Patents
Literature
9165results about "Organ movement/changes detection" patented technology
Efficacy Topic
Property
Owner
Technical Advancement
Application Domain
Technology Topic
Technology Field Word
Patent Country/Region
Patent Type
Patent Status
Application Year
Inventor
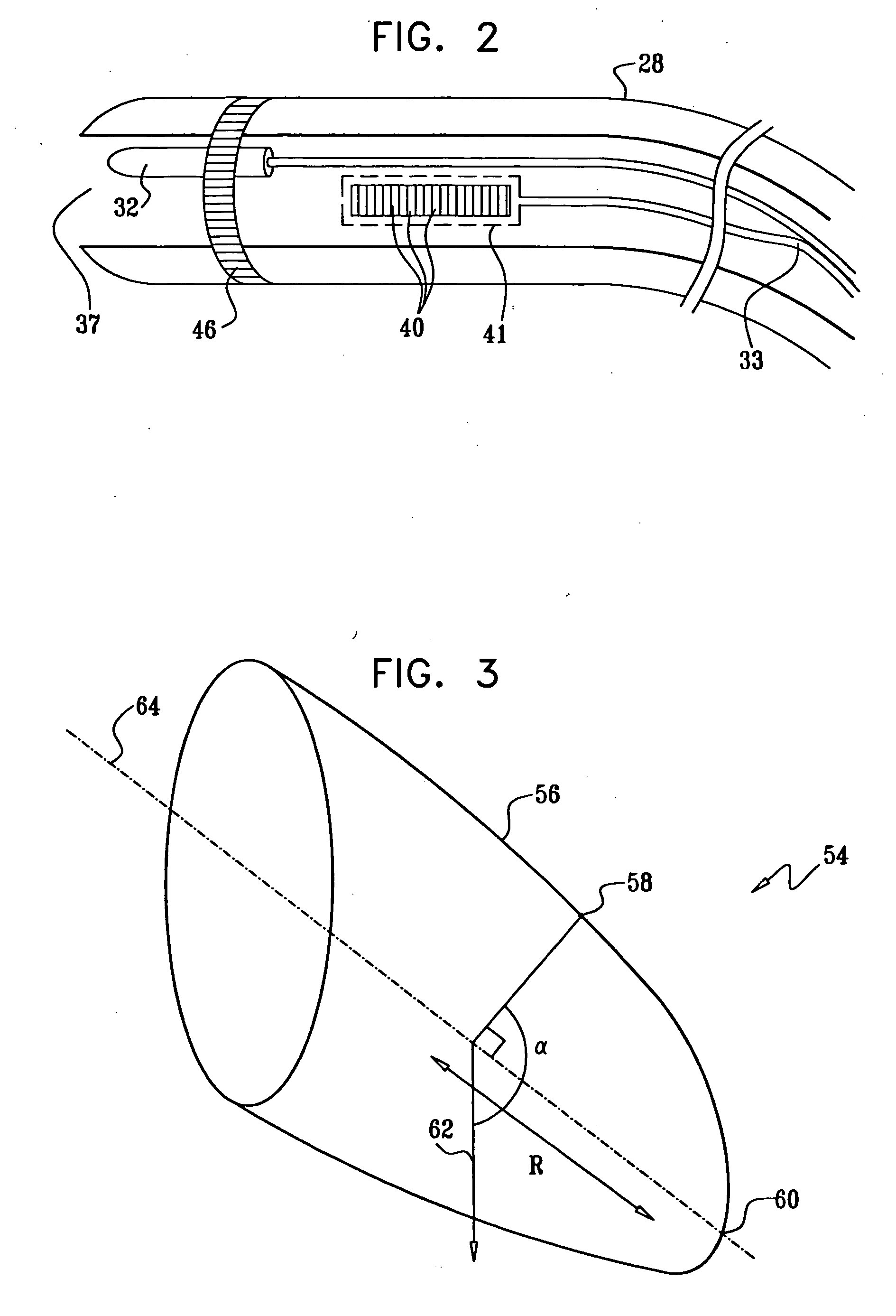
Ultrasonic needle guiding apparatus, method and system
InactiveUS20130158390A1Organ movement/changes detectionSurgical needlesPhase differenceDisplay device
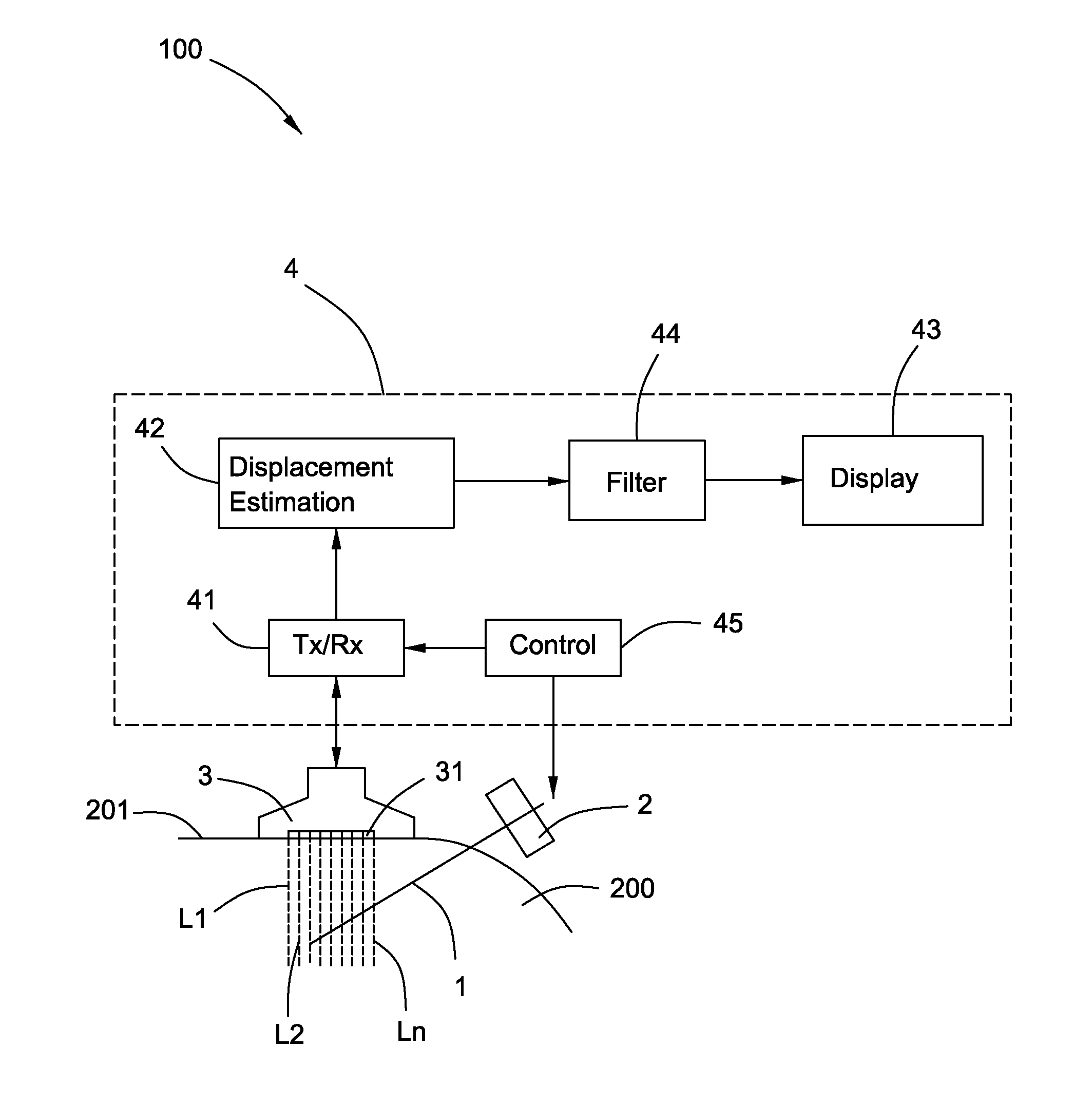
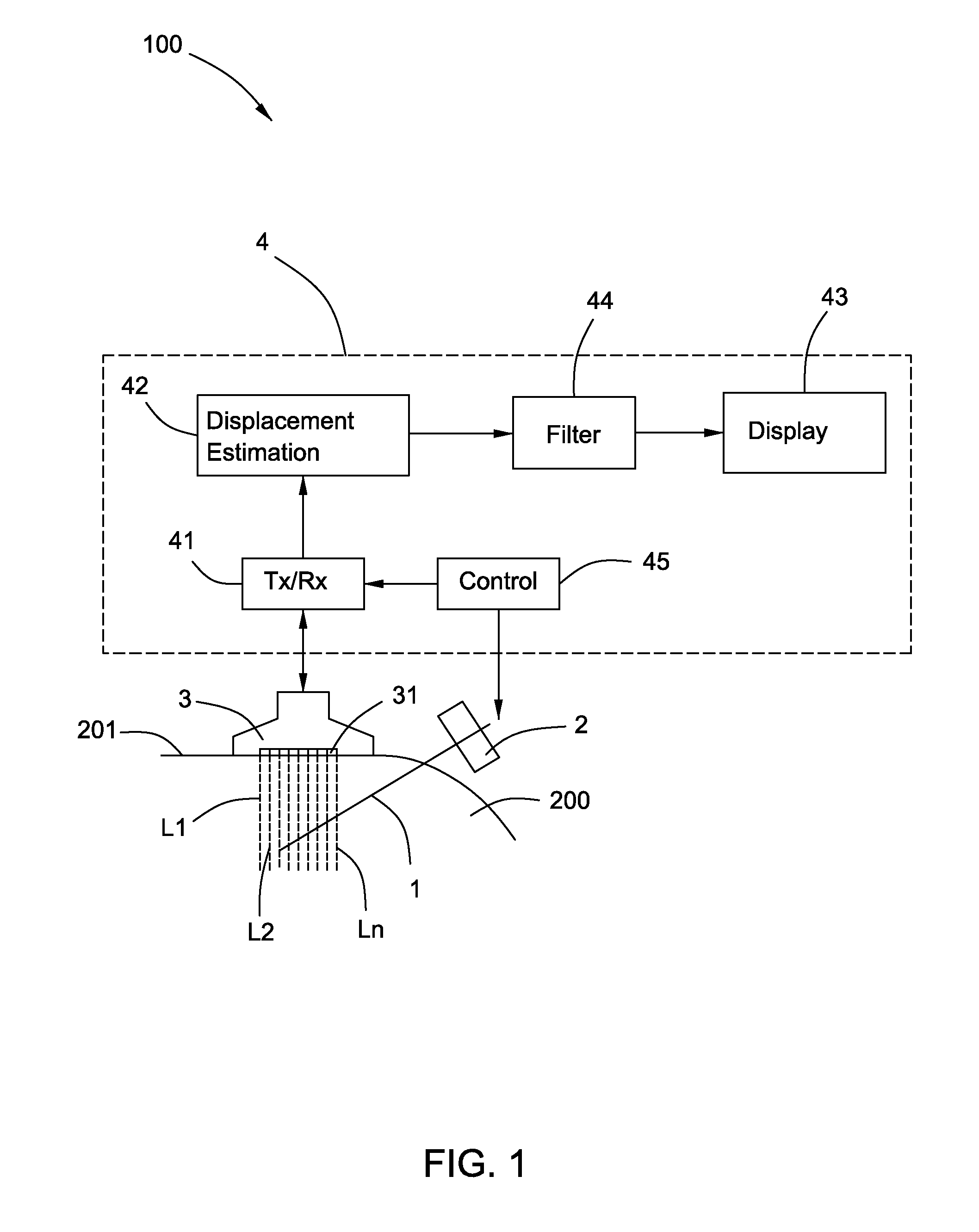
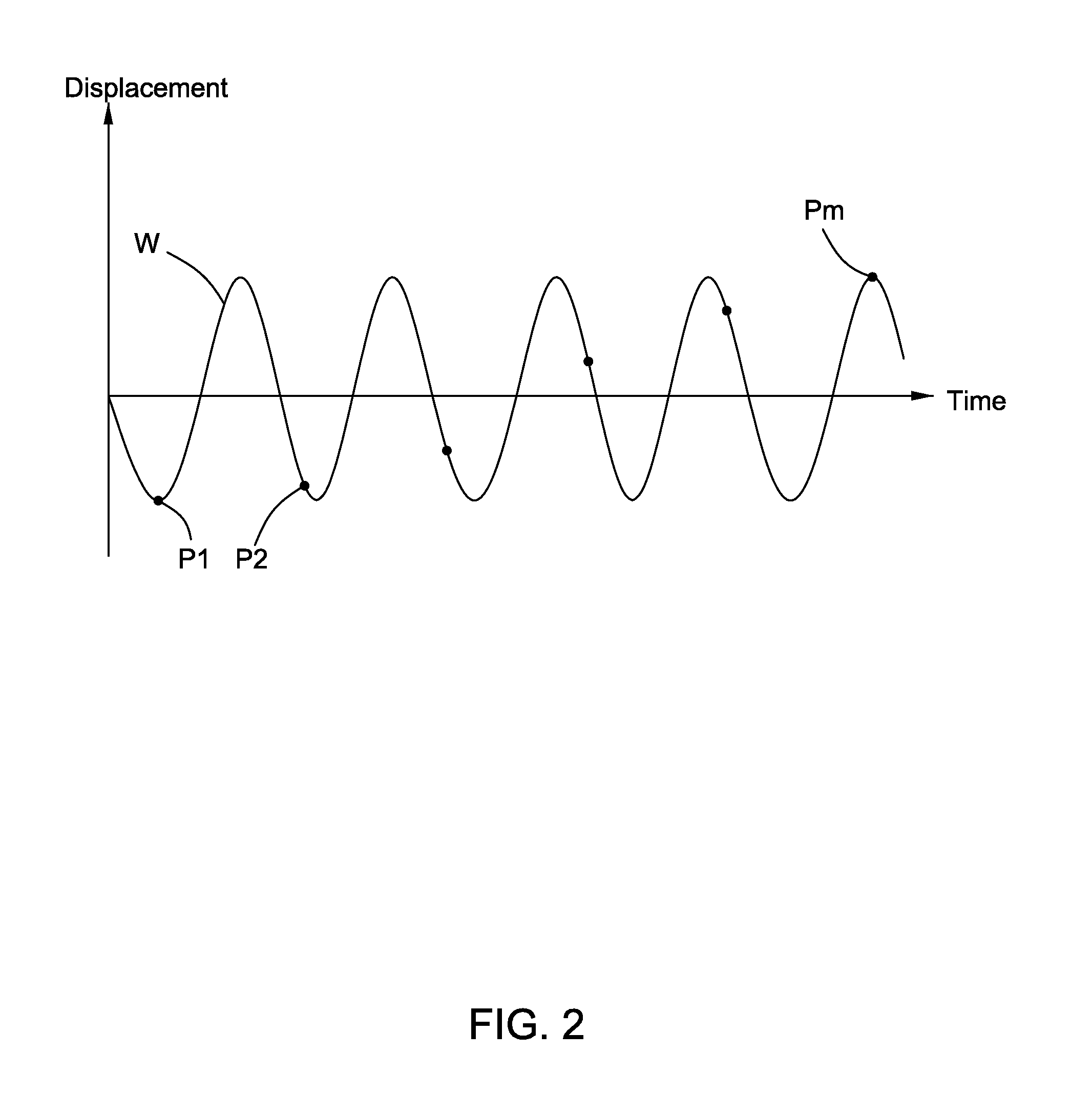
An apparatus is provided. The apparatus comprises a vibrator configured to vibrate a needle, an ultrasonic scanhead configured to transmit ultrasonic pulses and to receive return signals, and an ultrasonic system coupled to the ultrasonic scanhead. The ultrasonic system comprises a transmitter and receiver module coupled to the ultrasonic scanhead, a displacement estimation module coupled to the transmitter and receiver module, and a display coupled to the displacement estimation module. The transmitter and receiver module is configured to supply energizing pulses to the ultrasonic scanhead to transmit the ultrasonic pulses and to receive electrical signals produced by the ultrasonic scanhead according to the return signals. The displacement estimation module is configured to calculate motion displacements based on phase differences of the electrical signals. The display is configured to display an image according to the motion displacements.
Owner:GENERAL ELECTRIC CO
Imaging, therapy, and temperature monitoring ultrasonic system
An ultrasonic system useful for providing imaging, therapy and temperature monitoring generally comprises an acoustic transducer assembly configured to enable the ultrasound system to perform the imaging, therapy and temperature monitoring functions. The acoustic transducer assembly comprises a single transducer that is operatively connected to an imaging subsystem, a therapy subsystem and a temperature monitoring subsystem. The ultrasound systems may also include a display for imaging and temperature monitoring functions. An exemplary single transducer is configured such that when connected to the subsystems, the imaging subsystem can generate all image of a treatment region on the display, the therapy subsystem can generate high power acoustic energy to heat the treatment region, and the temperature monitoring subsystem can map and monitor the temperature of the treatment region and display the temperature on the display, an through the use of the single transducer. Moreover, the acoustic transducer assembly is configured such that the imaging, therapeutic heating and temperature monitoring of the treatment region can be conducted substantially simultaneously.
Owner:GUIDED THERAPY SYSTEMS LLC
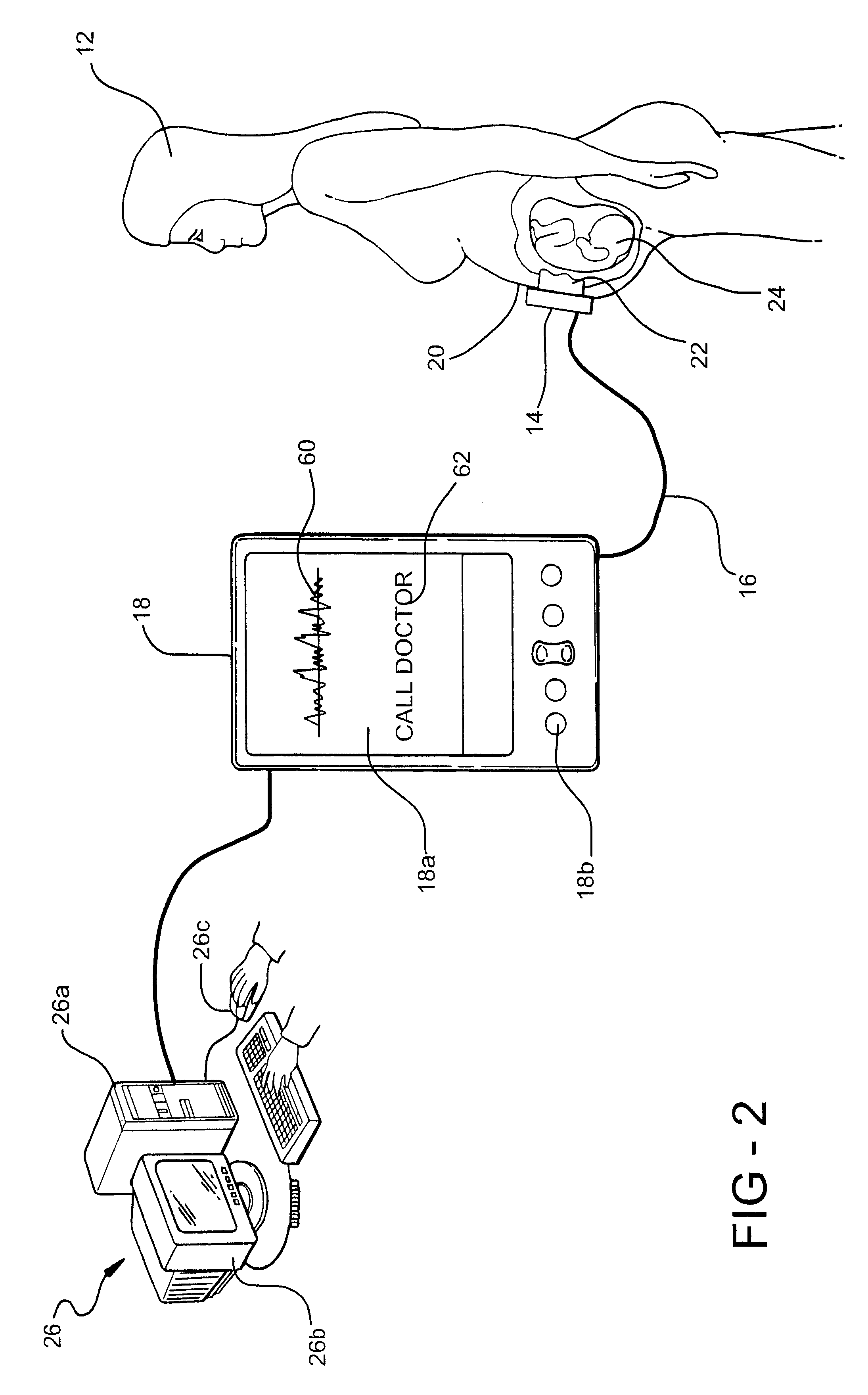
System and method for remote pregnancy monitoring
InactiveUS6610012B2Organ movement/changes detectionInfrasonic diagnosticsUltrasonic sensorTelecommunications link
Owner:MICROLIFE MEDICAL HOME SOLUTIONS
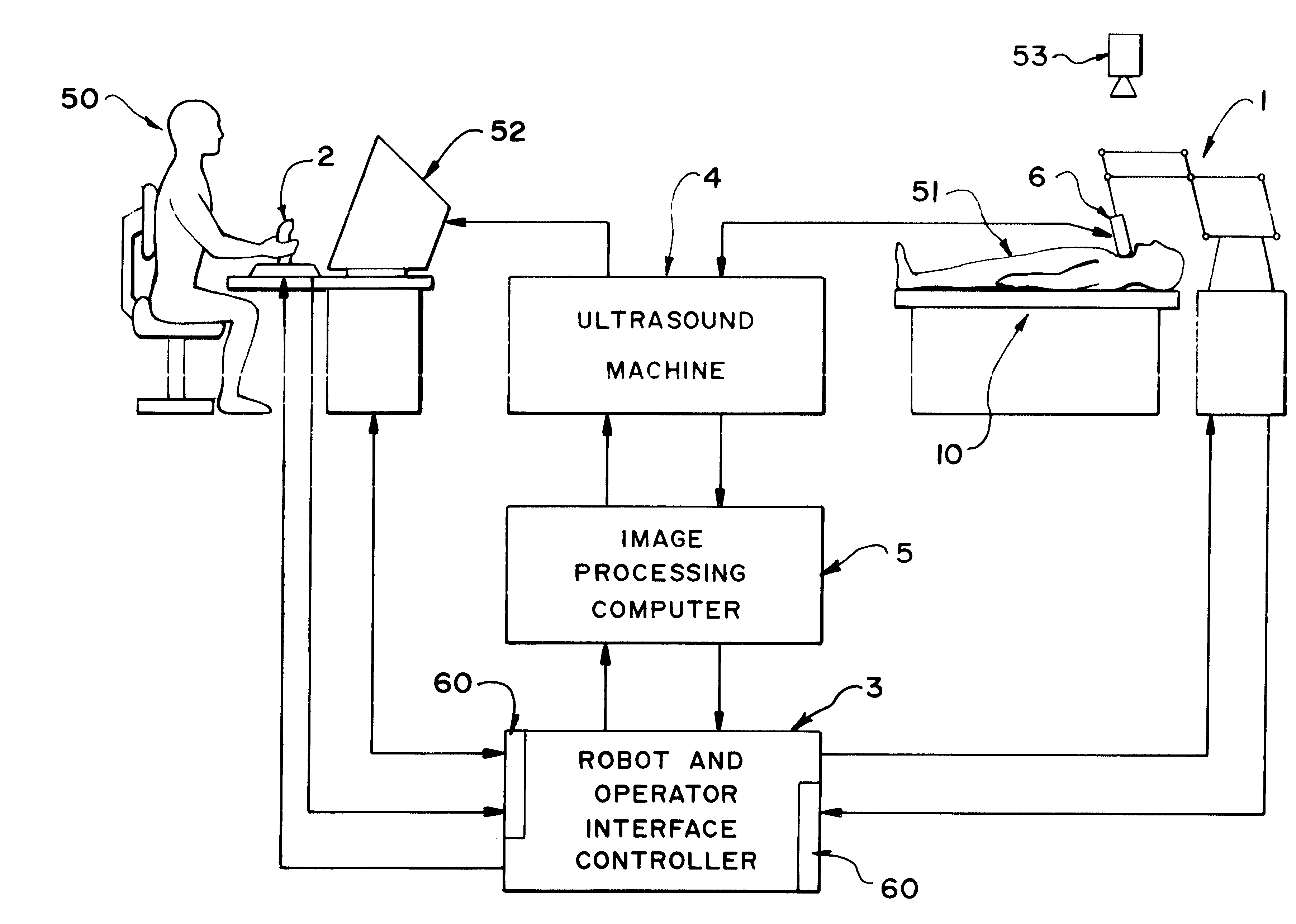
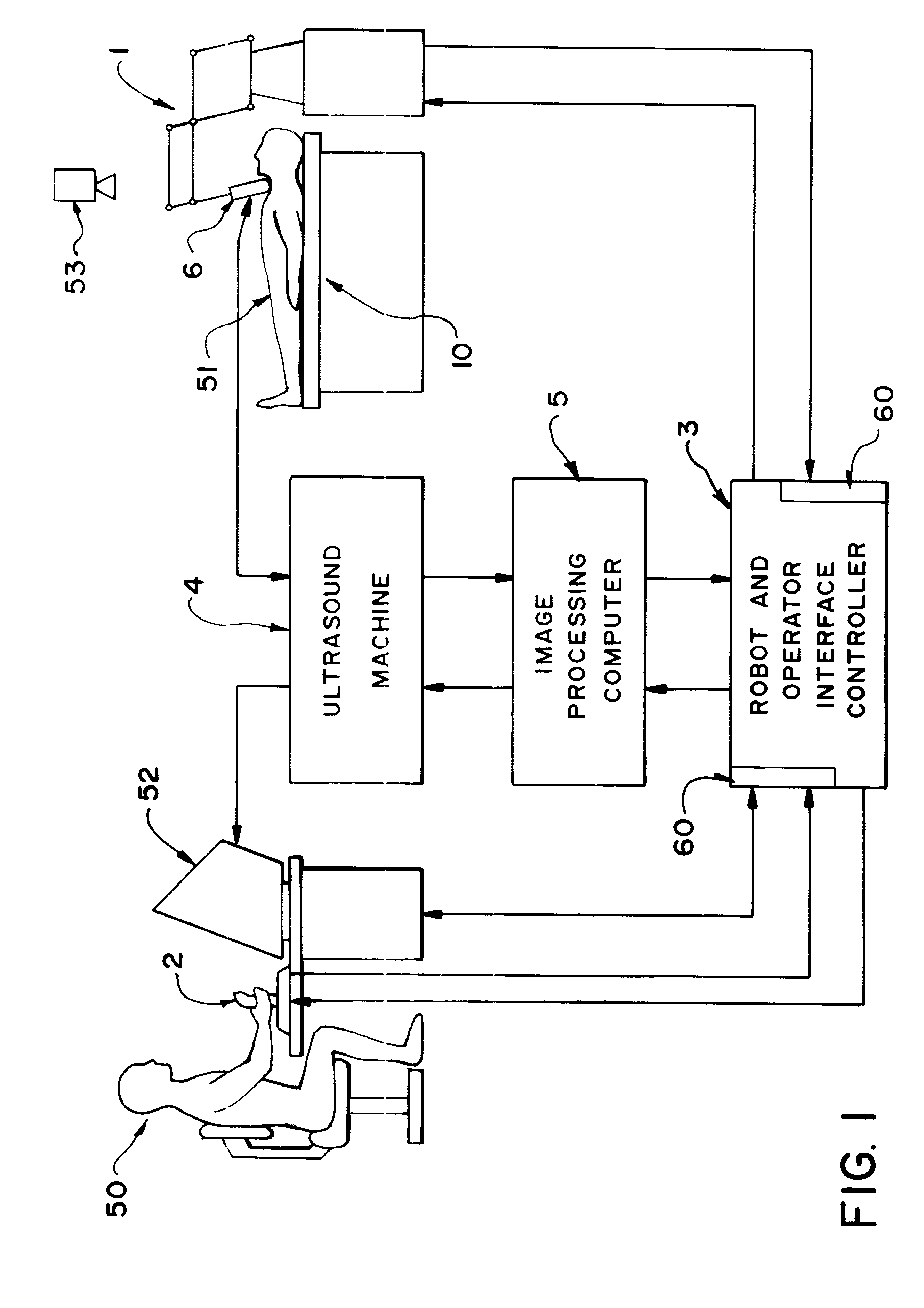
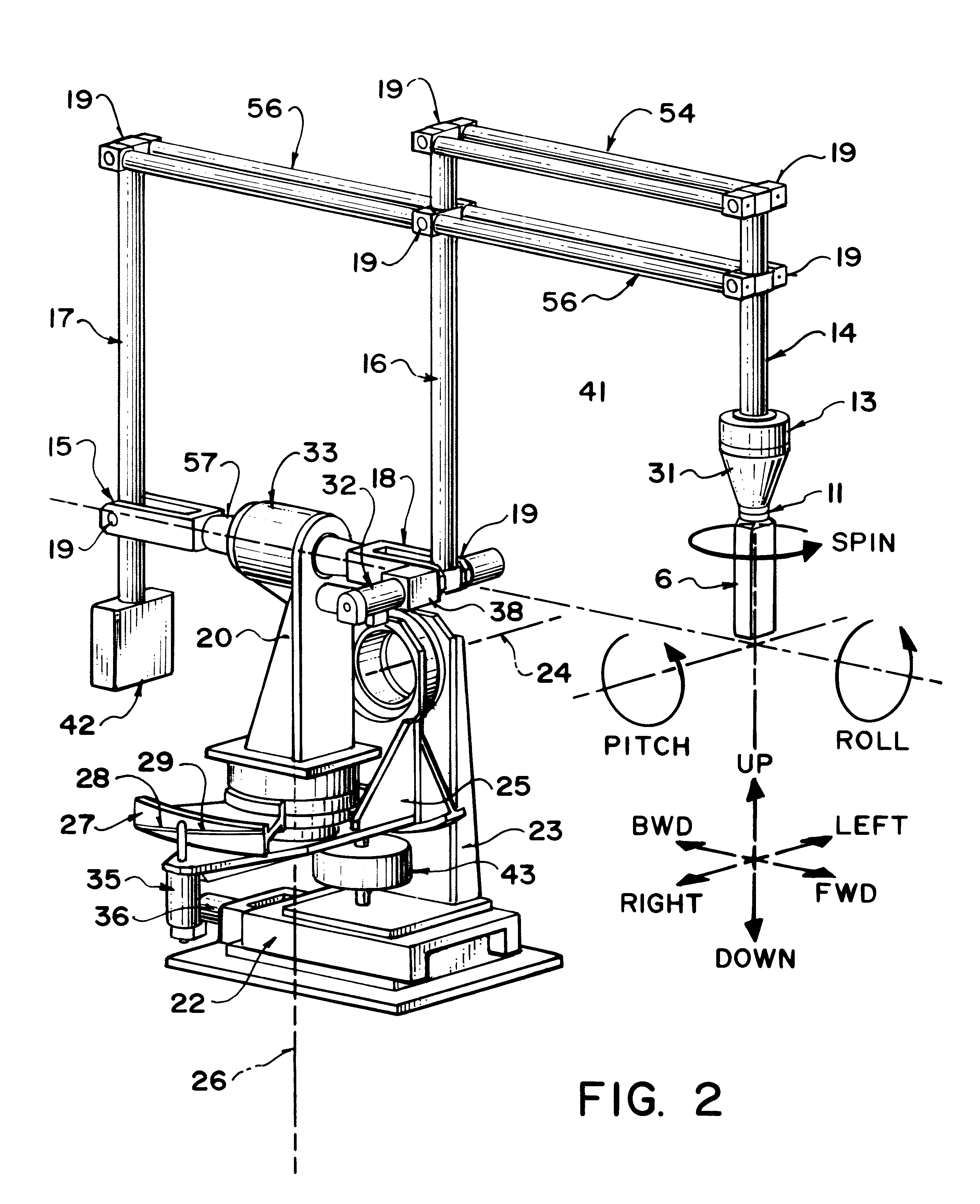
Robotically assisted medical ultrasound
InactiveUS6425865B1Maximize image signal-to-noise ratioMaximize signal to noise ratioBlood flow measurement devicesOrgan movement/changes detectionCo ordinateUltrasound image
A system for medical ultrasound in which the ultrasound probe is positioned by a robot arm under the shared control of the ultrasound operator and the computer is proposed. The system comprises a robot arm design suitable for diagnostic ultrasound, a passive or active hand-controller, and a computer system to co-ordinate the motion and forces of the robot and hand-controller as a function of operator input, sensed parameters and ultrasound images.
