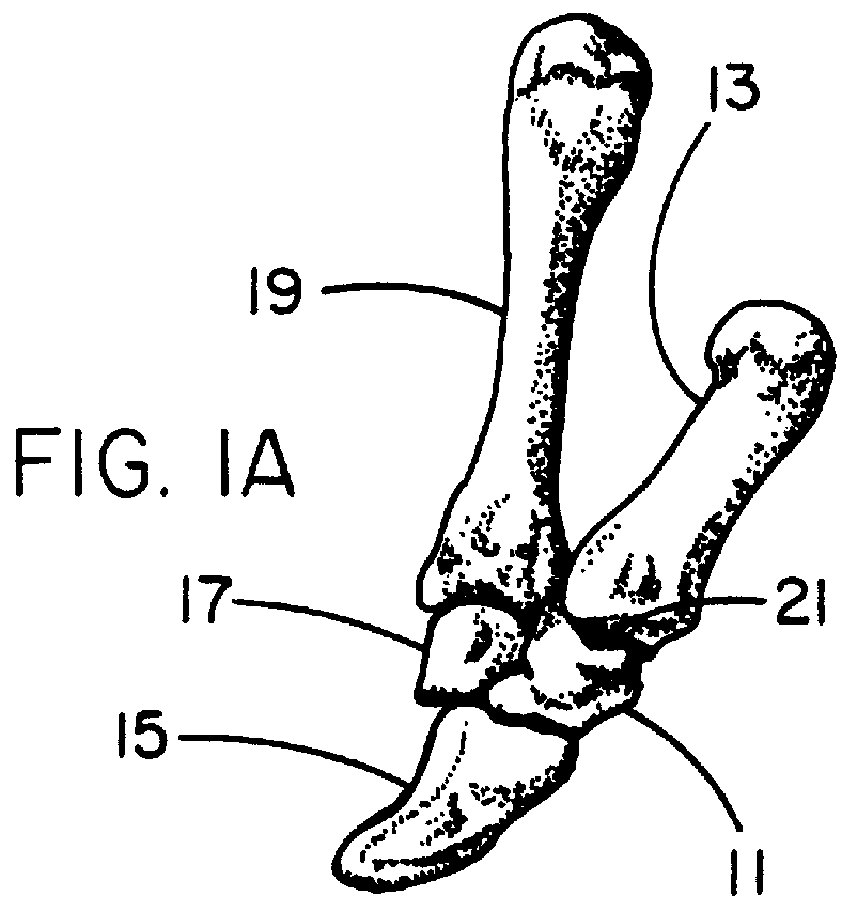
A distal component for a wrist prosthesis that utilizes fixation within the carpus complex, incorporates features that improve the probability of intercarpal fusion and allows modularity of articulating components. In one form, the subject invention includes an ovoid fixation plate having three holes and a boss. The three holes allow attachment of stems and / or screws distally for fixation in the carpus. The boss projects proximally from the plate, and serves as an attachment point for the articulating head. Modularity of the fixation and articulating components allow a surgeon many options for optimizing fixation distally, and articulation proximally. The proximal head of the distal component is designed to articulate with existing radial components. Since the proximal head of the distal component is modular, however, the head can be redesigned to accommodate later design changes in proximal components.
Owner:DEPUY PROD INC