Owner:THE UNIV OF BRITISH COLUMBIA
Method and apparatus for registration, verification, and referencing of internal organs
InactiveUS20050182319A1Sufficient informationPrevent material seeping into the deviceAudiometeringCatheterOrgan systemBiomedical engineering
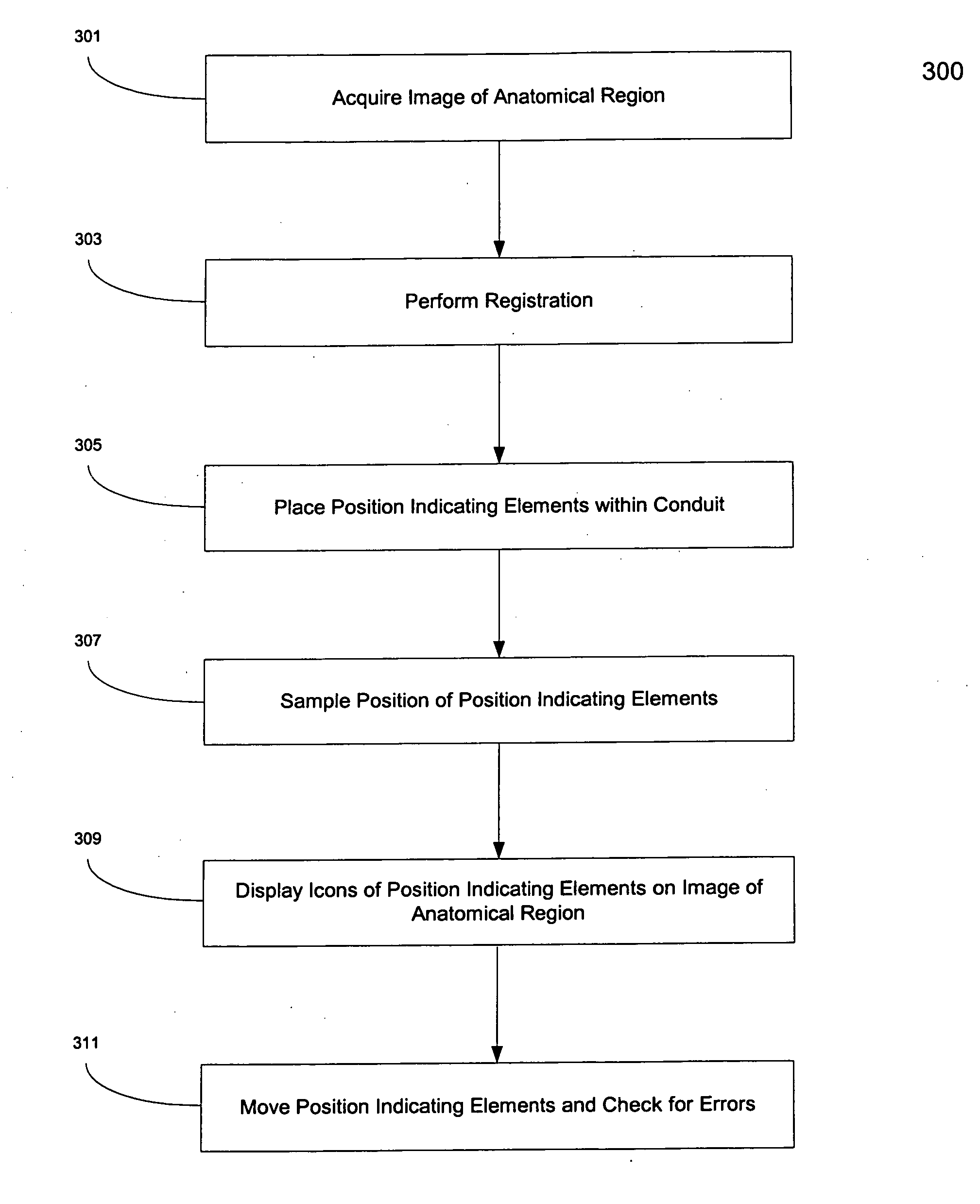
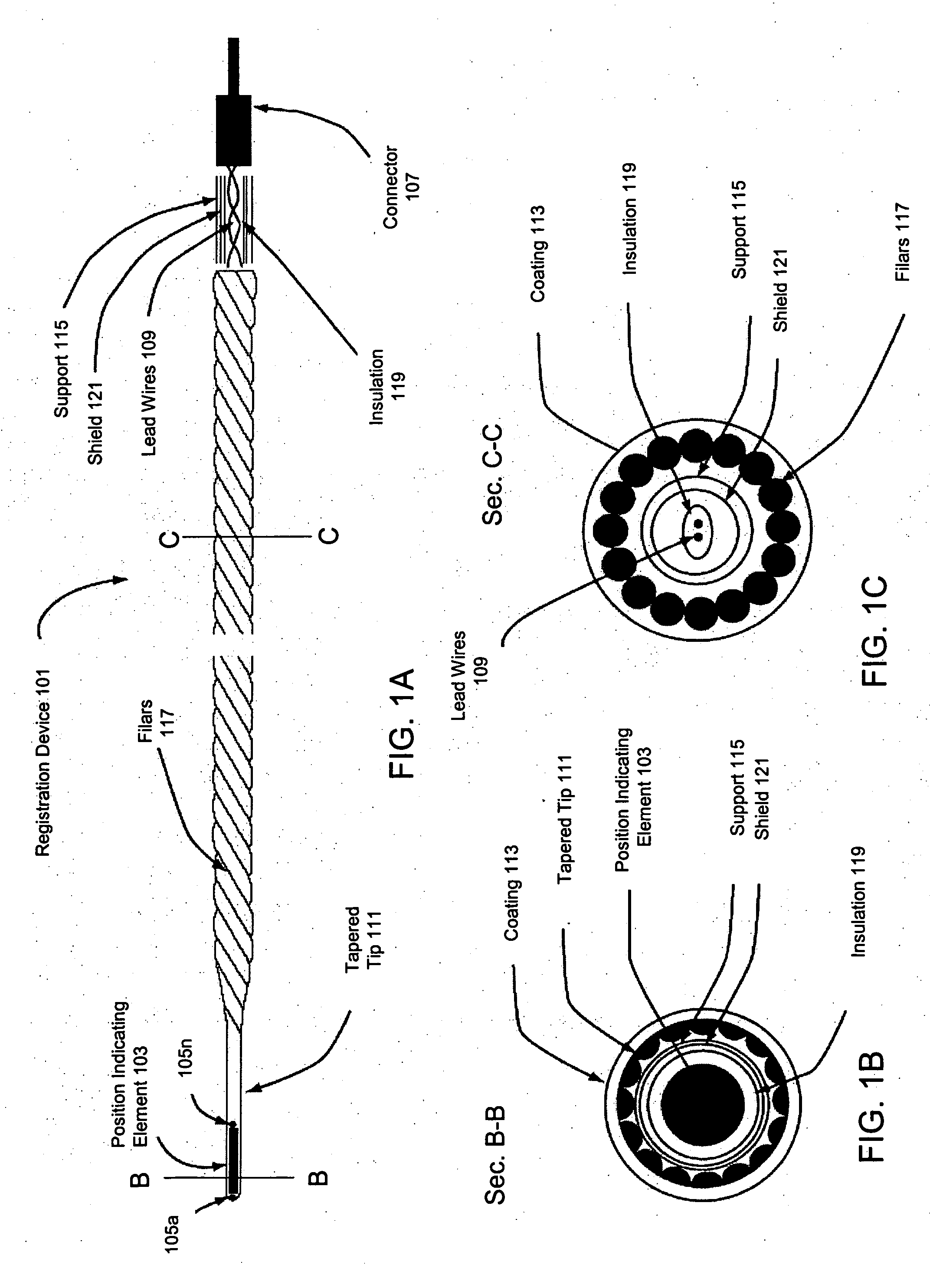
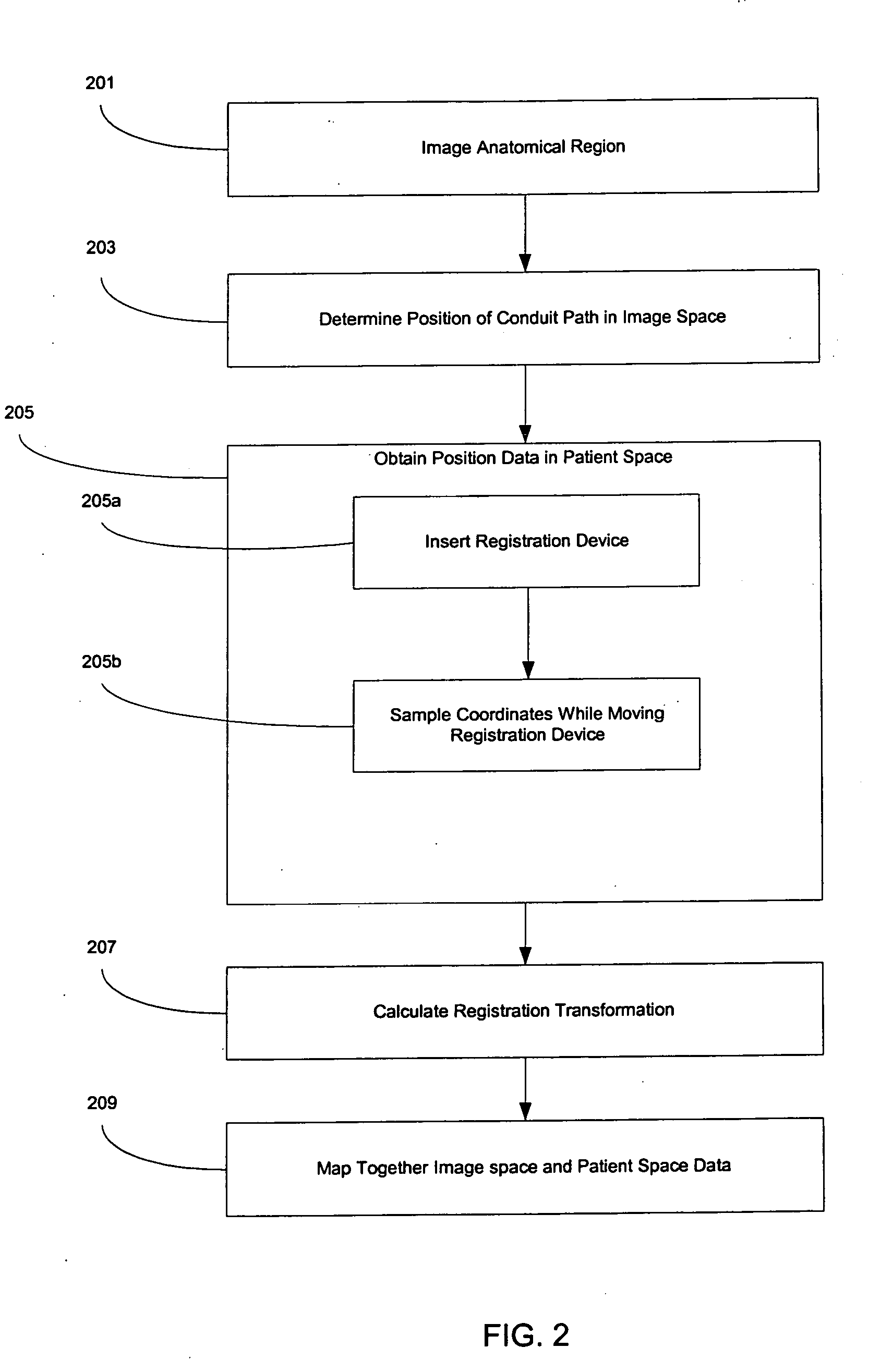
Systems and methods for registering, verifying, dynamically referencing, and navigating an anatomical region of interest of a patient are provided. In one embodiment, the anatomical region of interest is imaged using an imaging device such as, for example, an x-ray device. A tracked registration device may then be removably inserted in a conduit within the anatomical region and the position of the registration device may be sampled by a tracking device as the registration device is moved within the anatomical region through the catheter. The sampled position data is registered to the image data to register the path of the conduit to the anatomical region of interest. The same or a similar device may be used to dynamically reference the movements affecting the anatomical region and modify the registration in real time. The registration may also be verified.
Owner:PHILIPS ELECTRONICS LTD
Systems and methods for making noninvasive physiological assessments
InactiveUS6875176B2Improve accuracySensitive highOrgan movement/changes detectionSurgeryDiseaseNon invasive
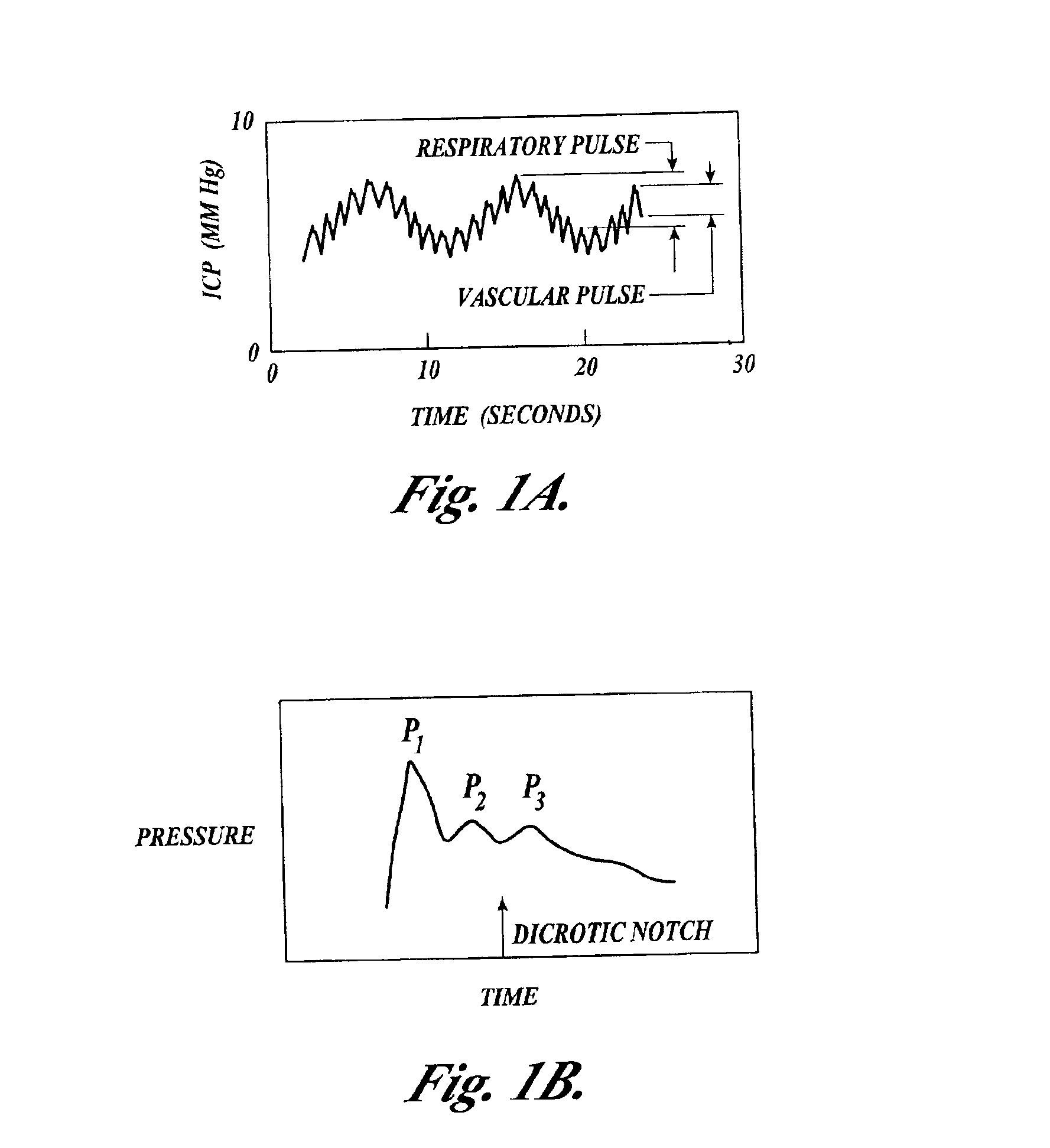
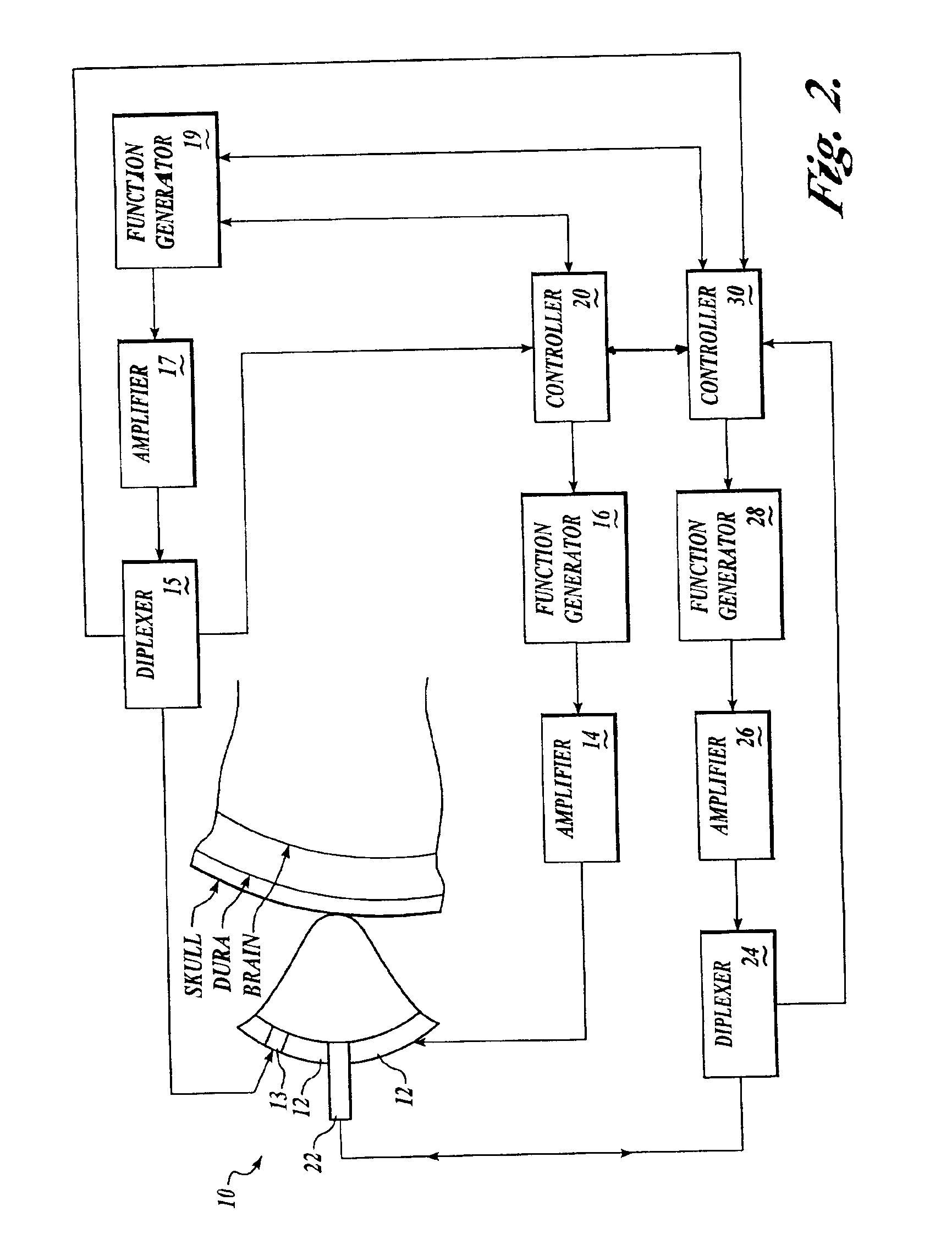
Systems and methods for assessment of tissue properties, noninvasively, by acquiring data relating to at least one aspect of intrinsic and / or induced tissue displacement, or associated biological responses, are provided. Data relating to tissue displacement and associated biological changes may be acquired by detecting acoustic properties of tissue using ultrasound interrogation pulses, preferably in a scatter or Doppler detection mode. Based on this data, tissue properties are assessed, characterized and monitored. Specific applications for systems and methods of the present invention include non-invasive assessment and monitoring of intracranial pressure (ICP), arterial blood pressure (ABP), CNS autoregulation status, vasospasm, stroke, local edema, infection and vasculitus, as well as diagnosis and monitoring of diseases and conditions that are characterized by physical changes in tissue properties. Methods and systems for localizing physiological condition(s) and / or biological response(s), such as pain, by targeting and selectively probing tissues using the application of focused ultrasound are also provided.
Owner:PHYSIOSONICS
Method and apparatus for real time quantitative three-dimensional image reconstruction of a moving organ and intra-body navigation
InactiveUS7343195B2Operating tablesUsing subsonic/sonic/ultrasonic vibration meansImage detectionMedical imaging
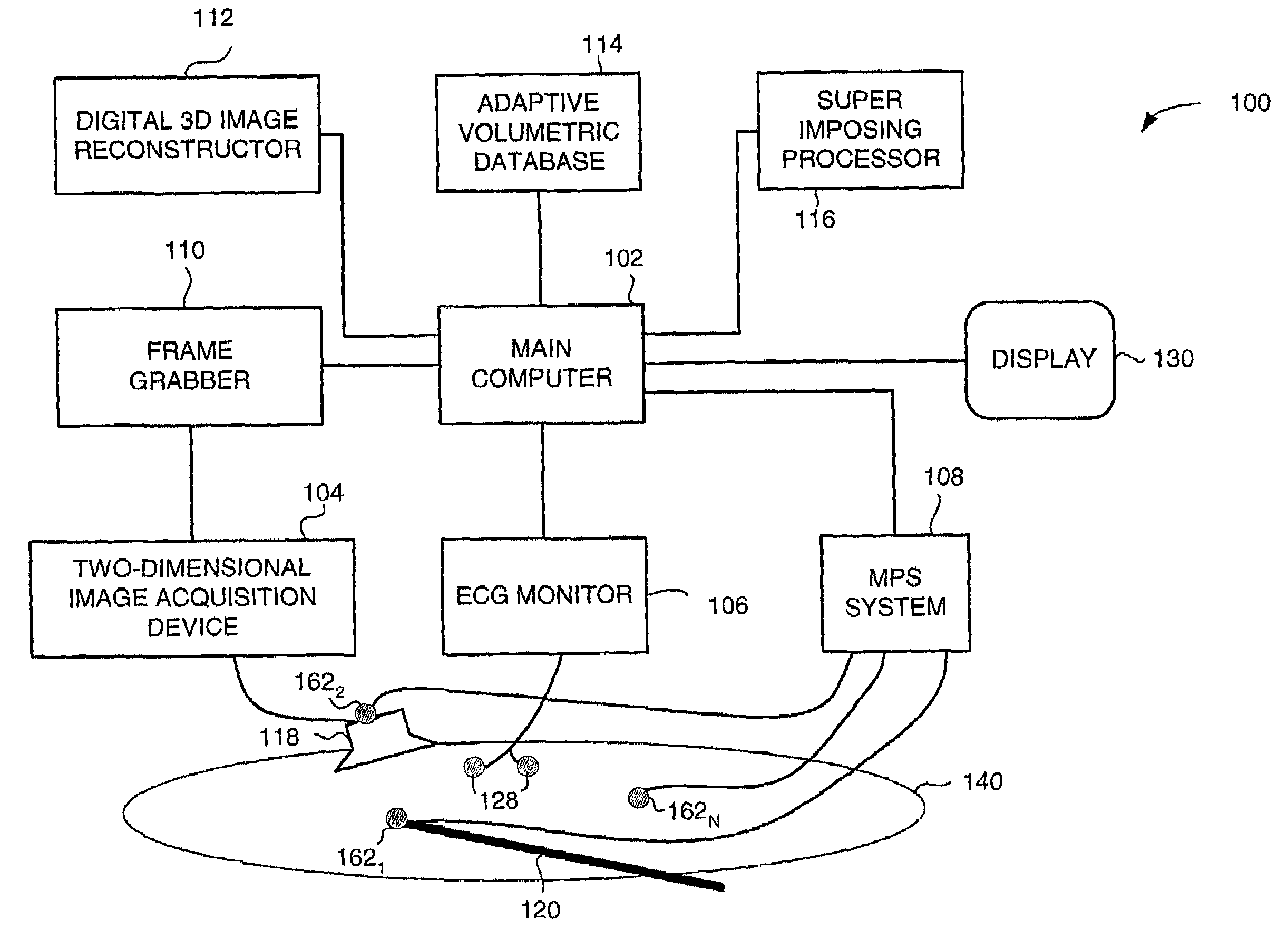
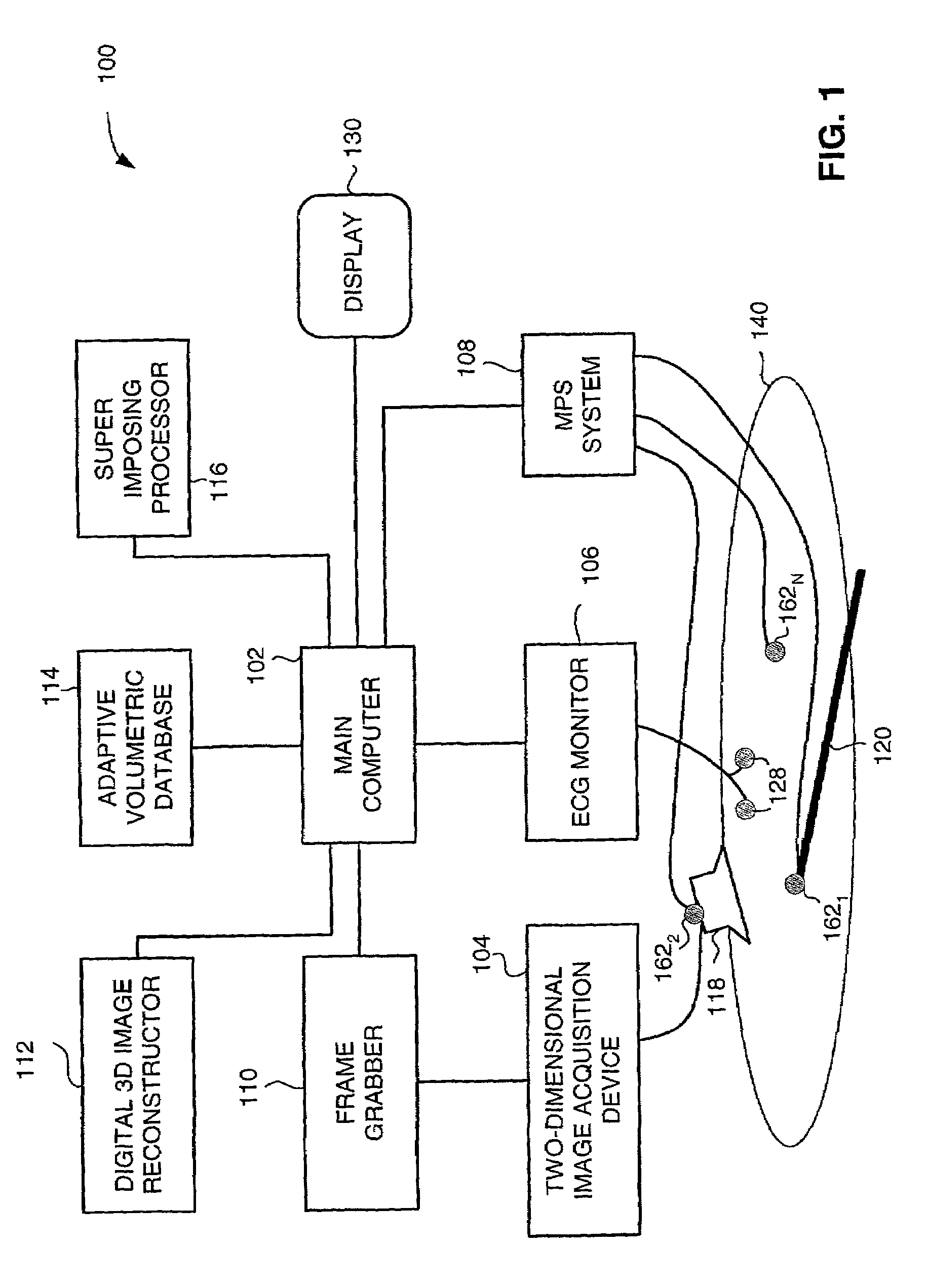
Medical imaging and navigation system including a processor, a medical positioning system (MPS), a two-dimensional imaging system and an inspected organ monitor interface, the MPS including an imaging MPS sensor, the two-dimensional imaging system including an image detector, the processor being coupled to a display unit and to a database, the MPS being coupled to the processor, the imaging MPS sensor being firmly attached to the image detector, the two-dimensional imaging system being coupled to the processor, the image detector being firmly attached to an imaging catheter.
Owner:ST JUDE MEDICAL INT HLDG SARL
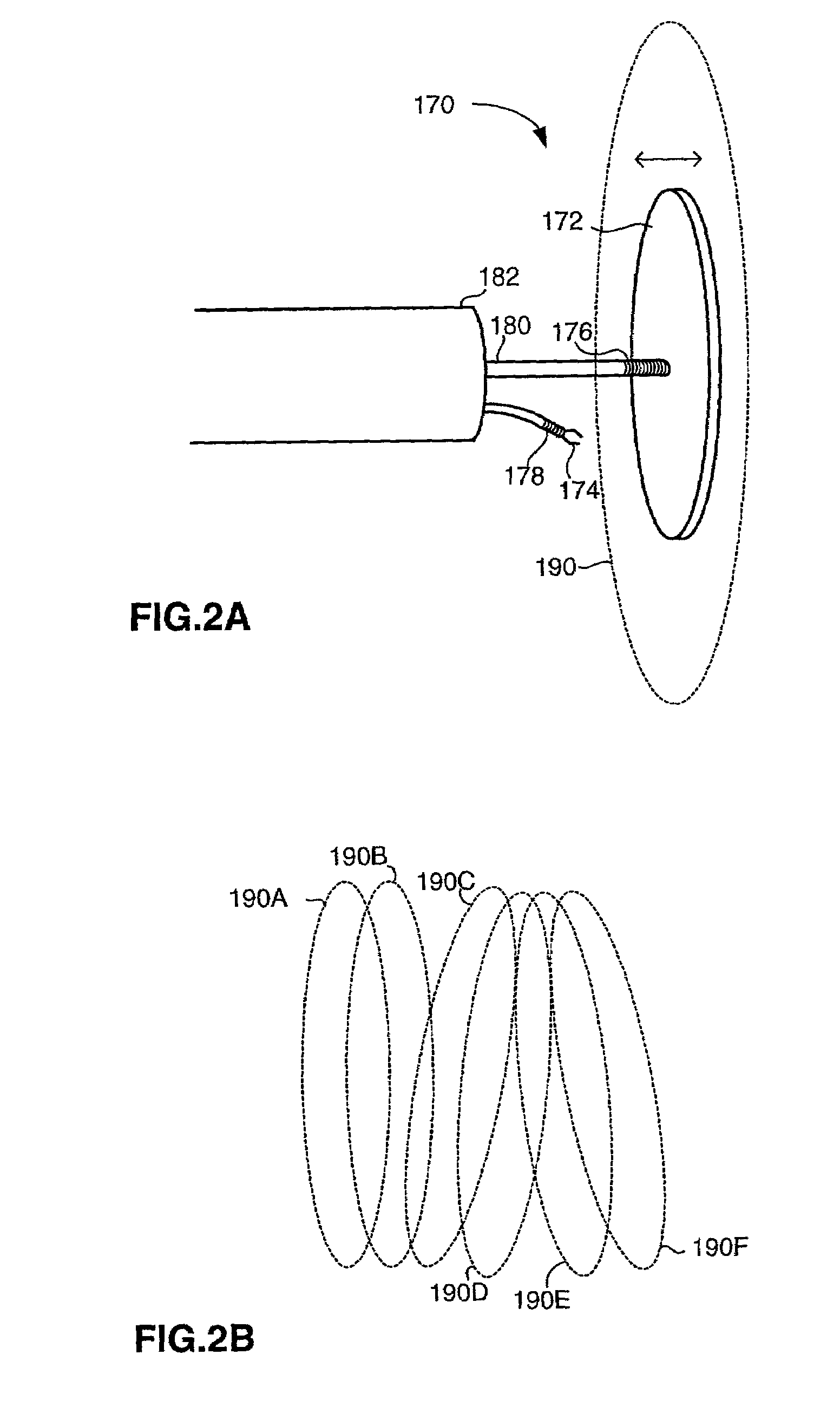
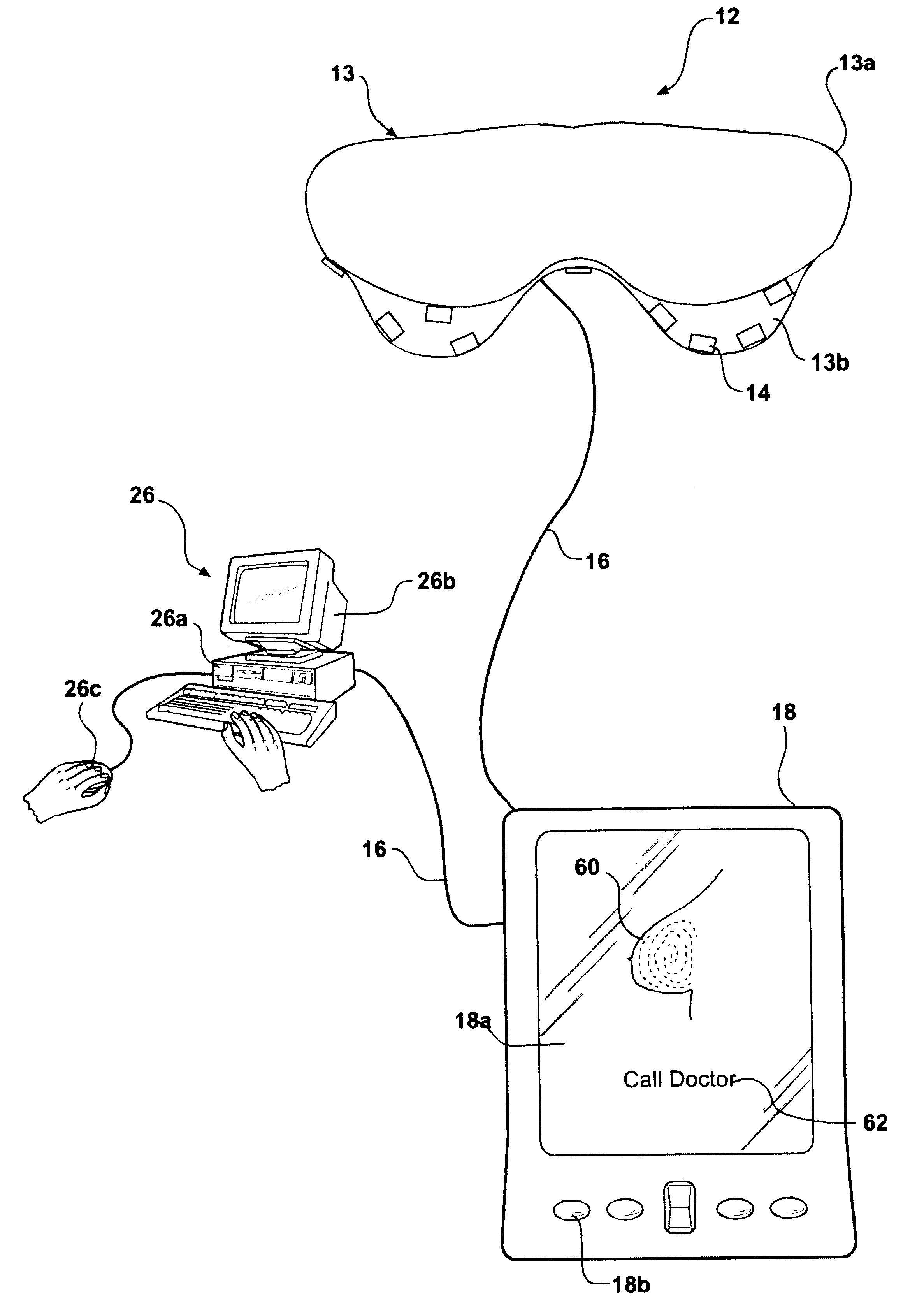
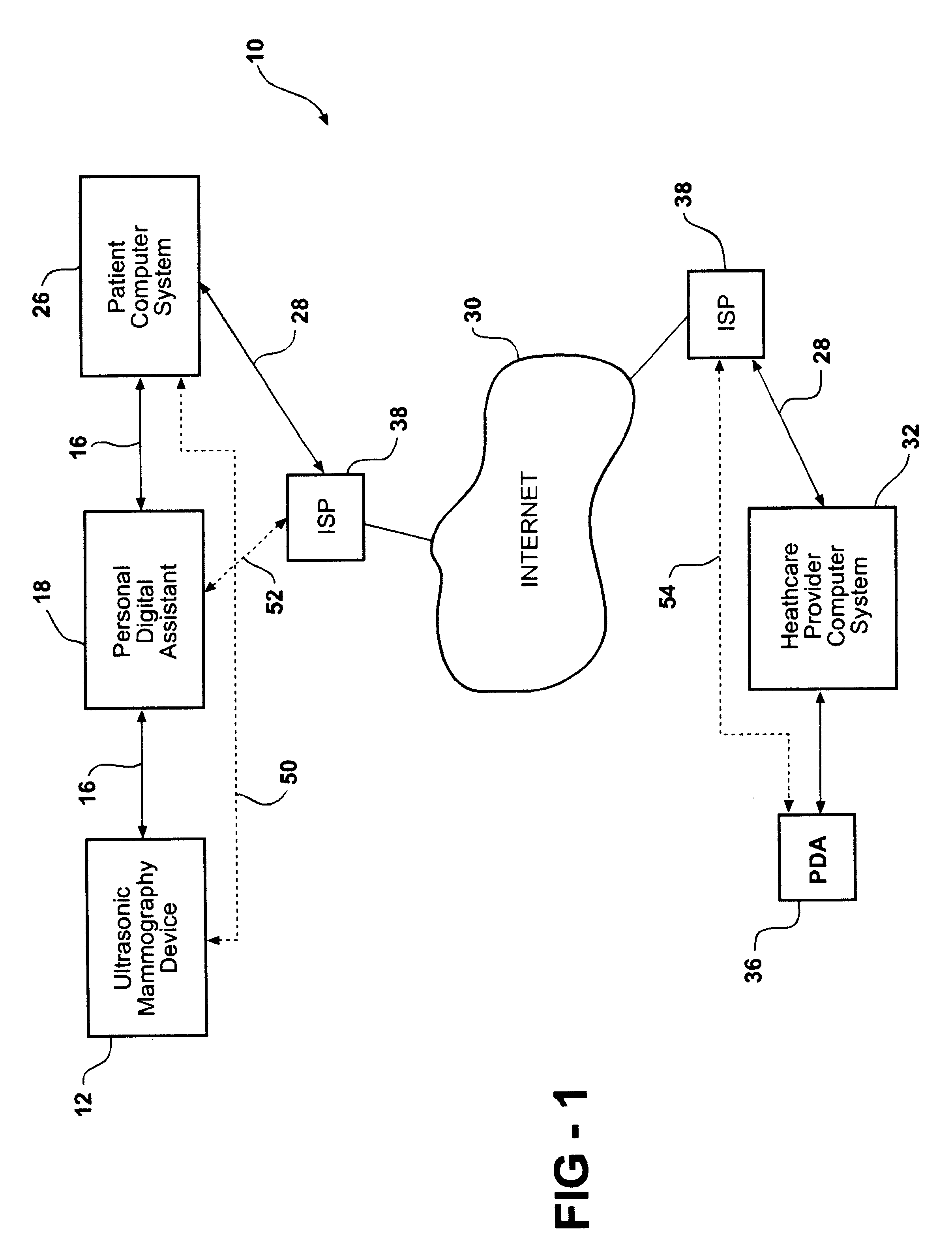
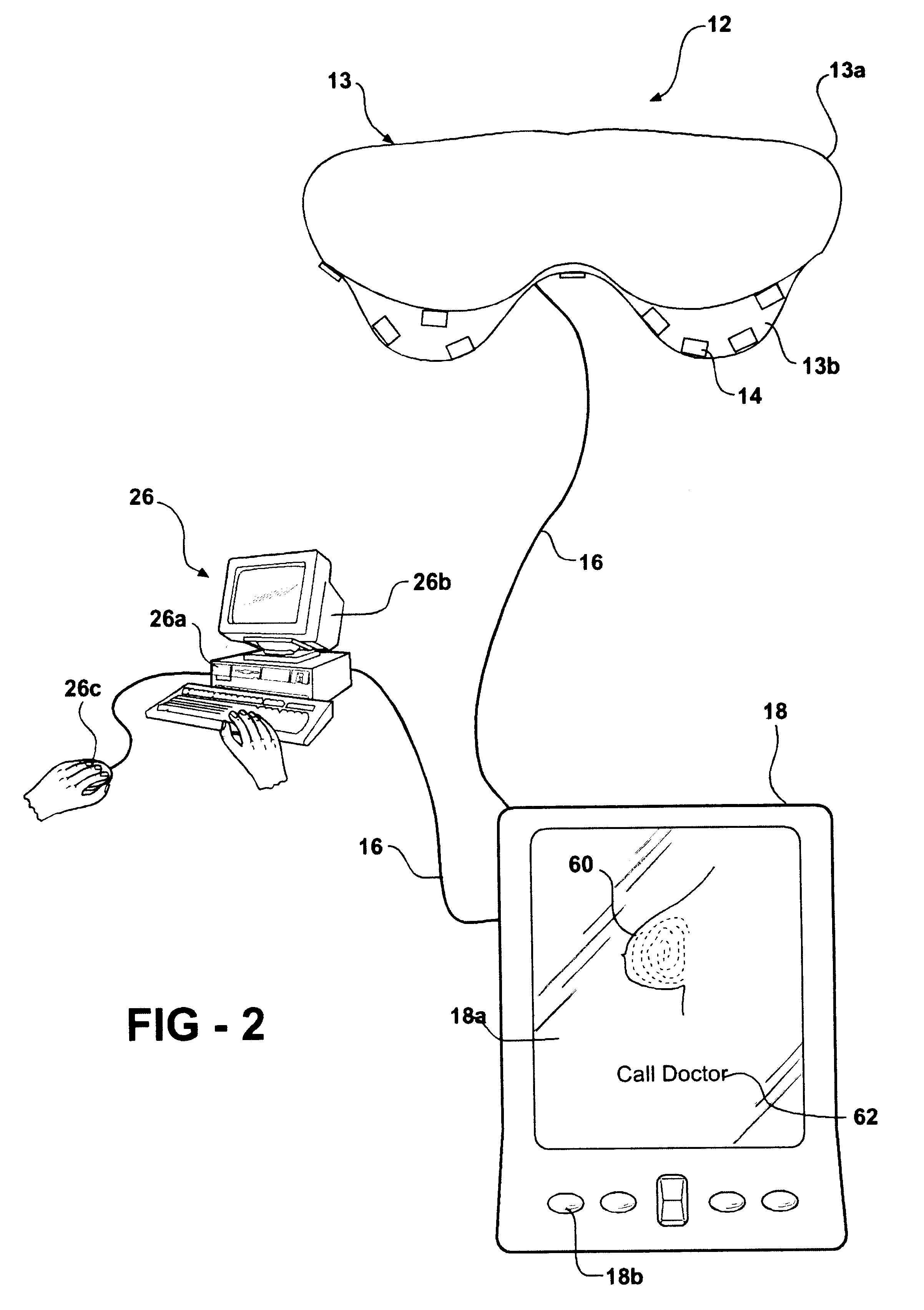
System and method of ultrasonic mammography
Owner:MICROLIFE MEDICAL HOME SOLUTIONS
Method and Apparatus for Monitoring Fluid Content within Body Tissues
InactiveUS20100234716A1Improve accuracy and reliabilityHydration of the target tissue can be determinedElectrocardiographyOrgan movement/changes detectionUltrasonic sensorBody tissue
Methods and devices for monitoring fluid content within body tissues. An adherent device having a support configured to transmit a signal into a body of a patient, and receive a reflected portion of the signal, and adhere to the skin of the patient. In many embodiments, the adherent device includes an ultrasonic transducer and other sensors. In many embodiments, the ultrasonic transducer is used in coordination with the other sensors to predict a cardiac decompensation.
Owner:MEDTRONIC MONITORING
Surgical navigation systems including reference and localization frames
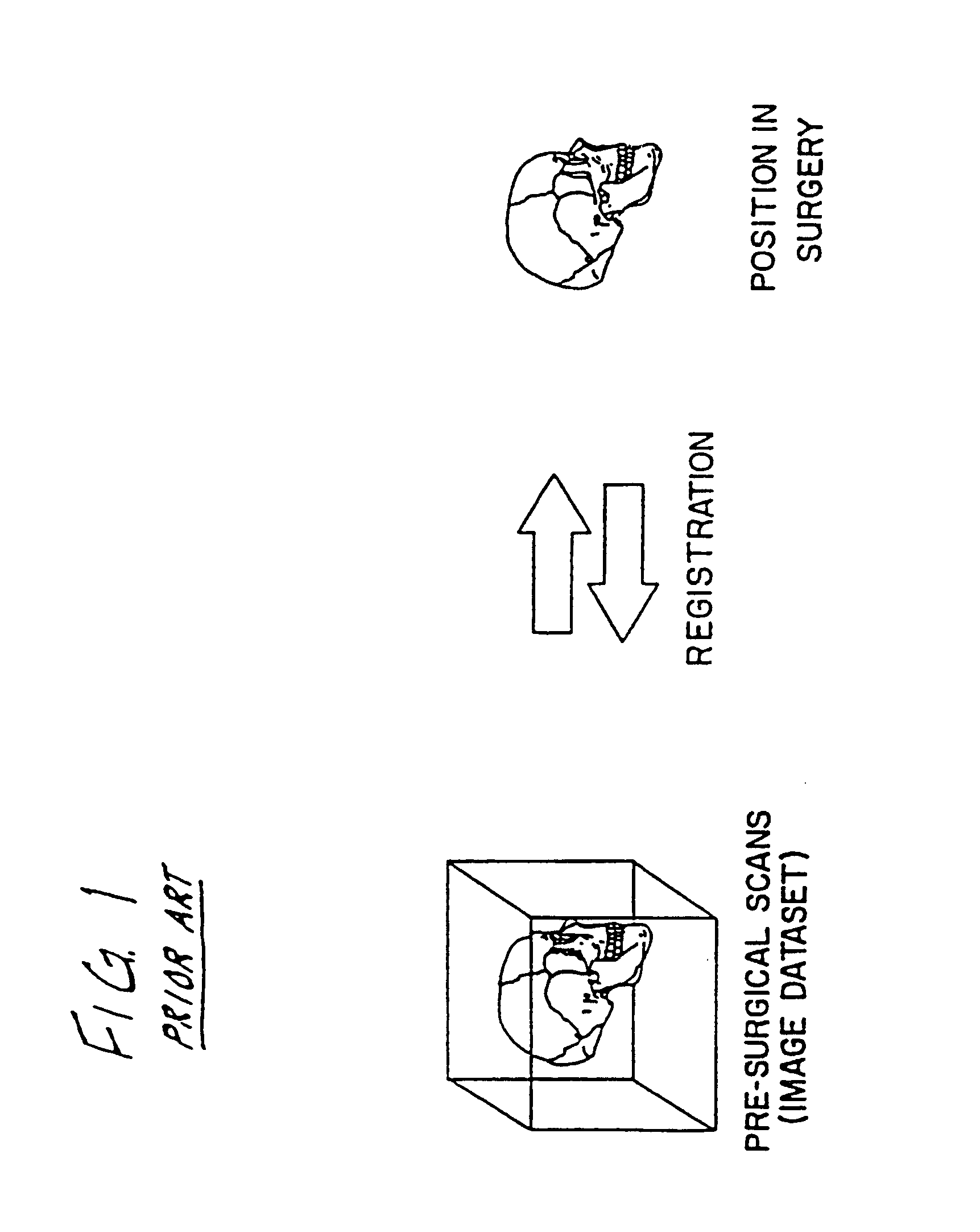
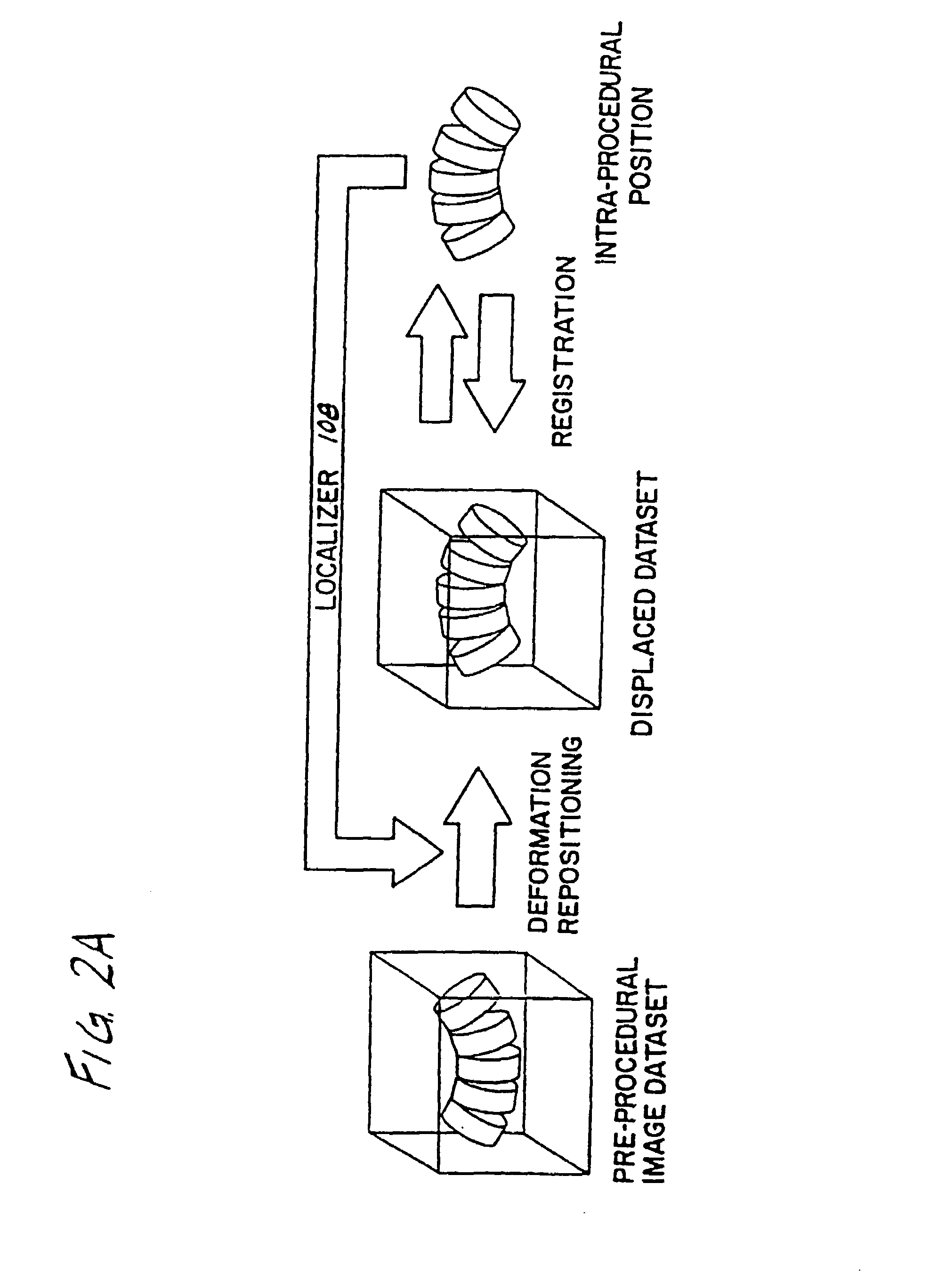
A system for use during a medical or surgical procedure on a body. The system generates an image representing the position of one or more body elements during the procedure using scans generated by a scanner prior or during the procedure. The image data set has reference points for each of the body elements, the reference points of a particular body element having a fixed spatial relation to the particular body element. The system includes an apparatus for identifying, during the procedure, the relative position of each of the reference points of each of the body elements to be displayed. The system also includes a processor for modifying the image data set according to the identified relative position of each of the reference points during the procedure, as identified by the identifying apparatus, said processor generating a displaced image data set representing the position of the body elements during the procedure. The system also includes a display utilizing the displaced image data set generated by the processor, illustrating the relative position of the body elements during the procedure. Methods relating to the system are also disclosed. Also disclosed are devices for use with a surgical navigation system having a sensor array which is in communication with the device to identify its position. The device may be a reference frame for attachment of a body part of the patient, such as a cranial reference arc frame for attachment to the head or a spine reference arc frame for attachment to the spine. The device may also be a localization frame for positioning an instrument relative to a body part, such as a localization biopsy guide frame for positioning a biopsy needle, a localization drill guide assembly for positioning a drill bit, a localization drill yoke assembly for positioning a drill, or a ventriculostomy probe for positioning a catheter.
Owner:SURGICAL NAVIGATION TECH +1
Segmentation and registration of multimodal images using physiological data
InactiveUS20070049817A1Improve accuracyMore rapidImage enhancementImage analysisComputer visionData system
Systems and methods are provided for registering maps with images, involving segmentation of three-dimensional images and registration of images with an electro-anatomical map using physiological or functional information in the maps and the images, rather than using only location information. A typical application of the invention involves registration of an electro-anatomical map of the heart with a preacquired or real-time three-dimensional image. Features such as scar tissue in the heart, which typically exhibits lower voltage than healthy tissue in the electro-anatomical map, can be localized and accurately delineated on the three-dimensional image and map.
Owner:BIOSENSE WEBSTER INC
Method and apparatus for safety delivering medicants to a region of tissue using imaging, therapy and temperature monitoring ultrasonic system
A method and apparatus for controlling the safe delivery of thermosensitive liposomes containing medicant to a targeted tissue region using ultrasound. Thermosensitive liposomes containing medicants are delivered to a region of interest, the region of interest is located using ultrasound imaging, ultrasound therapy is applied to heat the region of interest, and the temperature of the region is monitored to determine whether a designated threshold temperature has been reached which allows for the release of medicants from the liposomes. If the threshold temperature is reached, and the liposomes are melted, the treatment stops. If the threshold temperature has not been reached, the application of ultrasound therapy and ultrasound imaging are alternated until the threshold temperature is reached. The ultrasound imaging, temperature monitoring and ultrasound therapy are preferably performed with a single transducer.
Owner:GUIDED THERAPY SYSTEMS LLC
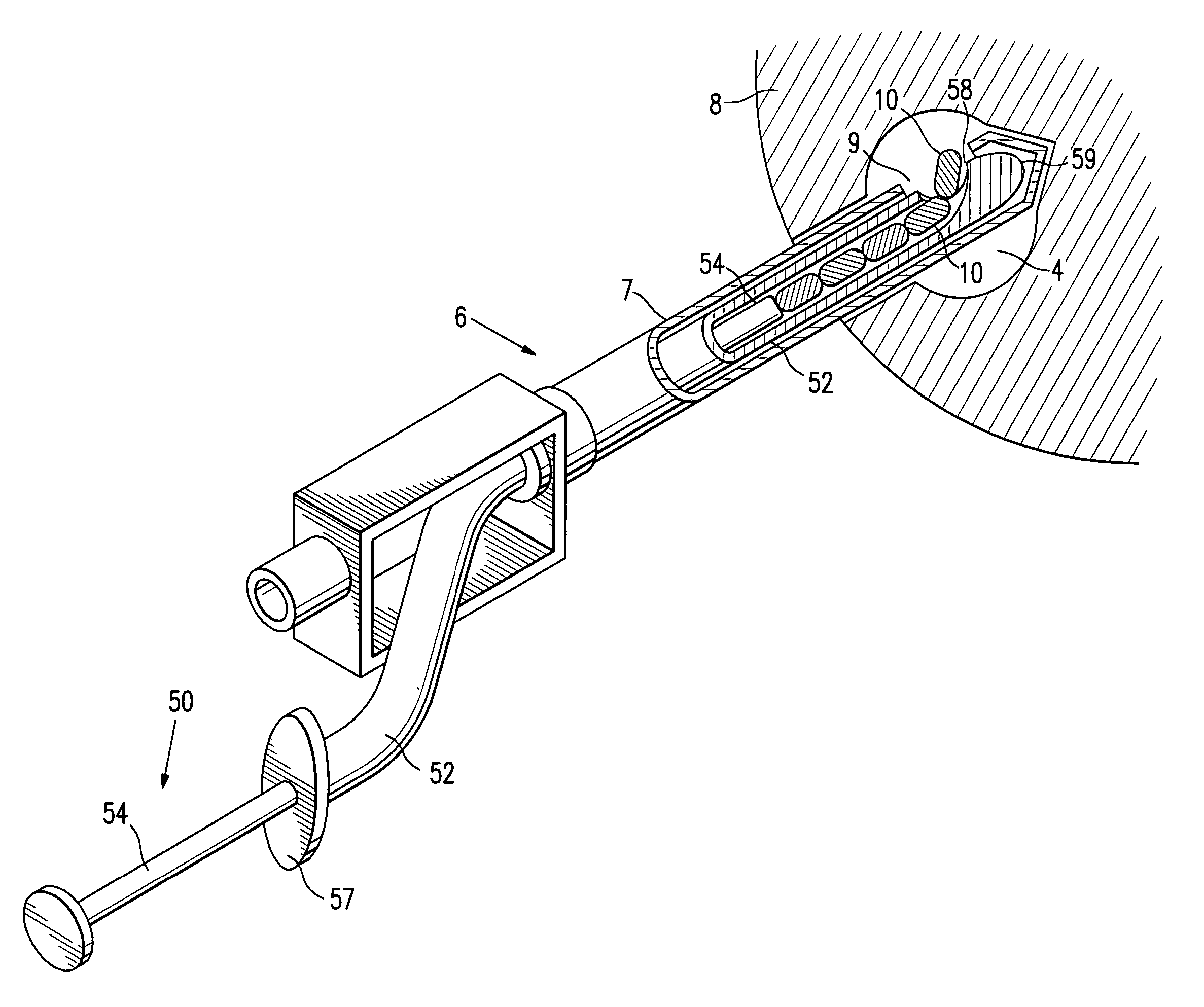
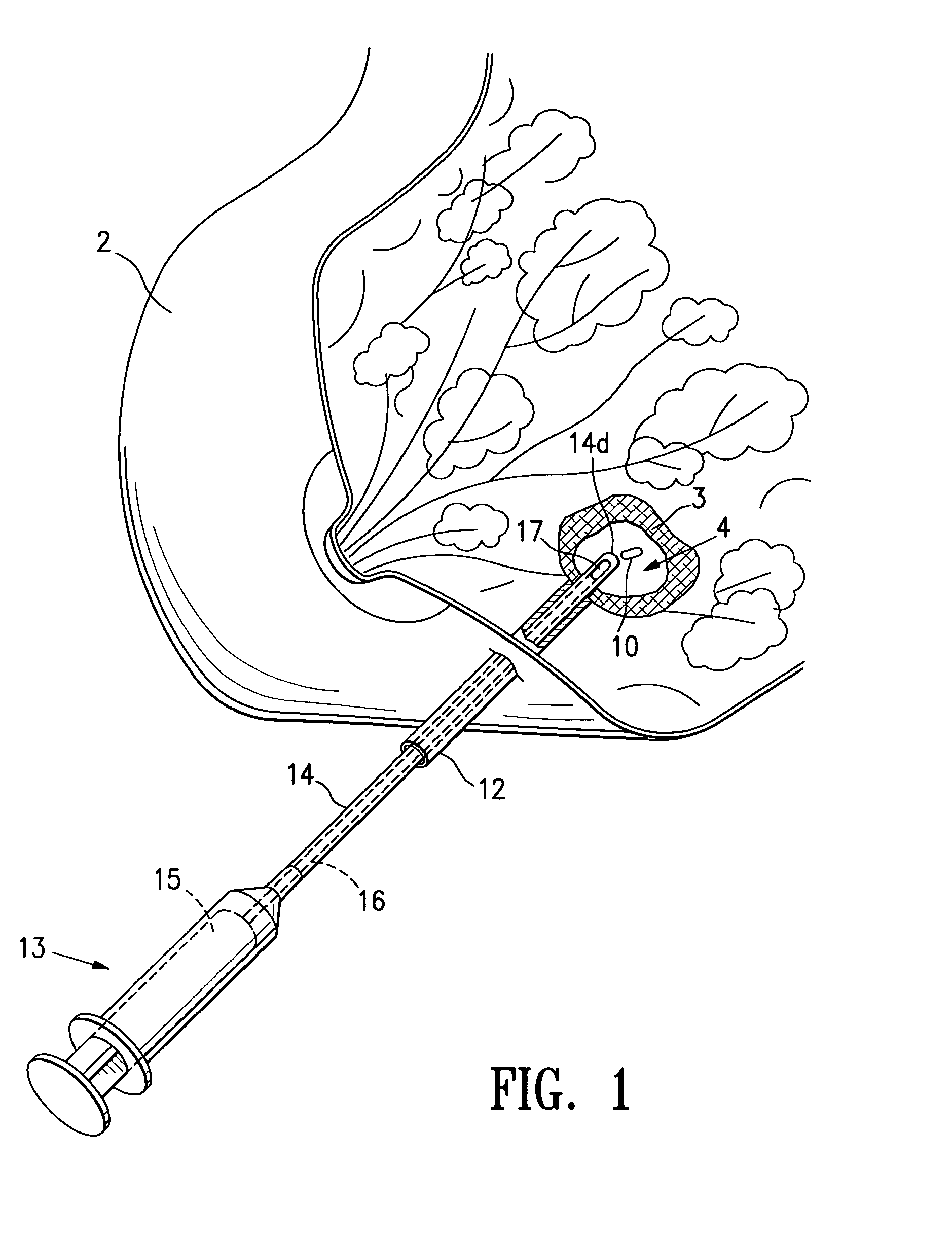
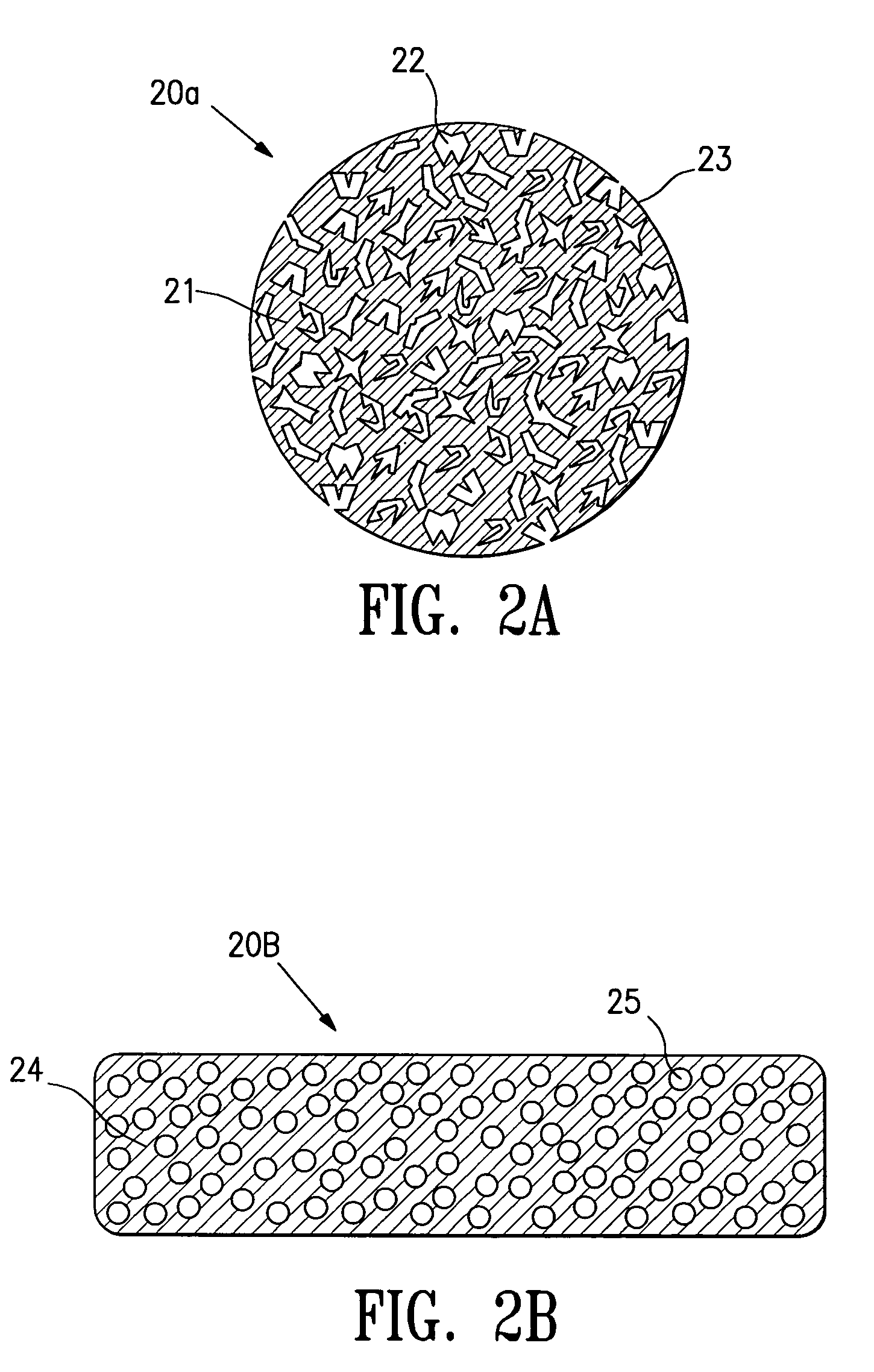
Tissue site markers for in vivo imaging
InactiveUS6993375B2Enhance acoustical reflective signature and signalEasy to detectLuminescence/biological staining preparationSurgical needlesContrast levelIn vivo
Owner:SENORX
Method and apparatus for sensing body gesture, posture and movement
InactiveUS6984208B2Less discomfortProvide usageOrgan movement/changes detectionPerson identificationBody positionsPostural orientation
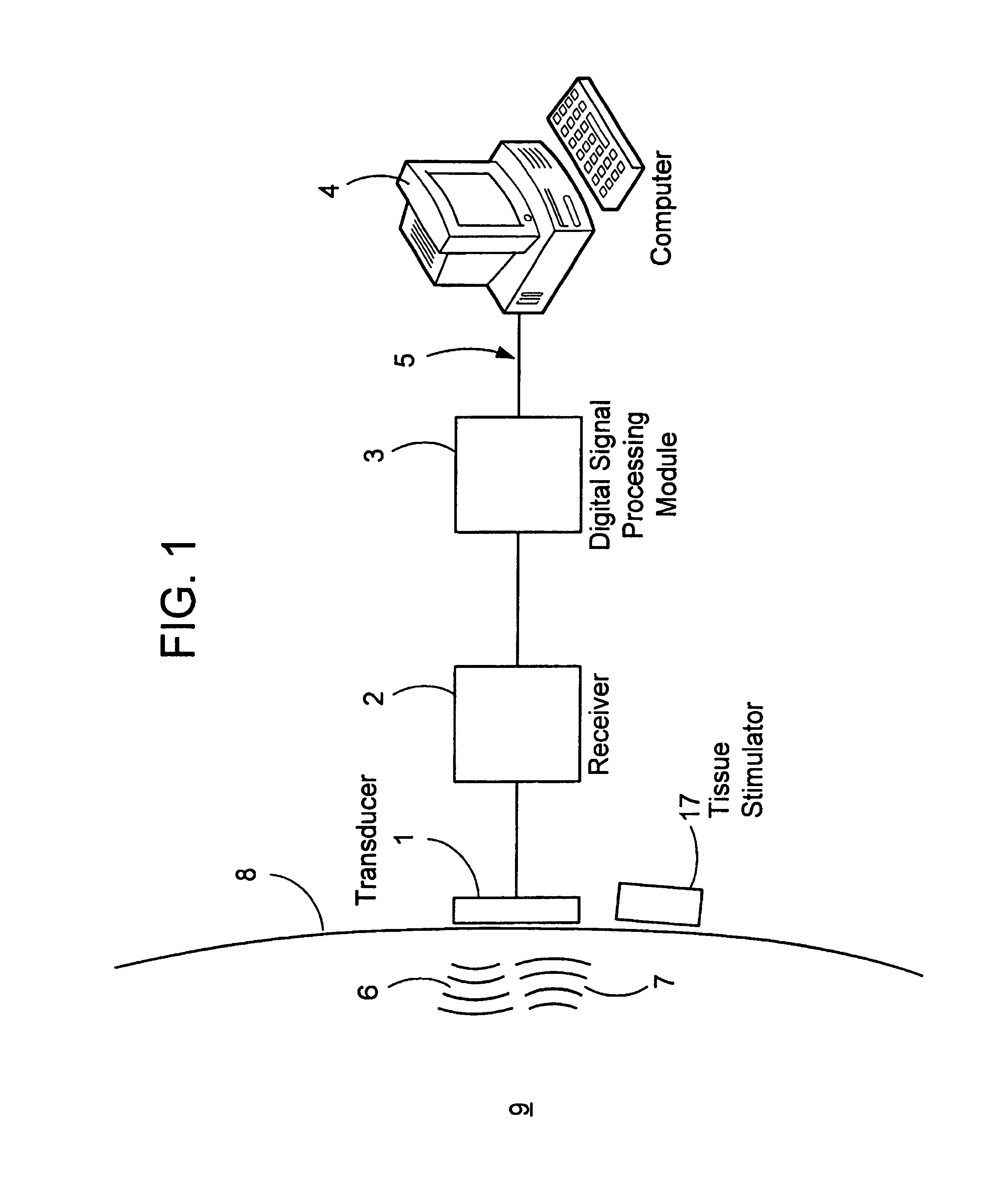
A method for indirectly assessing the gesture, posture or movement of a body part of a person includes transmitting an ultrasound signal into the soft tissue, particularly the muscle, of body part and manipulating the reflected ultrasound signal to obtain parameter data. The parameter data is compared to reference information to obtain gesture, posture or movement information for the body part. Apparatus includes an ultrasound transmitter and receiver for transmitting, a signal processor, and a processor for storing reference information and determining gesture, posture or movement information for the body part.
Owner:THE HONG KONG POLYTECHNIC UNIV
Electric tomography
Methods for evaluating motion of a tissue, such as of a cardiac location, e.g., heart wall, via electrical field tomography are provided. In the subject methods, an sensing element is stably associated with a tissue location of interest. Signals obtained from the sensing element are obtained to evaluate movement of the tissue location. Also provided are systems and devices for practicing the subject methods. In addition, innovative data displays and systems for producing the same are provided. The subject methods and devices find use in a variety of different applications, including cardiac resynchronization therapy.
Owner:PROTEUS DIGITAL HEALTH INC
User interface for handheld imaging devices
InactiveUS7022075B2Minimize timeEasy to distinguishLocal control/monitoringBlood flow measurement devicesData displayUltrasonography
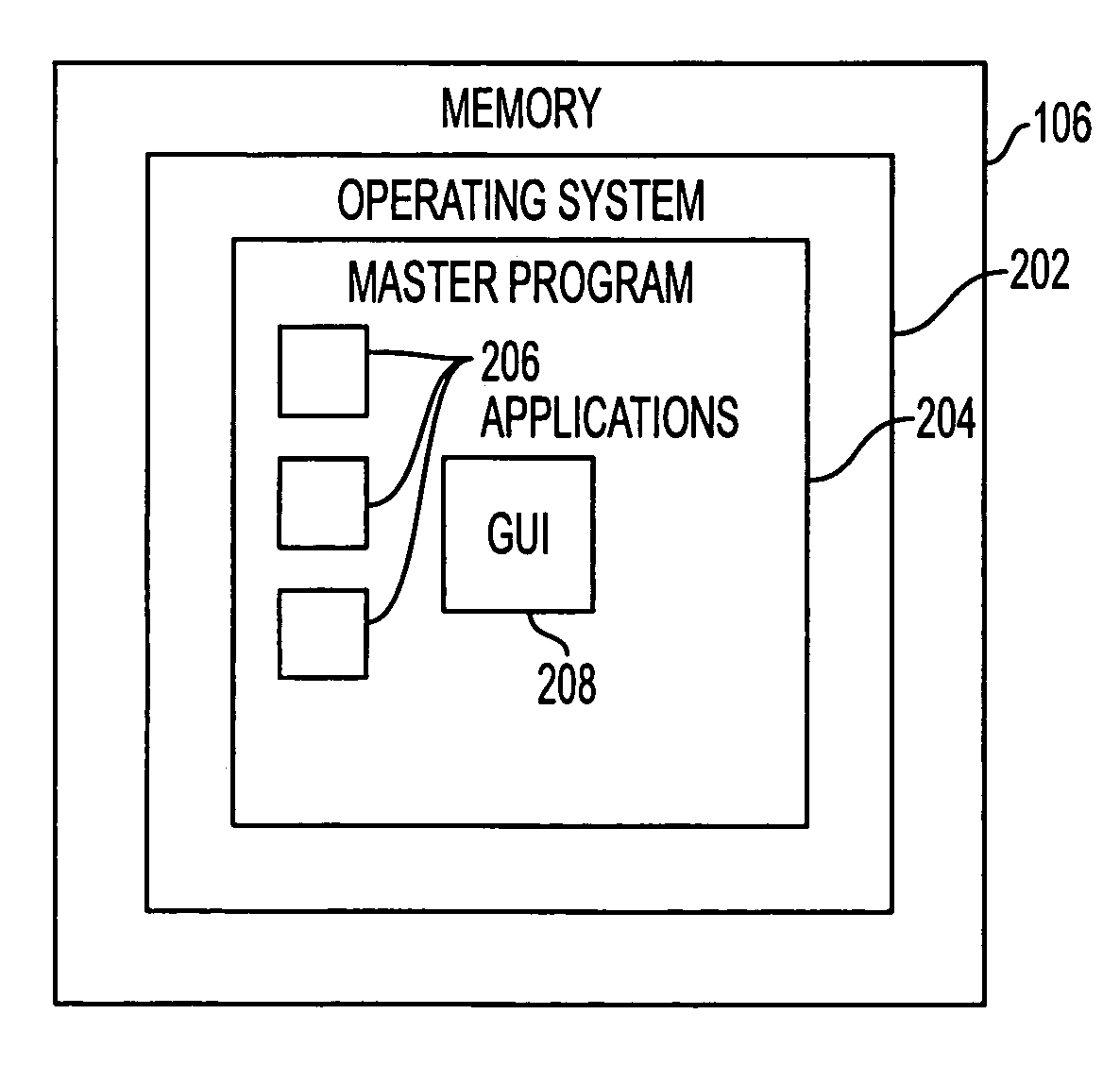
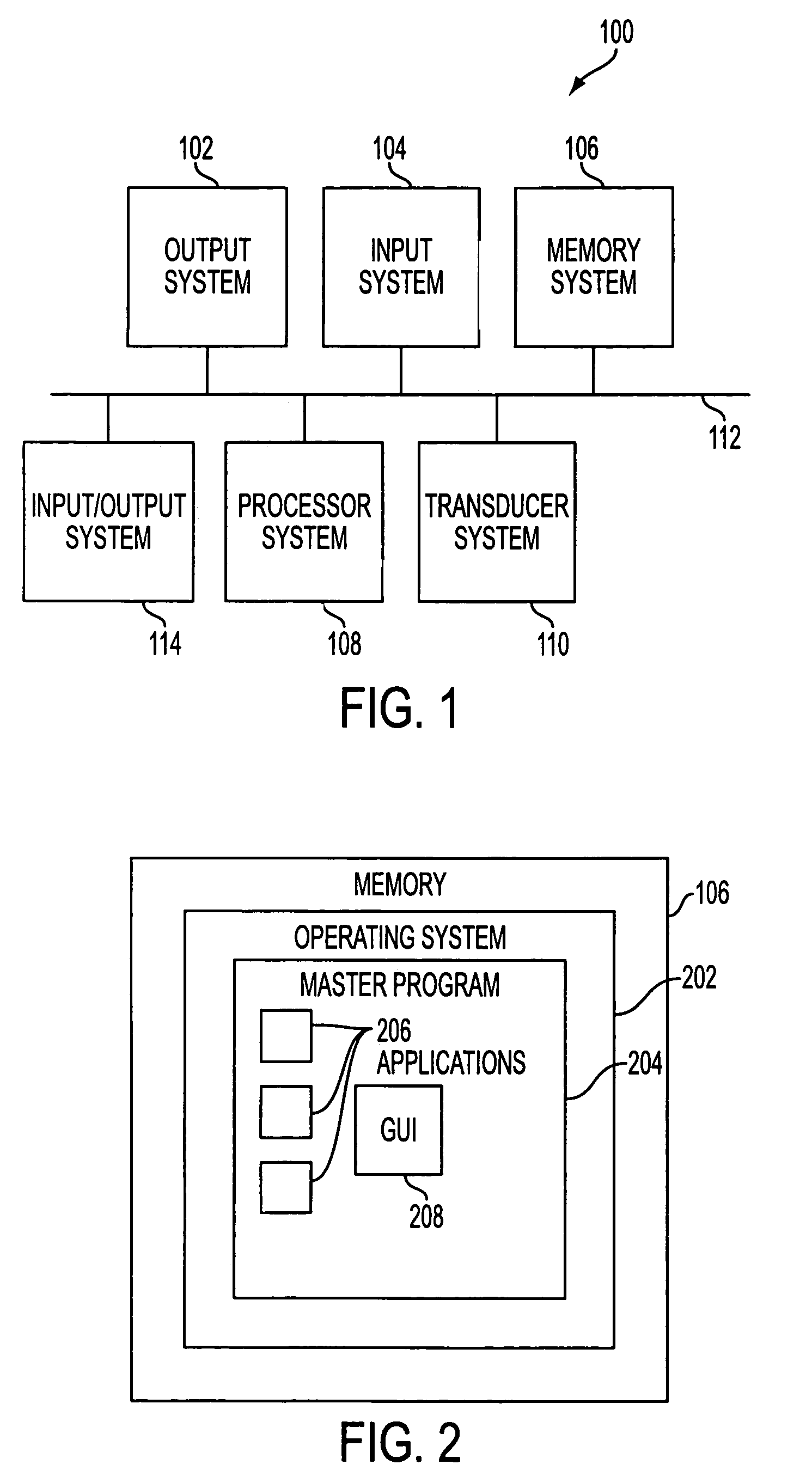
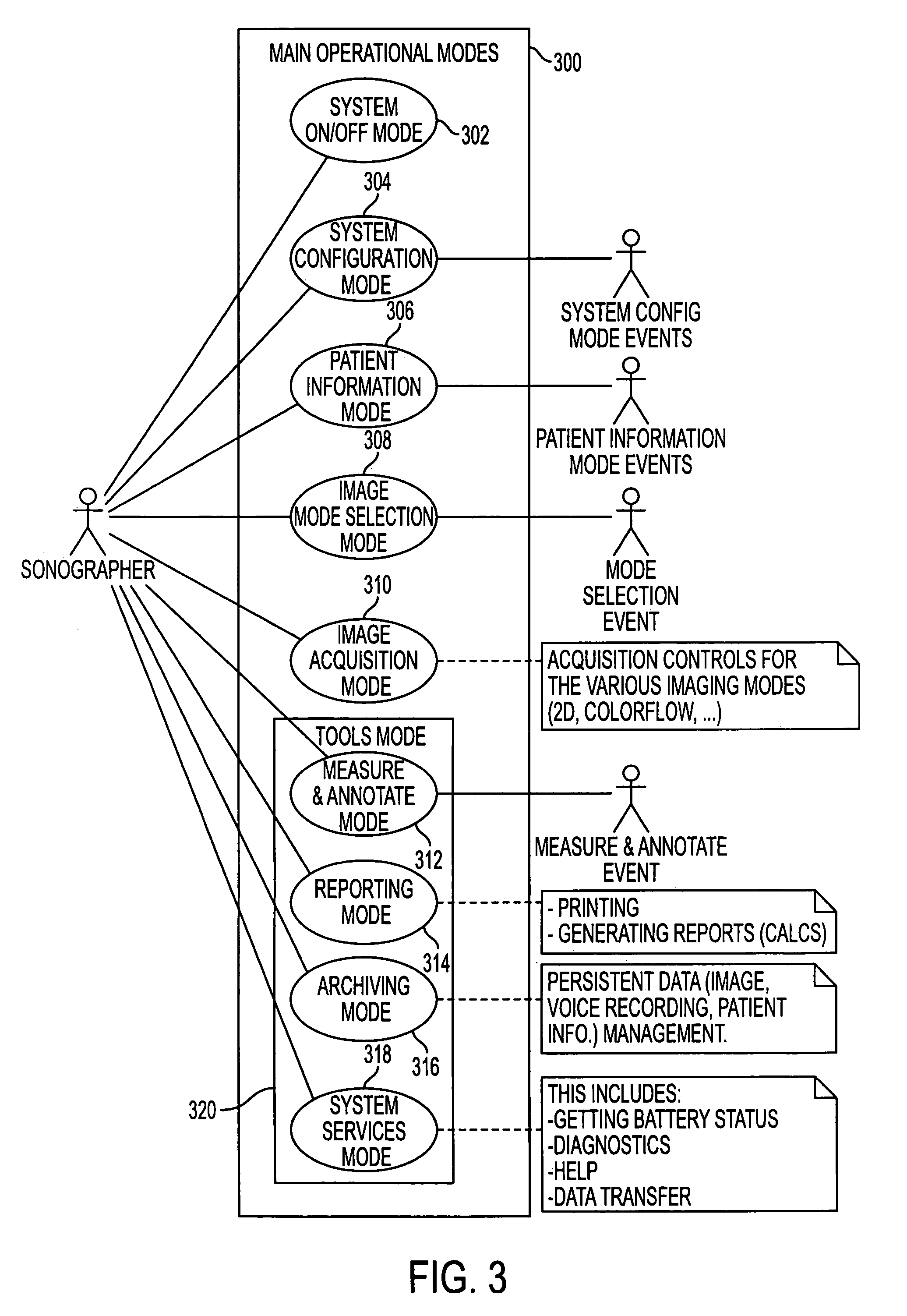
A Graphical User Interface (GUI) for an ultrasound system. The ultrasound system has operational modes and the GUI has corresponding icons, tabs, and menu items image and information fields. The User Interface (UI) provides several types of graphical elements with intelligent behavior, such as being context sensitive and adaptive, called active objects, for example, tabs, menus, icons, windows of user interaction and data display and an alphanumeric keyboard. In addition the UI may also be voice activated. The UI further provides for a touchscreen for direct selection of displayed active objects. In an embodiment, the UI is for a medical ultrasound handheld imaging instrument. The UI provides a limited set of hard and soft keys with adaptive functionality that can be used with only one hand and potentially with only one thumb.
Owner:SHENZHEN MINDRAY BIO MEDICAL ELECTRONICS CO LTD
User interface for remote control of medical devices
InactiveUS20060025679A1Diagnostic recording/measuringSurgical manipulatorsRemote controlDisplay device
An interface for remotely controlling a medical device in a patient's body provides a two dimensional display of a three dimensional rendering of the operating region, and allows the user to select the orientation or location of the distal end of the medical device on the display and then operate a navigation system to cause the distal end of the medical device to approximately assume the selected orientation or location.
Owner:STEREOTAXIS
Pulsed cavitational ultrasound therapy
ActiveUS20080319356A1Improve drug deliveryEasy to transportOrgan movement/changes detectionSurgerySonificationMicrobubbles
Owner:RGT UNIV OF MICHIGAN
Portable integrated physiological monitoring system
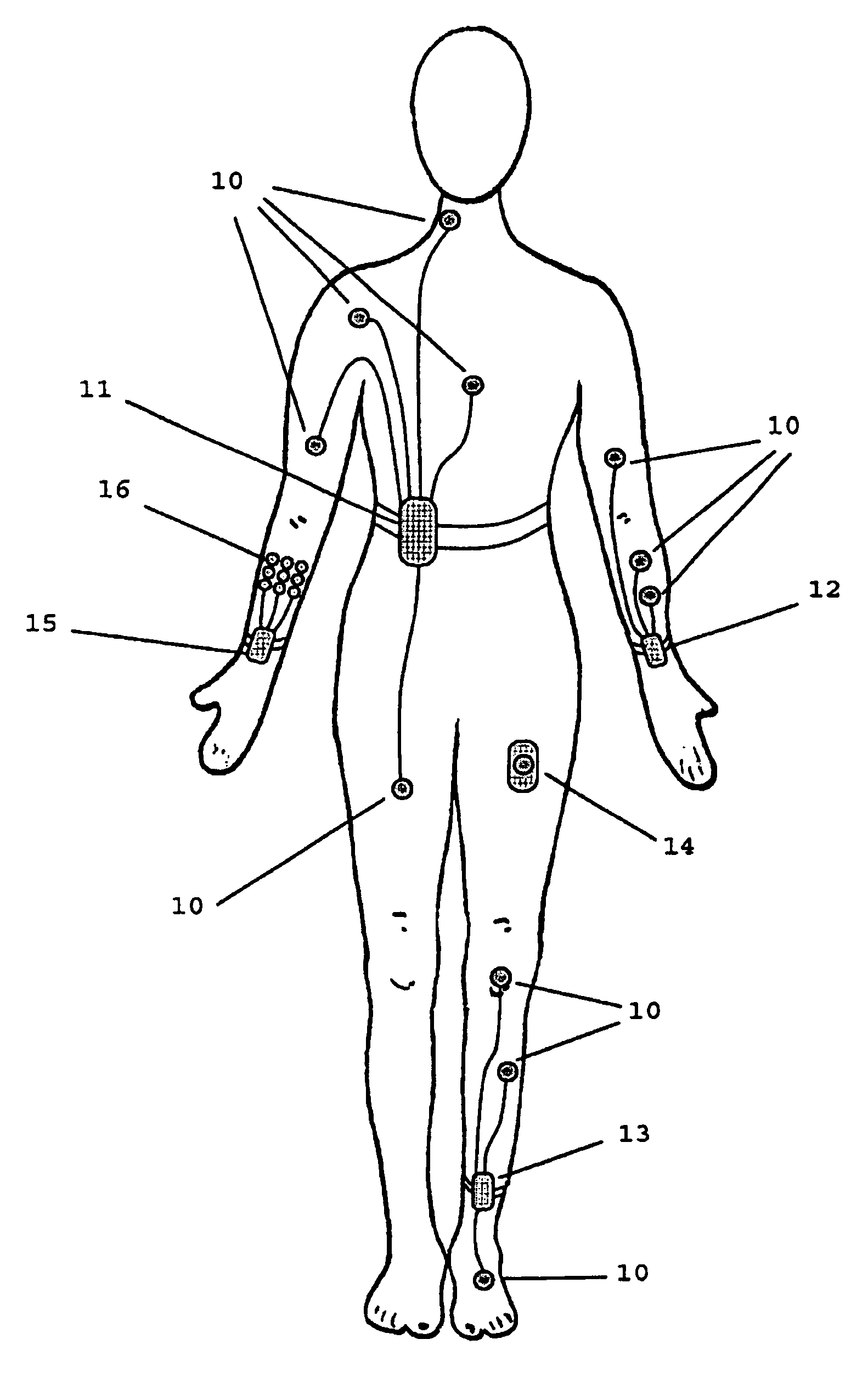
InactiveUS6083156ALow costEasy to transportElectrocardiographyElectromyographyMeasurement deviceUltrasonic sensor
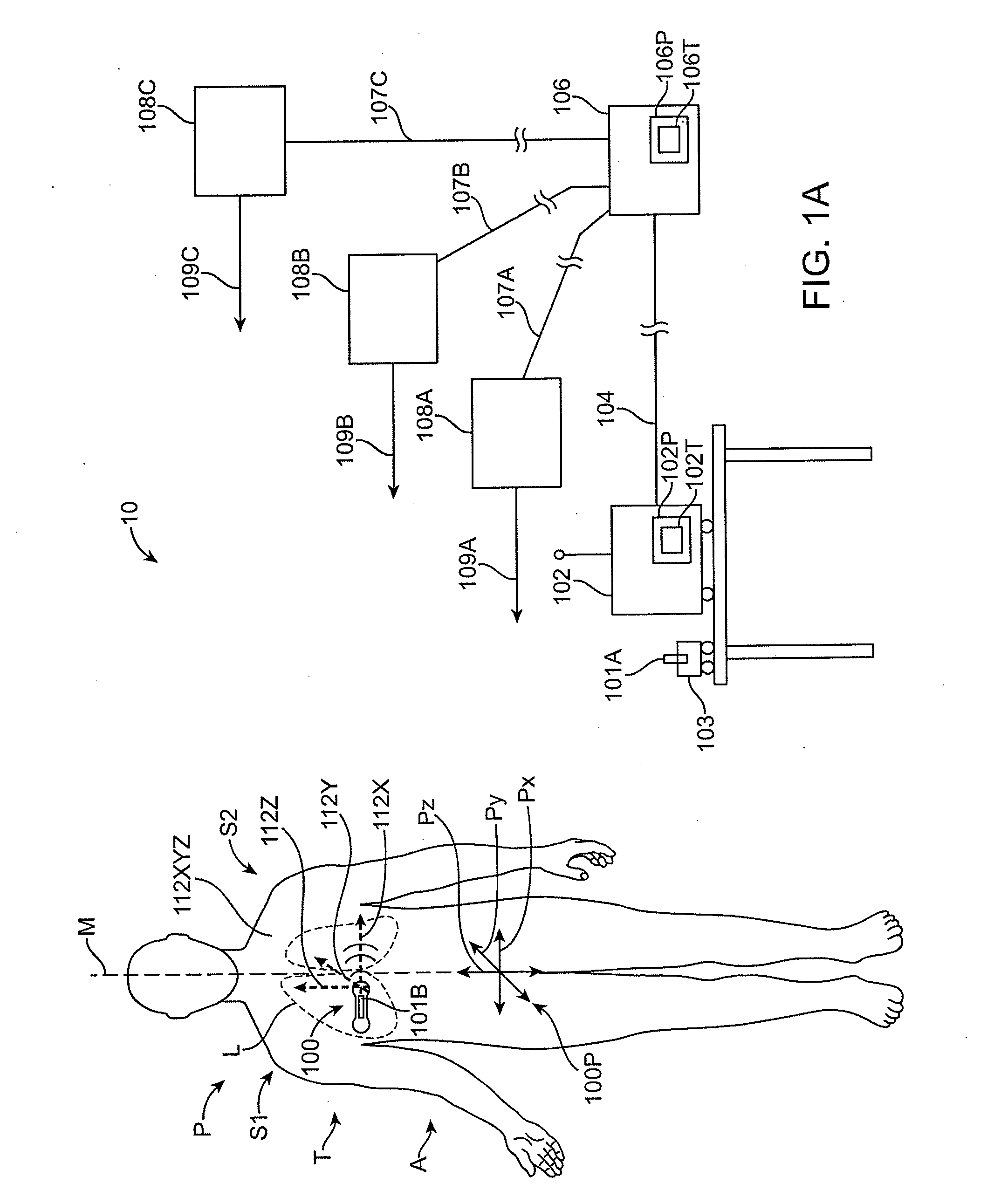
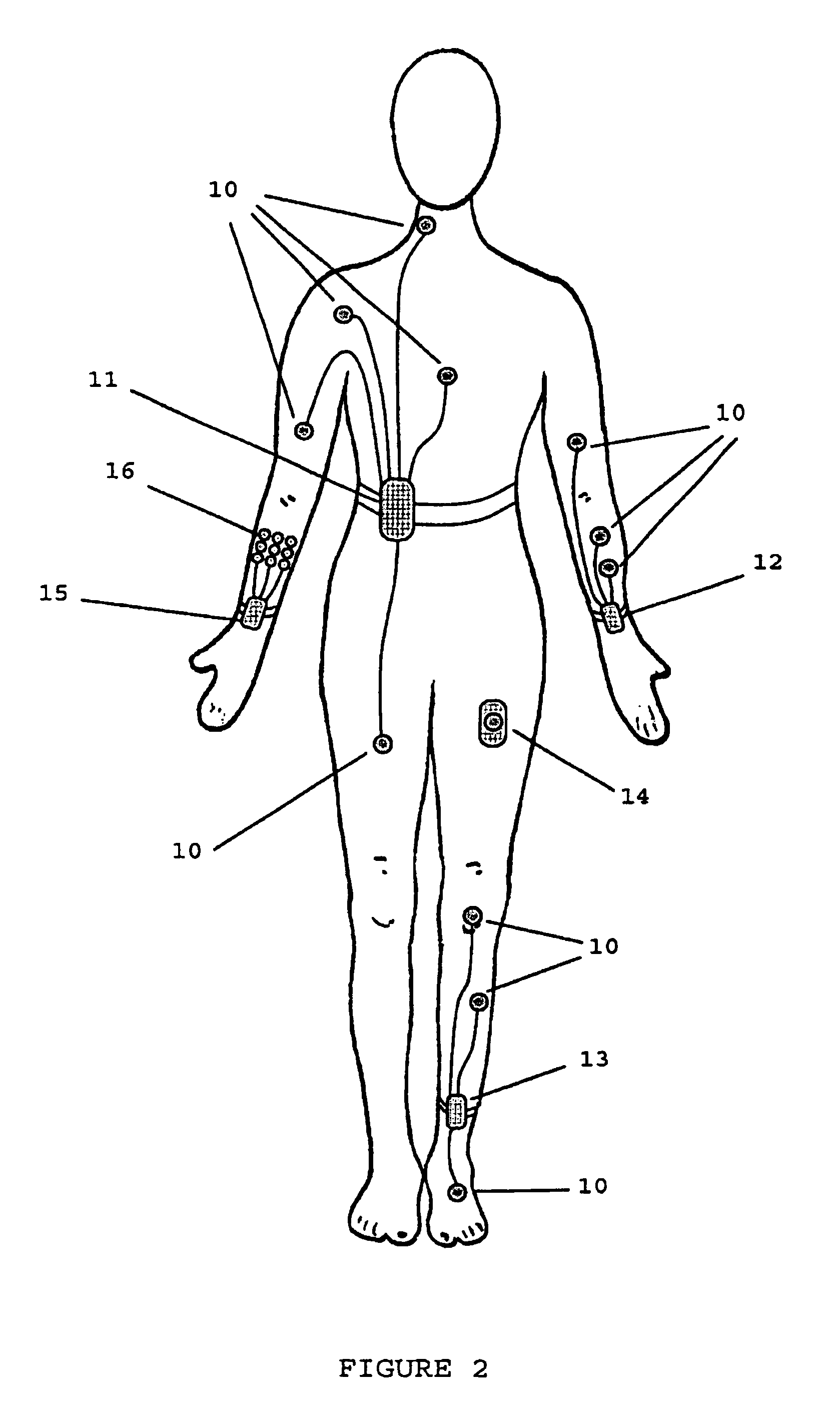
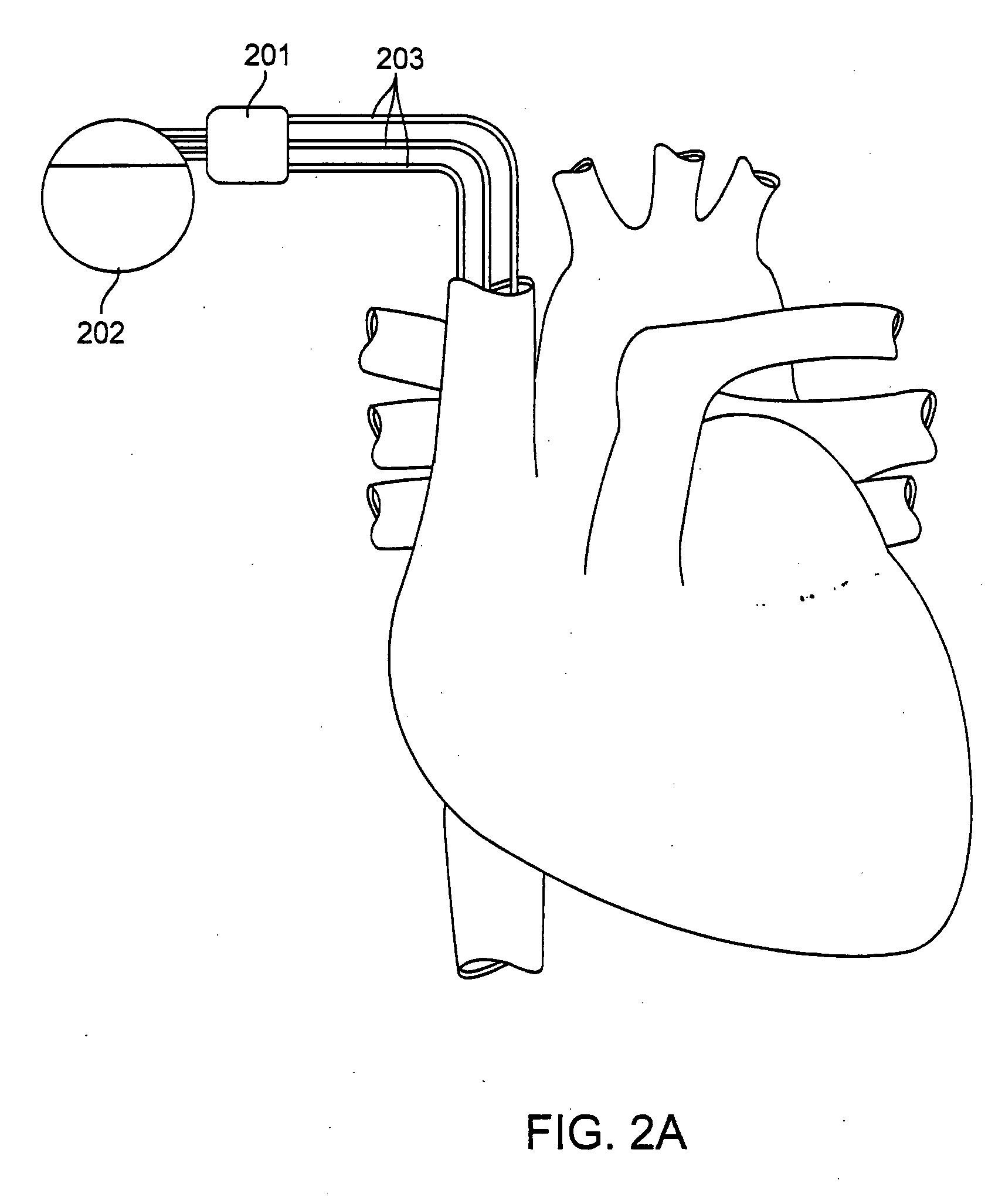
A portable, integrated physiological monitoring system is described for use in clinical outpatient environments. This systems consists of a plethora of sensors and auxiliary devices, an electronics unit (100) that interfaces to the sensors and devices, and a portable personal computer (102). Electrodes (106) are provided to acquisition electrocardiographic, electroencephalographic, and neuromuscular signals. Electrodes (108) are provided to stimulate neural and muscular tissue. A finger pulse oximeter (110), an M-mode ultrasonic transducer (112), an airflow sensor (114), a temperature probe (120), a patient event switch (116), and an electronic stethoscope (118) are provided. A portable personal computer (102) interfaces to the electronics unit (100) via a standard parallel printer port interface (258) to allow communication of commands and information to / from the electronics unit (100). Control and display of the information gathered from the electronics unit (100) is accomplished via an application program executing on the portable personal computer (102). Sharing of common data acquisition hardware along with preliminary processing of information gathered is accomplished within the electronics unit (100). The entire system is battery operated and portable. This system, because of its architecture, offers significant cost advantages as well as unique modes of operation that cannot be achieved from the individual physiological parameter measurement devices alone. The system allows for the integration of acquisitioned information from the sensors into a patient's database stored on the portable personal computer.
Owner:LISIECKI RONALD S
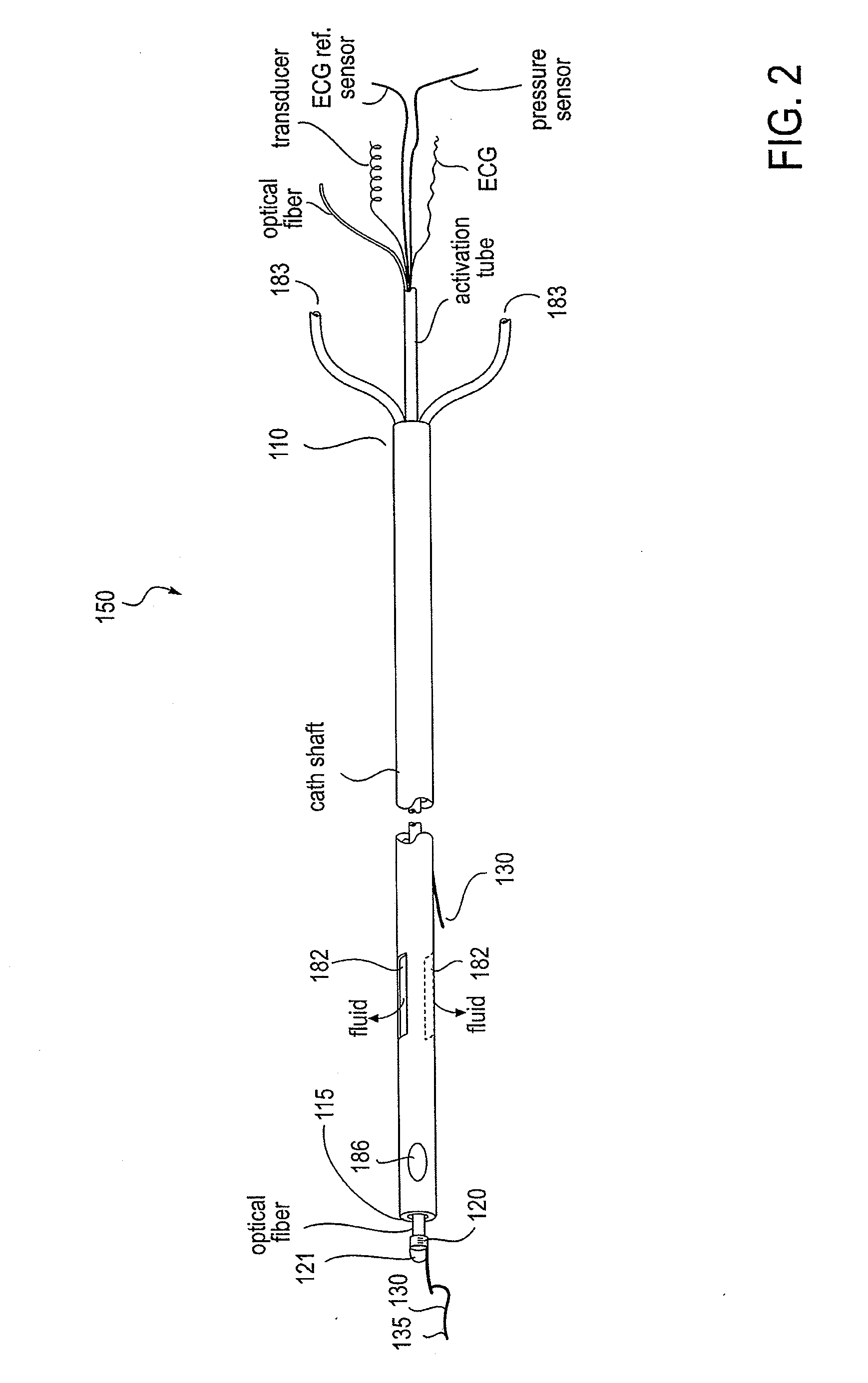
Endovascular devices and methods of use
ActiveUS20090177090A1StethoscopeHeart/pulse rate measurement devicesBalloon catheterIntravascular device
Owner:TELEFLEX LIFE SCI LTD
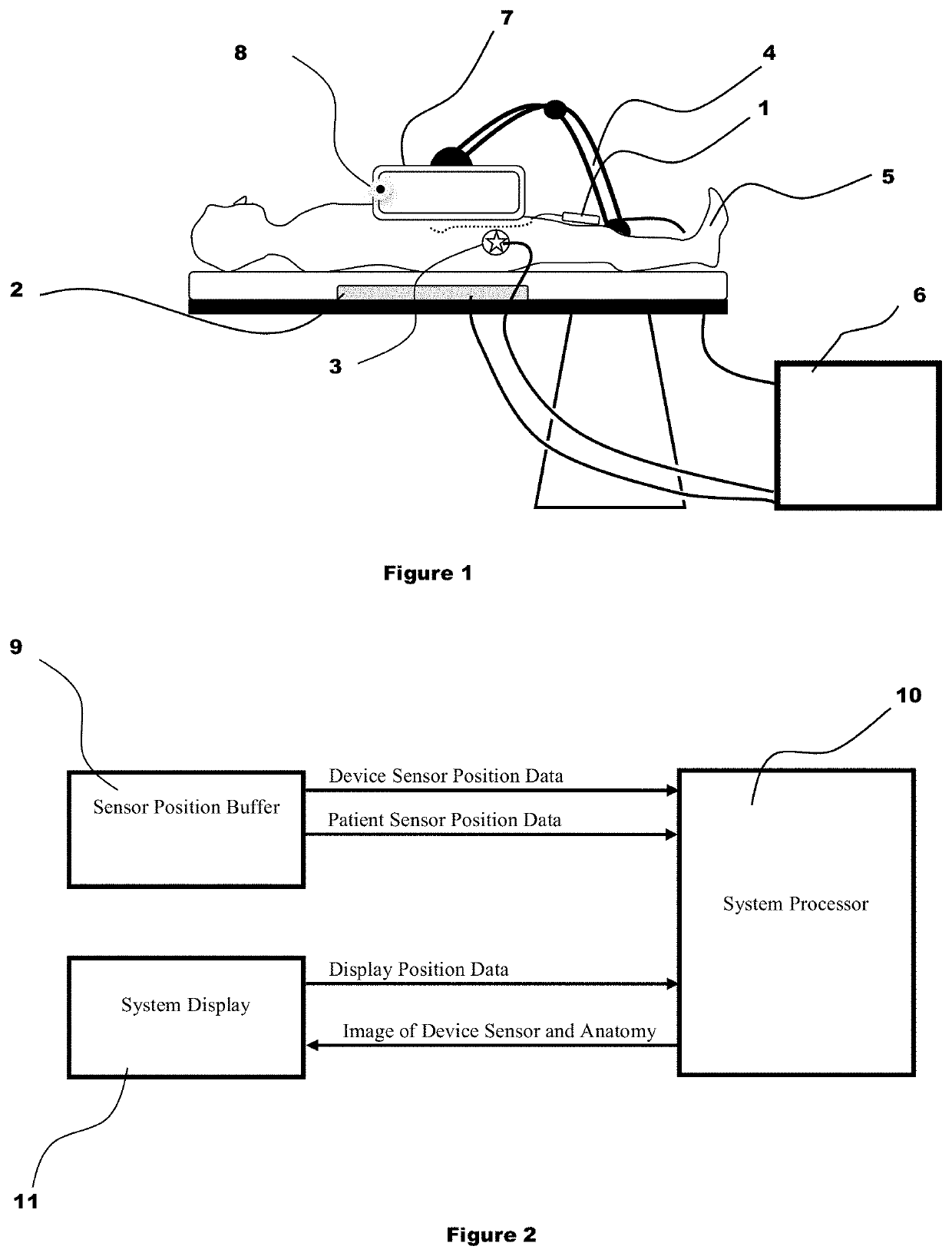
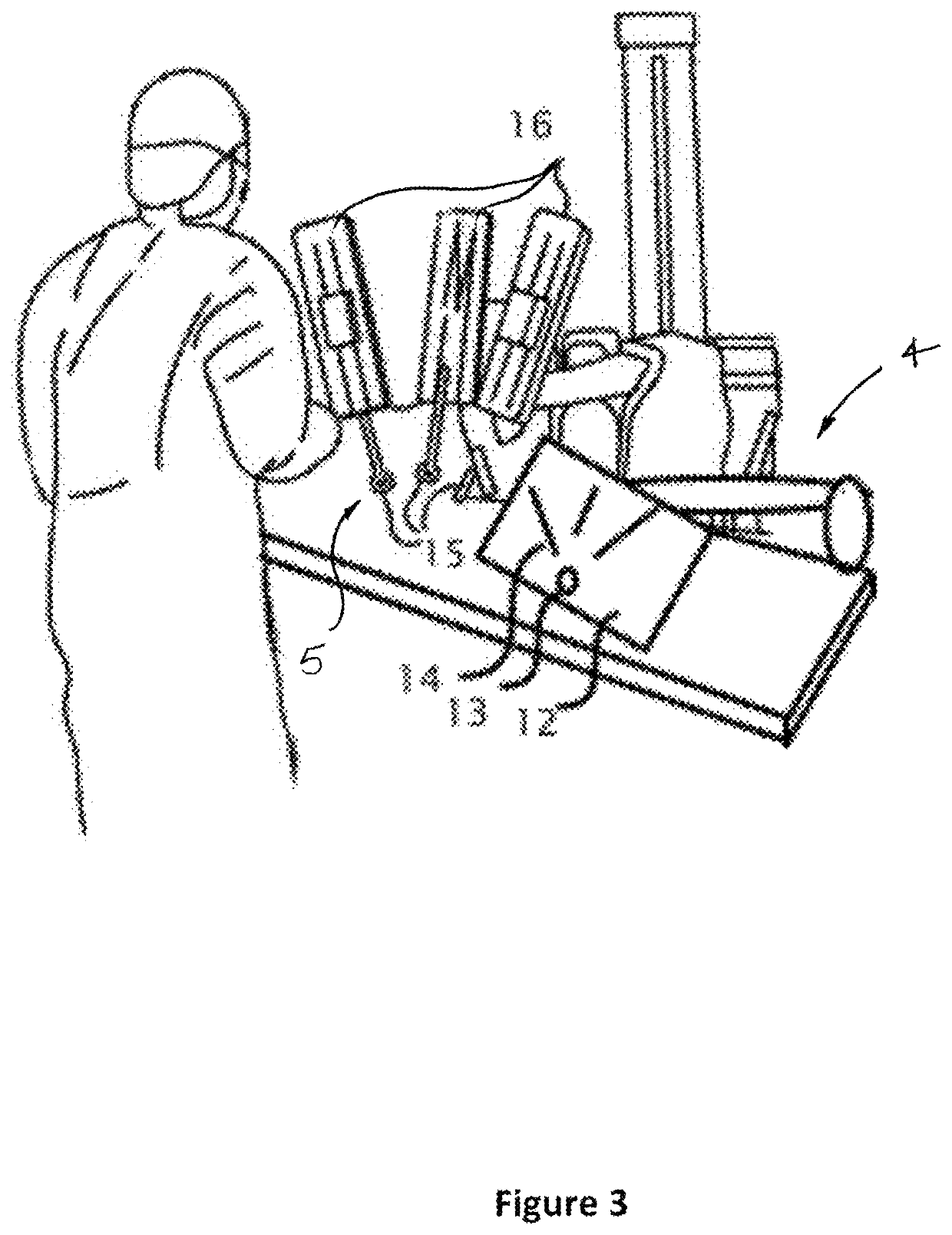
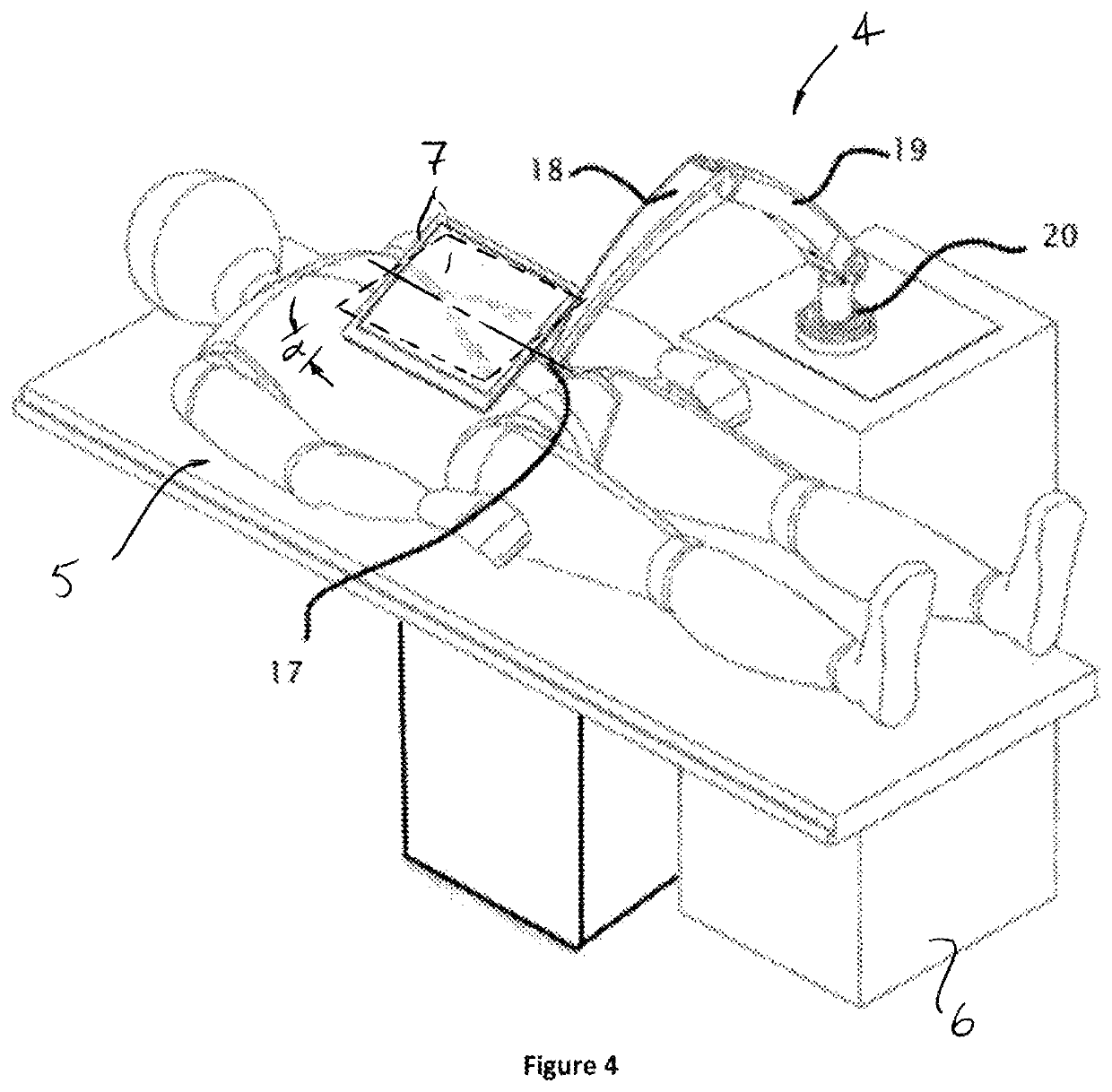
System and method for displaying anatomy and devices on a movable display
ActiveUS11020016B2Increase functional anatomical workspaceImprove ergonomicsMechanical/radiation/invasive therapiesDiagnostic recording/measuringHuman bodyRadiology
An image display system is provided comprised of a virtual window system that creates a visual coherency between the patient's anatomical images and the actual patient by aligning the image on the display to the patient and then presenting the image to the user in a way that feels as if the user is looking directly into the patient through the display. The image shown within the image display system is dependent upon the position of the image display apparatus and the position of the user so that the display orientation of the image may be biased slightly toward the user to improve ergonomics and usability.
Owner:AURIS HEALTH INC
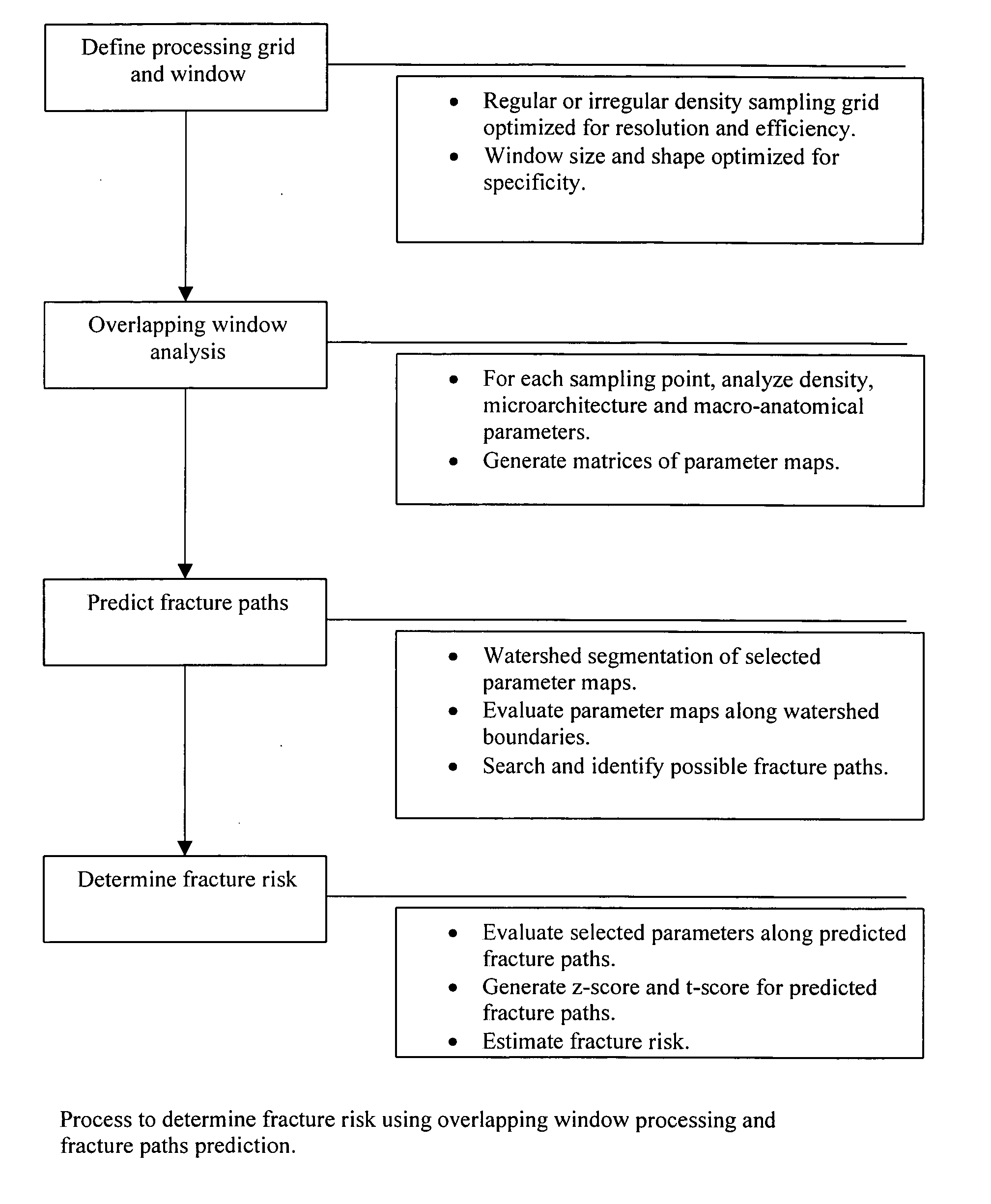
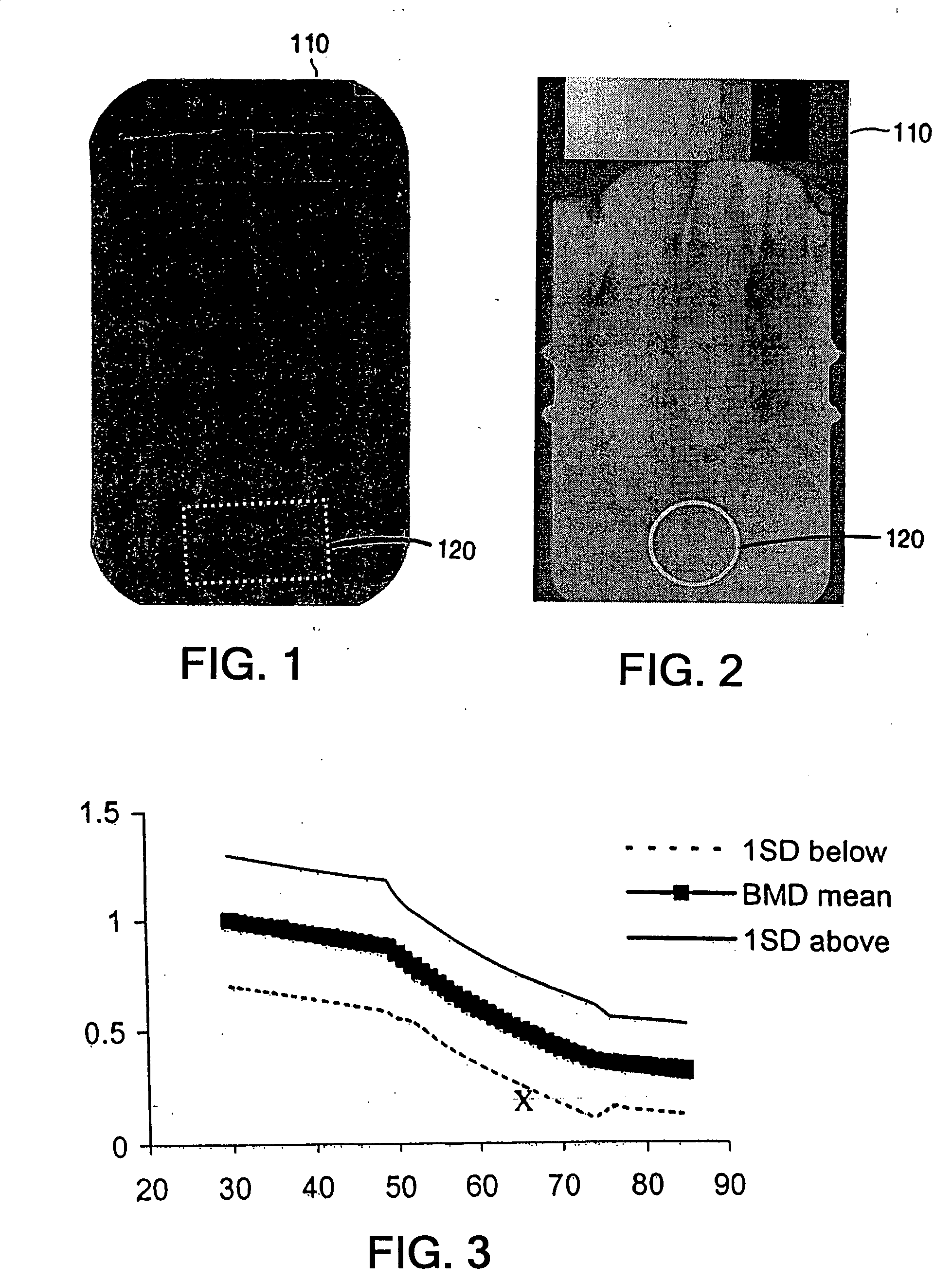
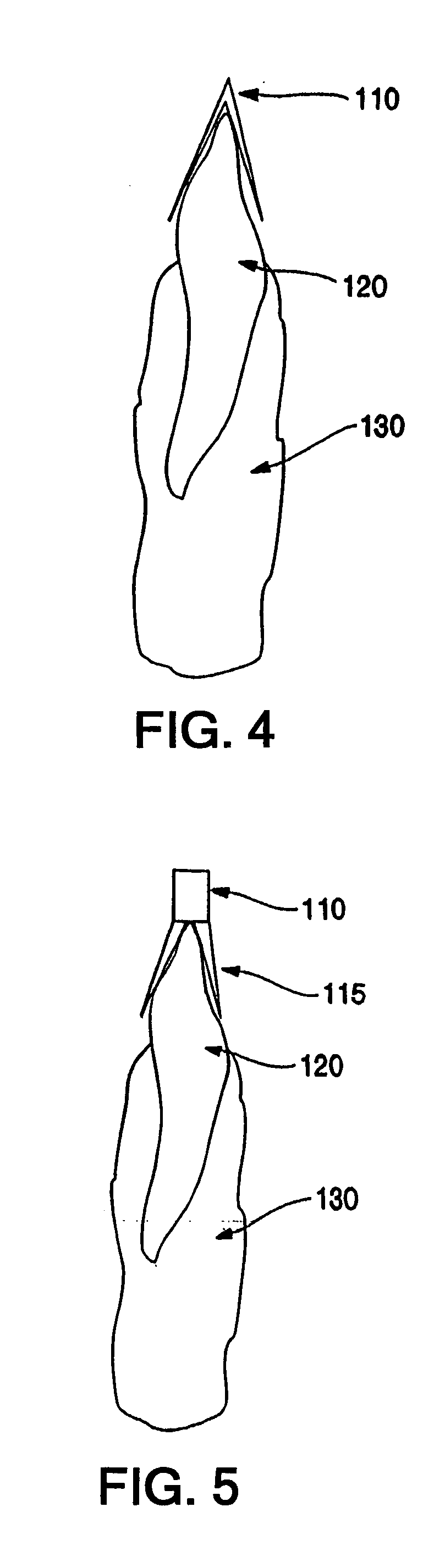
Methods for the compensation of imaging technique in the processing of radiographic images
The present invention relates to methods and devices for analyzing x-ray images. In particular, devices, methods and algorithms are provided that allow for the accurate and reliable evaluation of bone structure and macro-anatomical parameters from x-ray images.
Owner:IMATX
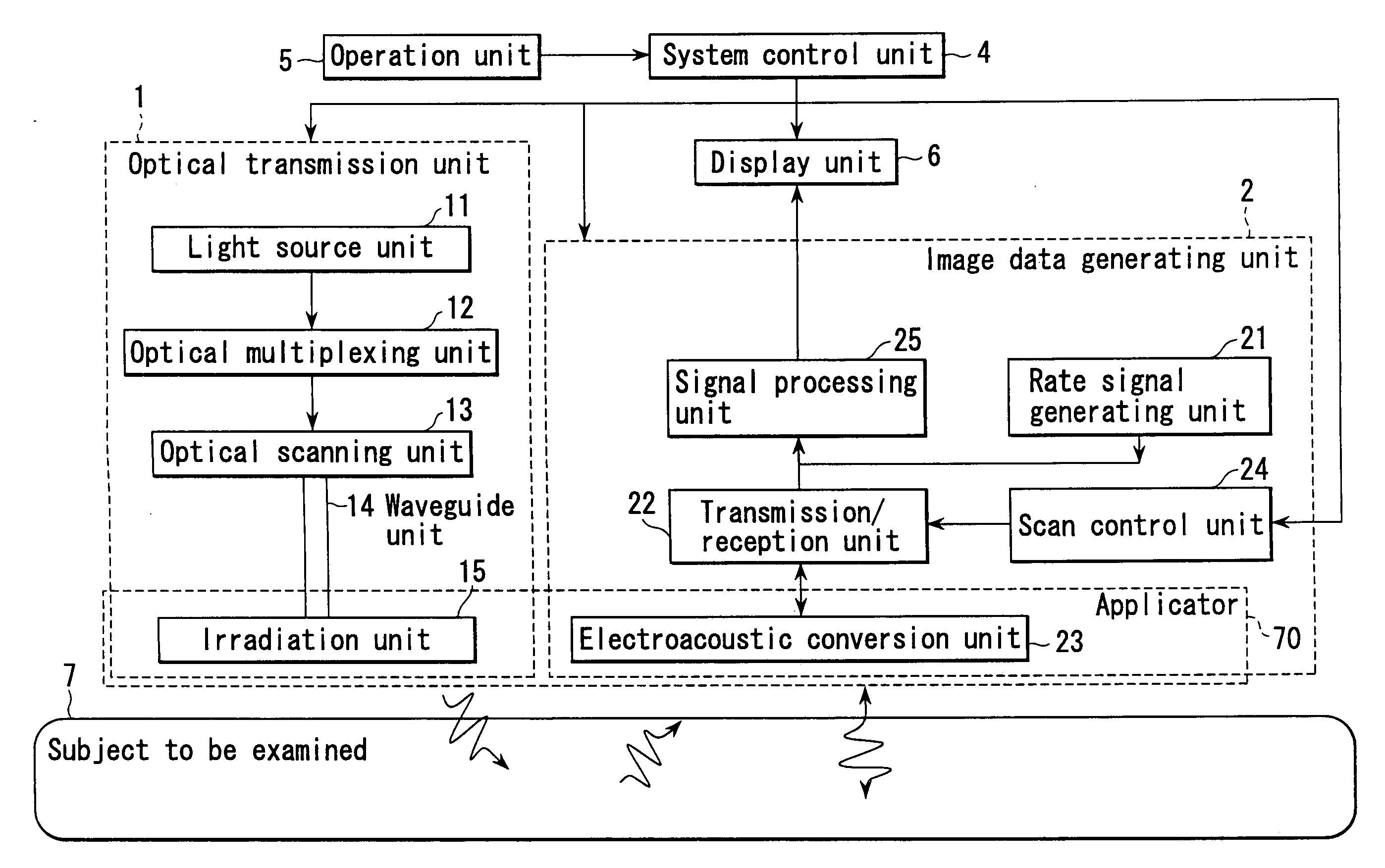
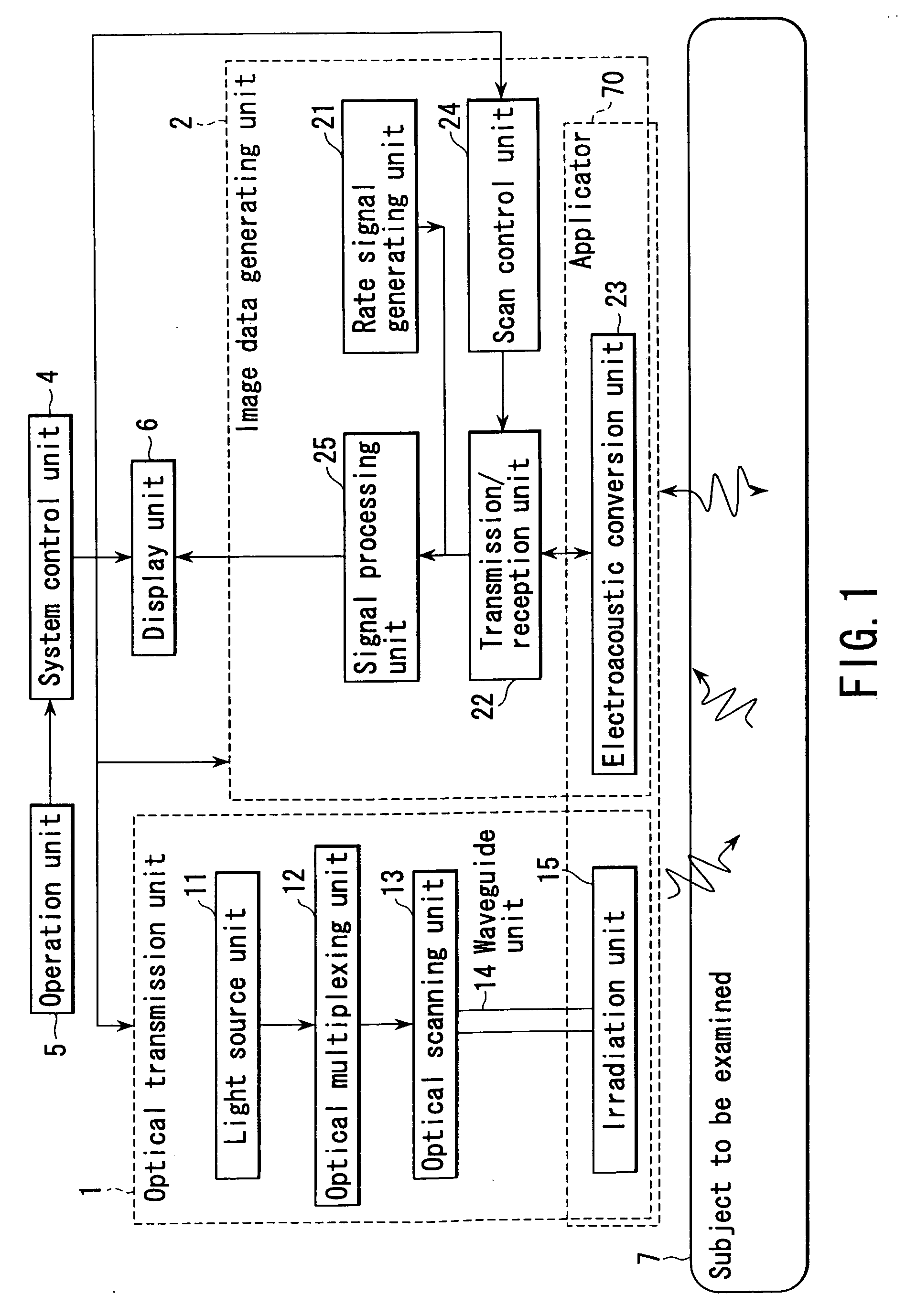
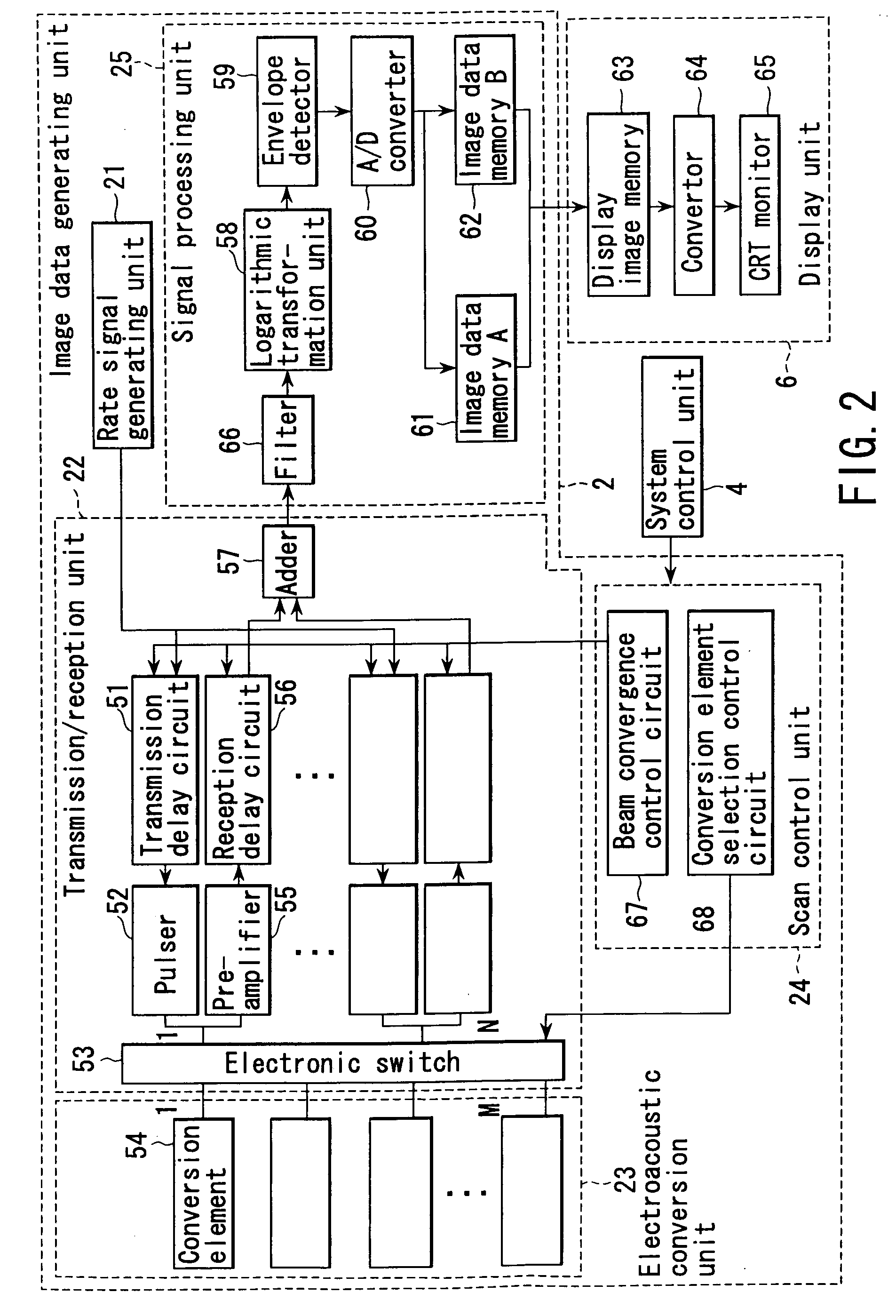
Method and apparatus for forming an image that shows information about a subject
ActiveUS20050004458A1Easy to operateImprove spatial resolutionAnalysing solids using sonic/ultrasonic/infrasonic wavesOrgan movement/changes detectionAcoustic waveLength wave
An apparatus includes an optical transmission unit which irradiates a subject to be examined with light containing a specific wavelength component, an electroacoustic conversion unit which receives acoustic waves generated inside the subject by the light radiated by the optical transmission unit and converts them into electrical signals, an image data generating unit which generates first image data on the basis of the reception signals obtained by the electroacoustic conversion unit, an electroacoustic conversion unit which receives ultrasonic reflection signals obtained by transmitting ultrasonic waves to the subject and converts them into electrical signals, an image data generating unit which generates second image data on the basis of the reception signals obtained by the electroacoustic conversion unit, and a display unit which combines the first and second image data and displays the resultant data.
Owner:TOSHIBA MEDICAL SYST CORP
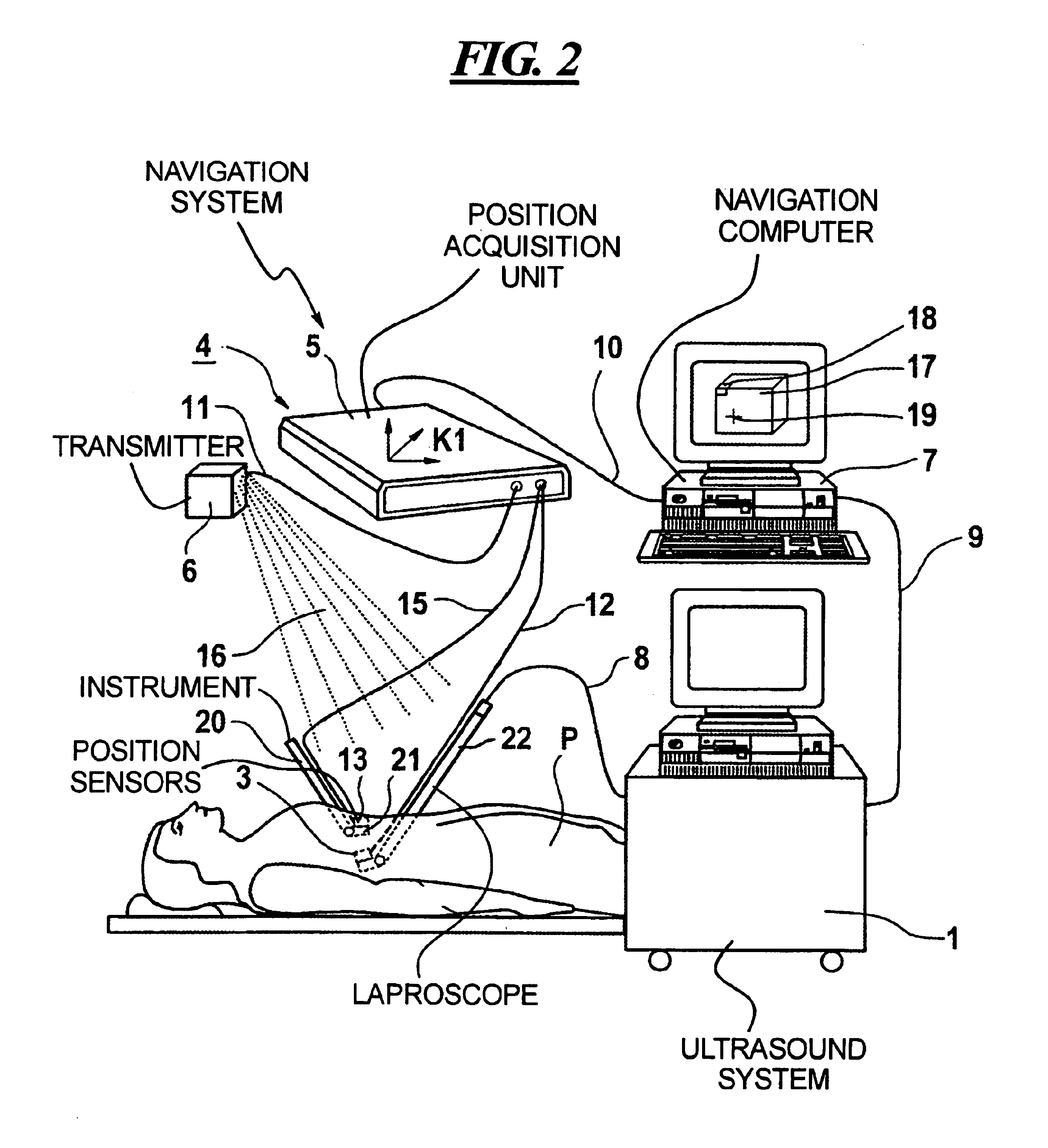
Medical workstation, imaging system, and method for mixing two images
InactiveUS6895268B1Well mixedEffective supportGeometric image transformationSurgeryWorkstationComputer science
In a system, method and workstation, images of a first subject are acquired with an image signal acquisition unit, the position of the image signal acquisition unit is determined, the position of a second subject is determined and the position of the second subject relative to the image signal acquisition unit is also determined and an image of the second subject is mixed into an image of the first subject acquired with the image signal acquisition unit.
Owner:SIEMENS AG
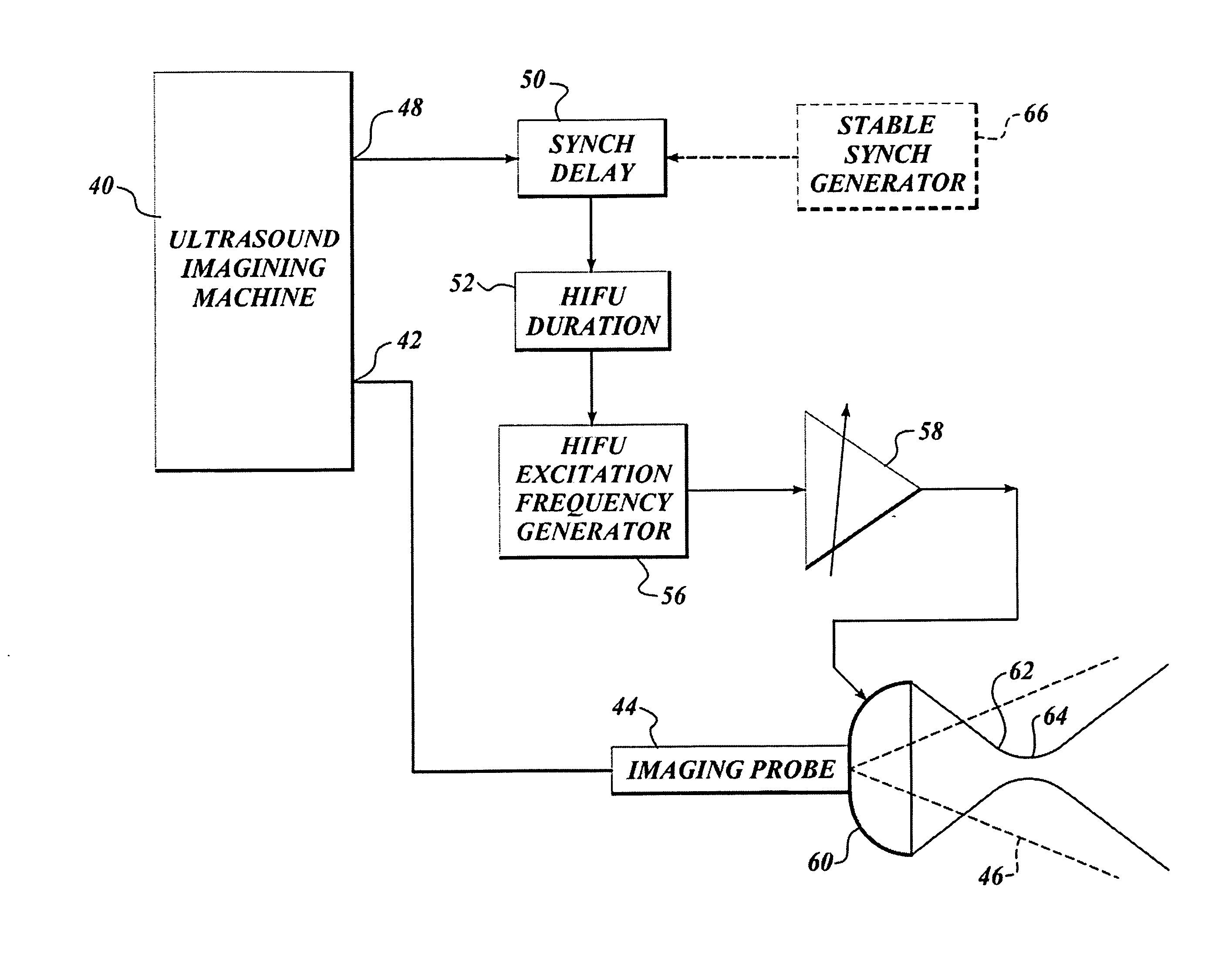
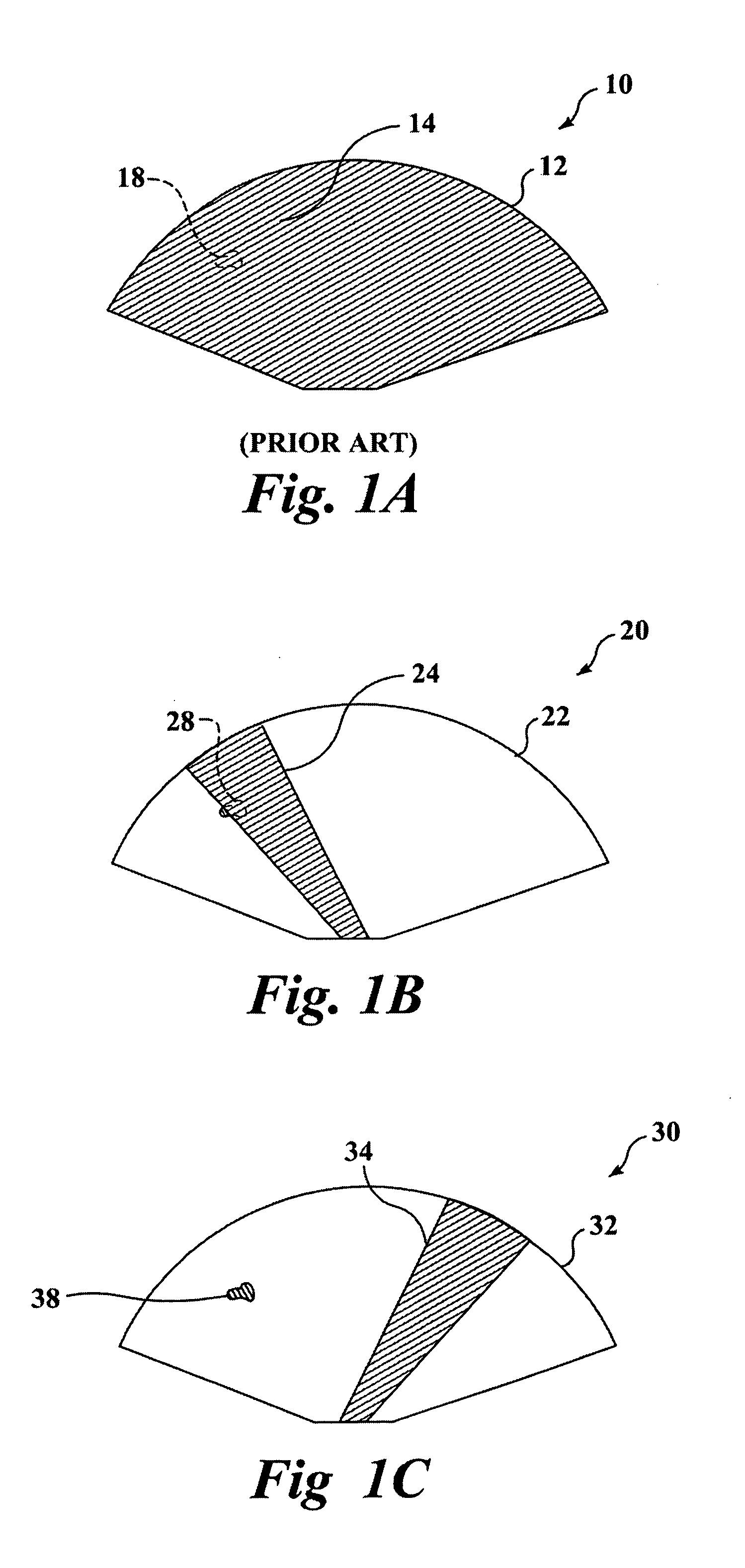
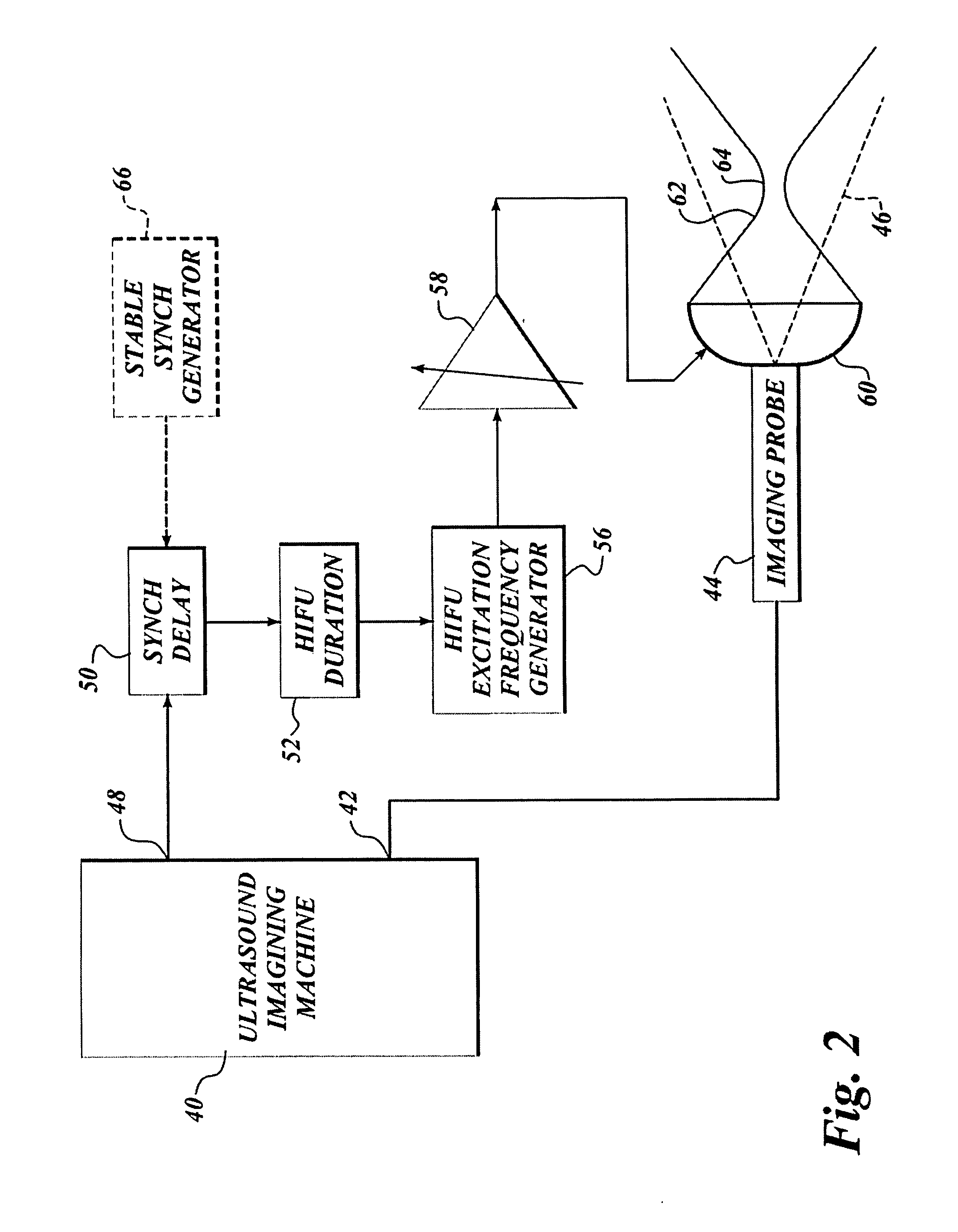
Use of contrast agents to increase the effectiveness of high intensity focused ultrasound therapy
InactiveUS20050038340A1Easy to useGood choiceUltrasound therapyBlood flow measurement devicesCavitationUltrasound contrast media
Ultrasound contrast agents are used to enhance imaging and facilitate HIFU therapy in four different ways. A contrast agent is used: (1) before therapy to locate specific vascular structures for treatment; (2) to determine the focal point of a HIFU therapy transducer while the HIFU therapy transducer is operated at a relatively low power level, so that non-target tissue is not damaged as the HIFU is transducer is properly focused at the target location; (3) to provide a positive feedback mechanism by causing cavitation that generates heat, reducing the level of HIFU energy administered for therapy compared to that required when a contrast agent is not used; and, (4) to shield non-target tissue from damage, by blocking the HIFU energy. Various combinations of these techniques can also be employed in a single therapeutic implementation.
Owner:UNIV OF WASHINGTON
Ultrasound system with stereo image guidance or tracking
ActiveUS20150148664A1Prevent movementOrgan movement/changes detectionSurgical navigation systemsDisplay deviceStereo image
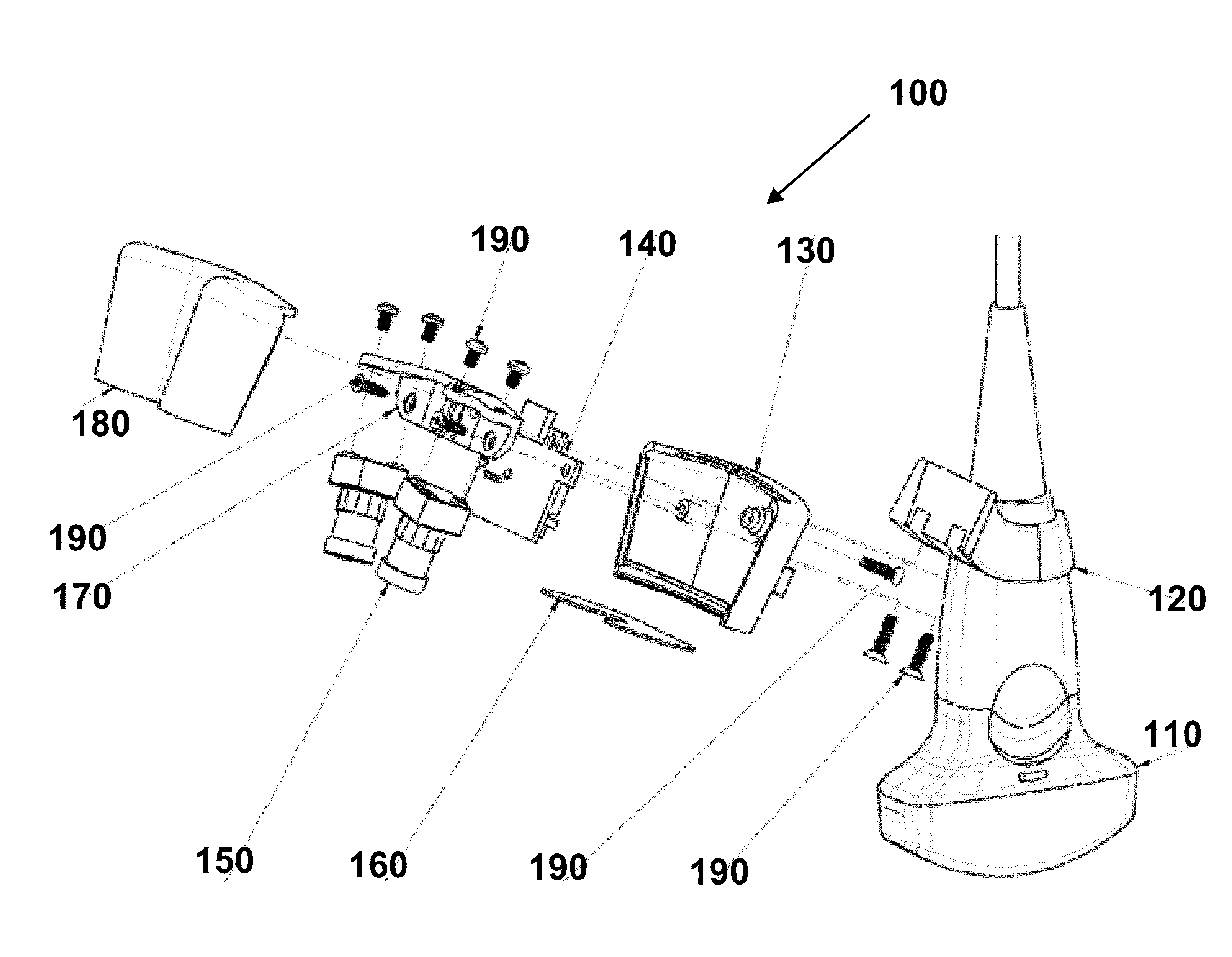
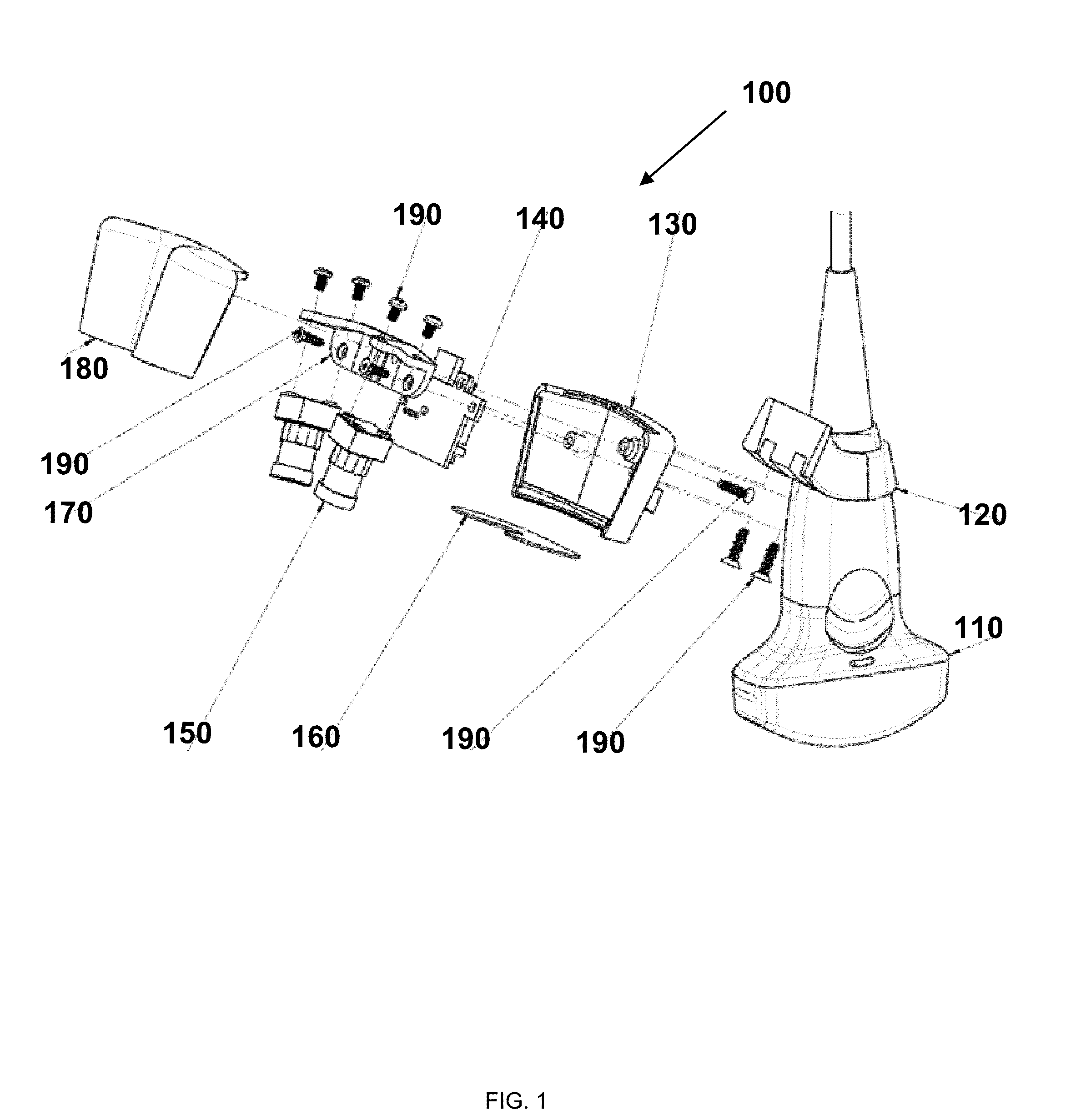
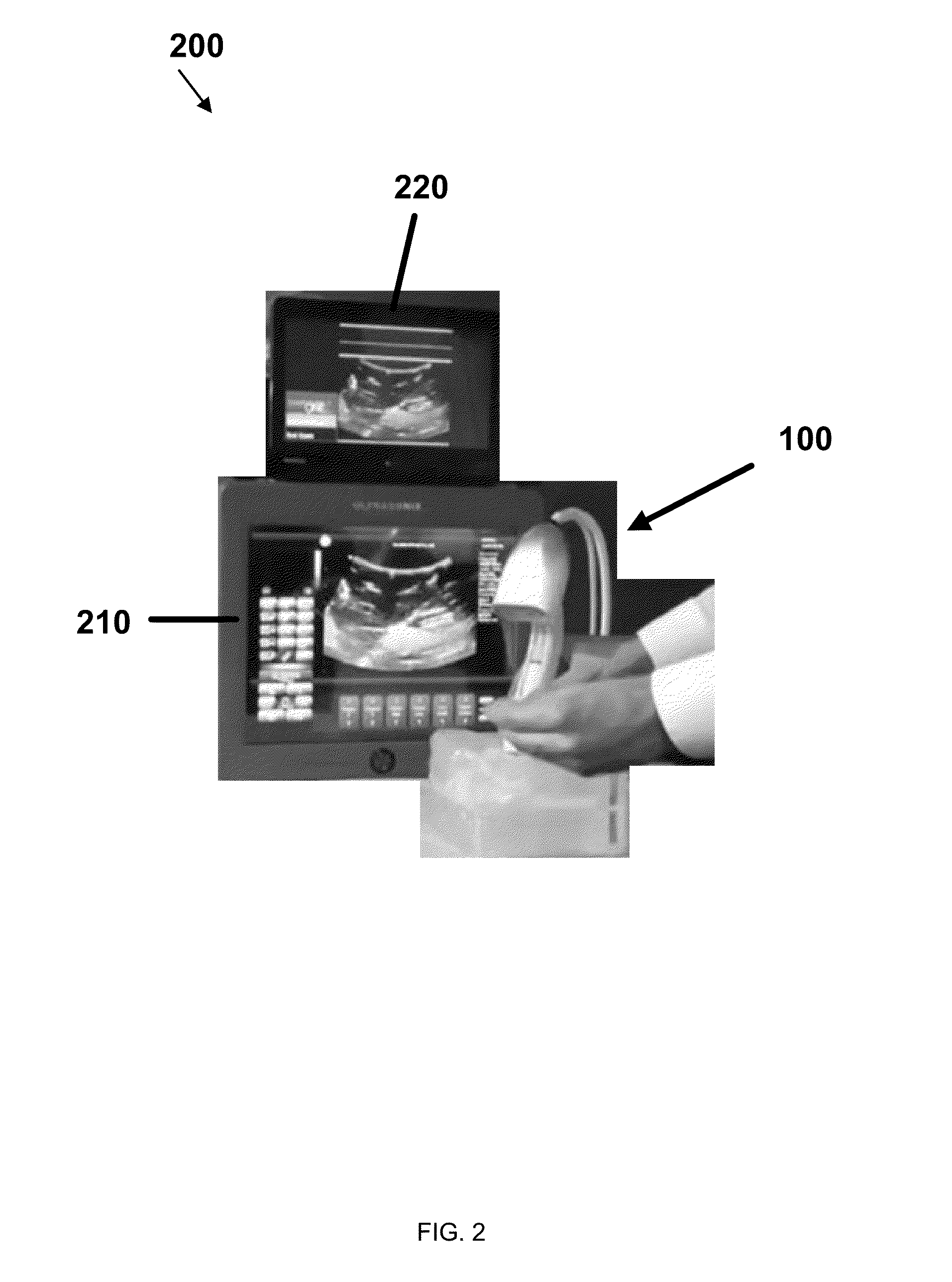
An image-guided ultrasound system may include an ultrasound probe, a display configured to communicate with the ultrasound probe to receive ultrasound signals to display images from the ultrasound probe, and an imaging device that may be attached to or integral with the ultrasound probe and configured to communicate with the display to display information derived from images from the imaging device. The imaging device may include a stabilization assembly, an imaging device assembly physically coupled to the stabilization assembly, a plurality of light-sensitive devices physically coupled to the stabilization assembly, and a memory unit physically coupled to the imaging device assembly, the memory unit configured to store calibration or usage information for the image-guided ultrasound system.
Owner:CLEAR GUIDE MEDICAL
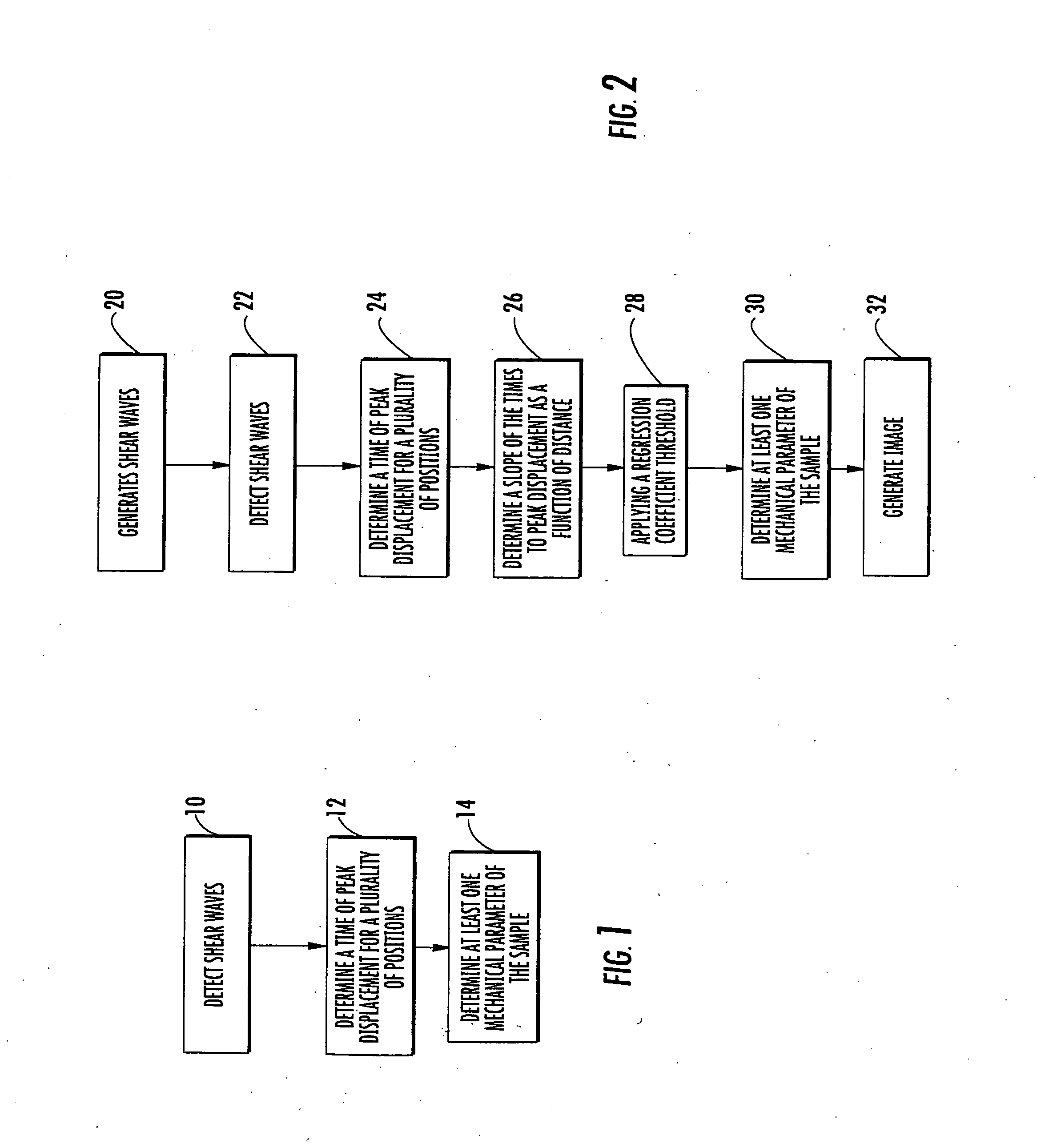
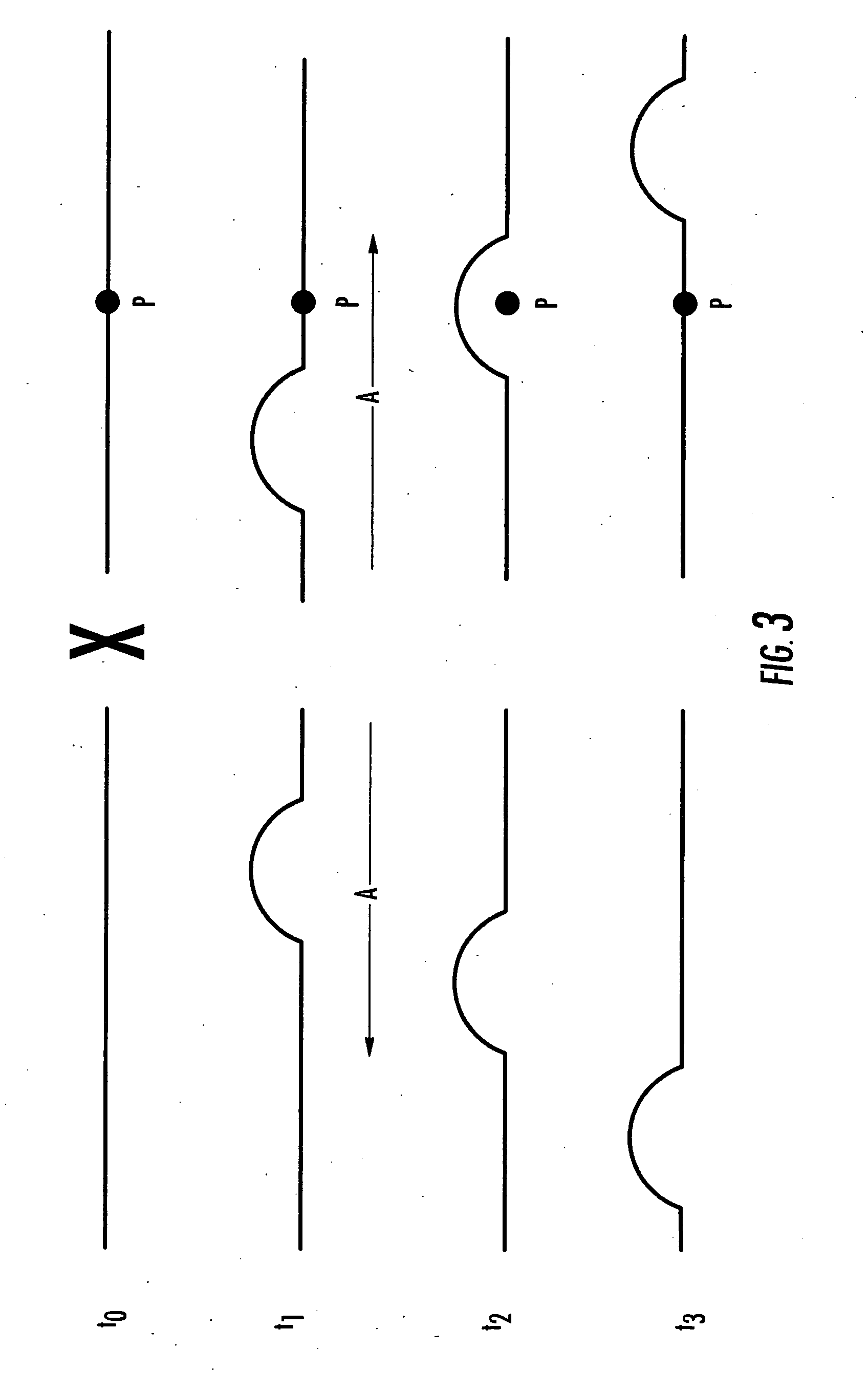
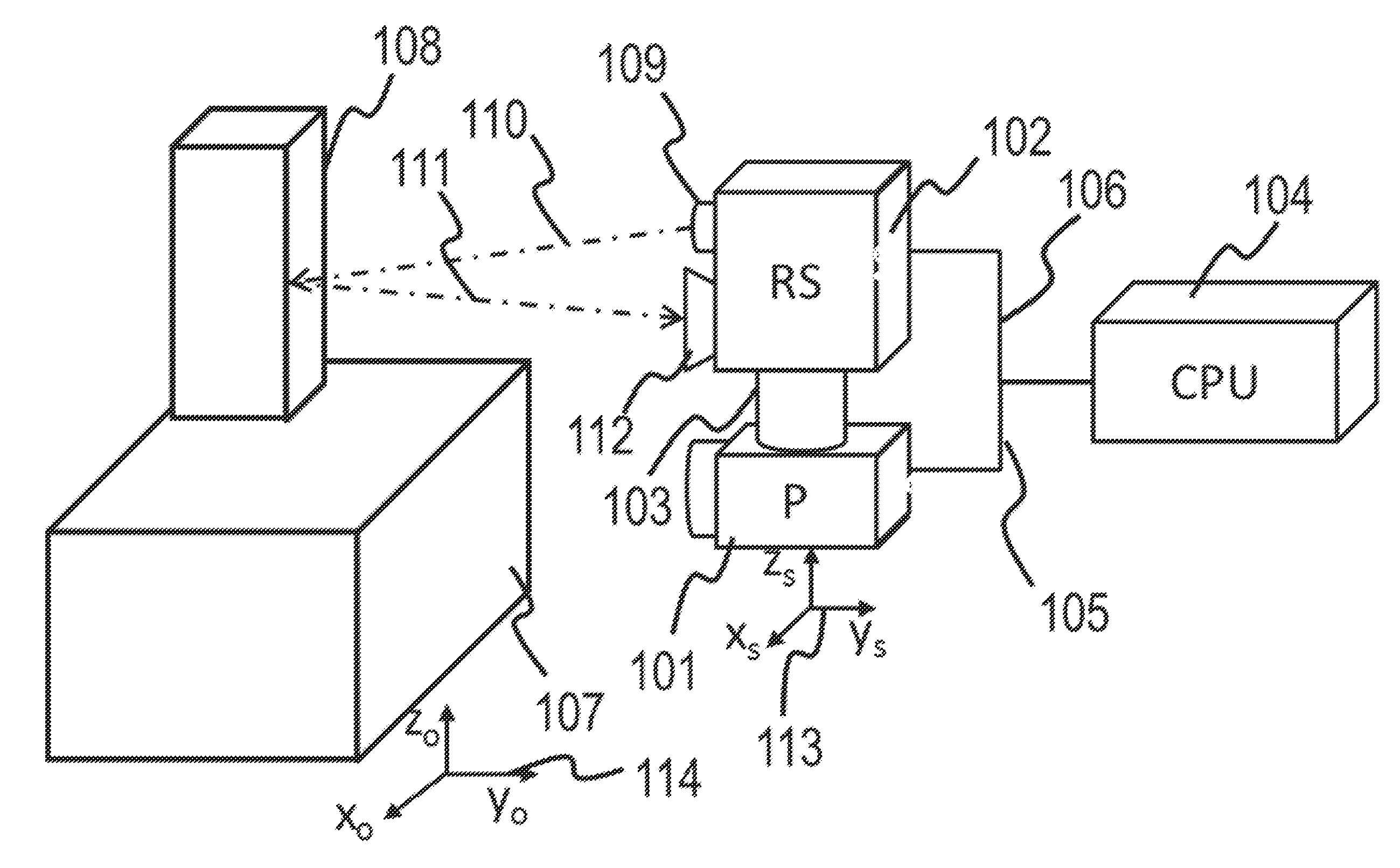
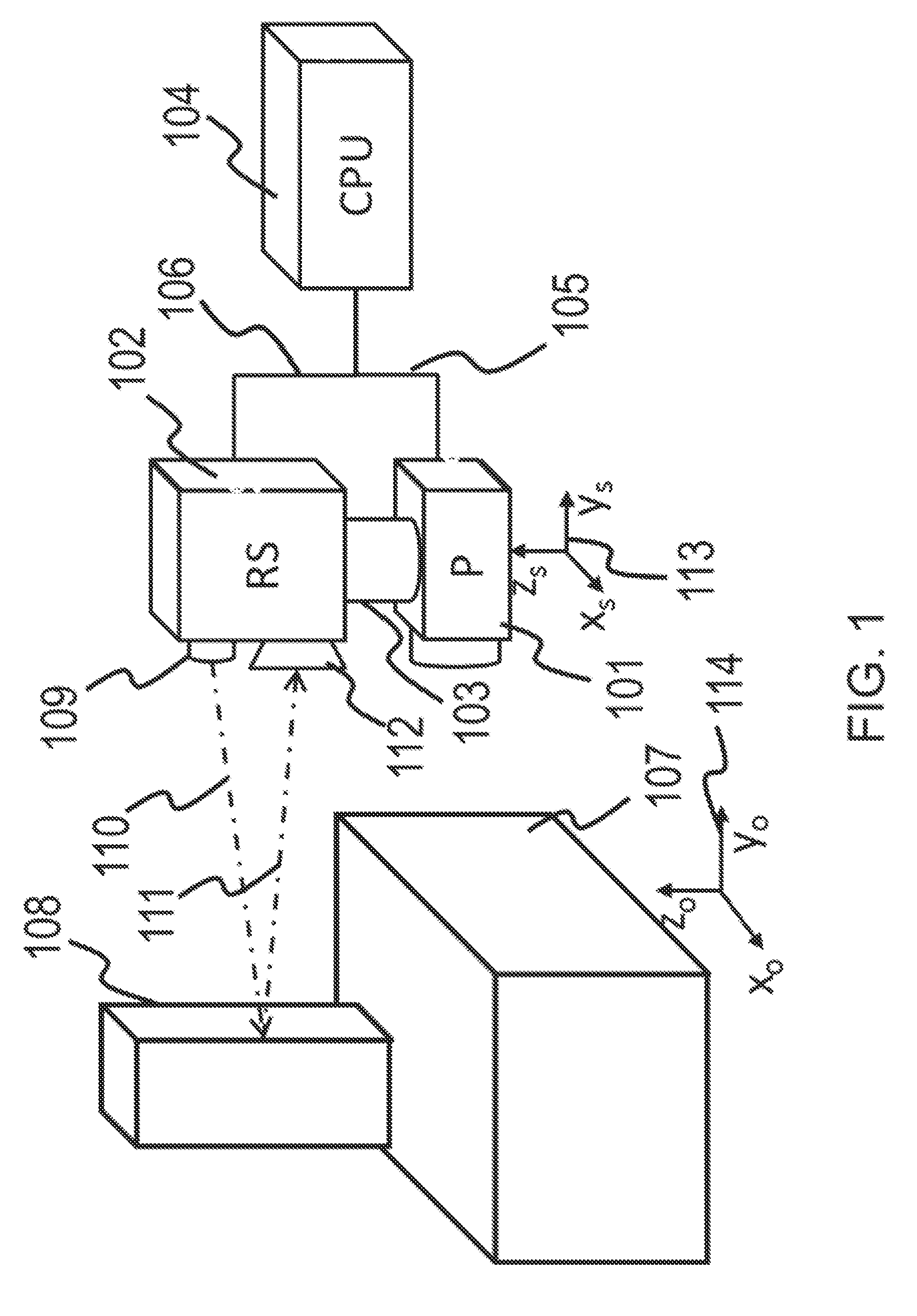
Methods, Systems and Computer Program Products for Ultrasound Shear Wave Velocity Estimation and Shear Modulus Reconstruction
ActiveUS20080249408A1Wave based measurement systemsOrgan movement/changes detectionShear modulusReconstruction method
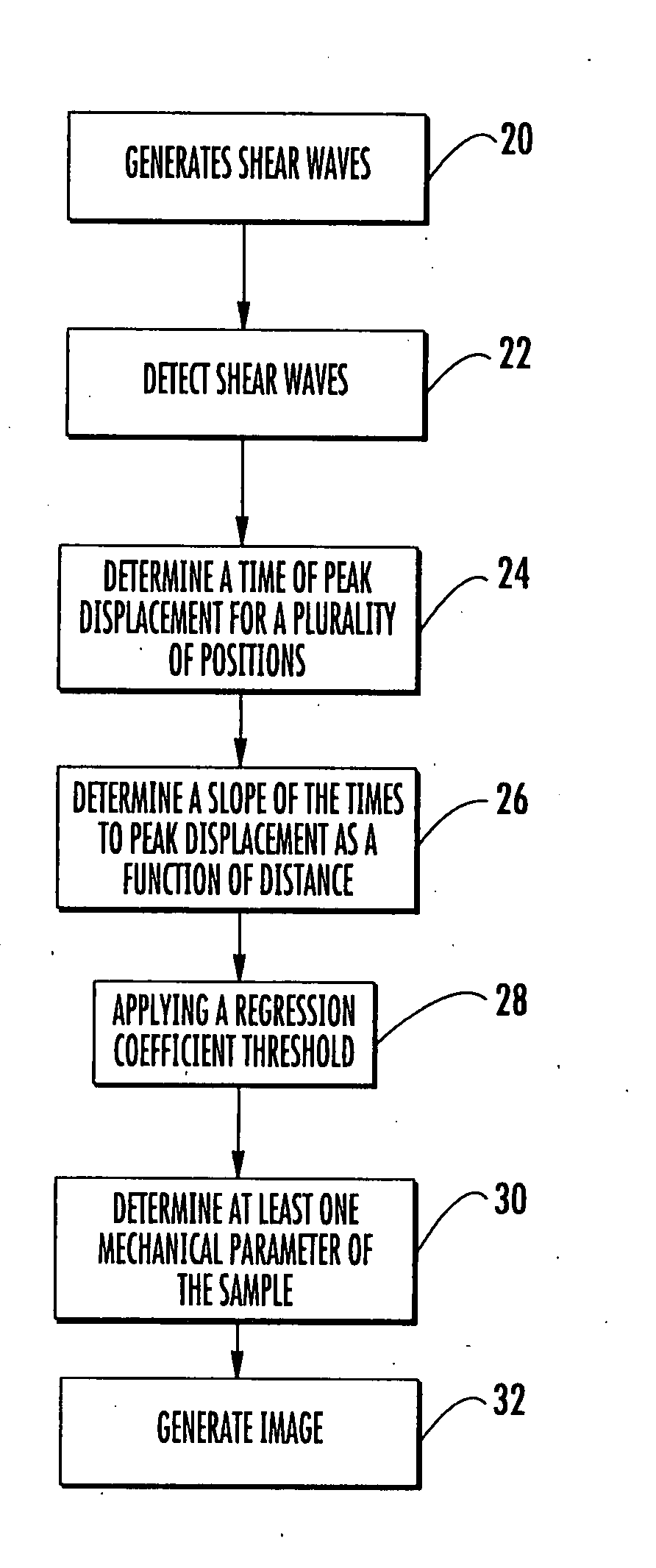
Methods for determining a mechanical parameter of a sample include detecting shear waves that have been generated in the sample by an applied shear wave source. A time of peak displacement of the shear waves for a plurality of sample positions is determined. At least one mechanical parameter of the sample based on the time of peak displacement for the plurality of sample positions is determined.
Owner:DUKE UNIV
Methods and systems for tracking and guiding sensors and instruments
ActiveUS20130237811A1Reduce ultrasound artifactSpeckle reductionMedical devicesDiagnostic recording/measuringMachine visionUltrasonic sensor
Owner:ZITEO INC
User interface for remote control of medical devices
InactiveUS20060041181A1Organ movement/changes detectionSurgical navigation systemsRemote controlDisplay device
An interface for remotely controlling a medical device in a patient's body provides a two dimensional display of a three dimensional rendering of the operating region, and allows the user to select the orientation or location of the distal end of the medical device on the display and then operate a navigation system to cause the distal end of the medical device to approximately assume the selected orientation or location.
Owner:STEREOTAXIS
Imaging, therapy, and temperature monitoring ultrasonic system
An ultrasonic system useful for providing imaging, therapy and temperature monitoring generally comprises an acoustic transducer assembly configured to enable the ultrasound system to perform the imaging, therapy and temperature monitoring functions. The acoustic transducer assembly comprises a single transducer that is operatively connected to an imaging subsystem, a therapy subsystem and a temperature monitoring subsystem. The ultrasound system may also include a display for imaging and temperature monitoring functions. An exemplary single transducer is configured such that when connected to the subsystems, the imaging subsystem can generate an image of a treatment region on the display, the therapy subsystem can generate high power acoustic energy to heat the treatment region, and the temperature monitoring subsystem can map and monitor the temperature of the treatment region and display the temperature on the display, all through the use of the single transducer. Additionally, the acoustic transducer assembly can be configured to provide three-dimensional imaging, temperature monitoring or therapeutic heating through the use of adaptive algorithms and / or rotational or translational movement. Moreover, a plurality of the exemplary single transducers can be provided to facilitate enhanced treatment capabilities.
Owner:GUIDED THERAPY SYSTEMS LLC